Operations research as a decision-making tool in the health sector: A state of the art
La utilización de la Investigación de Operaciones como soporte a la toma de decisiones en el sector salud: un estado del arte
DOI:
https://doi.org/10.15446/dyna.v84n201.57504Palabras clave:
Application, Decision Making, Health, Review (en)Aplicación, Toma de Decisiones, Salud, Revisión (es)
Descargas
Recibido: 8 de junio de 2016; Revisión recibida: 20 de octubre de 2016; Aceptado: 19 de diciembre de 2016
Abstract
The contributions of Operations Research (OR) in the healthcare field have been extensively studied in the scientific literature since the 1960s, covering decision support tools with operational, tactical, and strategic approaches. The aim of this article is to analyze the historical development of the application of OR models in healthcare. The application trends for optimization, planning, and decision- making models are studied through a descriptive literature review and a bibliometric analysis of scientific papers published between 1952 and 2016. An upward trend in the usage of operational models is observed with the predominance of resource optimization approaches and strategic decision-making for public health.
Keywords :
Application, Decision Making, Health, Review.Resumen
Los aportes de la Investigación de Operaciones (IO) en el campo de la salud han sido ampliamente estudiados en la literatura científica desde la década de 1960, abarcando herramientas para el soporte a la decisión en enfoques operacionales, tácticos y estratégicos. El objetivo de este artículo es analizar el avance y el desarrollo histórico del uso de modelos operativos en el campo de la salud. A través de una revisión bibliográfica descriptiva y un análisis bibliométrico de artículos científicos publicados durante el periodo 1952-2016, se estudia el comportamiento de las tendencias en la aplicación de modelos operativos para la optimización, la planificación y la toma de decisiones en el sector salud. Se evidencia una tendencia creciente en el uso de modelos de IO durante el periodo estudiado, predominando las aplicaciones orientadas a la optimización de recursos y decisiones estratégicas de salud pública.
Palabras clave :
Aplicación, Toma de Decisiones, Salud, Revisión.1. Introduction
Since its beginnings, in the mid-20th century, Operations Research (OR) has experienced a great surge in different problem-solving situations of multiple sectors. One of these is the health sector, in which decision-making processes are mainly related to supply allotment and optimization solutions, to the analysis of big databases, to activity and personnel scheduling, and to healthcare service planning [1]. Today, the definition of operative models applicable to decision support systems for problems associated to the health area can result in a complex task. Hence, identifying previous applications and development patterns in the discipline studied throughout time becomes imperative so as to facilitate the selection of quantitative models that adjust to the need of decision support.
The vast diversity of contributions and approaches set forth in literature makes OR become one of the most solid lines of research regarding decision support tools in the health sector. Some of the most recent contributions aim at solving ambulance allocation problems under uncertain demands [2], using hybrid models for hospital bed occupancy optimization [3], using Markov models for patient admission process [4], deciding on equipment acquisition under the concept of multi-criteria analysis through methods like RMPC (AHP, TOPSIS, SAW), PROMETHEE II) [5], using computational intelligence in formulation processes and medicine development for the pharmaceutical industry [6], and identifying factors to be monitored so as to reduce the gap between OR and the creation of technology and decision support systems for the healthcare sector [7].
Due to this, this paper aims to analyze the historical development of the application of OR models in healthcare in order to identify application trends and future work opportunities. To this end, this paper is organized as follows. Section 2 presents the methodology employed to carry out the review and selection criteria. In Section 3, main findings are organized per decades. Section 4 shows a bibliometric analysis of the publications related with OR in healthcare, based on Scopus citation database. Finally, conclusions and guidelines for future works are presented in Section 5.
2. Review methodology
A descriptive literature review of research papers was performed to make a general analysis of the development and implementation of OR tools, models, and approaches in health care.
Using a chronological procedure as a guideline for the analysis, the contributions and bibliographic references are set forth. The study aims to establishing a development timeline to relate concepts and viewpoints about this topic as well as creating a general overview of the evolution of these viewpoints and the approaches for the application of OR tools in the health field.
The search for scientific papers and literature reviews about OR applications in healthcare used the main specialized databases, like Science Direct, Scopus, Springer Link, and PubMed. Text strings were included among the search terms used, for instance, “Operation* Research” “Health application*”, “Operation* Research AND Healthcare OR Medicine” as well as terms related to models and specific applications like scheduling, “queue*”, “linear programming”, “nonlinear programming”, “markov*”, “inventory” “bed planning”, “blood inventory”, “facility allocation”,” location”, “resource planning”, etc.
Documents and papers published in scientific journals were considered a priority. During the search, filters such as publication date, location, or language were not set. The main criteria for paper selection were the following:
-
Is a systematic or descriptive literature review.
-
Poses an OR application case, related to the health care in a detailed and clear way.
-
Is a collection of OR applications in the health sector, or provides relevant information about the development of this discipline.
-
Presents a clear and replicable review methodology or an application of the operational model used.
About 30 documents related to literature reviews and 50 papers presenting the application of OR tools in healthcare services were recovered.
3. Literature review by decades
Since its beginnings as a resource optimization tool, OR ventured in the health care sector, having today a significant number of applications based on quantitative models. The development of OR applications is evident from the literature review; this study will start with the decade of the 1960’s when resource optimization was the main objective. As time passed, the patient’s safety becomes of greater importance and it develops as one of the main driving forces for the evolution of the discipline in health care.
