Somnolencia diurna excesiva en estudiantes de noveno semestre de Medicina de la Universidad Nacional de Colombia
Excessive daytime drowsiness in ninth-semester medical students attending the Universidad Nacional de Colombia
Palabras clave:
epidemiología, estudiantes de medicina, prevalencia, trastornos del sueño, trastornos por excesiva somnolencia (es)epidemiology, students, medical, prevalence, sleep disorders, disorders of excessive somnolence. (en)
Antecedentes. Tradicionalmente los estudiantes de medicina duermen poco, estudian largas jornadas nocturnas y como consecuencia padecen somnolencia diurna excesiva produciendo disminución en la atención que afecta su calidad de vida y rendimiento académico. Lo anterior se suma a los turnos nocturnos y al pobre conocimiento de higiene del sueño. En Colombia se conoce poco sobre la prevalencia, la gravedad de este síntoma y los efectos en esta población, al igual que en otros grupos como correturnos, vigilantes, personal sanitario, pilotos, militares, etc.
Objetivo. Determinar la incidencia de somnolencia diurna excesiva en estudiantes de noveno semestre de medicina de la Universidad Nacional de Colombia, quienes realizan turnos nocturnos en las rotaciones asignadas y evaluar su relación con la calidad e higiene de sueño.
Material y métodos. Estudio descriptivo transversal, realizado en una muestra de estudiantes 76,14% (n=83/ 109) de noveno semestre de medicina que aceptaron participar en la investigación mediante consentimiento informado. Se aplicó la escala de somnolencia de Epworth y el índice de calidad de sueño de Pittsburgh validados localmente y el índice de higiene de sueño validado en Perú.
Resultados. Los evaluados tuvieron un promedio de edad de 23 años, presentaron somnolencia diurna excesiva el 60,24% (n=50/83). Se halló 79,52% (n=66/83) de sujetos malos dormidores y 44,58% (n=37/83) con mala higiene de sueño.
Conclusiones. La prevalencia de somnolencia diurna excesiva en la población estudiada es cuantitativamente importante y superior a la hallada en otros estudios, muestra relación con la mala calidad de sueño y con una mala higiene de sueño considerable.
Background. Medical students traditionally sleep very little, study during long nocturnal periods and consequently suffer excessive daytime sleepiness, thereby leading to reduced attention which affects their quality of life and academic performance. The foregoing must be added to night shifts/duty and poor knowledge regarding the hygiene of sleep. Little is known in Colombia about this symptom's prevalence and seriousness or its effects on this population or on other groups such as shift-workers (working double shifts), watchmen, sanitary personnel, pilots, soldiers, etc.
Objective. Determining the incidence of excessive daytime sleepiness in ninth-semester medical students attending the Universidad Nacional de Colombia who were involved in night shifts as part of their assigned rotations and evaluating its relationship with the quality and hygiene of sleep.
Materials and methods. This was a cross-sectional descriptive study which was carried out on a sample of ninth-semester medical students (76.14%; n=83/109) who agreed to participate in the investigation by signing an informed consent form. The Epworth sleepiness scale was applied as was the locally-validated Pittsburgh sleep quality index and sleep hygiene index validated in Peru.
Results. The students being evaluated were 23 years old on average; 60.24% (n=50/83) of them presented excessive daytime sleepiness. It was found that 79.52% (n=66/83) were poor sleepers and 44.58% (n=37/83) had bad sleep hygiene.
Conclusions. The prevalence of excessive daytime sleepiness in the population being studied was quantitatively important and higher than that found in other studies, showing a relationship with poor sleep quality and considerable poor sleep hygiene.
Investigación original
SOMNOLENCIA DIURNA EXCESIVA EN ESTUDIANTES DE NOVENO SEMESTRE DE MEDICINA DE LA UNIVERSIDAD NACIONAL DE COLOMBIA
Excessive daytime drowsiness in ninth-semester medical students attending the Universidad Nacional de Colombia
Franklin Escobar-Córdoba1, Rafael Eduardo Benavides-Gélvez2, Hilda Gabriela Montenegro-Duarte2, Javier Hernando Eslava-Schmalbach3
1 Profesor Asociado de Psiquiatría. Facultad de Medicina, Universidad Nacional de Colombia, Bogotá. Director Científico Centro de Sueño Fundación Sueño Vigilia Colombia Bogotá.
2 Estudiante de noveno semestre. Facultad de Medicina, Universidad Nacional de Colombia, Bogotá.
3 Profesor Titular, Instituto de Investigaciones Clínicas, Facultad de Medicina, Universidad Nacional de Colombia, Bogotá.
Correspondencia: feescobarc@unal.edu.co
Recibido: 19/08/11/ Aceptado publicación: 30/08/11/
Resumen
Antecedentes. Tradicionalmente los estudiantes de medicina duermen poco, estudian largas jornadas nocturnas y como consecuencia padecen somnolencia diurna excesiva produciendo disminución en la atención que afecta su calidad de vida y rendimiento académico. Lo anterior se suma a los turnos nocturnos y al pobre conocimiento de higiene del sueño. En Colombia se conoce poco sobre la prevalencia, la gravedad de este síntoma y los efectos en esta población, al igual que en otros grupos como correturnos, vigilantes, personal sanitario, pilotos, militares, etc.
Objetivo. Determinar la incidencia de somnolencia diurna excesiva en estudiantes de noveno semestre de medicina de la Universidad Nacional de Colombia, quienes realizan turnos nocturnos en las rotaciones asignadas y evaluar su relación con la calidad e higiene de sueño.
Material y métodos. Estudio descriptivo transversal, realizado en una muestra de estudiantes 76,14% (n=83/ 109) de noveno semestre de medicina que aceptaron participar en la investigación mediante consentimiento informado. Se aplicó la escala de somnolencia de Epworth y el índice de calidad de sueño de Pittsburgh validados localmente y el índice de higiene de sueño validado en Perú.
