Adenoma metanéfrico: diagnóstico diferencial del carcinoma urotelial del tracto urinario superior. Reporte de un caso
Metanephric adenoma: differential diagnosis of upper tract urothelial carcinoma. A case report
DOI:
https://doi.org/10.15446/cr.v8n1.92283Palabras clave:
Kidney Neoplasms, Nephrectomy, Adenoma (en)Neoplasias Renales, Nefrectomía, Adenoma (es)
Descargas
Introduction: Metanephric adenoma is a rare benign kidney tumor. Patients with these tumors are usually asymptomatic, although polycythemia occurs in up 12% of cases. These masses are often described on diagnostic imaging as solid, single, well-defined, oval-shaped, unilateral lesions, located primarily in the renal medulla and without extrarenal involvement. These neoplasms are difficult to differentiate from malignant neoplasms of the upper urinary tract, so the definitive diagnosis is achieved by histopathology. Currently, the treatment of choice is radical nephrectomy.
Case presentation: A 51-year-old woman from Bogotá (Colombia) was referred to the urology service of a tertiary care hospital due to bilateral lumbar pain of non-specific characteristics. At the time of consultation, the patient was asymptomatic. Renal and urinary tract ultrasound showed hydronephrosis and right renal mass. Computed tomography urography was requested, which revealed a lesion in the right renal pelvis with parenchymal invasion highly suggestive of high-risk upper urinary tract urothelial carcinoma, as well as adenopathies in the para-aortic lymph nodes. The patient underwent a radical nephroureterectomy with bladder cuff, which allowed establishing a final diagnosis of metanephric adenoma according to the histopathological study.
Conclusions: Metanephric adenoma is a rare tumor that is difficult to diagnose through imaging, so it is necessary to explore additional tools to establish an accurate pre-surgical diagnosis that allows preserving the affected renal unit. Also, given their non-specificity, these tumors should be included in the differential diagnosis of lesions suggestive of upper tract urothelial carcinoma.
Introducción. El adenoma metanéfrico es un tumor renal benigno poco frecuente. Los pacientes con estos tumores no suelen presentar síntomas, aunque en el 12% de los casos se presenta policitemia. En las imágenes diagnósticas, los adenomas metanéfricos se observan como lesiones sólidas, únicas y bien definidas que, por lo general, comprometen la medula renal pero no ocasionan compromiso extrarenal. Estas neoplasias son difíciles de diferenciar imagenológicamente de neoplasias malignas del tracto urinario superior, por lo que el diagnóstico definitivo se logra mediante estudios histopatológicos. El tratamiento de elección es la nefrectomía radical.
Presentación del caso. Mujer de 51 años procedente de Bogotá (Colombia), quien fue remitida al servicio de urología de un hospital de tercer nivel de atención por dolor lumbar bilateral de características inespecíficas. Al momento de la consulta la paciente se encontraba asintomática. Mediante ecografía renal y de vías urinarias se evidenció hidronefrosis y una masa renal derecha. Se ordenó urografía por tomografía axial computarizada que documentó una lesión en la pelvis renal derecha con invasión al parénquima renal altamente sugestiva de carcinoma urotelial de tracto urinario superior de alto riesgo, así como adenopatías en los ganglios paraaórticos, por lo que se le realizó una nefroureterectomía radical derecha con cuña vesical que permitió establecer un diagnóstico final de adenoma metanéfrico según el estudio histopatológico. La paciente tuvo una evolución satisfactoria.
Conclusiones. El adenoma metanéfrico es un tumor poco frecuente y de difícil diagnóstico imagenológico, por lo que se requiere explorar herramientas adicionales para establecer un diagnóstico certero prequirúrgico que permita preservar la unidad renal afectada. Asimismo, dada su inespecificidad, estos tumores deben incluirse dentro de los diagnósticos diferenciales de las lesiones sugestivas de carcinoma urotelial de tracto urinario superior.
https://doi.org/10.15446/cr.v8n1.92283
Metanephric adenoma: differential diagnosis of upper tract urothelial carcinoma. A case report
Keywords: Kidney Neoplasms; Nephrectomy; Adenoma.
Palabras clave: Neoplasias renales; Nefrectomía; Adenoma.
