Categorización del fracaso para el tratamiento endodóntico primario
Categorization of failure for primary endodontic treatment
DOI:
https://doi.org/10.15446/aoc.v9n2.76432Palabras clave:
Endodoncia, periodontitis apical, resultado del tratamiento, tratamiento del conducto radicular, enfermedades periapicales (es)Endodontics, periapical periodontitis, treatment outcome, root canal therapy, periapical diseases (en)
Objetivo: caracterizar la enfermedad periapical posterior al tratamiento endodóntico primario realizado en una cohorte de individuos asistentes a las clínicas de la Especialidad en Endodoncia de la Facultad de Odontología de la Universidad Nacional de Colombia. Métodos: se realizó un estudio observacional retrospectivo en una muestra de 232 dientes con tratamiento endodóntico primario, procedentes de 155 individuos. Un análisis de frecuencia estimó la prevalencia entre la presencia de enfermedad periapical y las siguientes covariables: sexo, edad, tipo y localización del diente, diagnóstico previo, condiciones del tratamiento endodóntico, y tipo de restauración. Resultados: se registró un 24% de prevalencia de enfermedad periapical en la población observada. De este porcentaje, el 13,7% fue categorizado como EPE y el 10,3% fue categorizado como EPP. La distribución por sexo fue de 59% para mujeres y 41% para hombres, con promedio de edad de 55,8 años. La prevalencia de la enfermedad fue mayor en molares (44%) y el diagnóstico pulpar más frecuente fue necrosis pulpar (34%). El 20% de los tratamientos analizados presentó longitud de obturación corta y, de ellos, el 54,3% se asoció con aparición de la enfermedad. Conclusiones: la longitud de obturación corta resultó ser el factor que registró mayor relación clínica con la aparición de la enfermedad. Se reconoce a la EPE como el verdadero fracaso del tratamiento endodóntico primario.
Objetive: Identify the characteristics of the periapical disease in the primary endodontic treatment, in teeth to individuals person that included in the Speciality in Endodontics of the Faculty of Dentistry of the Universidad Nacional de Colombia. Methods: Retrospective observational study in a population of 232 teeth from 155 individuals with primary endodontic treatment. A frequency analysis was performed, estimating the prevalence between, the presence of periapical disease and the covariables sex, age, type and location of tooth, previous diagnosis, conditions of endodontic treatment and type of restoration. Results: For the total study population, 24% has been periapical postreatment disease, was categorized in 13,7% as EPD and 10,3% as PPD. The distribution by sex included 59% women and 41% men, age average of 55,8 years. 20% of the analyzed treatments presented a short obturation length, of which 54,3% were associated with EPD. Conclusions: The short obturation length proved to be the factor that registered the greatest clinical relation with the onset of the disease. EPE is recognized as the true failure of primary endodontic treatment.
Categorización del fracaso para el tratamiento endodóntico primario*
Categorization of failure for primary endodontic treatment
* Artículo original de investigación derivado del trabajo grado para optar por el título de Odontólogo. Forma parte del macroproyecto “Investigación en endodoncia clínica, pronóstico del tratamiento endodóntico en sus tres dimensiones, primario, secundario; ortógrado y retrogrado”. Código: 34933. Código quipu: 201010026625. Favorecido en la Convocatoria nacional de proyectos para el fortalecimiento de la investigación, creación e innovación de la Universidad Nacional de Colombia 2016-2018.
Citación sugerida
Sánchez Alemán J, García Guerrero C. Categorización del fracaso para el tratamiento endodóntico primario. Acta Odont Col [en línea] 2019 [fecha de consulta: dd/mm/aaaa]; 9(2): - 23. Disponible en: https://revistas.unal.edu.co/index.php/actaodontocol/article/view/76432
|
Recibido 26/11/2018 |
Aprobado 11/10/2018 |
Publicado 15/07/2019 |
Resumen
Objetivo: caracterizar la enfermedad periapical posterior al tratamiento endodóntico primario realizado en una cohorte de individuos asistentes a las clínicas de la Especialidad en Endodoncia de la Facultad de Odontología de la Universidad Nacional de Colombia. Métodos: se realizó un estudio observacional retrospectivo en una muestra de 232 dientes con tratamiento endodóntico primario, procedentes de 155 individuos. Un análisis de frecuencia estimó la prevalencia entre la presencia de enfermedad periapical y las siguientes covariables: sexo, edad, tipo y localización del diente, diagnóstico previo, condiciones del tratamiento endodóntico, y tipo de restauración. Resultados: se registró un 24% de prevalencia de enfermedad periapical en la población observada. De este porcentaje, el 13,7% fue categorizado como EPE y el 10,3% fue categorizado como EPP. La distribución por sexo fue de 59% para mujeres y 41% para hombres, con promedio de edad de 55,8 años. La prevalencia de la enfermedad fue mayor en molares (44%) y el diagnóstico pulpar más frecuente fue necrosis pulpar (34%). El 20% de los tratamientos analizados presentó longitud de obturación corta y, de ellos, el 54,3% se asoció con aparición de la enfermedad. Conclusiones: la longitud de obturación corta resultó ser el factor que registró mayor relación clínica con la aparición de la enfermedad. Se reconoce a la EPE como el verdadero fracaso del tratamiento endodóntico primario.
Palabras clave: endodoncia; periodontitis apical; resultado del tratamiento; tratamiento del conducto radicular; enfermedades periapicales.
Abstract
Objetive: Identify the characteristics of the periapical disease in the primary endodontic treatment, in teeth to individuals person that included in the Speciality in Endodontics of the Faculty of Dentistry of the Universidad Nacional de Colombia. Methods: Retrospective observational study in a population of 232 teeth from 155 individuals with primary endodontic treatment. A frequency analysis was performed, estimating the prevalence between, the presence of periapical disease and the covariables sex, age, type and location of tooth, previous diagnosis, conditions of endodontic treatment and type of restoration. Results: For the total study population, 24% has been periapical postreatment disease, was categorized in 13,7% as EPD and 10,3% as PPD. The distribution by sex included 59% women and 41% men, age average of 55,8 years. 20% of the analyzed treatments presented a short obturation length, of which 54,3% were associated with EPD. Conclusions: The short obturation length proved to be the factor that registered the greatest clinical relation with the onset of the disease. EPE is recognized as the true failure of primary endodontic treatment.
Key words: endodontics; periapical periodontitis; treatment outcome; root canal therapy; periapical diseases.
Introducción
El resultado del tratamiento endodóntico ortógrado depende directamente de un proceso de limpieza y desinfección, que supone la eliminación de microorganismos y de materia orgánica para permitir un sellado adecuado y tridimensional del espacio intraconducto y, así, promover la salud en los tejidos periapicales (1). A pesar de que, en endodoncia, la investigación clínica y tecnológica se ha desarrollado de manera acelerada en la última década, el resultado del tratamiento endodóntico ortógrado aún alcanza niveles de fracaso, que no satisfacen los estándares de calidad que la especialidad pretende alcanzar. En endodoncia, el fracaso está relacionado con la presencia de signos y síntomas clínicos y/o radiográficos, que plantean la exigencia de una segunda intervención, como el retratamiento ortógrado o retrógrado, o, en el peor escenario, la pérdida dental (1). En un análisis de supervivencia, Lee et al., 2012 (2) determinaron que la presencia de periodontitis apical persistente es la condición más prevalente que explica un resultado endodóntico adverso.