Resultados. Los evaluados tuvieron un promedio de edad de 23 años, presentaron somnolencia diurna excesiva el 60,24% (n=50/83). Se halló 79,52% (n=66/83) de sujetos malos dormidores y 44,58% (n=37/83) con mala higiene de sueño.
Conclusiones. La prevalencia de somnolencia diurna excesiva en la población estudiada es cuantitativamente importante y superior a la hallada en otros estudios, muestra relación con la mala calidad de sueño y con una mala higiene de sueño considerable.
Palabras claves: epidemiología, estudiantes de medicina, prevalencia, trastornos del sueño, trastornos por excesiva somnolencia (DcCS).
Summary
Background. Medical students traditionally sleep very little, study during long nocturnal periods and consequently suffer excessive daytime sleepiness, thereby leading to reduced attention which affects their quality of life and academic performance. The foregoing must be added to night shifts/duty and poor knowledge regarding the hygiene of sleep. Little is known in Colombia about this symptom's prevalence and seriousness or its effects on this population or on other groups such as shift-workers (working double shifts), watchmen, sanitary personnel, pilots, soldiers, etc.
Objective. Determining the incidence of excessive daytime sleepiness in ninth-semester medical students attending the Universidad Nacional de Colombia who were involved in night shifts as part of their assigned rotations and evaluating its relationship with the quality and hygiene of sleep.
Materials and methods. This was a cross-sectional descriptive study which was carried out on a sample of ninth-semester medical students (76.14%; n=83/109) who agreed to participate in the investigation by signing an informed consent form. The Epworth sleepiness scale was applied as was the locally-validated Pittsburgh sleep quality index and sleep hygiene index validated in Peru.
Results. The students being evaluated were 23 years old on average; 60.24% (n=50/83) of them presented excessive daytime sleepiness. It was found that 79.52% (n=66/83) were poor sleepers and 44.58% (n=37/83) had bad sleep hygiene.
Conclusions. The prevalence of excessive daytime sleepiness in the population being studied was quantitatively important and higher than that found in other studies, showing a relationship with poor sleep quality and considerable poor sleep hygiene.
Key words: epidemiology, students, medical, prevalence; sleep disorders, disorders of excessive somnolence (MeSH).
Introducción
Los trastornos del sueño en general constituyen uno de los problemas de salud más relevantes de la sociedad occidental. La calidad del sueño es fundamental como factor determinante de salud y elemento propiciador de una buena calidad de vida. Uno de los principales trastornos del sueño es la somnolencia diurna excesiva (SDE).
El individuo con SDE manifiesta un deseo de dormir irresistible ante cualquier circunstancia, incluso en actividades que demandan un alto nivel de alertamiento, se considera patológica, si se presenta por períodos de semanas y meses. Se clasifica según la severidad en leve (sin episodios de sueño involuntario pero con bostezos frecuentes, alteraciones atencionales y en la concentración), moderada (al realizar actividades sedentarias el individuo se duerme involuntariamente) y severa (el sueño se presenta aún durante la actividad física) (1,2).
Se requiere para la aproximación al diagnóstico una evaluación médica completa que incluya el uso de cuestionarios y estudios de laboratorio de sueño como la polisomnografía (PSG) y la prueba de latencias múltiples del sueño (PLMS) y de mantenimiento de la vigilia (3). La PSG y la PLMS permiten establecer la etiología de la SDE crónica (2). La SDE puede ser primaria o secundaria. Dada la frecuencia de estas, se diagnostica inicialmente SDE secundaria si hay una condición subyacente y SDE primaria una vez descartadas otras causas (1,2).
La prevalencia en el ámbito global se calcula en alrededor del 16%. En Colombia existen pocos estudios publicados sobre la prevalencia de la SDE (4), sumado a la ausencia de estudios poblacionales que permitan evaluar el efecto sobre la salud de los trabajadores por turnos como vigilantes, personal de salud, conductores, pilotos, controladores de tránsito aéreo, auxiliares de vuelo, policías, militares, entre otros. Se calcula que del 15 al 30% de los accidentes de tránsito se deben a la somnolencia frente al volante (5,6). Se desconocen cifras acerca de la accidentalidad laboral nacional relacionadas con la SDE, que también disminuye la productividad y el funcionamiento social de los afectados.
Los correturnos nocturnos tienen alrededor de ocho horas de sueño por semana menos que los sujetos que realizan turnos diurnos. Este problema seguirá incrementándose en tanto se aumente el número de trabajadores por turno, para garantizar el rendimiento laboral y económico (7). Lo anterior, sumado a la alternancia semanal de turnos diurnos, vespertinos y nocturnos en un mismo individuo generando en éste grandes dificultades en la adaptación al ciclo sueño-vigilia, que se asocia con frecuencia a insomnio y SDE (7-9). Dicha somnolencia se manifiesta principalmente con predominio vesperal, implica trastornos digestivos, irritabilidad y progresiva disminución en la atención y la coordinación.
Estas circunstancias han producido la privación voluntaria de sueño o la llamada deuda crónica de sueño. Esta privación voluntaria aguda o crónica de sueño, usualmente se produce por estrés ante factores sociales o económicos (2). Al no conciliar un sueño suficiente, se puede estar ante una privación severa que empeora el desempeño y el rendimiento en las actividades de la vida diaria. Además la falta de sueño se asocia con mayor prevalencia de diversas enfermedades somáticas y trastornos psiquiátricos (10), así como problemas sociales, provocando una jornada diurna de mala calidad, irritabilidad, cefalea o dificultad para concentrarse y recordar cosas sencillas.
Es conocido que los estudiantes de medicina duermen poco, estudian largas jornadas nocturnas y desde ciertos semestres realizan turnos nocturnos de más de doce horas, como consecuencia padecen SDE generando disminución en la atención y afectando su calidad de vida. Es evidente el impacto que tiene la realización de turnos nocturnos en la calidad de vida de las personas. El propósito de este estudio fue determinar la prevalencia de SDE en la población de estudiantes de noveno semestre de medicina de la Universidad Nacional de Colombia sede Bogotá (UNCB) matriculados en la asignatura Cirugía I (cirugía general) en el período 01 del año 2010, correlacionar los hallazgos con el rendimiento académico de los estudiantes y sus hábitos de higiene de sueño. Es importante resaltar que esta población en el período mencionado, por primera vez en la carrera de medicina, realiza turnos de más de doce horas.