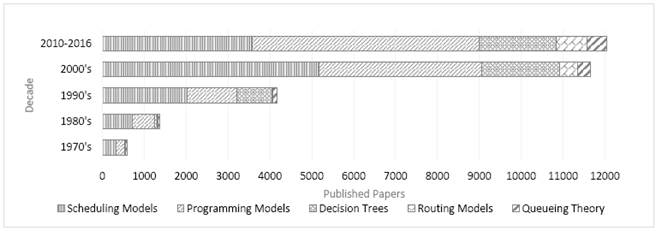
Fig. 1 summarizes the evolution of problems of interest and approaches over time. These issues will be discussed in detail in the following subsections.
3.1. The decade of the 1960’s
Despite the patient’s care and treatment was a priority, OR models had the important duty of relieving the economic effects of war on healthcare services management, hence, focusing mainly on the optimization and correct allocation of the available resources [8].
The need to find methods to balance OR’s main objectives arose in this decade: resource use versus quality patient’s attention. Flagle [8] identified --based on his experience-- the main scenarios for the action of OR within the medical scope in the United States at that time. So, dividing the review in four sections, some approaches focused on the solution of facility use, patient flow, resource optimization and allocation problems were listed. At the same time, he suggested orienting the development of OR in the health sector toward stochastic systems and probabilistic decision models.
After a year and using a similar classification, Feldstein [1] put forward the relevance of quantitative-based decision methods and their use as support tool for decisions of the medical staff based on common sense and value judgment, which were, in a beginning, the main decision tools. Among the principal applications were: medical treatment selection, medicine inventory management and monitoring, required hospitalization time determination, bed number planning and medical and nurse staff scheduling.
3.2. The decade of the 1970’s
Brant E. Fries stands out for his attention and follow up with the development of OR in the health care. In his documents [9,10], Fries contributed with a list of over more than 350 references organized in 15 different medical areas of interest. Another summary for OR applications in medical and hospital issues during the 60’s and part of the 70’s was delivered by Papageorgiou [11] and it concurs with Fries [10] in some items of his classification. This author points out some cases in which linear programming and variable maximization and minimization functions are used.
Figure 1. Overview: of OR topics and approaches trends in Scopus Citation Database
Despite OR was consolidating as one of the most important tools for decision making and optimization in health care, Rosenhead [12], who was knowledgeable of healthcare services’ situation and development level in the United States and the United Kingdom, focused his paper on using strategic planning horizons and disclosed the flaws in the applicability of certain decision-making tools and models.
Barber [13] also poses flaws in the applicability of some decision-making tools. First, the need to define a sole objective for OR optimization (this flaw would be later mended through the application of multi-objective optimization approaches). Second, problems related to accuracy and distortion that social issues quantification and its use as input data for OR models bring about.
3.3. The decade of the 1980’s
In in a selective literature review, Boldy & O’Kane [14] also agree with Fries [9, 10] in part of his classification and delivered an interesting conclusion about his contribution: they observed a larger amount of OR application papers between 1970 and 1973 than in the overall scientific production of the two previous decades. Although many applications and case studies related to this topic were not included in Fries’ list, the upsurge and development of OR in the health care during these years is evident [15].
Resource planning and its optimal management has always been a key element within economic and social development. As Kemball-Cook & Wright [16] mentioned, when considering certain cost-benefit relationships, limited resources, and lack of qualified personnel, OR seemed like a feasible tool for problem solving and decision making processes in certain “problem areas” like health care. In this review, they presented numerous application cases of this kind.
However, some years after, Reynolds [17] studied OR application in decision-making and data gathering processes for policy planning and definition of national programs in different countries on primary healthcare attention. As these are social matters from a community, the author concluded that traditional OR tools would not be very useful in some cases since countless variables -sometimes not identifiable or measurable-were involved [18]. This also relates to Rosenhead’s ideas [12] and the issues presented by Barber [13].
In 1987, Boldy [19] put forward the relationship between OR models and decision support systems (DSS) in the health sector. Through the compilation of case studies and OR applications in strategic decision making, the author emphasized in DSS features posed by Sprague [20], which he found relevant for decision making in the health sector. These were grounded on today’s CDSS (Clinical Decision Support Systems) functioning.
3.4. The Decade of the 1990’s
A little before and during the 90’s, the optimization and productive approach of OR applications in health revolved around social aspects. The use of quantitative-based decision models for problem solving and decision making in health care was addressed by Parker [21]. This author also made great emphasis in the relevance of applying them in developing countries.
Parker suggested the use of heuristics and programming models grounded on quantitative decision models (QDMs). Moreover, he noticed that the upsurge of OR for problem solving processes of social issues or “Social OR” would not be feasible in developing countries since the value of decision making models applied was restricted and these were not applied due to the non-quantitative nature of certain problems and the limited competences of analysts, information access, and technological obstacles. This problem of the non-quantitative nature of social problems relates again to Rosenhead [12] and Reynolds’ [17] conclusions.
Later, through the collection of 286 scientific papers and case studies (which were divided in seven categories), Datta [22] concluded that the applicability of basic OR models was feasible, mainly, in problems related to hospital management, certain diseases’ control and public health. On the other hand, problems revolving around strategic planning [23], such as facility location, nutrition plans, and health management, would need different and more elaborated methodologies and approaches.
Pierskalla & Brailer's [24] review is mostly centered in operative and tactical applications. These authors divided their work in three main categories: design and planning of the system, operation management, and medical management.