En general, el fracaso del tratamiento endodóntico primario ha sido descrito en diferentes poblaciones. En el año 2009, Da Silva et al. (3) determinaron fracaso del tratamiento endodóntico en un 21,43% para una muestra de 499 dientes tratados endodónticamente. A su vez, Ricucci et al. 2011 (4) reportaron un 10,9% de fracaso para una muestra de 816 dientes con tratamiento endodóntico ortógrado observados durante un periodo de 5 años. Por su parte, Moreno et al. 2013 (5) determinaron, para 1086 dientes tratados endodónticamente en una población colombiana, que el 49% presentó enfermedad postratamiento.
También se observa variabilidad entre los porcentajes de éxito y fracaso reportados en la literatura. Factores como presencia de patología periapical previa y mala calidad de la obturación endodóntica, entre otros, son determinantes en la aparición de fracaso endodóntico en un periodo de tiempo. En un trabajo publicado por Ng et al. 2011 (6) se estableció que la presencia de patología periapical previa disminuye el porcentaje de éxito del tratamiento endodóntico en un 49% en comparación con aquellos dientes que presentaron tejidos periapicales normales al momento de iniciar el tratamiento. Dos años después, Tsesis et al. 2013 (7) reportaron que en el 21% de los dientes con patología periapical preoperatoria no se registró radiográficamente reparación del tejido periapical. Adicionalmente, en cuanto a la asociación entre fracaso y calidad de la obturación, Zhong et al. 2008 (8) determinaron que, de 609 dientes analizados, el 11,2% presentó radiolucidez apical y, de este porcentaje, un 64,5% presentó una calidad de obturación insatisfactoria. Esto ha sido confirmado igualmente por el estudio realizado por Moreno et al. 2013 (5), donde el 54% de tratamientos con una inadecuada calidad de obturación fue clasificado como fracaso.
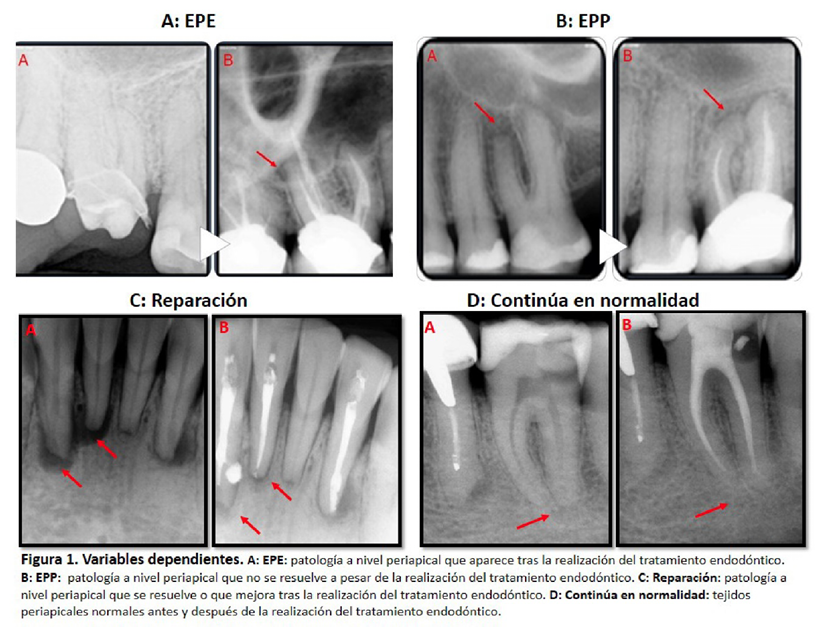
En el año 2014, Siqueira Jr. et al. (9) confirmaron que la enfermedad periapical radiográficamente observable aparece o persiste con posterioridad a la realización de un tratamiento endodóntico. Para mayor claridad, los autores establecen una diferencia entre la Enfermedad periapical emergente (EPE) —es decir, la patología que aparece tras la realización del tratamiento endodóntico (Figura 1a)—, y la Enfermedad periapical persistente (EPP) —donde, a pesar de la realización del tratamiento endodóntico, no se reconoce mejoría debido a que la lesión periapical previa no se resuelve (Figura 1b)—. El reconocimiento de la naturaleza de la enfermedad periapical pos-endodoncia y de las circunstancias anatómicas y mecánicas que favorecen su aparición, en conjunto con la intuición de que solo la EPE puede ser considerada como verdadero fracaso de un tratamiento endodóntico, permite cuestionar la validez de la distinción trazada entre EPE y EPP.
Tomando en cuenta estos antecedentes, el objetivo del presente trabajo consiste en identificar las características de la enfermedad periapical posterior al tratamiento endodóntico primario mediante la reconstrucción retrospectiva de la cohorte de dientes tratados endodónticamente que conforman la línea de pronóstico de la Especialidad en Endodoncia de la Facultad de Odontología de la Universidad Nacional de Colombia (FOUN).
Metodología
Se realizó un estudio observacional, de tipo cohorte y carácter retrospectivo, sobre una población de individuos con dientes permanentes con formación radicular completa y tratamiento endodóntico primario que asistieron a la Clínica de mantenimiento y control de la Línea de pronóstico de la Especialidad en Endodoncia de la FOUN. El registro clínico y radiográfico permitió la identificación del resultado postratamiento en un periodo de evaluación comprendido entre 1 y 16 años. Fueron excluidos los dientes con antecedentes de fractura vertical, trauma dentoalveolar y tratamiento de ortodoncia vigente, así como los dientes donde no fue posible recuperar la condición inicial periapical previa al tratamiento endodóntico y que contaban con periodos de control inferiores a 1 año. La unidad de estudio fue el diente. Esta investigación contó con un consentimiento informado y la aprobación del Comité de ética de la FOUN bajo Acta (B.CIEFO-261-16).
Se realizó un muestreo consecutivo en individuos con tratamiento endodóntico primario, recolectados en la base de datos de la Clínica de mantenimiento y control de la Línea de pronóstico de la Especialidad en Endodoncia de la FOUN. Se sometió a análisis un total de 232 dientes —correspondientes a 155 individuos— con tratamiento endodóntico primario, que contaron con registro clínico y radiográfico y que cumplieron los criterios de elegibilidad.
Los tratamientos observados fueron realizados por residentes de la Especialidad en Endodoncia de la FOUN bajo condiciones estandarizadas de acceso cameral, aislamiento absoluto y protocolo de irrigación con hipoclorito de sodio (NaOCl) al 5.25%, un lavado con agua desionizada, ácido etildiaminotetracético (EDTA) al 17% y un lavado final con agua desionizada.