Material y métodos
Previo a la recolección de los datos se realizó una búsqueda electrónica en bases de datos: Pubmed, Lilacs, Scielo y Scopus cruzando las palabras claves identificadas como términos Medical Subject Headings [MeSH] "Disorders of excessive somnolence" y "Students, medical", "Disorders of excessive somnolence" y "Underachievement" y "Hypnotics y Sedatives" y "Population", se incluyeron artículos publicados en diferentes idiomas, de 1966 a 2010. El resultado de la búsqueda arrojó veinte artículos. De estas publicaciones se leyeron los resúmenes y los que tenían mayor relación con el objetivo principal de la investigación; trece estudios, se obtuvieron en texto completo (11-23). La información obtenida sirvió de base para estructurar este estudio descriptivo transversal, realizado en la población de estudiantes que aparecían en el listado proporcionado por el Departamento de Cirugía y que cursaban la asignatura cirugía I de la carrera de medicina de la UNCB matriculados en noveno semestre y durante el primer período académico del año 2010. Cada uno de los participantes dio su consentimiento por escrito previo conocimiento del bajo riesgo del estudio. Los instrumentos de medición usados fueron la Escala de Somnolencia de Epworth (ESE) y el Índice de Calidad de Sueño de Pittsburg (ICSP), validados localmente y el Índice de Higiene de Sueño (IHS) validado en Perú; descritos a continuación (24-27).
Índice de Higiene de Sueño
El IHS, consta de trece preguntas de realización individual, que busca evaluar la presencia de comportamientos que se han identificado como irruptores de la higiene de sueño. A los sujetos se les pide que indiquen cuán frecuentemente incurren en comportamientos específicos (siempre, frecuentemente, alguna veces, raramente, nunca).
Los componentes que estructuran el IHS se derivaron de los criterios diagnósticos de higiene de sueño inadecuada de la Clasificación Internacional de Trastornos del Sueño de la Asociación Americana de Medicina del Sueño (2). Los puntajes de cada componente se suman obteniendo una evaluación global de la higiene de sueño. Los puntajes muy altos son indicativos de un estado maladaptativo de la higiene de sueño (26).
Escala de Somnolencia de Epworth
La ESE es una encuesta de reporte individual con ocho preguntas que genera puntajes de 0 a 24. Los puntajes mayores a 10 sugieren SDE. Esta escala tiene buenas propiedades psicométricas y se ha demostrado que diferencia individuos con o sin trastornos del sueño y aquellos que han sido o no privados de sueño (24).
Índice de Calidad de Sueño de Pittsburg
El ICSP es un instrumento de llenado individual con 19 preguntas que busca evaluar la calidad de sueño y las perturbaciones del sueño durante un mes en poblaciones clínicas y no clínicas. Se puntúa en un rango de 0 a 21, donde un puntaje total mayor de cinco indica mala calidad de sueño (25).
Resultados
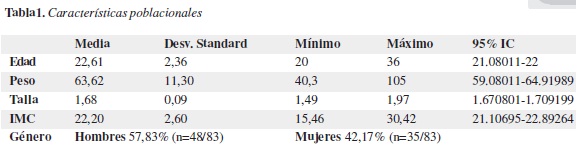
Se incluyó en el estudio al 76,14% (n=83/109) de la población de estudiantes, sus principales características se muestran en la tabla 1. Tras aplicar la ESE, se dividió al total de estudiantes en dos categorías: somnolencia normal, que sería aquella que no necesita tratamiento médico y es la esperada en la población general; y SDE, la cual debería ser abordada médicamente por ser patológica y tener repercusiones funcionales en las actividades básicas cotidianas. Se halló que el 39,76% (n=33/83) obtuvo puntajes entre 0-9 (somnolencia normal a leve) rango en el cual no es necesaria atención médica, y el restante 60,24% (n=50/83) puntajes iguales o superiores a diez, lo cual clasifica para SDE.
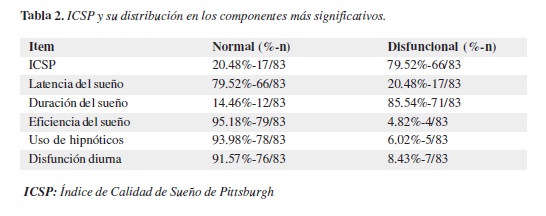
Se continuó la evaluación determinando la calidad de sueño de los encuestados basados en los resultados del ICSP, observando que sólo el 20,48% (n=17/83) de los encuestados es buen dormidor, dejando un 79,52% (n=66/83) de malos dormidores. Por componentes del ICSP, la latencia (tiempo requerido para conciliar el sueño) se vio aumentada (puntaje de 2-3) en un 20,48% (11=17/83), la duración del sueño (tiempo en cama destinado a dormir), de cinco horas o menos (puntaje 2-3), se encontró en un 85,54% (n=71/83), eficiencia del sueño (duración de sueño en la que efectivamente durmió) igual o mayor al 85% (puntaje 0) llegó al 95,18% (11=79/83), las perturbaciones no fueron significativas, pero llama la atención hallar un 6,02% (n=5/83) con uso de hipnóticos; la disfunción diurna encontrada sólo alcanza el 8,43% (n=7/ 83) (Tabla 2).
Al evaluar el IHS se tomó como punto de corte 35 (rango=13-65) dada su significancia estadística al relacionarse con la ESE (Pearson chi2=9.1695, Pr=0.002) y el ICSP (Pearson chi2=3.8339, Pr=0.050), dando como resultado un 55.42% (n=46/83) de estudiantes con buena o aceptable higiene de sueño y un 44.58% (n=37/ 83) con mala higiene de sueño.