Juan Camilo Álvarez-Restrepo
Víctor Iván Romero-Nieto
Wilfredo Donoso-Donoso
Universidad Nacional de Colombia
- Bogotá Campus - Faculty of Medicine -
Department of Surgery - Urology Unit
- Bogotá D.C. - Colombia.
Universidad Nacional de Colombia
- Bogotá Campus- Faculty of Medicine -
Urology Research and Innovation Group
- Bogotá D.C. - Colombia.
David Andrés Castañeda-Millán
Universidad Nacional de Colombia
- Bogotá Campus - Faculty of Medicine -
Urology Research and Innovation Group
- Bogotá D.C. - Colombia.
Servicios Médicos Especializados Semedes Ltda - Urology Service - Bogotá D.C. - Colombia.
Diego Camacho-Nieto
Jorge Forero-Muñoz
Servicios Médicos Especializados Semedes Ltda - Urology Service - Bogotá D.C. - Colombia.
Instituto Nacional de Cancerología - Urologic Oncology Unit - Bogotá D.C. - Colombia.
Corresponding author
Juan Camilo Álvarez-Restrepo. Unidad de Urología,
Departamento de Cirugía, Facultad de Medicina,
Universidad Nacional de Colombia.
Bogotá D.C. Colombia.
Email: juancalvarezr92@hotmail.com
Received: 09/12/2020 Accepted: 09/02/2021
Abstract
Introduction: Metanephric adenoma is a rare benign kidney tumor. Patients with these tumors are usually asymptomatic, although polycythemia occurs in up to 12% of cases. These masses are often described on diagnostic imaging as solid, single, well-defined, oval-shaped, unilateral lesions, located primarily in the renal medulla and without extrarenal involvement. These neoplasms are difficult to differentiate from malignant neoplasms of the upper urinary tract, so the definitive diagnosis is achieved by histopathology. Currently, the treatment of choice is radical nephrectomy.
Case presentation: A 51-year-old woman from Bogotá (Colombia) was referred to the urology service of a tertiary care hospital due to bilateral lumbar pain of non-specific characteristics. At the time of consultation, the patient was asymptomatic. Renal and urinary tract ultrasound showed hydronephrosis and right renal mass. Computed tomography urography was requested, which revealed a lesion in the right renal pelvis with parenchymal invasion highly suggestive of high-risk upper urinary tract urothelial carcinoma, as well as adenopathies in the para-aortic lymph nodes. The patient underwent a radical nephroureterectomy with bladder cuff, which allowed establishing a final diagnosis of metanephric adenoma according to the histopathological study.
Conclusions: Metanephric adenoma is a rare tumor that is difficult to diagnose through imaging, so it is necessary to explore additional tools to establish an accurate pre-surgical diagnosis that allows preserving the affected renal unit. Also, given their non-specificity, these tumors should be included in the differential diagnosis of lesions suggestive of upper tract urothelial carcinoma.
Resumen
Introducción. El adenoma metanéfrico es un tumor renal benigno poco frecuente. Los pacientes con estos tumores no suelen presentar síntomas, aunque en el 12% de los casos se presenta policitemia. En las imágenes diagnósticas, los adenomas metanéfricos se observan como lesiones sólidas, únicas y bien definidas que, por lo general, comprometen la médula renal pero no ocasionan compromiso extrarenal. Estas neoplasias son difíciles de diferenciar imagenológicamente de neoplasias malignas del tracto urinario superior, por lo que el diagnóstico definitivo se logra mediante estudios histopatológicos. El tratamiento de elección es la nefrectomía radical.
Presentación del caso. Mujer de 51 años procedente de Bogotá (Colombia), quien fue remitida al servicio de urología de un hospital de tercer nivel de atención por dolor lumbar bilateral de características inespecíficas. Al momento de la consulta la paciente se encontraba asintomática. Mediante ecografía renal y de vías urinarias se evidenció hidronefrosis y una masa renal derecha. Se ordenó urografía por tomografía axial computarizada que documentó una lesión en la pelvis renal derecha con invasión al parénquima renal altamente sugestiva de carcinoma urotelial de tracto urinario superior de alto riesgo, así como adenopatías en los ganglios paraaórticos, por lo que se le realizó una nefroureterectomía radical derecha con cuña vesical que permitió establecer un diagnóstico final de adenoma metanéfrico según el estudio histopatológico. La paciente tuvo una evolución satisfactoria.