Toward the end of the decade, Royston [25] poses the need to achieve a balance between certain aspects (planning horizon, scope, approach, complexity, etc.) in the application of OR models in the health care. In addition, this author mentions some of the most used ORMS (Operations Research and Management Science) tools, for example, scenario forecasting and analysis methods, neural networks and expert systems, simulations, and multi-criteria analysis methods.
Lagergren [26] summarizes the influence and impact of modeling approaches in the health care. This author highlights that technology improvements in hardware and software allowed, to a great extent, the creation and use of more complex models.
3.5. Beginnings of the 21st Century
In this period, and in a general way, resource management is still a high priority in the health systems management [27]. The first decade of the 21st century witnessed the upsurge of decision support systems (DSS) and the establishment of the concept of Clinical Decision Support Systems -CDSS [28,29], OR models became the force in the functioning of these computer tools [30-33] and its fast development led to an assessment requirement so as to compare them to traditional medical decision-making procedures [34,35].
Rais & Viana’s [36] work gathers a great amount of sources concerning OR applications in health care. Taking into account their conclusions and the high amount of sources, the study of OR development in health faces the arduous task of differentiating successful models’ implementations, their advantages, disadvantages, and improvement opportunities in order to attain a general overview of the discipline’s evolution, current status, and future.
The scientific journals that published literature reviews related to the development of OR in the healthcare are shown in Fig. 2. In this list, the European Journal of Operational Research stands out for having the highest number of reviews. It is also important to underline that the rising levels of scientific contributions brings an upward trend in the number of specialized journals focused in the study of OR applied to health care.
Figure 2: Literature Reviews related with OR applied to health care published in Scientific Journals 1962 - 2016
4. Description of the analyzed scientific production
In this section, a general analysis of scientific production related to the application of Operations Research methods in the health sector is presented. The information was selected from the Scopus citation database.
In the first place, OR influence in the health care can be estimated in a general way through the presence of keywords like “Operations Research” - “Operational Research” as well as with search terms like “Health” OR “Healthcare”.
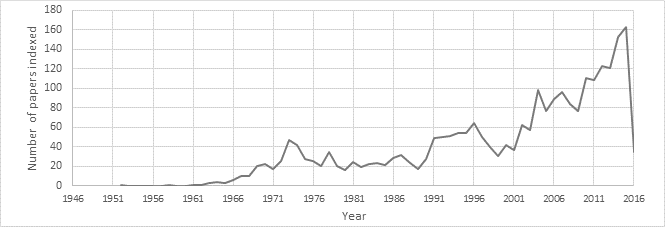
The citation database reports a total of 2563 documents related to the use of OR in the health field between the years 1952 and 2016 (Fig.3). These documents were classified as follows: 1698 scientific papers, 283 review papers, 279 conference papers, and 312 documents of other types. A similar result is obtained when using the same search terms in the PubMed database (2581 documents).
Figure 3: Scientific Production related to Operations Research in Health Care (Scopus 1952-2016).
Approximately, a 52% of the documents indexed by Scopus were published in Medicine journals and 18.2% in Decision Science journals. Regarding the geographical origin of the publications, the United States and the United Kingdom lead the first two places in the ranking for the number of documents indexed, followed by India, Canada, and Switzerland.
4.1. Decision trees
The application of decision trees in the health care goes back to the decade of the 1970’s [37]. The analysis of medical decisions [38 - 41], illness diagnosis [42,43], and assessment of treatment alternatives [44-52] are some of the most frequent uses for this type of decision model.
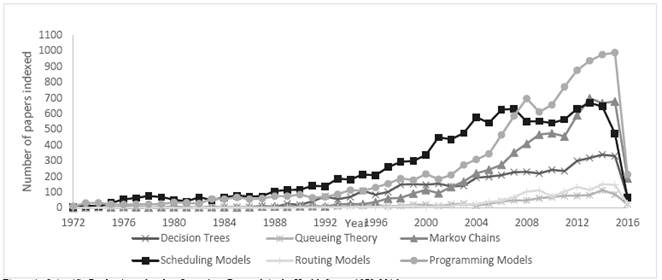
In accordance with the report (Fig. 4), when using the search terms Decision trees AND health* between the years 1973 and 2016, approximately 4600 scientific and literature review papers related to the use of this type of model in the health sector were presented.
Figure 4: Scientific Production related to Operations Research in the Health Sector 1972-2016.
These contributions were mainly published in journals related to Medicine, Nursing, Biochemistry, Genetics, Molecular Biology, Pharmacology, and Toxicology. This fact provides a general overview of the nature of the problems frequently addressed through the use of decision trees.
4.2. Scheduling models
Surgery, medical staff (nurse scheduling), and patient scheduling are the most frequent subjects within the literature consulted [53-64]. Using the search terms “Scheduling” AND Health*, the Scopus database reports 11839 documents between the years 1961 and 2016 (Fig. 4). Of all the documents indexed, approximately 9564 correspond to scientific research papers, 1146 to literature reviews, and 1129 to conference papers. Nearly a 77% of the papers were published in Medicine and Nursing scientific journals.
4.3. Programming models
Exact models of mathematical programming (mixed, linear, and nonlinear) are common in the health field. These allow finding optimal and faster solutions for problems with a relatively low complexity. For this reason, it is useful within operational planning.
With the search terms “Programming” AND Health*, the database reports a total of 11263 documents: a 66% are research papers, a 12% review papers, and a 22% conference papers. Around 90% of the documents were published in scientific journals of Medicine (nearly a 50%), Computer Sciences, and Engineering. According to Fig. 4, the behavior of scientific production for this type of model reaches the highest values. This may be consequence of the great amount of variations this model can provide along with the generalization of the search term used.