Análisis de Datos
Dado el carácter observacional y exploratorio del presente estudio, y con el objetivo de establecer la frecuencia de las posibles categorías correlacionadas con el resultado del tratamiento endodóntico primario, un análisis de frecuencia estimó la prevalencia de estas para la población analizada. Los datos fueron recolectados como muestra secundaria bajo la lectura de historias clínicas y observación de radiografías periapicales.
La observación radiográfica postratamiento se llevó a cabo por parte de dos evaluadores ciegos bajo condiciones estandarizadas, mediante el sistema de radiografía digital Carestream RVG (Radio Visio Graphy® 5100® y software Dental Imaging de Carestream®), el cual opera a 60-63 Kv, 8mA y 0,25-0,32 segundos de exposición para una dosis de radiación de 0,033 mSv, dependiente del tipo y localización del diente. Las imágenes fueron tomadas con posicionadores XCP-DS Fit Endo Kit para Carestream RVG, lo que permitió garantizar una técnica de paralelismo. Las observaciones fueron almacenadas mediante una base de datos en archivo digital con Microsoft Excel (Microsoft® versión 2010).
Variables
Las variables independientes seleccionadas pertenecen a tres categorías: características basales, condiciones intraoperatorias y condiciones posperatorias. Las características basales observadas fueron: sexo, edad, tipo y localización del diente, diagnóstico inicial pulpar y periapical —según Guía para el diagnóstico clínico para patologías pulpares y periapicales (10)—, y condición periapical previa al tratamiento endodóntico —con lesión o sin lesión, de acuerdo con los criterios de Molven et al.; 1987 (11)—. Las condiciones intraoperatorias observadas fueron: presencia o ausencia de accidentes intraoperatorios del tercio apical, fractura de instrumento y escalón, número de citas en que se realizó el tratamiento endodóntico, y calidad de obturación, evaluada mediante tres criterios (12): homogeneidad —presencia o ausencia de espacios en la obturación observables radiográficamente— (13); conicidad —estrechamiento continuo del diámetro transversal del conducto radicular de cervical hasta apical— (14); y límite de obturación —distancia entre la extensión final del material de obturación y el ápice radiográfico—, dividido en tres categorías —corto: distancia mayor o igual a 2 mm; largo: distancia menor o igual a 0 mm—; a ras: distancia mayor que 0 mm y menor que 2 mm— (15). Para localizar el límite apical se definió el ápice radiográfico como el extremo anatómico más distal de la raíz (16). Por último, las condiciones posoperatorias observadas fueron: tipo de restauración —directa o indirecta—, rol de la restauración —individual o pilar de prótesis—, calidad de la restauración —adaptada o desadaptada—, presencia o ausencia de poste intrarradicular, y tiempo de evaluación.
La variable dependiente, por su parte, corresponde al resultado del tratamiento endodóntico primario. Esta variable se compone de cuatro categorías: EPE (Figura 1a), EPP (Figura 1b), Reparación (Figura 1c), y Continúa en normalidad (Figura 1d). De ellas, las dos primeras constituyen categorías de fracaso, mientras que las dos últimas constituyen categorías de éxito. Para la ponderación de esta variable se emplearon los criterios de Zuolo et al.; 2000 (17) y la clasificación de Siqueira Jr. et al.; 2014 (9).
Figura 1. Variables dependientes.
Resultados
La muestra total estuvo conformada por 232 dientes, aportados por 155 individuos. En general, se registró una tasa de fracaso del tratamiento endodóntico primario del 24%, distribuido en un 13,7% para EPE y 10,3%, para EPP. El 76% de la población presentó un resultado exitoso, con una distribución de 22,5% para la categoría Reparación y 53,5% para la categoría Continúa en normalidad. La Tabla 1, a continuación, muestra la distribución porcentual de los factores según las categorías de resultado.
Características basales
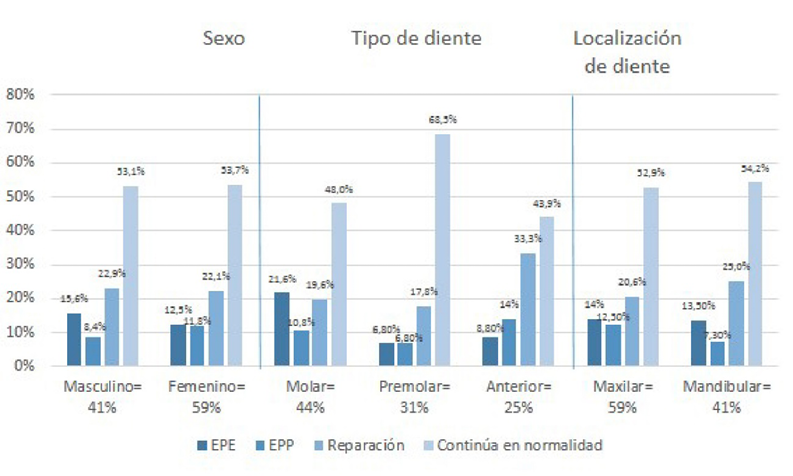
En la población estudiada, la distribución porcentual de individuos por sexo fue de 59% para femenino y 41% para masculino, y el promedio de edad fue de 55,8 años. Se registró que el 44% de los dientes analizados eran molares y el 59% se localizaban en el maxilar superior. Los diagnósticos iniciales pulpares y periapicales más frecuentes fueron necrosis pulpar (34%) y tejido apical normal (63%) (Figura 2).