Conclusiones. El adenoma metanéfrico es un tumor poco frecuente y de difícil diagnóstico imagenológico, por lo que se requiere explorar herramientas adicionales para establecer un diagnóstico certero prequirúrgico que permita preservar la unidad renal afectada. Asimismo, dada su inespecificidad, estos tumores deben incluirse dentro de los diagnósticos diferenciales de las lesiones sugestivas de carcinoma urotelial de tracto urinario superior.
Introduction
Metanephric adenoma (MA) is a rare benign tumor that originates in renal epithelial cells and is usually detected as an incidental finding (1). This neoplasm is difficult to differentiate from malignant tumors affecting the upper urinary tract in the pre-surgical stage.
The definitive diagnosis of MA is established based on immunohistochemistry and histopathological findings. However, it has been proposed that the presence of solid, single, well-defined, oval-shaped, unilateral lesions predominantly in the renal medulla and without extrarenal involvement in imaging studies is a useful finding to differentiate it from other tumors. This finding also allows to consider MA as a differential diagnosis in patients with upper urinary tract masses and thus avoid ablative treatment in the affected kidney and ureter (2).
The following is the case of a patient who underwent right radical nephroureterectomy due to clinical suspicion of high-risk upper urinary tract urothelial carcinoma, whose final diagnosis was MA according to the histopathological study.
Case presentation
A 51-year-old Latin American woman from Bogotá D.C. (Colombia), housewife, from a lower-middle income household and without a relevant medical history, presented to the outpatient clinic of the urology service of a public tertiary healthcare center in Bogotá with mild to moderate bilateral lumbar pain of non-specific characteristics that lasted three months. The patient was referred by the general medicine service, which had previously requested a renal/urinary tract ultrasound that showed a right renal mass with ipsilateral grade I hydronephrosis.
During the history-taking process, the patient was asymptomatic, and no relevant findings were found on the physical examination. Consequently, a computed tomography (CT) urography was ordered, and the results were analyzed at the follow-up appointment 2 weeks after the initial assessment. CT showed a 44x44x28mm lesion in the right renal pelvis with invasion of the renal parenchyma at the lower pole and adenopathies in the para-aortic nodes that measured up to 17mm (Figures 1 and 2). Given this finding, a CT scan of the chest (assessed in a second follow-up appointment) was requested, finding no metastatic involvement, as well as a serial urinary cytology with findings consistent with a type II category lesion according to the Paris classification (negative for high-grade urothelial carcinoma) (3). In addition, the glomerular filtration rate (GFR) estimated with the CKD-EPI equation at that time was 101 mL/min/1.73 m2.

Figure 1 Computed tomography (CT) urography. Nephrogenic phase; axial plane.
Source: Document obtained during the study.
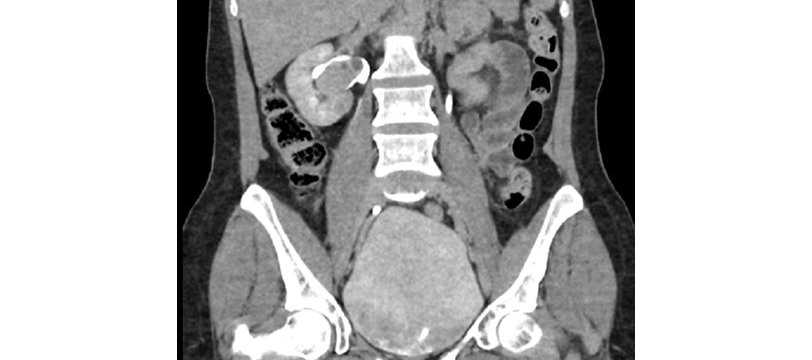
Figure 2 Computed tomography (CT) urography. Excretory phase; coronal plane.
Source: Document obtained during the study.
Due to the high suspicion of high-risk upper tract urothelial carcinoma (staging: cT3N1M0 according to the 2017 TNM classification), the presence of hydronephrosis, and the detection of adenopathies on the CT scan, during the second follow-up appointment, the patient was considered a candidate for a transurethral cystoscopy and then right radical nephroureterectomy with bladder cuff and right retroperitoneal lymph node dissection with curative intent. The surgery was scheduled to be conducted in an outpatient clinic with the urology department one month following the initial assessment.