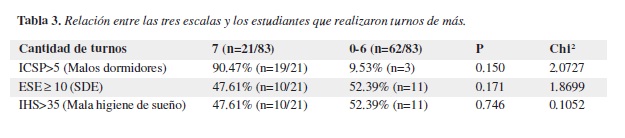
La cantidad de turnos nocturnos de 12 horas o más realizados en el último mes por la población encuestada, como primer variable a evaluar dentro del contexto de SDE, mala calidad de sueño y mala higiene de sueño, fue en promedio de 4.38/ mes. Para relacionarlo con la ESE, el ICSP y el IHS, se tomó como punto de corte el percentil 75 (7 turnos) valorándolos como la población que hizo más turnos 25,3% (n=21/83) de los encuestados. En esta población se encontró un 90,47% (n=19/ 21) de malos dormidores, 47,61% (n=10/21) de estudiantes con SDE que necesitaban atención médica y 47,61% (n=10/21) de encuestados con mala higiene de sueño (Tabla 3).
La calificación promedio de los estudiantes en la asignatura Cirugía I, en la cual se realizaron los turnos, fue de 4,0/5,0, aunque es necesario precisar que aquellos estudiantes que perdieron la materia se rehusaron a participar en el estudio. Dado este sesgo, se optó por evaluar las calificaciones mayores a 4,0/5,0 (36.14%-n=30/83) y su relación con la calidad de sueño, la somnolencia diurna y la higiene de sueño; y se encontró que el 20% (n=6/30) de las notas superiores correspondieron a buenos dormidores, 43,33% (n=13/30) con somnolencia normal y 56,6% (n=17/30) de las notas mayores a 4,0/5,0 son de estudiantes con higiene de sueño buena o aceptable (Tabla 4).
Se asociaron algunos resultados, y evidenció que el 60.56% (n=43/71) de los estudiantes con cinco horas o menos de sueño, sufrían de somnolencia diurna patológica y un 85,91% (n=61/71) eran malos dormidores. El 76,47% (n=13/17) de los encuestados con latencia aumentada, padecían SDE. El 66% (n=33/50) de los pacientes con SDE poseían mala higiene de sueño, así como el 56,06% (n=37/66) de los malos dormidores.
Discusión
Para la población de este estudio, la prevalencia puntual de SDE (60,24%, n=50/83, ESE>10) indica que más de la mitad de la población estudiada sufre de SDE, de moderada a grave según la clasificación de la ESE. En estudios previos realizados con poblaciones similares a la nuestra se evidencia que es recurrente encontrar SDE en los estudiantes de medicina que realicen o no turnos mayores de 12 horas (11,28). Incluso se encontró que la prevalencia de SDE es mayor a la reportada en médicos internos y residentes de algunas muestras recolectadas pero con características diferentes como lo reportó Handel et al (29). Por su estudio con residentes de medicina de emergencia (n=602) en quienes encontró ESE=11-16 con SDE (38%, n=229/602) y el 7% con SDE severa (ESE>16).
Teniendo en cuenta un estudio previo realizado en estudiantes no expuestos a turnos mayores de 12 horas de la misma universidad y facultad, se encontraron resultados consistentes en la pre-valencia de SDE al compararlos (59,6%, n=59/ 99, ESE>10 vs 60.24%, n=50/109, ESE>10). Esta prevalencia encontrada es superior a la prevalencia global de la SDE reportada alrededor del 16% (6). Situación que plantearía que el hacer turnos (promedio=4.38/mes) no es indiferente a las dos poblaciones en cuanto a la presencia de SDE.
En cuanto a la calidad de sueño se halló que 2/3 de la población (79,52% n=66/83) superan la puntuación de cinco en el ICSP siendo definidos como malos dormidores o con pobre calidad de sueño. Este hallazgo es muy superior a los estudios previos realizados bajo parámetros similares en distintas poblaciones (12).
Las alteraciones halladas en calidad subjetiva, latencia, duración, eficiencia habitual del sueño, no fueron significativas, pero llama la atención encontrar un aumento de la latencia del sueño (20,48%, n=17/83), una duración disminuida del sueño (igual o menor a 5 horas, 85,54%, n=71/ 83) y 6,02% (n=5/83) de uso de hipnóticos, lo cual es preocupante al tratarse de una población pequeña. Sierra et al, en una muestra de 716 estudiantes universitarios de psicología, población que no realiza turnos reportó el consumo de hipnóticos en 13% y mayor en mujeres que en hombres (30). Varios autores refieren que entre 10 y 15% de la población mundial toma hipnóticos, el 10% de la población general refiere consumo, y 7,1% lo hace de forma ocasional, este último dato es similar a la población estudiada que consumía hipnóticos en un 6.02% (n=5/ 83), (22-23).
Se evaluó la higiene del sueño evidenciando que algo menos de la mitad de los estudiantes (44,58%, n=37/83) tienen mala higiene de sueño, tratándose de estudiantes de medicina de los últimos años de la carrera. Los resultados muestran malos hábitos como ir a la cama estresado, enojado, molesto, o nervioso; acostarse a dormir en horas diferentes cada día, usar la cama para estudiar, leer, ver televisión, etc, e ir a la cama con preocupaciones además de planear y organizar horarios, cuando se debería destinar ese tiempo a dormir. Estas actividades no se recomiendan y explican el aumento de la latencia del sueño reportada en ICSP, y también reflejan el desconocimiento acerca de la higiene del sueño. Al comparar el rendimiento académico y la higiene del sueño (56,6%, n=17/30) se encontró que los estudiantes con mejores calificaciones tienen buena o aceptable higiene de sueño.
Más de la mitad (66%, n=33/50) de los estudiantes con SDE tuvieron mala higiene de sueño y la mayoría de malos dormidores tienen malos hábitos del sueño (56.06%, n=37/66). De los estudiantes que refirieron malos hábitos de higiene del sueño, se encontraron datos aún más elevados y más evidentes si se tomaba parte de la muestra correspondiente a los que realizaron más turnos, encontrando que casi la mitad (47,61%, n=10/21) de encuestados tienen mala higiene de sueño.