4.4. Queueing theory
Waiting line optimization is a common topic within OR and its development goes hand in hand with health systems’ growth and functioning [65].
Queueing studies sometimes are key elements in the definition of necessary abilities for health system designs, and for the improvement of service and attention periods in medical units and emergency services [66-70].
Using the search terms Queu* AND Health*, the database reported a total of 1052 published documents between 1961 and 2016. Of all these documents regarding the queueing model in health issues, a 71% correspond to research papers, a 22% to conference papers, and a 5% to review articles.
As seen in Fig. 4, this type of model, together with routing models, represent substantially less documents indexed in scientific literature. As of the decade of 2000, an increase is observed.
4.5. Location, allocation, and routing models
Determination of quantity and location of medical facilities to increase healthcare service coverage is one of the main applications of location models in this field. These models are commonly used in supply chain design and, together with routing models, they help in travel reduction and resource optimization [71,72].
When using the search terms Location - Allocation AND health*, a total of 125 documents are reported between 1976 and 2016. Of these, a 76% refers to scientific research papers. Regarding routing models, the search terms used were Routing AND Health*. The database reported a total of 1258 documents produced during the years 1971 and 2016. A 52% belongs to conference papers, a 44% to research papers, and the remaining 3% to review papers. The documents comprising this list were mostly published in Computer Science and Medicine journals, and the number is similar to that previously presented for the queueing theory.
4.6. Markov chain models
The use of this type of models in the health sector is quite new. As they are based on statistical methods, Markov chains are usually combined with other models like queueing and scheduling. Some of their applications comprise prognosis and inventory management of hospital resources [73], waiting time reduction [74], and prognosis of a patient’s condition or the development of illnesses [75].
Using the search term Markov AND health*, the database reports a total of 6390 documents of which an 82% are scientific papers, an 11.4% are conference papers, and a 6.3% accounts for literature reviews.
4.7 Discrete-Event simulation
Simulation models in healthcare and hospital milieus have contributed to the study and behavior understanding of variables within health systems by considering objectives, resources, and restrictions established [76-79].
Simulation environments have played an integrating role in the application of strategic decision-making models [80], in programming and scheduling [81], resource and hospital facility allocation, waiting line time reduction, and attention and service levels enhancement [82]. Using the search terms Discrete Event Simulation AND health*, the database reports a total of 790 documents.
In the Figs. 2, 3, 4, previously shown, high similarity is observed in the behavior of the literature related to the general term of “operations research” (Fig. 3) and that related to the specific operational models (Fig. 4). Hence, a similar behavior development is evident, however, the values for every type of model is different
5. Conclusions
The different approaches in operations research allow addressing the broad variety of problems in health care. Solutions for qualitative-oriented problems (public health issues) and optimization requirements for economic variables, attention levels, and patient’s safety were effectively and equally provided.
Contributions related to the use of OR methods in health care sector show a development pattern towards Clinical Decisions Support Systems, which is defined by an upward trend in paper publishing that started after the 70’s decade, reaching its highest levels in the subsequent period of 2013.
Technology development and its improvements in computational processing and storage capacity played an important role in OR applications development through time. To establish a direct causal relation between these two aspects, represents an interesting objective for future research.
The OR in health care is starting to be considered as almost a different discipline, independent from the general conception of OR applications. The rising number of specialized journals are a proof of the fast development of this discipline and the need of more focused scientific platforms to share new contributions and results in this field.
Acknowledgements
This contribution is the direct result of the Project “Definición de parámetros aplicables a sistemas de soporte a la decisión clínica” (Definition of Parameters for Clinical Practice Decision Support Systems), funded by Universidad de la Costa and Colciencias through the Young and Innovative Researcher Internship Scholarship for the period 2015-2016.
References
Referencias
Feldstein, M., Operational research and efficiency in the health service. Lancet. 281(7279), pp.491-492. 1963. DOI: 10.1016/S0140-6736(63)92381-X
Lam, S.S.W., Ng, Y.S., Lakshmanan, M.R., Ng, Y.Y. and Ong, M.E.H., Ambulance deployment under demand uncertainty. J Adv Manag Sci. 4(3), pp. 187-194, 2016.