Transurethral cystoscopy revealed no endoluminal bladder lesions, however during surgery, a tumor of approximately 5cm in diameter was discovered in the right renal pelvis with no macroscopic involvement of adjacent tissues; no retroperitoneal adenopathies were observed on macroscopic examination (Figures 3 and 4). It should be noted that nephroureterectomy with bladder cuff was performed using the intravesical approach.
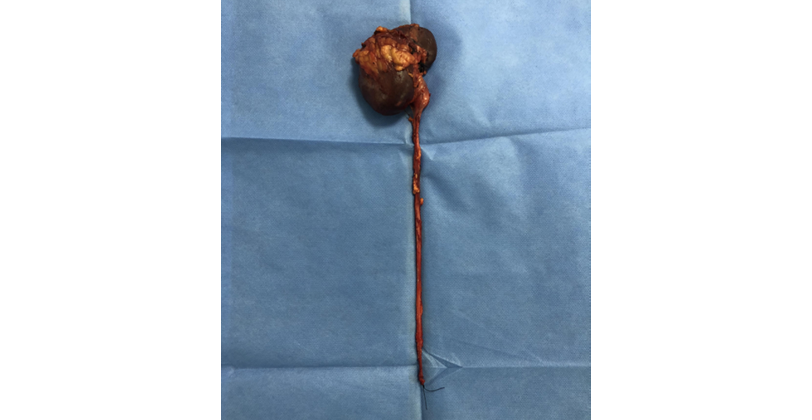
Figure 3 Surgical specimen.
Source: Photographs obtained during the surgery.
The patient presented no postoperative complications, her course was satisfactory, and she was discharged three days after the procedure. The pathology report showed a mixed epithelial and stromal tumor of the kidney with free borders, and immunohistochemistry confirmed the presence of a MA (positive for CD57, vimentin, and WT1; negative for CK7 and CD10).
During the first postoperative follow-up, 3 weeks after the procedure, the patient was asymptomatic and had a GFR according to the CKD-EPI formula of 85 mL/min/1.73m2. In the second follow-up, 6 months after surgery, the patient was still asymptomatic, and no tumor relapse was observed in the CT of the abdomen and pelvis.
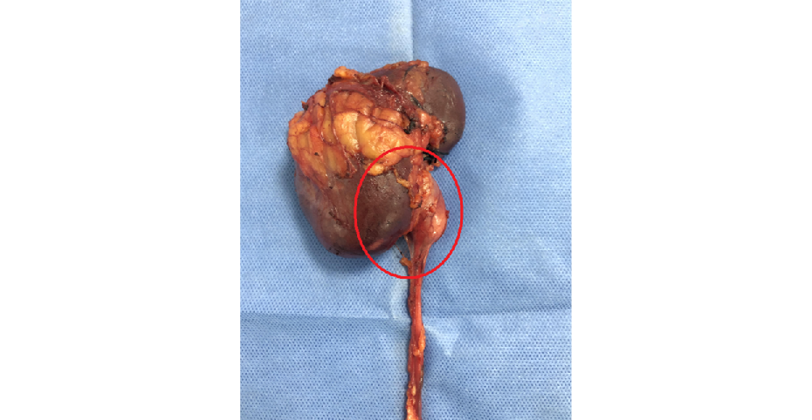
Figure 4 Approach to the area of interest (in red). Projection of the mass contained in the right renal pelvis.
Source: Photographs obtained during the surgery.
Discussion
MA is a rare renal neoplasm that accounts for 0.2% of adult renal epithelial tumors and has less than 200 cases reported in the literature (1,4). This type of tumor, according to Jiang et al. (1), was classified by the World Health Organization in 2016 as a subtype of metanephric neoplasm, which also includes adenofibroma and stromal tumors.
MAs can occur at any age, but they are most common in patients aged 50 to 60 years, with a female-to-male ratio of 2-2.6:1 (1,4). Genetic analyzes have revealed, as reported by Ding et al. (5), that the missense mutation of BRAF V600E could be detected in approximately 90% of these types of neoplasms.
Patients with MA usually have no symptoms, although lower back pain, gross hematuria, and fever occur in 10-50% of cases (2,6). In addition, polycythemia has been reported in about 12% of MA patients with hematuria (1).