Al tratarse de estudiantes que realizan por primera vez turnos en el curso de la carrera de medicina cabe resaltar una prevalencia de SDE elevada (ESE>10) en relación a la reportada por Wada et al en residentes japoneses de medicina, en quienes se evaluaron las horas de sueño (menos de cinco horas/día) y la frecuencia de los turnos (SDE=59,6%, n=59/99 vs SDE= 28,1%, n=55/196 respectivamente) encontrando asociaciones entre dormir poco (cOR=1.57, IC95%=1.02-2.16) y fumar cigarrillo (cOR=1.65, IC95%=1.01-2.32) con la presencia de SDE (31). Lo anterior es compatible con los hallazgos de nuestra población, las personas que tienen mayor SDE y necesitan atención médica corresponden a las que realizan más turnos (7 turnos al mes percentil 75 (25,3% n=21/83) de los cuales el 90,47% (n=19/21) son malos dormidores y 47,61% (n=10/21) tienen SDE.
El rendimiento académico no se vio afectado, en general, la mayoría de los estudiantes obtuvo buenas notas pese a una alta prevalencia de SDE, haciendo la salvedad que existe sesgo, debido a que los estudiantes que no aprobaron la materia no desearon participar en el estudio. Se halló que las mejores calificaciones: mayores a 4,0/50 (36,14% n=30/83) correspondieron a buenos dormidores y a somnolencia diurna no patológica (20% n=6/30 y 43,33% n=13/30).
Los estudiantes con mejor rendimiento académico son en su gran mayoría malos dormidores, pero de ellos la proporción que padece SDE corresponde a menos de la mitad y además la mayoría tienen buenos conocimientos acerca de higiene del sueño que es un factor protector en relación con la SDE (20%, n=6/30; 43,33%, n=13/30; y 56,6% n=17/30). La muestra era una población francamente afectada por la SDE en rangos patológicos, en su mayoría malos dormidores con malos hábitos de higiene del sueño.
En este estudio no es clara la relación de SDE y el rendimiento académico debido al sesgo de selección. Pero es importante realizar estudios que relacionen SDE y el desempeño académico, dado que es un síntoma común que influye ya directa o indirectamente en el proceso académico, e incluso puede llevar a fracaso escolar (15,28,32).
En términos generales, se hacen evidentes las limitaciones de este estudio, los cuestionarios son autoaplicados y por ende sometidos a la subjetividad de quienes los diligencian, con la posibilidad de tener sesgo de memoria. Tanto la calidad de sueño y la somnolencia son variables subjetivas e individuales y se subestiman o sobrestiman al criterio del encuestado, además la evaluación se realiza teniendo en cuenta un periodo específico correspondiente al mes de rotación en el que se realizan los turnos, dejando por fuera el periodo vacacional en que también se encontrarían hallazgos de SDE, de acuerdo a algunos estudios en los que se reporta disminución leve en período vacacional, pero en rangos altos con respecto a la población general, lo cual indica que los estudiantes persisten somnolientos en vacaciones.
Pese a que los hallazgos fueron poco significativos y corresponde a una muestra pequeña, se puede realizar una comparación con estudios realizados con muestras similares e incluso correspondientes a estudiantes de la misma facultad y Universidad Nacional de Colombia, son también consistentes con la literatura mundial, demostrando el evidente impacto que tiene en los estudiantes de medicina la realización de turnos de más de 12 horas y la SDE patológica en esta población en particular (6,14).
Algunos estudios han concluído que no hay diferencia con respecto a la somnolencia y calidad del sueño entre los estudiantes que no cursan internado y los que lo cursan (17), se debe tener en cuenta el rigor académico y el plan de estudios diferente en todas las escuelas de medicina por ende es evidente que se requieran más estudios que determinen la influencia de los turnos en la vida de las personas. Los accidentes laborales se incrementan si la calidad del sueño se encuentra alterada y más aún si existe SDE, por ello en Estados Unidos y en algunos países europeos, debido al elevado número de errores médicos cometidos por estudiantes de pregrado, postgrado y los médicos internos en los turnos hospitalarios, se ha reglamentado un máximo de horas por jornada laboral y de turnos semanales para los estudiantes de medicina de pregrado y especialidades médico quirúrgicas (28,33-38).
Como se trata de una población de jóvenes aparentemente sanos con una alta exigencia académica y una mala higiene del sueño, se puede explicar que entre las causas probables de SDE se halla el síndrome de insuficiencia crónica de sueño que tanto afecta a la sociedad contemporánea (8,39), sumado a la influencia de los turnos, que deterioran los ritmos circadianos de los alumnos (13), disminuyendo las horas de descanso y promueven una deuda crónica de sueño, que conlleva a SDE, la cual desencadena una pobre capacidad de concentración y memorización, afectando el desempeño e incrementando el riesgo de accidentes laborales y errores médicos, tal como se ha demostrado en estudios previos (38).
Aún no son claras las causas de la SDE en este grupo, por ello es pertinente seguir realizando investigaciones que logren dilucidar los factores que juegan un rol importante en el desarrollo de esta condición patológica, que permitirían llevar una mejor calidad de vida para los estudiantes y evitar los riesgos a los que se exponen tanto los pacientes como los médicos en ejercicio que padecen de SDE.
En general, se debe promover los buenos hábitos de higiene del sueño en los profesionales de la salud y población general, especialmente en los correturnos, ya que se trata de una población especial que se halla en continuo riesgo. Con base en los datos obtenidos se propone que los estudiantes de medicina de la UNCB, tengan presentes adecuados hábitos de higiene del sueño, y en lo posible, como máximo realicen un turno nocturno semanal de 12 horas con su correspondiente período de descanso posturno, esto redundará en un mejor aprendizaje y rendimiento académico.