|
Tabla 1. Distribución de los factores y su categorización en las variables resultado. |
|||||||||
|
*: Necrosis pulpar, †: pulpitis irreversible sintomática, ‡: pulpitis irreversible asintomática, ¶: pulpa normal, **: periodontitis apical sintomática, ††: periodontitis apical asintomática; ‡‡: absceso apical agudo, ¶¶: absceso apical crónico, ***: tejido apical normal. |
|||||||||
|
FACTORES / N: 232 |
N (%) |
FRACASO 56 (24%) |
ÉXITO 176 (76%) |
||||||
|
EMERGENTE |
PERSISTENTE 24 (10,3%) |
REPARACIÓN |
CONTINÚA EN NORMALIDAD 124 (53,5%) |
||||||
|
SEXO |
|||||||||
|
MASCULINO |
96 (41) |
15 |
(15,6) |
8 |
(8,4) |
22 |
(22,9) |
51 |
(53,1) |
|
FEMENINO |
136 (59) |
17 |
(12,5) |
16 |
(11,8) |
30 |
(22,1) |
73 |
(53,7) |
|
TIPO DE DIENTE |
|||||||||
|
MOLAR |
102 (44) |
22 |
(21,6) |
11 |
(10,8) |
20 |
(19,6) |
49 |
(48) |
|
PREMOLAR |
73 (31) |
5 |
(6,8) |
5 |
(6,8) |
13 |
(17,8) |
50 |
(68,5) |
|
ANTERIOR |
57 (25) |
5 |
(8,8) |
8 |
(14) |
19 |
(33,3) |
25 |
(43,9) |
|
LOCALIZACIÓN DEL DIENTE |
|||||||||
|
MAXILAR |
136 (59) |
19 |
(14,0) |
17 |
(12,5) |
28 |
(20,6) |
72 |
(52,9) |
|
MANDIBULAR |
96 (41) |
13 |
(13,5) |
7 |
(7,3) |
24 |
(25) |
52 |
(54,2) |
|
DIAGNÓSTICO PULPAR INICIAL |
|||||||||
|
NP* |
80 (34) |
0 |
(0,0) |
24 |
(30) |
47 |
(58,8) |
9 |
(11,3) |
|
PIS† |
71 (31) |
15 |
(21,1) |
0 |
(0) |
1 |
(1,4) |
55 |
(77,5) |
|
PIA‡ |
58 (25) |
13 |
(22,4) |
0 |
(0) |
0 |
(0) |
45 |
(77,6) |
|
PN¶ |
23 (10) |
4 |
(17,4) |
0 |
(0) |
4 |
(17,4) |
15 |
(65,2) |
|
DIAGNÓSTICO PERIAPICAL INICIAL |
|||||||||
|
PAS** |
26 (11) |
0 |
(0,0) |
7 |
(26,9) |
12 |
(46,2) |
7 |
(26,9) |
|
PAA†† |
33 (14) |
0 |
(0,0) |
11 |
(33,3) |
19 |
(57,6) |
3 |
(9,1) |
|
AAA‡‡ |
8 (3) |
0 |
(0,0) |
1 |
(12,5) |
7 |
(87,5) |
0 |
(0) |
|
AAC¶¶ |
19 (8) |
0 |
(0,0) |
5 |
(26,3) |
14 |
(73,7) |
0 |
(0) |
|
TAN*** |
146 (63) |
32 |
(21,9) |
0 |
(0) |
0 |
(0) |
114 |
(78,1) |
|
ESTADO PERIAPICAL PREVIO |
|||||||||
|
CON LESIÓN |
76 (33) |
0 |
(0,0) |
24 |
(31,6) |
52 |
(68,4) |
0 |
(0) |
|
SIN LESIÓN |
156 (67) |
32 |
(20,5) |
0 |
(0) |
0 |
(0) |
124 |
(79,5) |
|
NÚMERO DE CITAS |
|||||||||
|
1 |
140 (60) |
31 |
(22,1) |
0 |
(0) |
0 |
(0) |
109 |
(77,9) |
|
2 |
90 (39) |
1 |
(1,1) |
22 |
(24,4) |
52 |
(57,8) |
15 |
(16,7) |
|
3 |
2 (1) |
0 |
(0,0) |
2 |
(100) |
0 |
(0) |
0 |
(0) |
|
LÍMITE DE OBTURACIÓN |
|||||||||
|
CORTO |
46 (20) |
25 |
(54,3) |
9 |
(19,6) |
4 |
(8,7) |
8 |
(17,4) |
|
LARGO |
13 (6) |
1 |
(7,7) |
3 |
(23,1) |
3 |
(23,1) |
6 |
(46,2) |
|
A RAS |
173 (74) |
6 |
(3,5) |
12 |
(6,9) |
45 |
(26) |
110 |
(63,6) |
|
HOMOGENEIDAD DE OBTURACIÓN |
|||||||||
|
INADECUADA |
23 (10) |
12 |
(52,2) |
5 |
(21,7) |
1 |
(4,3) |
5 |
(21,7) |
|
ADECUADA |
209 (90) |
20 |
(9,6) |
19 |
(9,1) |
51 |
(24,4) |
119 |
(56,9) |
|
CONICIDAD DE OBTURACIÓN |
|||||||||
|
INADECUADA |
13 (6) |
9 |
(69,2) |
2 |
(15,4) |
0 |
(0) |
2 |
(15,4) |
|
ADECUADA |
219 (94) |
23 |
(10,5) |
22 |
(10,0) |
52 |
(23,7) |
122 |
(55,7) |
|
ESCALÓN |
|||||||||
|
SÍ |
12 (5) |
6 |
(50,0) |
0 |
(0,0) |
3 |
(25) |
3 |
(25) |
|
NO |
220 (95) |
26 |
(11,8) |
24 |
(10,9) |
49 |
(22,3) |
121 |
(55) |
|
FRACTURA DE INSTRUMENTO |
|||||||||
|
SÍ |
21 (9) |
2 |
(9,5) |
5 |
(23,8) |
2 |
(9,5) |
12 |
(57,1) |
|
NO |
211 (91) |
30 |
(14,2) |
19 |
(9,0) |
50 |
(23,7) |
112 |
(53,1) |
|
TIPO DE RESTAURACIÓN |
|||||||||
|
DIRECTA |
86 (37) |
6 |
(7,0) |
12 |
(14,0) |
23 |
(26,7) |
45 |
(52,3) |
|
INDIRECTA |
146 (63) |
26 |
(17,8) |
12 |
(8,2) |
29 |
(19,9) |
79 |
(54,1) |
|
POSTE INTRARRADICULAR |
|||||||||
|
SÍ |
124 (53) |
21 |
(16,9) |
11 |
(8,9) |
21 |
(16,9) |
71 |
(57,3) |
|
NO |
108 (47) |
11 |
(10,2) |
13 |
(12,0) |
31 |
(28,7) |
53 |
(49,1) |
|
ROL DE LA RESTAURACIÓN |
|||||||||
|
PILAR DE PRÓTESIS |
21 (9) |
5 |
(23,8) |
1 |
(4,8) |
6 |
(28,6) |
9 |
(42,9) |
|
INDIVIDUAL |
211 (91) |
27 |
(12,8) |
23 |
(10,9) |
46 |
(21,8) |
115 |
(54,5) |
|
CALIDAD DE LA RESTAURACIÓN |
|||||||||
|
DESADAPTADA |
17 (7) |
5 |
(29,4) |
3 |
(17,6) |
2 |
(11,8) |
7 |
(41,2) |
|
ADAPTADA |
215 (93) |
27 |
(12,6) |
21 |
(9,8) |
50 |
(23,3) |
117 |
(54,4) |
|
TIEMPO DE CONTROL |
|||||||||
|
< 5 AÑOS |
142 (61) |
17 |
(12,0) |
18 |
(12,7) |
31 |
(21,8) |
76 |
(53,5) |
|
5– 10 AÑOS |
56 (24) |
10 |
(17,9) |
5 |
(8,9) |
11 |
(19,6) |
30 |
(53, 6) |
|
> 10 AÑOS |
34 (15) |
5 |
(14,7) |
1 |
(2,9) |
10 |
(29,4) |
18 |
(52,9) |
Figura 2. Distribución de las características basales y su categorización en las variables resultado.
Condiciones intraoperatorias
De los tratamientos realizados, el 60% fue realizado en una única cita. En cuanto a la calidad de obturación, se observó que el 74% tenía una longitud de obturación a ras (Figura 3), mientras que el 90% y 94% presentaron homogeneidad y conicidad adecuadas, respectivamente (Figura 4). Los accidentes intraoperatorios, escalón (5%) y fractura de instrumento (9%), fueron poco frecuentes.
Consideraciones posoperatorias
De los dientes analizados, el 63% presentó restauraciones indirectas, el 53%, retenedor intrarradicular; el 91%, restauraciones individuales; y el 93%, restauración coronal adaptada. El 61% de los tratamientos fue evaluado en un tiempo menor a 5 años.