Belciug, S. and Gorunescu, F., A hybrid genetic algorithm-queuing multi-compartment model for optimizing inpatient bed occupancy and associated costs. Artif Intell Med. 68, pp. 59-69, 2016. DOI: 10.1016/j.artmed.2016.03.001
Gedik, R., Zhang, S. and Rainwater, C,. Strategic level proton therapy patient admission planning: A Markov decision process modeling approach. Health Care Manag Sci. 20(2), pp. 286-302, 2017. DOI: 10.1007/s10729-016-9354-6
Ivlev, I., Jablonsky, J. and Kneppo, P., Multiple-criteria comparative analysis of magnetic resonance imaging systems. Int J Med Eng Inform. 8(2), pp. 124-141, 2016. DOI: 10.1504/IJMEI.2016.075757
Khalid, M.H., Tuszyński. P.K., Kazemi, P., Szlek, J., Jachowicz, R. and Mendyk. A., Transparent computational intelligence models for pharmaceutical tableting process. Complex Adapt Syst Model. Springer Berlin Heidelberg. 4(7) pp. 1-11, 2016. DOI 10.1186/s40294-016-0019-6
Saleem, J.J., Militello, L.G., Russ, A.L. and Wilck, N.R., The divide between applied research and operations in health information technology advancement: reducing the Gap. Proc Hum Factors Ergon Soc Annu Meet. SAGE Publications. 59(1) pp. 460-460, 2015. DOI: 10.1177/1541931215591098
Flagle, C.D., Operational research in the health services. Ann N Y Acad Sci. 107(2), pp. 748-759, 1962. DOI: 10.1111/j.1749-6632.1963.tb13318.x
Fries, B.E., Bibliography of operations research in health-care systems. Oper Res. INFORMS. 24(5), pp. 801-814, 1976. DOI: 10.1287/opre.24.5.801
Fries, B.E., Technical note—bibliography of operations research in health-care systems: An update. Oper Res. INFORMS. 27(2), pp. 408-419, 1979. DOI: 10.1287/opre.27.2.408
Papageorgiou, J.C., Some operations research applications to problems of health care systems (A survey). Int J Biomed Comput. 9(2), pp. 1-14, 1978. DOI: 10.1016/0020-7101(78)90002-8
Rosenhead, J., Operational research in health services planning. Eur J Oper Res. 2(2), pp. 75-85, 1978. DOI: 10.1016/0377-2217(78)90103-0
Barber, B., The implementation and utilisation of operational research in the reorganised National Health Service Part II. Eur J Oper Res. 1(3), pp. 146-153, 1977. DOI: 10.1016/0377-2217(77)90021-2
Boldy, D.P. and O'Kane, P.C., Health operational research —A selective overview. Eur J Oper Res. 10(1), pp. 1-9, 1982. DOI: 10.1016/0377-2217(82)90124-2
Hull, J.C., Operational research applied to health services. J Oper Res Soc. Nature Publishing Group. 32(8), pp.736-737. 1981.
Kemball-Cook, D. and Wright, D.J., The search for appropriate O.R.: A review of operational research in developing countries. J Oper Res Soc. Nature Publishing Group. 32(11), pp. 1021-1037, 1981.
Reynolds, J., Introduction: Operations research in primary health care. Socioecon Plann Sci. 21(2), pp. 73-77, 1987. DOI: 10.1016/0038-0121(87)90016-4
Eaton, D., Church, R., Bennett, V., Hamon, B. and Lopez, L., On deployment of health resources in rural Valle Del Cauca Colombia. In: Cook, W. and Kuhn, T., editors. Planning processes in developing countries: Techniques and achievements. Amsterdam: Amsterdam Netherlands and New York, North-Holland, 1982.
Boldy, D., The relationship between decision support systems and operational research: Health care examples. Eur J Oper Res. 29(2), pp. 128-134, 1987. DOI: 10.1016/0377-2217(87)90102-0
Sprague, R., A framework for the development of decision support systems. MIS Q. 6(4), pp. 1-26, 1980. DOI: 10.2307/248957
Parker, B.R., In quest of useful health care decision models for developing countries. European Journal of Operation Research. 49(2), pp. 279-288, 1990. DOI: 10.1016/0377-2217(90)90346-D
Datta, S., Applications of O.R. in health in developing countries: A review. Soc Sci Med. 37(12), pp. 1441-1450, 1993. DOI: 10.1016/0277-9536(93)90178-7
Heidenberger, K., Strategic decision support in preventive health care. Socioecon Plann Sci. 26(2), pp. 129-146, 1992. DOI: 10.1016/0038-0121(92)90019-2
Pierskalla, W.P. and Brailer, D.J., Applications of operations research in health care delivery. In: Pollock, S.M., Rothkopf, M.H. and Barnett, A., editors. Handbooks in OR & MS. Vol. 6. Amsterdam, The Netherlands: Elsevier Science, pp. 469-505, 1994.
Royston, G., Shifting the balance of health care into the 21st century. Eur J Oper Res. 105(2), pp. 267-276, 1998. DOI: 10.1016/S0377-2217(97)00234-8
Lagergren, M., What is the role and contribution of models to management and research in the health services? A view from Europe. Eur J Oper Res., 105(2), pp. 257-266, 1998. DOI: 10.1016/S0377-2217(97)00233-6
Rauner, M.S. and Vissers, J.M.H., OR applied to health services: Planning for the future with scarce resources. Eur J Oper Res. 150(1), pp. 1-2, 2003. DOI: 10.1016/S0377-2217(02)00775-0
Berner, E.S., Clinical decision support systems: State of the art [online]. Agency for Healthcare Research and Quality. 2009. Available at: https://healthit.ahrq.gov/sites/default/files/docs/page/09-0069-EF_1.pdf
Bonis, J.J., Sancho, J.J. y Sanz, F., Sistemas informáticos de soporte a la decisión clínica. Med Clin. Elsevier. 122(1), pp. 39-44, 2004. DOI: 10.1157/13057545
Dexter, P.R., Perkins, S., Overhage, J.M., Maharry, K., Kohler, R.B. and McDonald, C.J., A computerized reminder system to increase the use of preventive care for hospitalized patients. N Engl J Med. 345, pp.965-970, 2001. DOI: 10.1056/NEJMsa010181
McCowan, C., Neville, R.G., Ricketts, I.W., Warner, F.C. and Hoskins, G.T., Lessons from a randomized controlled trial designed to evaluate computer decision support software to improve the management of asthma. Med Inf Internet Med. 18, pp. 586-596, 2001.