Es importante diagnosticar y tratar a quienes padecen esta condición patológica que deteriora la funcionalidad, calidad de vida e impacta no solo al estudiante de medicina sino a su entorno, para evitar que se ponga en riesgo su vida y la de otras personas (19,21).
Es pertinente continuar con la realización de investigaciones somnológicas, para ampliar los conocimientos no solo en el tratamiento de los pacientes sino en los efectos de la privación del sueño en distintos grupos poblacionales de cualquier característica, para mejorar la calidad de vida de las personas.
Referencias
1. Chica-Urzola H, Escobar-Córdoba F, Echeverry-Chabur J. Evaluación clínica del hipersomnio. Rev Colomb Psiquiatr. 2004; 33:45-63.
2. ASDA: International Classification of Sleep Disorders, Revised, Diagnostic and Coding Manual. Rochester: American Sleep Disorders Association; 1997.
3. Richardson GS, Carskadon MA, Flagg W, Van den Hoed J, Dement WC, Mitler MM. Excessive daytime sleepiness in man: multiple sleep latency measurement in narcoleptic and control subjects. Electroence-phalogr Clin Neurophysiol. 1978; 45:621-627.
4. Escobar-Córdoba F, Eslava-Schmalbach J, Folino JO. Síntomas de estrés postraumático y trastornos del sueño en un grupo de mujeres adultas de Bogotá. Univ Med. 2008; 49: 29-45.
5. Radun I, Summala H. Sleep-related fatal vehicle accidents: characteristics of decisions made by multidisciplinary investigation teams. Sleep. 2004; 27:224-227.
6. Escobar-Córdoba F, Cortes-Rueda MF, Canal-Ortiz JS et al. Somnolencia diurna excesiva en estudiantes de tercer semestre de medicina de la Universidad Nacional de Colombia. Rev Fac Med Univ Nac Colomb. 2008, 56:235-244.
7. Roth T, Franklin M, Bramley TJ. The state of insomnia and emerging trends. Am J Manag Care. 2007; 13(5 Suppl):S117-120.
8. Valencia M, Salín-Pascual R, Pérez R. Trastornos del dormir, 1 edn. México: McGraw-Hill Interamericana; 2000.
9. Escobar-Córdoba F, Echeverry-Chabur J. Implicaciones ocupacionales del insomnio. En: Avances. Bogotá-Colombia. Ed: Javegraf. 2006; 7:60-76.
10. Souza MF, Silva G de R. [Risk of minor psychiatric disorders in a metropolitan area of southeast Brazil]. Rev Saude Publica. 1998;32:50-8.
11. Veldi M, Aluoja A, Vasar V. Sleep quality and more common sleep-related problems in medical students. Sleep Med. 2005;6:269-75.
12. Rosales-Mayor E, Egoavil- Rojas MT, La Cruz-Dávila C, Rey de Castro-Mujica J. [Sleepiness and sleep quality in medical students of a Peruvian university]. Somnolencia y calidad del sueño en estudiantes de medicina de una universidad peruana. An Fac Med (Perú). 2007;68:150-158.
13. Danda J, Ferreira G, Azenha M, Souza K, Bastos O. [Sleep-wake cycle pattern and excessive daytime sleepiness in medical students]. Padrão do ciclo sonovigília e sonolência excessiva diurna em estudantes de medicina. J Bras Psiquiatr. 2005;54:102-106.
14. Zailinawati AH, Teng CL, Chung YC, Teow TL, Lee PN, Jagmohni KS. Daytime sleepiness and sleep quality among Malaysian medical students. Med J Malaysia. 2009; 64:108-110.
15. Rodrigues RND, Viegas CAA, Abreu E, Silva A, Tavares P. Daytime sleepiness and academic performance in medical students. Arq Neuropsiquiatr. 2002; 60:6-11.
16. Pedroso A, Cheroto A, Aloe F, Tavares SM. [Epworth sleepiness scale outcome in 480 Brazilian medical students]. Resultados da escala de sonolencia Epworth em 480 alunos de graduacao da Faculdade de Medicina da Universidade de Sao Paulo. Rev med (Säo Paulo). 1996;75:100-7.
17. Braz S, Neumann BRG, Tufik S. [Evaluation of sleep problems in medical students]. Avaliaçäo dos problemas de sono em alunos do curso de medicina. Pesqui méd (Porto Alegre). 1987;21:95-100.
18. Hidalgo MPL, De Souza CM, Zanette CB, Nunes PV. Association of daytime sleepiness and the morningness/eveningness dimension in young adult subjects in Brazil. Psychological Reports. 2003; 93:427-434.
19. Kamdar BB, Kaplan KA, Kezirian EJ. Dement WC. The impact of extended sleep on daytime alertness, vigilance, and mood. Sleep Medicine. 2004;5: 441-448.
20. Hidalgo MP, Caumo W. Sleep disturbances associated with minor psychiatric disorders in medical students. Neurol Sci. 2002;23:35-39.
21. Loayza P, Ponte S, Carvalho CG, Pedrotti M, Nunes P, Souza C, Zanette C, Voltolini S, Chaves MF. Association between mental health screening by self-report questionnaire and insomnia in medical students. Arq Neuropsiquiatr. 2001;59:180-185.
22. Kageyama T, Kabuto M, Nitta H, Kurokawa Y, Taira K, Suzuki S, Takemoto TI. Prevalence of use of medically prescribed hypnotics among adult Japanese women in urban residential areas. Psychiatry Clin Neurosci. 1998;52:69-74.
23. Seppälä M, Hyyppä MT, Impivaara O, Knuts LR, Sourander L. Subjective quality of sleep and use of hypnotics in an elderly urban population. Aging (Milano). 1997;9:327-34.
24. Chica-Urzola HL, Escobar-Cordoba F, Eslava-Schmalbach J. Validating the Epworth sleepiness scale. Revista de salud pública. Colombia. 2007; 9:558-567.
25. Escobar-Cordoba F, Eslava-Schmalbach J. Colombian validation of the Pittsburgh Sleep Quality Index. Rev Neurol. 2005;40:150-5.