MAs have a low rate of diagnostic certainty using imaging and the diagnosis is usually incidental, which may be explained by the low suspicion and prevalence (2). Similarly, these tumors are difficult to differentiate in the pre-surgical stage from other malignancies such as Wilms’ tumor, metastatic papillary thyroid carcinoma, and papillary renal cell carcinoma (7).
The imaging characteristics described for MAs in small case series, such as Zhu et al. (2) in 8 patients with MA who were hospitalized at the Subei People’s Hospital (China) between 2006 and 2011, refer to solid, single, well-defined, oval-shaped, unilateral lesions predominantly in the renal medulla and without extrarenal involvement. Ultrasound can detect hypo- or hyperechoic lesions with lower Doppler flow compared to other tumors (1). On nuclear magnetic resonance imaging, these neoplasms are hypointense with delayed enhancement of contrast material in T1W1 sequence and hyperintense in DWI sequence (1). Finally, the predominant findings on CT scan are lesions with well-defined boundaries with enhancement, calcifications (20% of cases), and homogeneous enhancement that is lower compared to that of renal parenchyma in all enhanced phases (1,8).
The origin of MAs in epithelial cells of the renal collecting duct explains the imaging finding of invasion or displacement of the collecting system and suggests a differential diagnosis with urothelial carcinoma of the upper urinary tract (1,2). However, Li and collaborators, cited by Yan et al. (9), found that 83.3% of tumors of this type were located in the periphery of the renal cortex without involvement of the collecting system.
The characteristics of MAs have not been widely studied, but Jiménez-Heffernan et al. (10), in their letter to the editor, established that cytology, either as fine-needle aspirates or during intraoperative procedures, can be quite useful in identifying these tumors. Thus, the characteristic cytology findings are generally small, clustered cells, oval or round, with uniform basophilic nuclei and without nucleoli and scant cytoplasm; the absence of nuclear atypia, necrosis, and mitosis are also common findings in patients with MA (7,11). Taking into account these histopathological findings in cytological studies, it is necessary to consider Wilms’ tumor and papillary renal cell carcinoma as differential diagnoses (7,10,11).
On the other hand, as reported by Le Nué et al. (12), MA diagnosis may be supported by core-needle renal biopsy. If a biopsy is performed hemostasis must be double-checked, as there is a possible association with acquired von Willebrand disease, as described in two pediatric cases.
MAs usually have a good prognosis, and the treatment of choice is complete surgical resection by partial or radical nephrectomy, depending on size; definitive diagnosis is established based on histopathological studies and immunohistochemistry (13-15).
Macroscopically, MA is described as a well-circumscribed brownish-yellow mass and with the presence of pseudocapsule (4,7,8). Microscopically, these neoplasms are comprised of tubules of different sizes and shapes, divided into lobes with fine fibrovascular septa; in addition, their cells are characterized by small cell nuclei and very low mitotic activity (2,5). These tumors have the following immunohistochemical pattern: positive for vimentin, pancytokeratin, WT1 and CD57; negative for CK7, AMACR, and CD10 (2,5).
Li et al. (16) conducted a cohort study of 18 patients with MA in which, through pathological examination, they found that 6 (33.3%) tumors had other carcinoma components concomitantly and 2 (11.1%) were malignant MA, a surprisingly high proportion of simultaneously malignant cases. In the same study, the authors suggested a subclassification of these neoplasms into classic MA, malignant MA, and MA with concomitant malignant component, concluding that their biological behavior is not yet well defined (16).
As reported in the literature and with the experience of the case described here, it can be said that MA is a rare pathology that is within the differential diagnosis of upper urinary tract masses. Pre-surgical diagnosis is difficult and treatment in general does not differ from the standard for renal carcinoma or urothelial carcinoma of the upper urinary tract, depending on the case. The diagnostic suspicion of this type of tumor may increase in patients in whom endoscopic assessment with biopsy is possible along with magnetic resonance imaging to complement imaging studies. The surgical treatment implemented in the case reported here is based on the recommendations of the 2020 European Association of Urology Guidelines on Upper Urinary Tract Urothelial Carcinoma (staging: cT3N1M0) (17,18).
Conclusion
MA is a very rare benign tumor that affects the upper urinary tract and is difficult to differentiate from other tumors with imaging studies. Its diagnosis is usually made by histopathological study and immunohistochemistry, although some research suggests the usefulness of pre-surgical fine-needle aspiration cytology. Given the low prevalence of this disease, reports and case series are of great importance as they allow to broaden the knowledge on the subject and to propose possible pre-surgical diagnostic strategies that, in turn, allow to implement treatment strategies that preserve the renal unit involved.
