Adaptación transcultural al español de la escala Health-Related Quality of Life In Stroke Patients HRQOLISP-40
Spanish Cross-cultural adaptation of the scale Health-Related Quality of Life in Stroke Patients (HRQOLISP-40)
DOI:
https://doi.org/10.15446/revfacmed.v63n4.45503Palabras clave:
Calidad de vida, cuestionarios, Trastornos cerebrovasculares, Comparación transcultural (es)Quality of life, Questionnaires, Cerebrovascular Disorders, Cross-Cultural Comparison (en)
Antecedentes. La medición de calidad de vida en pacientes con accidente cerebrovascular es importante, ya que puede orientar el manejo de los procesos de rehabilitación. En Colombia no existen instrumentos de medición de calidad de vida validados para pacientes con este tipo de afección.
Objetivo. Realizar la adaptación transcultural de la escala Health-Related Quality of Life In Stroke Patients HRQOLISP-40 para su uso en Colombia.
Materiales y métodos. Se siguieron las recomendaciones metodológicas del grupo de calidad de vida EORTC: traducción inicial, traducción inversa y estudio piloto.
Resultados. Las traducciones directas fueron similares en 24/40 ítems; en 12 ítems hubo variaciones en redacción sin cambio de palabras; en las instrucciones, una opción de respuesta y en 4 ítems se requirió escoger la mejor opción de traducción de una palabra. Las traducciones inversas fueron similares entre sí y a la versión original de la escala. Por otra parte, en la prueba piloto se observó cierta dificultad de comprensión en 3 ítems, se adoptaron las sugerencias del autor respecto a las inquietudes de los pacientes, no hubo dificultades por molestia ni se sugirió un nuevo parafraseo.
Conclusión. Al terminar esta fase se cuenta con la versión en español (de Colombia) de la escala HRQOLISP-40 para ser sometida a una validación previa a su uso en la evaluación de calidad de vida en pacientes con accidente cerebrovascular.
Background. The measurement of quality of life in patients with stroke is important because it can guide the management of rehabilitation processes. In Colombia there are no instruments for measuring quality of life in stroke patients. The objective was to perform the cross-cultural adaptation of Health-Related Quality of Life In Stroke Patients HRQLISP-40 scale for use in Colombia.
Objective. To make a transcultural adaptation to the Health-Related Quality of Life In Stroke Patients HRQOLISP-40 scale in order to use it in Colombia.
Materials and Methods. The methodological recommendations by EORTC quality of life group were taken: initial translation, back translation and pilot study.
Results. Direct translations were similar in 24/40 items; in 12 items there were variations in writing without changing the words; in the instructions, an option of choices and 4 items were required to choose the best translation of a word. The reverse translations were similar to each other and with the original version of the scale; in the pilot test there were difficulty in comprehension understanding 3 items and were adopted the author's suggestions concerns the patients, there was no trouble or non-comfortableness nor any paraphrase were suggested.
Conclusion. To finish this phase it is the Colombian Spanish version of HRQLISP-40 scale to be submitted for validation prior to use in assessing quality of life in stroke patients.
DOI: https://doi.org/10.15446/revfacmed.v63n4.45503
INVESTIGACIÓN ORIGINAL
Adaptación transcultural al español de la escala Health-Related Quality of Life In Stroke Patients HRQOLISP-40
Spanish Cross-cultural adaptation of the scale Health-Related Quality of Life in Stroke Patients (HRQOLISP-40)
Yahira Rossini Guzmán-Sabogal1, Jorge Pla Vidal2, Ricardo Sánchez-Pedraza3, Felipe Ortuño Sánchez-Pedreño2, Catalina Gómez-Guevara4
1 Universidad de La Sabana - Chía - Colombia.
2 Universidad de Navarra - Pamplona - España.
3 Universidad Nacional de Colombia - Bogotá D.C. - Colombia.
4 Clínica Universidad de La Sabana - Chía - Colombia.
Correspondencia: Yahira Rossini Guzmán-Sabogal. Universidad de La Sabana. Autopista Norte Km 7. Teléfono: +57 1 8615555, extensión: 23015-23004. Chía. Colombia. Correo electrónico: yahira.guzman@unisabana.edu.co
Recibido: 09/09/2014 Aceptado: 26/02/2015
Resumen
Antecedentes. La medición de calidad de vida en pacientes con accidente cerebrovascular es importante, ya que puede orientar el manejo de los procesos de rehabilitación. En Colombia no existen instrumentos de medición de calidad de vida validados para pacientes con este tipo de afección.