Figura 3. Distribución del límite apical y categorización del mismo en las variables resultado.
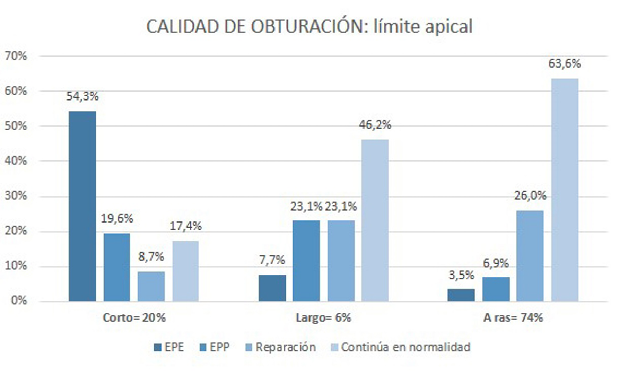
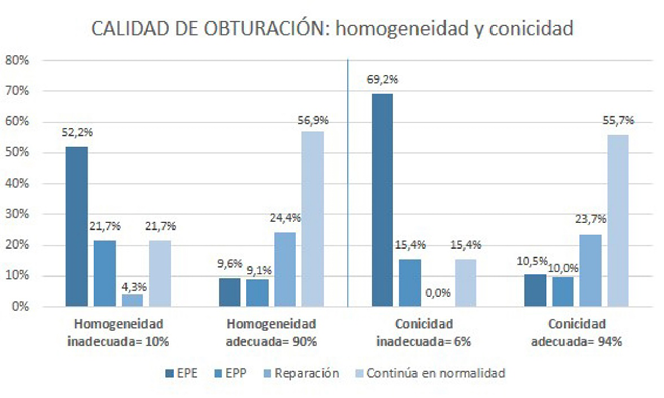
Figura 4. Distribución de homogeneidad y conicidad y categorización de las mismas en las variables resultado.
Discusión
Se realizó un estudio observacional de tipo cohorte retrospectivo, que exploró una población de 155 pacientes con 232 dientes que presentaron tratamiento endodóntico primario. Por tratarse de un estudio de caracterización, se identificaron los rasgos de la población analizada con el objetivo de establecer la diferencia entre la persistencia y la emergencia de la enfermedad periapical postratamiento.
De manera general, fue posible establecer que, de los dientes con tratamiento endodóntico primario observados en un periodo entre 1 y 16 años, el 24% presentó fracaso. Por su parte, el resultado del tratamiento endodóntico se distribuyó de la siguiente manera: 13,7% para EPE, 10,3% para EPP, 22,5% para Reparación, y 53,5% para Continúa en normalidad (Tabla 1).
En comparación con el 24% de fracaso del tratamiento endodóntico primario de la población de estudio analizada, Marquis et al.; 2006 (18) registraron un 14% de enfermedad periapical postratamiento. Así mismo, Ng et al.; 2007 (19), en una revisión sistemática, postulan un porcentaje de fracaso que oscila entre 15% y 32% después de un año de control. Recientemente, Azim et al.; 2016 (20) determinaron un porcentaje de fracaso del 22%, resultado que no ofrece discriminación entre los tratamientos primario y secundario (retratamiento).
La categorización de la enfermedad periapical postratamiento permitió identificar un porcentaje mayor del 3,4% de la EPE, sobre la EPP, diferencia descrita teóricamente por Siqueira et al.; 2014 (9), quienes reconocieron el carácter de la EPE como infección secundaria que aparece con posterioridad a un tratamiento endodóntico realizado en un diente que se encontraba libre de contaminación bacteriana. En contraste con la EPE, la EPP confirma la resistencia de la flora bacteriana al tratamiento endodóntico y, por lo tanto, se asocia con una mala calidad de la obturación visible radiográficamente, o con la persistencia de la enfermedad a pesar de que los estándares de tratamiento se consideren óptimos (21).
Estas evidencias sugieren que la EPE podría ser considerada como el verdadero fracaso del tratamiento endodóntico. Sobre este supuesto, el análisis de las características basales y condiciones intra y posoperatorias de la población estudiada adquiere relevancia.
Características basales
Pese a que, en la muestra analizada en el presente estudio, la población femenina superó a la masculina en un 18%, se observó que, para el caso de los hombres y en contraste con el de las mujeres, el porcentaje de aparición de la enfermedad supera al de la persistencia de la misma con un 15,6%. Al respecto, Marquis et al.; 2006 (18), reconocen, con una diferencia significativa (P= 0,04), mayor prevalencia de la enfermedad para los hombres. Tales resultados coinciden con los hallazgos de Hummonenn et al.; 2017 (22), y de Van der Veken, et al.; 2017 (23), quienes registraron una mayor asociación de la enfermedad en la población masculina, en comparación con la femenina (P=<0,001). La población analizada presentó un promedio de edad de 55,8 años, lo que podría indicar que, a mayor edad, el fracaso del tratamiento endodóntico primario es más prevalente, lo que coincide con la relación proporcional reportada en el ENSAB IV (24). En el presente estudio, la presencia de fracaso del tratamiento en molares superiores se hizo patente. En cuanto a ello, se ha registrado mayor prevalencia de la enfermedad periapical postratamiento en molares —en comparación con dientes anteriores— (23, 25).
La categoría de diagnóstico que generó mayor fracaso endodóntico fue la necrosis pulpar (34%), seguida de la inflamación pulpar de tipo irreversible, sintomática (31%) y asintomática (25%). Tomando en cuenta que un 10% de los dientes con pulpa normal generó enfermedad, es claro que la presencia tanto de bacterias como de inflamación de tipo irreversible puede generar el fracaso en endodoncia. Los resultados coinciden con los hallazgos de Azim et al.; 2016 (20), quienes reconocen una diferencia significativa (P= 0.001) entre el fracaso del tratamiento endodóntico para dientes vitales (5,6%) y no vitales (27,9%). Por su parte, Ng et al.; 2008 (26) determinan una prevalencia de enfermedad entre el 10% y el 15% para dientes vitales y no vitales sin presencia de patología periapical previa.
Condiciones intraoperatorias
El 20% de los tratamientos analizados presentó una longitud de obturación corta, y la categorización de este valor puso en evidencia que el 54,3% se relacionó con la categoría EPE. De este hallazgo puede inferirse que una longitud de obturación corta influye de manera importante en el pronóstico del tratamiento endodóntico. Lo contrario sucede para el caso de la longitud de obturación larga, para la cual pudo observarse relación con la persistencia de la enfermedad (23,1%). Al respecto, se ha reportado que la longitud de obturación inadecuada es un factor que se relaciona significativamente con fracaso del tratamiento (P<0,001) (26, 27) (Figura 3).