Frijling, B.D., Lobo, C.M., Hulscher, M.E., Akkermans, R.P., Braspenning, J.C., Prins, A. et al., Multifaceted support to improve clinical decision making in diabetes care: A randomised controlled trial in general practice. Diabet Med. 1910, pp. 836-842, 2002. DOI: 10.1046/j.1464-5491.2002.00810.x
Friedlin, J., Dexter, P.R. and Overhage, J.M., Details of a successful clinical decision support system. AMIA 2007 Symposium Proceedings. American Medical Informatics Association. pp. 254-258, 2007.
Kaplan, B., Evaluating informatics applications—clinical decision support systems literature review. Int J Med Inform. 64(1), pp.15-37, 2001. DOI: 10.1016/S1386-5056(01)00183-6
Bouaud, J., Seroussi, B., Antoine, E.C. and Zelek, L.S.M., A before-after study using OncoDoc, a guideline-based decision support-system on breast cancer management: Impact upon physician prescribing behaviour. Medinfo. 10, pp. 420-424, 2001.
Rais, A. and Viana, A., Operations Research in healthcare: A survey. Int Trans Oper Res. 18(1), pp. 1-31, 2010. DOI: 10.1111/j.1475-3995.2010.00767.x
Podgorelec, V., Kokol, P., Stiglic, B. and Rozman, I., Decision trees: An overview and their use in medicine. J Med Syst. Kluwer Academic Publishers-Plenum Publishers, 26(5), pp. 445-463, 2002.
Torres, P., Ria-o, D. and López-Vallverdú, J., Inducing decision trees from medical decision processes. In: Ria-o, D., Ten Teije, A., Miksch, S. and Peleg, M., editors., Knowledge representation for health-care SE - 4. Springer Berlin Heidelberg. pp. 40-55, 2011. DOI: 10.1007/978-3-642-18050-7_4
Cornalba, C., Clinical and operational risk: A bayesian approach. Methodol Comput Appl Probab. 11(1), pp. 47-63, 2008. DOI: 10.1007/s11009-007-9068-9
Gardino, S.L., Jeruss, J.S. and Woodruff, T.K,. Using decision trees to enhance interdisciplinary team work: The case of oncofertility. J Assist Reprod Genet. 27(5), pp.227-231, 2010. DOI: 10.1007/s10815-010-9413-8
Hazen, G.B., Stochastic trees and the stotree modeling environment: Models and software for medical decision analysis. J Med Syst. Kluwer Academic Publishers-Plenum Publishers; 26(5), pp. 399-413, 2002.
Stasis, A.C., Loukis, E.N., Pavlopoulos, S.A. and Koutsouris, D., A multiple decision trees architecture for medical diagnosis: The differentiation of opening snap, second heart sound split and third heart sound. Comput Manag Sci. 1(3), pp. 245-274, 2004. DOI: 10.1007/s10287-004-0015-8
Barrientos-Martínez, R.E., Cruz-Ramírez, N., Acosta-Mesa, H.G., Suárez, I.R., Gogeascoechea-Trejo. M. del C., Pavón-León ,P., et al., Árboles de decisión como herramienta en el diagnóstico médico. Rev Médica la Univ Veracruzana, 9(2), 2009.
Wang, J., Li, M., Hu, Y. and Zhu, Y., Comparison of hospital charge prediction models for gastric cancer patients: Neural network vs. decision tree models. BMC Health Serv Res. 9(161), pp. 1-6, 2009. DOI: 10.1186/1472-6963-9-161
Bonner, G., Decision making for health care professionals: use of decision trees within the community mental health setting. J Adv Nurs. 35(3), pp. 349-356, 2001. DOI: 10.1046/j.1365-2648.2001.01851.x
Ali, S., Razali, A., Bakar, A. and Suradi, N., Developing treatment plan support in outpatient health care delivery with decision trees technique. In: Cao, L., Zhong, J. and Feng, Y., editors. Advanced data mining and applications SE - 47. Springer Berlin Heidelberg. pp. 475-482, 2010. DOI: 10.1007/978-3-642-17313-4_47
Hu, Y-J., Ku, T-H., Jan, R-H., Wang, K., Tseng, Y-C. and Yang, S-F., Decision tree-based learning to predict patient controlled analgesia consumption and readjustment. BMC Med Inform Decis Mak. 12(131), pp. 1-15, 2012. DOI: 10.1186/1472-6947-12-131
Nakayama, N., Oketan,i M., Kawamura, Y., Inao, M., Nagoshi, S., Fujiwara, K., et al., Algorithm to determine the outcome of patients with acute liver failure: a data-mining analysis using decision trees. J Gastroenterol. 47(6), pp. 664-677, 2012. DOI: 10.1007/s00535-012-0529-8
Chao, C-M., Yu, Y-W., Cheng, B-W. and Kuo, Y-L., Construction the model on the breast cancer survival analysis use support vector machine, logistic regression and decision tree. J Med Syst. 38(10), pp. 106. 2014. DOI: 10.1007/s10916-014-0106-1
Tsai, M-H., Wang, H-C., Lee, G-W., Lin, Y-C. and Chiu, S-H., A decision tree based classifier to analyze human ovarian cancer cDNA microarray datasets. J Med Syst. 40(1), pp. 21, 2015. DOI: 10.1007/s10916-015-0361-9
De la Hoz-Manotas, A.K., Martínez-Palacio, U.J. y Mendoza-Palechor, F.E., Técnicas de ml en medicina cardiovascular. Memorias. Dec 5, 11(20), pp. 41-46, 2013.