Ethical considerations
According to Resolution 8430 of 1993 of the Ministry of Health of Colombia (19), this case report is a risk-free investigation. The patient completed an informed consent form, and the principles outlined in the Declaration of Helsinki (20) were adhered to.
Conflicts of interest
None stated by the authors.
Funding
None stated by the authors.
Acknowledgments
None stated by the authors.
References
1.Jiang T, Li W, Lin D, Wang J, Ding Z. Imaging features of metanephric adenoma and their pathological correlation. Clin Radiol. 2019;74(5):408.e9-17. https://doi.org/h2mz.
2.Zhu Q, Zhu W, Wu J, Chen W, Wang S. The clinical and CT imaging features of metanephric adenoma. Acta Radiol. 2014;55(2):231-8. https://doi.org/h2m3.
3.Barkan GA, Wojcik EM, Nayar R, Savic-Prince S, Quek ML, Kurtycz DF, et al. The Paris System for Reporting Urinary Cytology: The Quest to Develop a Standardized Terminology. Adv Anat Pathol. 2016;23(4):193-201. https://doi.org/gkb4km.
4.Rodríguez-Zarco E, Vallejo-Benítez A, Farfán-López FJ, Vilches-Arenas Á, Pereira-Gallardo S, Vázquez-Ramírez FJ. Adenoma metanéfrico: presentación de 2 casos y revisión de la literatura. Arch. Specialist. Urol. 2017;70(9):792-6.
5.Ding Y, Wang C, Li X, Jiang Y, Mei P, Huang W, et al. Novel clinicopathological and molecular characterization of metanephric adenoma: a study of 28 cases. Diagn Pathol. 2018;13(1):54. https://doi.org/gmbs4g.
6.Santafé-Galvis JS, Cruz-Arévalo DA, Salgado-Tovar JM. Una masa renal poco común en una adolescente - presentación de caso y revisión de la literatura. Revista Urología Colombiana. 2019;28(4):321-9. https://doi.org/h2nz.
7.Obulareddy SJ, Xin J, Truskinovsky AM, Anderson JK, Franklin MJ, Dudek AZ. Metanephric adenoma of the kidney: an unusual diagnostic challenge. Rare Tumors. 2010;2(2):e38. https://doi.org/h2n2.
8.Raman SP, Hruban RH, Fishman EK. Beyond renal cell carcinoma: rare and unusual renal masses. Abdom Imaging. 2012;37(5):873-84. https://doi.org/h2n3.
9.Yan J, Cheng JL, Li CF, Lian YB, Zheng Y, Zhang XP, et al. The findings of CT and MRI in patients with metanephric adenoma. Diagn Pathol. 2016;11(1):104. https://doi.org/h2nw.
10.Jiménez-Heffernan JA, Tejerina E, González-Peramato P, Vicandi B, López-García A. Cytologic features of metanephric adenoma of the kidney. Cytojournal. 2009;6:7. https://doi.org/c4t76g.
11.Blanco LZ, Schein CO, Patel T, Heagley DE, Cimbaluk DJ, Reddy V, et al. Fine-needle aspiration of metanephric adenoma of the kidney with clinical, radiographic and histopathologic correlation: a review. Diagn Cytopathol. 2013;41(8):742-51. https://doi.org/h2n4.
12.Le Nué R, Marcellin L, Ripepi M, Henry C, Kretz JM, Geiss S. Conservative treatment of metanephric adenoma. A case report and review of the literature. J Pediatr Urol. 2011;7(4):399-403. https://doi.org/dgsfft.
13.Van Poppel H, Da Pozzo L, Albrecht W, Matveev V, Bono A, Borkowski A, et al. A prospective, Randomised EORTC Intergroup Phase 3 study comparing The Oncologic outcome of Elective Nephron-sparing surgery and Radical Nephrectomy for Low-Stage renal cell carcinoma. Eur Urol. 2011;59(4):543-52. https://doi.org/fj27kh.
14.14. MacLennan S, Imamura M, Lapitan MC, Omar MI, Lam TB, Hilvano-Cabungcal AM, et al. Systematic review of perioperative and quality-of-life outcomes following surgical management of localised renal cancer. Eur Urol. 2012;62(6):1097-117. https://doi.org/f2j5bg.