De los dientes analizados en el presente estudio, 90% y 94% de los registros correspondieron a homogeneidad y conicidad adecuadas, respectivamente (Figura 4). Tal evidencia sugiere que estos factores podrían llegar a influir en la aparición de la enfermedad, sin la contundencia que demostró el límite apical. Ng et al.; 2008 (26) encuentran asociación entre el fracaso del tratamiento endodóntico primario y una inadecuada obturación endodóntica. Por su parte, Kirkevang et al.; 2017 (27) relacionan significativamente la presencia de espacios en la obturación endodóntica con el fracaso del tratamiento (P<0,001). En contraste, Hoskinson et al.; 2002 (28) no encuentran diferencia significativa en los resultados del tratamiento endodóntico para los casos de una preparación estrecha y una cónica.
La presente caracterización parece sugerir que Límite de la obturación endodóntica es la categoría que podría establecer una asociación con la presencia de enfermedad postratamiento; sin embargo, esta afirmación debe ser explorada bajo un análisis estadístico.
La presencia de accidentes intraoperatorios del tercio apical, como el escalón y la fractura de instrumento, fueron registrados con un 5% y 9%, respectivamente. Resulta interesante observar que el 50% de los dientes con presencia de escalones se relacionaron con EPE, lo que sugiere que estos podrían tener incidencia en el resultado del tratamiento endodóntico primario. Adicionalmente, estudios que respaldan los resultados de la presente investigación concluyen que hay una relación significativa (P<0,001) entre los errores intraoperatorios y el aumento del riesgo de fracaso endodóntico (18, 20).
Condiciones posoperatorias
La muestra analizada en el presente estudio permitió determinar los siguientes valores: 63% de las restauraciones coronales eran indirectas, el 53% tenían retenedor intrarradicular, el 91% de dientes analizados presentaban restauraciones individuales y, de ellas, el 93% estaban adaptadas; lo que da a entender que el estado de la restauración no influye de manera importante en el resultado del tratamiento endodóntico primario. De la misma forma, se ha reportado que la calidad y el tipo de relación no se asocian de manera significativa con la presencia de periodontitis apical postratamiento (27, 29).
En referencia al tiempo de observación, se registraron los siguientes valores: el 61% de los dientes se analizaron en un periodo menor a 5 años, el 24% se evaluó en un periodo de 5 a 10 años, y el 15% restante correspondió a dientes controlados por más de 10 años. Fue interesante observar que el análisis de este último grupo desde la perspectiva del fracaso arrojó que la categoría EPE es porcentualmente mayor (14,7%) a la categoría EPP (2,9%), lo que sugiere que, aun después de varios años de realizado el tratamiento endodóntico, la enfermedad puede presentarse de manera asintomática (diente funcional) (30).
A pesar de las limitaciones de la presente investigación, se puede concluir que:
- se encontró que, de los dientes con tratamiento endodóntico primario observados, el 24% presentó enfermedad periapical postratamiento;
- es posible categorizar el fracaso del tratamiento endodóntico primario mediante las categorías EPE y EPP;
- la longitud de obturación corta resultó ser el factor intraoperatorio más frecuente en la aparición de la enfermedad periapical postratamiento;
- en comparación con la enfermedad periapical persistente, la enfermedad periapical emergente exhibió una frecuencia mayor, por lo que se reconoce esta última como el verdadero fracaso del tratamiento endodóntico primario.
Recomendaciones
Se recomienda realizar un estudio de carácter analítico que explore la asociación entre las categorías del resultado endodóntico propuestas y los factores clínicos inherentes al paciente, al diente o a las condiciones del tratamiento endodóntico.
Agradecimientos
Este trabajo fue desarrollado en la Universidad Nacional de Colombia, como parte del macroproyecto “Investigación en endodoncia clínica, pronóstico del tratamiento endodóntico en sus tres dimensiones, primario, secundario; ortógrado y retrógrado”, código: 34933, código Quipu: 201010026625. Esta iniciativa resultó favorecida en la Convocatoria nacional de proyectos para el fortalecimiento de la investigación, creación e innovación de la Universidad Nacional de Colombia 2016-2018.
Los autores no declaramos conflicto de intereses.
Referencias
- Chandra A. Discuss the factors that affect the outcome of endodontic treatment. Aust Endod J 2009; 35(2): 98-107. https://doi.org/10.1111/j.1747 4477.2009.00199.x.
- Lee AH, Cheung GS, Wong MC. Long-term outcome of primary non-surgical root canal treatment. Clin Oral Investig 2012; 16(6): 1607-1617. https://doi.org/10.1007/s00784-011-0664-2
- Da Silva K, Lam JM, Wu N, Duckmanton P. Cross-sectional study of endodontic treatment in an Australian population. Aust Endod J 2009; 35(3): 140-146. https://doi.org/10.1111/j.1747-4477.2009.00215.x.
- Ricucci D, Russo J, Rutberg M, Burleson JA, Spangberg LS. A prospective cohort study of endodontic treatments of 1,369 root canals: results after 5 years. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2011; 112(6): 825-842. https://doi.org/10.1016/j.tripleo.2011.08.003.
- Moreno JO, Alves FR, Goncalves LS, Martínez AM, Rocas IN, Siqueira JF, Jr. Periradicular status and quality of root canal fillings and coronal restorations in an urban Colombian population. J Endod 2013; 39(5): 600-604.https://doi.org/10.1016/j.joen.2012.12.020.
- Ng YL, Mann V, Gulabivala K. A prospective study of the factors affecting outcomes of nonsurgical root canal treatment: part 1: periapical health. Int Endod J 2011; 44(7): 583-609. https://doi.org/10.1111/j.1365-2591.2011.01872.x
- Tsesis I, Goldberger T, Taschieri S, Seifan M, Tamse A, Rosen E. The dynamics of periapical lesions in endodontically treated teeth that are left without intervention: a longitudinal study. J Endod 2013; 39(12): 1510-1515. https://doi.org/10.1016/j.joen.2013.09.010
- Zhong Y, Chasen J, Yamanaka R, Garcia R, Kaye EK, Kaufman JS, et al. Extension and density of root fillings and postoperative apical radiolucencies in the Veterans Affairs Dental Longitudinal Study. J Endod 2008; 34(7): 798-803. https://doi.org/10.1016/j.joen.2008.03.022
- Siqueira JF, Rocas IN, Ricucci D, Hulsmann M. Causes and management of post-treatment apical periodontitis. Br Dent J 2014; 216(6): 305-312. https://doi.org/10.1038/sj.bdj.2014.200
- Marroquín T GC. Guidelines for clinical diagnosis of pulp and periapical pathologies. adapted and updated from the «consensus conference recommended diagnostic terminology» published by the American Association of Endodontists. Rev Fac Odontol Univ Antioquia 2015: 26(2): 398-442.
- Molven O, Halse A, Grung B. Observer strategy and the radiographic classification of healing after endodontic surgery. Int J Oral Maxillofac Surg 1987; 16(4): 432-439. https://doi.org/10.1016/S0901-5027(87)80080-2
- Robia G. Comparative radiographic assessment of root canal obturation quality: manual verses rotary canal preparation technique. Int J Biomed Sci 2014; 10(2): 136-142.
- Santos SM, Soares JA, Costa GM, Brito-Junior M, Moreira AN, de Magalhaes CS. Radiographic parameters of quality of root canal fillings and periapical status: a retrospective cohort study. J Endod 2010; 36(12):1932-1937. https://doi.org/10.1016/j.joen.2010.08.050.