Bayat, S., Cuggia, M., Rossille, D., Kessler, M. and Frimat, L., Comparison of Bayesian network and decision tree methods for predicting access to the renal transplant waiting list. Stud Health Technol Inform. 150, pp. 600-604, 2009.
Pham, D-N. and Klinkert, A., Surgical case scheduling as a generalized job shop scheduling problem. Eur J Oper Res. 185(3), pp. 1011-1025, 2008. DOI: 10.1016/j.ejor.2006.03.059
Koeleman, P.M., Bhulai, S. and van Meersbergen, M., Optimal patient and personnel scheduling policies for care-at-home service facilities. Eur J Oper Res. 219(3), pp. 557-563, 2012. DOI: 10.1016/j.ejor.2011.10.046
Pradenas-Rojas, L. y Matamala-Vergara, E., Una formulación matemática y de solución para programar cirugías con restricciones de recursos humanos en el hospital público. Ingeniare Rev Chil Ing. Universidad de Tarapacá, 20(2), pp. 230-241, 2012.
Cordier, J-P. and Riane, F., Towards a centralised appointments system to optimise the length of patient stay. Decis Support Syst. 55(2), pp. 629-639, 2013. DOI: 10.1016/j.dss.2012.10.017
Ma, G. and Demeulemeester, E., A multilevel integrative approach to hospital case mix and capacity planning. Comput Oper Res. 40(9), pp. 2198-2207, 2013. DOI: 10.1016/j.cor.2012.01.013
M'Hallah, R. amd Alkhabbaz, A., Scheduling of nurses: A case study of a Kuwaiti health care unit. Oper Res Heal Care. 2(1-2), pp. 1-19, 2013. DOI: 10.1016/j.orhc.2013.03.003
Marques, I., Captivo, M.E. and Vaz-Pato. M., Scheduling elective surgeries in a Portuguese hospital using a genetic heuristic. Oper Res Heal Care. 3(2), pp. 59-72, 2014. DOI: 10.1016/j.orhc.2013.12.001
Lanzarone, E. and Matta, A., Robust nurse-to-patient assignment in home care services to minimize overtimes under continuity of care. Oper Res Heal Care. 3(2), pp. 48-58, 2014. DOI: 10.1016/j.orhc.2014.01.003
Marques, I. and Captivo, M.E., Bicriteria elective surgery scheduling using an evolutionary algorithm. Oper Res Heal Care, 18, pp. 251-266, 2015.
Vancroonenburg, W., Smet, P. and Vanden-Berghe, G., A two-phase heuristic approach to multi-day surgical case scheduling considering generalized resource constraints. Oper Res Heal Care. 7, pp. 27-39, 2015.
Xiang, W., Yin, J. and Lim, G,. An ant colony optimization approach for solving an operating room surgery scheduling problem. Comput Ind Eng. 85, pp. 335-345, 2015. DOI: 10.1016/j.cie.2015.04.010
Riise, A., Mannino, C. and Burke, E.K., Modelling and solving generalised operational surgery scheduling problems. Comput Oper Res. 66, pp. 1-11, 2016. DOI: 10.1016/j.cor.2015.07.003
Lakshmi, C. and Sivakumar, A.I.. Application of queueing theory in health care: A literature review. Oper Res Heal Care. 2(1-2), pp. 25-39, 2013. DOI: 10.1016/j.orhc.2013.03.002
Wu, G., Application of the queueing theory with Monte Carlo simulation to inhalation toxicology. Arch Toxicol. 72(6), pp. 330-335, 1998. DOI: 10.1007/s002040050510
Izady, N. and Worthington, D., Setting staffing requirements for time dependent queueing networks: The case of accident and emergency departments. Eur J Oper Res. 219(3), pp. 531-540, 2012. DOI: 10.1016/j.ejor.2011.10.040
Sharif, A., Stanford, D.A., Taylor, P. and Ziedins, I., A multi-class multi-server accumulating priority queue with application to health care. Oper Res Heal Care. 3(2), pp. 73-79, 2014. DOI: 10.1016/j.orhc.2014.01.002
Asaduzzaman, M. and Chaussalet, T.J., Capacity planning of a perinatal network with generalised loss network model with overflow. Eur J Oper Res. 232(1), pp. 178-185, 2014. DOI: 10.1016/j.ejor.2013.06.037
Kozlowski, D. and Worthington, D., Use of queue modelling in the analysis of elective patient treatment governed by a maximum waiting time policy. Eur J Oper Res. 244, pp. 331-338, 2015. DOI: 10.1016/j.ejor.2015.01.024
Rahman, S. and Smith, D.K., Use of location-allocation models in health service development planning in developing nations. Eur J Oper Res. 123(3), pp. 437-452, 2000. DOI: 10.1016/S0377-2217(99)00289-1
Mitropoulos, P., Mitropoulos, I. and Giannikos, I., Combining DEA with location analysis for the effective consolidation of services in the health sector. Comput Oper Res. 40(9), pp. 2241-2250, 2013. DOI: 10.1016/j.cor.2012.01.008
Broyles, J.R., Cochran, J.K. and Montgomery, D.C., A statistical Markov chain approximation of transient hospital inpatient inventory. Eur J Oper Res. 207(3), pp. 1645-1657, 2010. DOI: 10.1016/j.ejor.2010.06.021
Almehdawe, E., Jewkes, B. and He, Q-M., A Markovian queueing model for ambulance offload delays. Eur J Oper Res. 226(3), pp. 602-614, 2013. DOI: 10.1016/j.ejor.2012.11.030
Sáez, P. and Herrera, C., Proposición de un método basado en cadenas de Markov para el pronóstico de fibrilaciones auriculares paroxísticas. Ingeniare Rev Chil. Ing. 23(3), pp.449-457, 2015. DOI: 10.4067/S0718-33052015000300014
Jun, J.B., Jacobson, S.H. and Swisher, J.R., Application of discrete-event simulation in health care clinics: A survey. J Oper Res Soc. Nature Publishing Group. 50(2), pp. 109-123, 1999.