15.Thompson RH, Boorjian SA, Lohse CM, Leibovich BC, Kwon ED, Cheville JC, et al. Radical nephrectomy for PT1A renal masses may be associated with decreased overall survival compared with Partial Nephrectomy. J Urol. 2008;179(2):468-73. https://doi.org/bq2dsf.
16.Li G, Tang Y, Zhang R, Song H, Zhang S, Niu Y. Adult metanephric adenoma presumed to be all benign? A clinical perspective. BMC Cancer. 2015;15(1):310. https://doi.org/f689d2.
17.Margulis V, Shariat SF, Matin SF, Kamat AM, Zigeuner R, Kikuchi E, et al. Outcomes of radical nephroureterectomy: A series from the upper tract urotelial carcinoma collaboration. Cancer. 2009;115(6):1224-33. https://doi.org/dbhgqk.
18.Rouprêt M, Babjuk M, Burger M, Capoun O, Cohen D, Compérat EM, et al. European Association of Urology guidelines on upper urinary Tract Urothelial Carcinoma: 2020 Update. Eur Urol. 2021;79(1):62-79. https://doi.org/gpfmhq.
19.Colombia. Ministerio de Salud. Resolución 8430 de 1993 (octubre 4): Por la cual se establecen las normas científicas, técnicas y administrativas para la investigación en salud. Bogotá D.C.; octubre 4 de 1993.
20.World Medical Association (WMA). WMA Declaration of Helsinki - Ethical principles for medical research involving human subjects. Fortaleza: 64th WMA General Assembly; 2013.
Referencias
Jiang T, Li W, Lin D, Wang J, Ding Z. Imaging features of metanephric adenoma and their pathological correlation. Clin Radiol. 2019;74(5):408.e9-17. https://doi.org/h2mz.
Zhu Q, Zhu W, Wu J, Chen W, Wang S. The clinical and CT imaging features of metanephric adenoma. Acta Radiol. 2014;55(2):231-8. https://doi.org/h2m3.
Barkan GA, Wojcik EM, Nayar R, Savic-Prince S, Quek ML, Kurtycz DF, et al. The Paris System for Reporting Urinary Cytology: The Quest to Develop a Standardized Terminology. Adv Anat Pathol. 2016;23(4):193-201. https://doi.org/gkb4km.
Rodríguez-Zarco E, Vallejo-Benítez A, Farfán-López FJ, Vilches-Arenas Á, Pereira-Gallardo S, Vázquez-Ramírez FJ. Adenoma metanéfrico: presentación de 2 casos y revisión de la literatura. Arch. Specialist. Urol. 2017;70(9):792-6.
Ding Y, Wang C, Li X, Jiang Y, Mei P, Huang W, et al. Novel clinicopathological and molecular characterization of metanephric adenoma: a study of 28 cases. Diagn Pathol. 2018;13(1):54. https://doi.org/gmbs4g.
Santafé-Galvis JS, Cruz-Arévalo DA, Salgado-Tovar JM. Una masa renal poco común en una adolescente - presentación de caso y revisión de la literatura. Revista Urología Colombiana. 2019;28(4):321-9. https://doi.org/h2nz.
Obulareddy SJ, Xin J, Truskinovsky AM, Anderson JK, Franklin MJ, Dudek AZ. Metanephric adenoma of the kidney: an unusual diagnostic challenge. Rare Tumors. 2010;2(2):e38. https://doi.org/h2n2.
Raman SP, Hruban RH, Fishman EK. Beyond renal cell carcinoma: rare and unusual renal masses. Abdom Imaging. 2012;37(5):873-84. https://doi.org/h2n3.
Yan J, Cheng JL, Li CF, Lian YB, Zheng Y, Zhang XP, et al. The findings of CT and MRI in patients with metanephric adenoma. Diagn Pathol. 2016;11(1):104. https://doi.org/h2nw.
Jiménez-Heffernan JA, Tejerina E, González-Peramato P, Vicandi B, López-García A. Cytologic features of metanephric adenoma of the kidney. Cytojournal. 2009;6:7. https://doi.org/c4t76g.