- Schilder H. Filling root canals in three dimensions. Dent Clin North Am 1967: 723-744.
- Sjogren U, Hagglund B, Sundqvist G, Wing K. Factors affecting the long-term results of endodontic treatment. J Endod 1990; 16(10): 498-504. https://doi.org/10.1016/S0099-2399(07)80180-4
- Olson AK, Cavataio RE, Luciano J. The ability of the radiograph to determine the location of the apical foramen. Int Endod J 1991; 24(1): 28-35. https://doi.org/10.1111/j.1365-2591.1991.tb00867.x
- Zuolo ML, Ferreira MO, Gutmann JL. Prognosis in periradicular surgery: a clinical prospective study. Int Endod J 2000; 33(2): 91-98. https://doi.org/10.1046/j.1365-2591.2000.00263.x
- Marquis VL, Dao T, Farzaneh M, Abitbol S, Friedman S. Treatment outcome in endodontics: the Toronto Study. Phase III: initial treatment. J Endod 2006; 32(4): 299-306. https://doi.org/10.1016/j.joen.2005.10.050
- Ng YL, Mann V, Rahbaran S, Lewsey J, Gulabivala K. Outcome of primary root canal treatment: systematic review of the literature - part 1. Effects of study characteristics on probability of success. Int Endod J 2007; 40(12): 921-939. https://doi.org/10.1111/j.1365-2591.2007.01322.x
- Azim AA, Griggs JA, Huang GT. The Tennessee study: factors affecting treatment outcome and healing time following nonsurgical root canal treatment. Int Endod J 2016; 49(1): 6-16. https://doi.org/10.1111/iej.12429
- Nair PN, Sjogren U, Krey G, Kahnberg KE, Sundqvist G. Intraradicular bacteria and fungi in root-filled, asymptomatic human teeth with therapy-resistant periapical lesions: a long-term light and electron microscopic follow-up study. J Endod 1990; 16(12): 580-588. https://doi.org/10.1016/S0099-2399(07)80201-9
- Huumonen S, Suominen AL, Vehkalahti MM. Prevalence of apical periodontitis in root filled teeth: findings from a nationwide survey in Finland. Int Endod J 2017; 50(3): 229-236. https://doi.org/10.1111/iej.12625
- Van der Veken D CF, Fieuws S, Lambrechts P. Prevalence of apical periodontitis and root filled teeth in a Belgian subpopulation found on CBCT images. International Endodontic Journal 2017; 50(4): 317–329. https://doi.org/10.1111/iej.12631
- República de Colombia - Ministerio de Salud. IV Estudio Nacional de Salud Bucal. Situación en Salud Bucal. Bogotá; 2015 [Available from: https://www.minsalud.gov.co/sites/rid/Lists/BibliotecaDigital/RIDE/VS/PP/ENSAB-IV-Situacion-Bucal-Actual.pdf
- Hussein FE, Liew AK, Ramlee RA, Abdullah D, Chong BS. Factors Associated with Apical Periodontitis: A Multilevel Analysis. J Endod 2016; 42(10): 1441-1445. https://doi.org/10.1016/j.joen.2016.07.009
- Ng YL, Mann V, Rahbaran S, Lewsey J, Gulabivala K. Outcome of primary root canal treatment: systematic review of the literature -- Part 2. Influence of clinical factors. Int Endod J 2008; 41(1): 6-31. https://doi.org/10.1111/j.1365-2591.2007.01323.x
- Kirkevang LL, Orstavik D, Bahrami G, Wenzel A, Vaeth M. Prediction of periapical status and tooth extraction. Int Endod J 2017; 50(1): 5-14. https://doi.org/10.1111/iej.12581
- Hoskinson SE, Ng YL, Hoskinson AE, Moles DR, Gulabivala K. A retrospective comparison of outcome of root canal treatment using two different protocols. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2002; 93(6): 705-715. https://doi.org/10.1067/moe.2001.122822
- Timmerman A, Calache H, Parashos P. A cross sectional and longitudinal study of endodontic and periapical status in an Australian population. Aust Dent J 2017; 62(3): 345-354. https://doi.org/10.1111/adj.12512
- Friedman S, Mor C. The success of endodontic therapy--healing and functionality. J Calif Dent Assoc 2004;32(6): 493-503.
Referencias
Chandra A. Discuss the factors that affect the outcome of endodontic treatment. Aust Endod J 2009; 35(2): 98-107. https://doi.org/10.1111/j.17474477.2009.00199.x.
Lee AH, Cheung GS, Wong MC. Long-term outcome of primary non-surgical root canal treatment. Clin Oral Investig 2012; 16(6): 1607-1617. https://doi.org/10.1007/s00784-011-0664-2
Da Silva K, Lam JM, Wu N, Duckmanton P. Cross-sectional study of endodontic treatment in an Australian population. Aust Endod J 2009; 35(3): 140-146. https://doi.org/10.1111/j.1747-4477.2009.00215.x.
Ricucci D, Russo J, Rutberg M, Burleson JA, Spangberg LS. A prospective cohort study of endodontic treatments of 1,369 root canals: results after 5 years. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2011; 112(6): 825-842. https://doi.org/10.1016/j.tripleo.2011.08.003.
Moreno JO, Alves FR, Goncalves LS, Martínez AM, Rocas IN, Siqueira JF, Jr. Periradicular status and quality of root canal fillings and coronal restorations in an urban Colombian population. J Endod 2013; 39(5): 600-604. https://doi.org/10.1016/j.joen.2012.12.020.
Ng YL, Mann V, Gulabivala K. A prospective study of the factors affecting outcomes of nonsurgical root canal treatment: part 1: periapical health. Int Endod J 2011; 44(7): 583-609. https://doi.org/10.1111/j.1365-2591.2011.01872.x
Tsesis I, Goldberger T, Taschieri S, Seifan M, Tamse A, Rosen E. The dynamics of periapical lesions in endodontically treated teeth that are left without intervention: a longitudinal study. J Endod 2013; 39(12): 1510-1515. https://doi.org/10.1016/j.joen.2013.09.010
Zhong Y, Chasen J, Yamanaka R, Garcia R, Kaye EK, Kaufman JS, et al. Extension and density of root fillings and postoperative apical radiolucencies in the Veterans Affairs Dental Longitudinal Study. J Endod 2008; 34(7): 798-803. https://doi.org/10.1016/j.joen.2008.03.022
Siqueira JF, Rocas IN, Ricucci D, Hulsmann M. Causes and management of post-treatment apical periodontitis. Br Dent J 2014; 216(6): 305-312. https://doi.org/10.1038/sj.bdj.2014.200
Marroquín T GC. Guidelines for clinical diagnosis of pulp and periapical pathologies. adapted and updated from the «consensus conference recommended diagnostic terminology» published by the American Association of Endodontists. Rev Fac Odontol Univ Antioquia 2015: 26(2): 398-442.