26. Mastin D, Bryson J, Corwyn R. Assessment of sleep hygiene using the sleep hygiene index. J Behavioral Med. 2006; 29:223-227.
27. Varela L. Validación del índice de higiene del sueño para adultos mayores. Instituto de Gerontología. Memorias: XII Congreso de la Federación Latinoamericana de Sociedades de Sueño / FLASS.I Congreso de la Asociación Peruana de Medicina del Sueño /APEMES. 10-12 octubre 2008. Lima, Perú.
28. West CP, Tan AD, Habermann TM, Sloan JA, Shanafelt TD. Association of resident fatigue and distress with perceived medical errors. JAMA. 2009;302:1294-300.
29. Handel DA, Raja A, Lindsell CJ. The use of sleep aids among Emergency Medicine residents: a web based survey. BMC health services research. 2006; 6:136.
30. Sierra JC, Delgado-Domínguez C, Carretero-Dios H. Propiedades psicométricas de la Dysfunctional Beliefs and Attitudes about Sleep Scale (DBAS) en una muestra española de sujetos normales. Rev Latinoam Psicol. 2005; 37:523-39.
31. Wada K, Sakata Y, Theriault G, Narai R, Yoshino Y, Tanaka K, Aizawa Y. Associations of excessive sleepiness on duty with sleeping hours and number of days of overnight work among medical residents in Japan. J Occup Health. 2007; 49:523-27.
32. Joo S, Shin C, Kim J, Yi H, Ahn Y, Park M et al. Prevalence and correlates of excessive daytime sleepiness in high school students in Korea. Psychiatry Clin Neurosci. 2005; 59:433-40.
33. Ohaeri JU, Odejide AO, Ikuesan BA, Adeyemi JD. The pattern of isolated sleep paralysis among Nigerian medical students. JAMA. 1989; 81:805-808.
34. Lockley SW, Cronin JW, Evans EE, Cade BE, Lee CJ, Landrigan CP, Rothschild JM, et al. Effect of reducing interns' weekly work hours on sleep and attentional failures. NEJM. 2004, 351:1829-37.
35. Arnedt JT, Owens J, Crouch M, Stahl J, Carskadon MA. Neurobehavioral performance of residents after heavy night cali vs after alcohol ingestión. JAMA. 2005; 294:1025-33.
36. Baldwin DC Jr, Daugherty SR. Sleep deprivation and fatigue in residency training: results of a national survey of first- and second-year residents. Sleep. 2004; 27:217-23.
37. Howard SK, Gaba DM, Rosekind MR, Zarcone VP. The risks and implications of excessive daytime sleepiness in resident physicians. Acad Med. 2002;77:1019-1025.
38. Fletcher KE, Underwood W3rd, Davis SQ, Mangrulkar RS, McMahon LFJr, Saint S. Effects of work hour reduction on residents' lives: a systematic review. JAMA. 2005; 294:1088-1100.
39. Morin CM, Culbert JP, Schwartz SM. Nonpharmacological interventions for insomnia: a meta-analysis of treatment efficacy. Am J Psychiatry. 1994; 151:1172-80.
Referencias
Chica-Urzola H, Escobar-Córdoba F, Echeverry-Chabur J. Evaluación clínica del hipersomnio. Rev Colomb Psiquiatr. 2004; 33:45-63.
ASDA: International Classification of Sleep Disorders, Revised, Diagnostic and Coding Manual. Rochester: American Sleep Disorders Association; 1997.
Richardson GS, Carskadon MA, Flagg W, Van den Hoed J, Dement WC, Mitler MM. Excessive daytime sleepiness in man: multiple sleep latency measurement in narcoleptic and control subjects. Electroence-phalogr Clin Neurophysiol. 1978; 45:621-627.
Escobar-Córdoba F, Eslava-Schmalbach J, Folino JO. Síntomas de estrés postraumático y trastornos del sueño en un grupo de mujeres adultas de Bogotá. Univ Med. 2008; 49: 29-45.
Radun I, Summala H. Sleep-related fatal vehicle accidents: characteristics of decisions made by multidisciplinary investigation teams. Sleep. 2004; 27:224-227.
Escobar-Córdoba F, Cortes-Rueda MF, Canal-Ortiz JS et al. Somnolencia diurna excesiva en estudiantes de tercer semestre de medicina de la Universidad Nacional de Colombia. Rev Fac Med Univ Nac Colomb. 2008, 56:235-244.
Roth T, Franklin M, Bramley TJ. The state of insomnia and emerging trends. Am J Manag Care. 2007; 13(5 Suppl):S117-120.
Valencia M, Salín-Pascual R, Pérez R. Trastornos del dormir, 1 edn. México: McGraw-Hill Interamericana; 2000.
Escobar-Córdoba F, Echeverry-Chabur J. Implicaciones ocupacionales del insomnio. En: Avances. Bogotá-Colombia. Ed: Javegraf. 2006; 7:60-76.
Souza MF, Silva G de R. [Risk of minor psychiatric disorders in a metropolitan area of southeast Brazil]. Rev Saude Publica. 1998;32:50-8.
Veldi M, Aluoja A, Vasar V. Sleep quality and more common sleep-related problems in medical students. Sleep Med. 2005;6:269-75.
Rosales-Mayor E, Egoavil- Rojas MT, La Cruz-Dávila C, Rey de Castro-Mujica J. [Sleepiness and sleep quality in medical students of a Peruvian university]. Somnolencia y calidad del sueño en estudiantes de medicina de una universidad peruana. An Fac Med (Perú). 2007;68:150-158.
Danda J, Ferreira G, Azenha M, Souza K, Bastos O. [Sleep-wake cycle pattern and excessive daytime sleepiness in medical students]. Padrão do ciclo sonovigília e sonolência excessiva diurna em estudantes de medicina. J Bras Psiquiatr. 2005;54:102-106.