Brailsford, S. and Schmidt, B., Towards incorporating human behaviour in models of health care systems: An approach using discrete event simulation. Eur J Oper Res. 150(1), pp. 19-31, 2003. DOI: 10.1016/S0377-2217(02)00778-6
Hosseinifard, S.Z., Abbasi, B. and Minas, J.P., Intensive care unit discharge policies prior to treatment completion. Oper Res Heal Care. 3(3), pp. 168-175, 2014. DOI: 10.1016/j.orhc.2014.06.001
Viana, J., Brailsford, S.C., Harindra, V. and Harper, P.R., Combining discrete-event simulation and system dynamics in a healthcare setting: A composite model for Chlamydia infection. Eur J Oper Res. 237(1), pp. 196-206, 2014. DOI: 10.1016/j.ejor.2014.02.052
Atkins, D., Noonan, V.K., Santos, A., Lewis, R., Fehlings, M., Burns, A., et al., Secondary complications in SCI across the continuum: using operations research to predict the impact and optimize management strategies. Top Spinal Cord Inj Rehabil. 18(1), pp. 57-66, 2012. DOI: 10.1310/sci1801-57
Liu, Z., Cabrera, E., Taboada, M., Epelde, F., Rexachs, D. and Luque, E., Quantitative evaluation of decision effects in the management of emergency department problems. Procedia Comput Sci. 51, pp. 433-442, 2015. DOI: 10.1016/j.procs.2015.05.265
De Angelis, V., Felici, G. and Impelluso, P., Integrating simulation and optimisation in health care centre management. Eur J Oper Res. 150(1), pp. 101-114, 2003. DOI: 10.1016/S0377-2217(02)00791-9
Cómo citar
IEEE
ACM
ACS
APA
ABNT
Chicago
Harvard
MLA
Turabian
Vancouver
Descargar cita
CrossRef Cited-by
1. Miguel Ortiz-Barrios, Juan-José Alfaro-Saiz, Ashkan Memari. (2020). An integrated approach for designing in-time and economically sustainable emergency care networks: A case study in the public sector. PLOS ONE, 15(6), p.e0234984. https://doi.org/10.1371/journal.pone.0234984.
2. Mohammad Rashid Hussain, Ayman Qahmash, Salem Alelyani, Mohammed Saleh Alsaqer. (2021). Intelligent Computing. Lecture Notes in Networks and Systems. 284, p.1151. https://doi.org/10.1007/978-3-030-80126-7_81.
3. Miguel Angel Ortíz-Barrios, Dayana Milena Coba-Blanco, Juan-José Alfaro-Saíz, Daniela Stand-González. (2021). Process Improvement Approaches for Increasing the Response of Emergency Departments against the COVID-19 Pandemic: A Systematic Review. International Journal of Environmental Research and Public Health, 18(16), p.8814. https://doi.org/10.3390/ijerph18168814.
4. Sahar Mahmood. (2023). Decision making model for detecting infected people with COVID-19. Yugoslav Journal of Operations Research, 33(4), p.601. https://doi.org/10.2298/YJOR221115009M.
5. Yuandong Cheng. (2024). Construction and application of a performance assessment model for teaching operations research based on Bayesian network technology. Applied Mathematics and Nonlinear Sciences, 9(1) https://doi.org/10.2478/amns-2024-1867.
6. Amir Ahmadi-Javid, Nasrin Ramshe. (2020). A stochastic location model for designing primary healthcare networks integrated with workforce cross-training. Operations Research for Health Care, 24, p.100226. https://doi.org/10.1016/j.orhc.2019.100226.
7. Natalia Romero-Sandoval, Mónica Torres, Víctor Hugo Solis, Fabricio Orellana, Pilar Avila Castells, Diego Andrade, Héctor Sánchez-Pérez, Patricia Jiménez, Joan Pau Millet, Joan A. Cayla, Miguel Martín. (2025). Patterns and Treatment Timelines of Tuberculosis in Males From Ecuador’s Largest Prison. Journal of Correctional Health Care, 31(5), p.327. https://doi.org/10.1177/10783458251380507.
Dimensions
PlumX
Visitas a la página del resumen del artículo
Descargas
Licencia
Derechos de autor 2017 DYNA

Esta obra está bajo una licencia internacional Creative Commons Atribución-NoComercial-SinDerivadas 4.0.
El autor o autores de un artículo aceptado para publicación en cualquiera de las revistas editadas por la facultad de Minas cederán la totalidad de los derechos patrimoniales a la Universidad Nacional de Colombia de manera gratuita, dentro de los cuáles se incluyen: el derecho a editar, publicar, reproducir y distribuir tanto en medios impresos como digitales, además de incluir en artículo en índices internacionales y/o bases de datos, de igual manera, se faculta a la editorial para utilizar las imágenes, tablas y/o cualquier material gráfico presentado en el artículo para el diseño de carátulas o posters de la misma revista.