Molven O, Halse A, Grung B. Observer strategy and the radiographic classification of healing after endodontic surgery. Int J Oral Maxillofac Surg 1987; 16(4): 432-439. https://doi.org/10.1016/S0901-5027(87)80080-2
Robia G. Comparative radiographic assessment of root canal obturation quality: manual verses rotary canal preparation technique. Int J Biomed Sci 2014; 10(2): 136-142.
Santos SM, Soares JA, Costa GM, Brito-Junior M, Moreira AN, de Magalhaes CS. Radiographic parameters of quality of root canal fillings and periapical status: a retrospective cohort study. J Endod 2010; 36(12):1932-1937. https://doi.org/10.1016/j.joen.2010.08.050.
Schilder H. Filling root canals in three dimensions. Dent Clin North Am 1967: 723-744.
Sjogren U, Hagglund B, Sundqvist G, Wing K. Factors affecting the long-term results of endodontic treatment. J Endod 1990; 16(10): 498-504. https://doi.org/10.1016/S0099-2399(07)80180-4
Olson AK, Cavataio RE, Luciano J. The ability of the radiograph to determine the location of the apical foramen. Int Endod J 1991; 24(1): 28-35. https://doi.org/10.1111/j.1365-2591.1991.tb00867.x
Zuolo ML, Ferreira MO, Gutmann JL. Prognosis in periradicular surgery: a clinical prospective study. Int Endod J 2000; 33(2): 91-98. https://doi.org/10.1046/j.1365-2591.2000.00263.x
Marquis VL, Dao T, Farzaneh M, Abitbol S, Friedman S. Treatment outcome in endodontics: the Toronto Study. Phase III: initial treatment. J Endod 2006; 32(4): 299-306. https://doi.org/10.1016/j.joen.2005.10.050
Ng YL, Mann V, Rahbaran S, Lewsey J, Gulabivala K. Outcome of primary root canal treatment: systematic review of the literature - part 1. Effects of study characteristics on probability of success. Int Endod J 2007; 40(12): 921-939. https://doi.org/10.1111/j.1365-2591.2007.01322.x
Azim AA, Griggs JA, Huang GT. The Tennessee study: factors affecting treatment outcome and healing time following nonsurgical root canal treatment. Int Endod J 2016; 49(1): 6-16. https://doi.org/10.1111/iej.12429
Nair PN, Sjogren U, Krey G, Kahnberg KE, Sundqvist G. Intraradicular bacteria and fungi in root-filled, asymptomatic human teeth with therapy-resistant periapical lesions: a long-term light and electron microscopic follow-up study. J Endod 1990; 16(12): 580-588. https://doi.org/10.1016/S0099-2399(07)80201-9
Huumonen S, Suominen AL, Vehkalahti MM. Prevalence of apical periodontitis in root filled teeth: findings from a nationwide survey in Finland. Int Endod J 2017; 50(3): 229-236. https://doi.org/10.1111/iej.12625
Van der Veken D CF, Fieuws S, Lambrechts P. Prevalence of apical periodontitis and root filled teeth in a Belgian subpopulation found on CBCT images. International Endodontic Journal 2017; 50(4): 317-329. https://doi.org/10.1111/iej.12631
Ministerio de Salud-Colombia. IV Estudio Nacional de Salud Bucal. Situación en Salud Bucal. Bogotá; 2015 [Available from: https://www.minsalud.gov.co/sites/rid/Lists/BibliotecaDigital/RIDE/VS/PP/ENSAB-IV-Situacion-Bucal-Actual.pdf.
Hussein FE, Liew AK, Ramlee RA, Abdullah D, Chong BS. Factors Associated with Apical Periodontitis: A Multilevel Analysis. J Endod 2016; 42(10): 1441-1445. https://doi.org/10.1016/j.joen.2016.07.009
Ng YL, Mann V, Rahbaran S, Lewsey J, Gulabivala K. Outcome of primary root canal treatment: systematic review of the literature -- Part 2. Influence of clinical factors. Int Endod J 2008; 41(1): 6-31. https://doi.org/10.1111/j.1365-2591.2007.01323.x
Kirkevang LL, Orstavik D, Bahrami G, Wenzel A, Vaeth M. Prediction of periapical status and tooth extraction. Int Endod J 2017; 50(1): 5-14. https://doi.org/10.1111/iej.12581
Hoskinson SE, Ng YL, Hoskinson AE, Moles DR, Gulabivala K. A retrospective comparison of outcome of root canal treatment using two different protocols. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2002; 93(6): 705-715. https://doi.org/10.1067/moe.2001.122822
Timmerman A, Calache H, Parashos P. A cross sectional and longitudinal study of endodontic and periapical status in an Australian population. Aust Dent J 2017; 62(3): 345-354. DOI: 10.1111/adj.12512
Friedman S, Mor C. The success of endodontic therapy--healing and functionality. J Calif Dent Assoc 2004;32(6): 493-503.
Cómo citar
APA
ACM
ACS
ABNT
Chicago
Harvard
IEEE
MLA
Turabian
Vancouver
Descargar cita
CrossRef Cited-by
1. Francisco Alfredo Ceballos Soledispa, Alba María Mendoza Castro. (2026). Anomalías en la anatomía de conductos radiculares y su preparación química – mecánica. Salud & Ciencias Médicas, , p.12. https://doi.org/10.56124/saludcm.v5i8.002.
2. Mateo Leonidas Flores Sacoto, Paola Alexandra Duran Neira, Magda Zulay Bastidas Calva, Diana Patricia Álvarez Álvarez. (2024). Innovación odontológica: impresión 3D de dientes caninos para mejorar la formación endodóntica. Anatomía Digital, 7(3), p.120. https://doi.org/10.33262/anatomiadigital.v7i3.3150.
Dimensions
PlumX
Visitas a la página del resumen del artículo
Descargas
Licencia
Derechos de autor 2019 José Antonio Sánchez Alemán, Claudia Carmiña García-Guerrero

Esta obra está bajo una licencia internacional Creative Commons Atribución-NoComercial-SinDerivadas 4.0.
Aquellos autores/as que tengan publicaciones con esta revista, aceptan los términos siguientes:
- Los autores/as conservarán sus derechos de autor y garantizarán a la revista el derecho de primera publicación de su obra, el cuál estará simultáneamente sujeto a la licencia Reconocimiento-NoComercial-SinObraDerivada 4.0 Internacional que permite a terceros compartir la obra siempre que se indique su autor y su primera publicación esta revista.
- Los autores/as podrán adoptar otros acuerdos de licencia no exclusiva de distribución de la versión de la obra publicada (p. ej.: depositarla en un archivo telemático institucional o publicarla en un volumen monográfico) siempre que se indique la publicación inicial en esta revista.
- Se permite y recomienda a los autores/as difundir su obra a través de Internet (p. ej.: en archivos telemáticos institucionales o en su página web) antes y durante el proceso de envío, lo cual puede producir intercambios interesantes y aumentar las citas de la obra publicada. (Véase El efecto del acceso abierto).
- Una vez sometido el artículo no se aceptaran cambios respecto a la incorporación o retiro de autores.






