Zailinawati AH, Teng CL, Chung YC, Teow TL, Lee PN, Jagmohni KS. Daytime sleepiness and sleep quality among Malaysian medical students. Med J Malaysia. 2009; 64:108-110.
Rodrigues RND, Viegas CAA, Abreu E, Silva A, Tavares P. Daytime sleepiness and academic performance in medical students. Arq Neuropsiquiatr. 2002; 60:6-11.
Pedroso A, Cheroto A, Aloe F, Tavares SM. [Epworth sleepiness scale outcome in 480 Brazilian medical students]. Resultados da escala de sonolencia Epworth em 480 alunos de graduacao da Faculdade de Medicina da Universidade de Sao Paulo. Rev med (Säo Paulo). 1996;75:100-7.
Braz S, Neumann BRG, Tufik S. [Evaluation of sleep problems in medical students]. Avaliaçäo dos problemas de sono em alunos do curso de medicina. Pesqui méd (Porto Alegre). 1987;21:95-100.
Hidalgo MPL, De Souza CM, Zanette CB, Nunes PV. Association of daytime sleepiness and the morningness/eveningness dimension in young adult subjects in Brazil. Psychological Reports. 2003; 93:427-434.
Kamdar BB, Kaplan KA, Kezirian EJ. Dement WC. The impact of extended sleep on daytime alertness, vigilance, and mood. Sleep Medicine. 2004;5: 441-448.
Hidalgo MP, Caumo W. Sleep disturbances associated with minor psychiatric disorders in medical students. Neurol Sci. 2002;23:35-39.
Loayza P, Ponte S, Carvalho CG, Pedrotti M, Nunes P, Souza C, Zanette C, Voltolini S, Chaves MF. Association between mental health screening by self-report questionnaire and insomnia in medical students. Arq Neuropsiquiatr. 2001;59:180-185.
Kageyama T, Kabuto M, Nitta H, Kurokawa Y, Taira K, Suzuki S, Takemoto TI. Prevalence of use of medically prescribed hypnotics among adult Japanese women in urban residential areas. Psychiatry Clin Neurosci. 1998;52:69-74.
Seppälä M, Hyyppä MT, Impivaara O, Knuts LR, Sourander L. Subjective quality of sleep and use of hypnotics in an elderly urban population. Aging (Milano). 1997;9:327-34.
Chica-Urzola HL, Escobar-Cordoba F, Eslava-Schmalbach J. Validating the Epworth sleepiness scale. Revista de salud pública. Colombia. 2007; 9:558-567.
Escobar-Cordoba F, Eslava-Schmalbach J. Colombian validation of the Pittsburgh Sleep Quality Index. Rev Neurol. 2005;40:150-5.
Mastin D, Bryson J, Corwyn R. Assessment of sleep hygiene using the sleep hygiene index. J Behavioral Med. 2006; 29:223-227.
Varela L. Validación del índice de higiene del sueño para adultos mayores. Instituto de Gerontología. Memorias: XII Congreso de la Federación Latinoamericana de Sociedades de Sueño / FLASS.I Congreso de la Asociación Peruana de Medicina del Sueño /APEMES. 10-12 octubre 2008. Lima, Perú.
West CP, Tan AD, Habermann TM, Sloan JA, Shanafelt TD. Association of resident fatigue and distress with perceived medical errors. JAMA. 2009;302:1294-300.
Handel DA, Raja A, Lindsell CJ. The use of sleep aids among Emergency Medicine residents: a web based survey. BMC health services research. 2006; 6:136.
Sierra JC, Delgado-Domínguez C, Carretero-Dios H. Propiedades psicométricas de la Dysfunctional Beliefs and Attitudes about Sleep Scale (DBAS) en una muestra española de sujetos normales. Rev Latinoam Psicol. 2005; 37:523-39.
Wada K, Sakata Y, Theriault G, Narai R, Yoshino Y, Tanaka K, Aizawa Y. Associations of excessive sleepiness on duty with sleeping hours and number of days of overnight work among medical residents in Japan. J Occup Health. 2007; 49:523-27.
Joo S, Shin C, Kim J, Yi H, Ahn Y, Park M et al. Prevalence and correlates of excessive daytime sleepiness in high school students in Korea. Psychiatry Clin Neurosci. 2005; 59:433-40.
Ohaeri JU, Odejide AO, Ikuesan BA, Adeyemi JD. The pattern of isolated sleep paralysis among Nigerian medical students. JAMA. 1989; 81:805-808.
Lockley SW, Cronin JW, Evans EE, Cade BE, Lee CJ, Landrigan CP, Rothschild JM, et al. Effect of reducing interns' weekly work hours on sleep and attentional failures. NEJM. 2004, 351:1829-37.
Arnedt JT, Owens J, Crouch M, Stahl J, Carskadon MA. Neurobehavioral performance of residents after heavy night cali vs after alcohol ingestión. JAMA. 2005; 294:1025-33.
Baldwin DC Jr, Daugherty SR. Sleep deprivation and fatigue in residency training: results of a national survey of first- and second-year residents. Sleep. 2004; 27:217-23.
Howard SK, Gaba DM, Rosekind MR, Zarcone VP. The risks and implications of excessive daytime sleepiness in resident physicians. Acad Med. 2002;77:1019-1025.
Fletcher KE, Underwood W3rd, Davis SQ, Mangrulkar RS, McMahon LFJr, Saint S. Effects of work hour reduction on residents' lives: a systematic review. JAMA. 2005; 294:1088-1100.
Morin CM, Culbert JP, Schwartz SM. Nonpharmacological interventions for insomnia: a meta-analysis of treatment efficacy. Am J Psychiatry. 1994; 151:1172-80.
Cómo citar
APA
ACM
ACS
ABNT
Chicago
Harvard
IEEE
MLA
Turabian
Vancouver
Descargar cita
Visitas a la página del resumen del artículo
Descargas
Licencia
Derechos de autor 2011 Revista de la Facultad de Medicina

Esta obra está bajo una licencia Creative Commons Reconocimiento 3.0 Unported.
-