Blanco LZ, Schein CO, Patel T, Heagley DE, Cimbaluk DJ, Reddy V, et al. Fine-needle aspiration of metanephric adenoma of the kidney with clinical, radiographic and histopathologic correlation: a review. Diagn Cytopathol. 2013;41(8):742-51. https://doi.org/h2n4.
Le Nué R, Marcellin L, Ripepi M, Henry C, Kretz JM, Geiss S. Conservative treatment of metanephric adenoma. A case report and review of the literature. J Pediatr Urol. 2011;7(4):399-403. https://doi.org/dgsfft.
Van Poppel H, Da Pozzo L, Albrecht W, Matveev V, Bono A, Borkowski A, et al. A prospective, Randomised EORTC Intergroup Phase 3 study comparing The Oncologic outcome of Elective Nephron-sparing surgery and Radical Nephrectomy for Low-Stage renal cell carcinoma. Eur Urol. 2011;59(4):543-52. https://doi.org/fj27kh.
MacLennan S, Imamura M, Lapitan MC, Omar MI, Lam TB, Hilvano-Cabungcal AM, et al. Systematic review of perioperative and quality-of-life outcomes following surgical management of localised renal cancer. Eur Urol. 2012;62(6):1097-117. https://doi.org/f2j5bg.
Thompson RH, Boorjian SA, Lohse CM, Leibovich BC, Kwon ED, Cheville JC, et al. Radical nephrectomy for PT1A renal masses may be associated with decreased overall survival compared with Partial Nephrectomy. J Urol. 2008;179(2):468-73. https://doi.org/bq2dsf.
Li G, Tang Y, Zhang R, Song H, Zhang S, Niu Y. Adult metanephric adenoma presumed to be all benign? A clinical perspective. BMC Cancer. 2015;15(1):310. https://doi.org/f689d2.
Margulis V, Shariat SF, Matin SF, Kamat AM, Zigeuner R, Kikuchi E, et al. Outcomes of radical nephroureterectomy: A series from the upper tract urotelial carcinoma collaboration. Cancer. 2009;115(6):1224-33. https://doi.org/dbhgqk.
Rouprêt M, Babjuk M, Burger M, Capoun O, Cohen D, Compérat EM, et al. European Association of Urology guidelines on upper urinary Tract Urothelial Carcinoma: 2020 Update. Eur Urol. 2021;79(1):62-79. https://doi.org/gpfmhq.
Colombia. Ministerio de Salud. Resolución 8430 de 1993 (octubre 4): Por la cual se establecen las normas científicas, técnicas y administrativas para la investigación en salud. Bogotá D.C.; octubre 4 de 1993.
World Medical Association (WMA). WMA Declaration of Helsinki - Ethical principles for medical research involving human subjects. Fortaleza: 64th WMA General Assembly; 2013.
Cómo citar
APA
ACM
ACS
ABNT
Chicago
Harvard
IEEE
MLA
Turabian
Vancouver
Descargar cita
Licencia

Esta obra está bajo una licencia internacional Creative Commons Atribución 4.0.
Los autores al someter sus manuscritos conservarán sus derechos de autor. La revista tiene el derecho del uso, reproducción, transmisión, distribución y publicación en cualquier forma o medio.
El Formulario de Divulgación Uniforme para posibles Conflictos de Interés y los oficios de cesión de derechos y de responsabilidad deben ser entregados junto con el original.
Aquellos autores/as que tengan publicaciones con esta revista, aceptan los términos siguientes:
Los autores/as conservarán sus derechos de autor y garantizarán a la revista el derecho de primera publicación de su obra, el cual estará simultáneamente sujeto a la Licencia de reconocimiento de Creative Commons 4.0 que permite a terceros compartir la obra siempre que se indique su autor y su primera publicación en esta revista.
Los autores/as podrán adoptar otros acuerdos de licencia no exclusiva de distribución de la versión de la obra publicada (p. ej.: depositarla en un archivo telemático institucional o publicarla en un volumen monográfico) siempre que se indique la publicación inicial en esta revista.
Se permite y recomienda a los autores/as difundir su obra a través de Internet (p. ej.: en archivos telemáticos institucionales o en su página web) antes y durante el proceso de envío, lo cual puede producir intercambios interesantes y aumentar las citas de la obra publicada. (Véase El efecto del acceso abierto).


