Objetivo. Realizar la adaptación transcultural de la escala Health-Related Quality of Life In Stroke Patients HRQOLISP-40 para su uso en Colombia.
Materiales y métodos. Se siguieron las recomendaciones metodológicas del grupo de calidad de vida EORTC: traducción inicial, traducción inversa y estudio piloto.
Resultados. Las traducciones directas fueron similares en 24/40 ítems; en 12 ítems hubo variaciones en redacción sin cambio de palabras; en las instrucciones, una opción de respuesta y en 4 ítems se requirió escoger la mejor opción de traducción de una palabra. Las traducciones inversas fueron similares entre sí y a la versión original de la escala. Por otra parte, en la prueba piloto se observó cierta dificultad de comprensión en 3 ítems, se adoptaron las sugerencias del autor respecto a las inquietudes de los pacientes, no hubo dificultades por molestia ni se sugirió un nuevo parafraseo.
Conclusión. Al terminar esta fase se cuenta con la versión en español (de Colombia) de la escala HRQOLISP-40 para ser sometida a una validación previa a su uso en la evaluación de calidad de vida en pacientes con accidente cerebrovascular.
Palabras clave: Calidad de vida; cuestionarios; Trastornos cerebrovasculares; Comparación transcultural (DeCS).
Guzmán-Sabogal YR, Pla Vidal J, Sánchez-Pedraza R, Ortuño Sánchez-Pedreño F, Gómez-Guevara C. Adaptación transcultural al español de la escala Health-Related Quality of Life In Stroke Patients HRQOLISP-40. Rev. Fac. Med. 2015;63(4):583-93. doi: https://doi.org/10.15446/revfacmed.v63n4.45503.
Summary
Background. The measurement of quality of life in patients with stroke is important because it can guide the management of rehabilitation processes. In Colombia there are no instruments for measuring quality of life in stroke patients. The objective was to perform the cross-cultural adaptation of Health-Related Quality of Life In Stroke Patients HRQLISP-40 scale for use in Colombia.
Objective. To make a transcultural adaptation to the Health-Related Quality of Life In Stroke Patients HRQOLISP-40 scale in order to use it in Colombia.
Materials and Methods. The methodological recommendations by EORTC quality of life group were taken: initial translation, back translation and pilot study.
Results. Direct translations were similar in 24/40 items; in 12 items there were variations in writing without changing the words; in the instructions, an option of choices and 4 items were required to choose the best translation of a word. The reverse translations were similar to each other and with the original version of the scale; in the pilot test there were difficulty in comprehension understanding 3 items and were adopted the author's suggestions concerns the patients, there was no trouble or non-comfortableness nor any paraphrase were suggested.
Conclusion. To finish this phase it is the Colombian Spanish version of HRQLISP-40 scale to be submitted for validation prior to use in assessing quality of life in stroke patients.
Keywords: Quality of life; Questionnaires; Cerebrovascular Disorders; Cross-Cultural Comparison (MeSH).
Guzmán-Sabogal YR, Pla Vidal J, Sánchez-Pedraza R, Ortuño Sánchez-Pedreño F, Gómez-Guevara C. [Spanish Cross-cultural adaptation of the scale Health-Related Quality of Life in Stroke Patients (HRQOLISP-40)]. Rev. Fac. Med. 2015;63(4):583-93. Spanish. doi: https://doi.org/10.15446/revfacmed.v63n4.45503.
Introducción
Los accidentes cerebrovasculares (ACV) constituyen la tercera causa de muerte y la más importante de discapacidad en el adulto (1,2). Según la Organización Mundial de la Salud, la calidad de vida se ha definido como "la percepción que las personas tienen de su lugar en la vida, en el contexto y en el sistema de valores en los cuales viven y en relación con sus objetivos, esperanzas e intereses" (3). Se consideran entonces cuatro dimensiones en la calidad de vida relacionada con la salud: física, funcional, psicológica y social (4).
De igual forma, se debe tener en cuenta que después de un ACV suele ocurrir un compromiso muy global; por lo tanto los dominios a evaluar deben incluir la mayoría de factores que puedan afectar a esta población (5). En un estudio publicado en 2011 por Howitt et al. (6), se evidenció que factores como edad, depresión, ansiedad, discapacidad, función motora, y desempeño social están frecuentemente alterados en pacientes con ACV, todas ellas pueden verse modificadas excepto la edad.
La posibilidad de cercanía a la muerte hace que tanto los pacientes que sobreviven a un ACV como sus familias revisen sus vidas buscándole un sentido, incluso, los pacientes expresan su necesidad de estar en paz y pueden llegar a manifestar inquietudes espirituales durante la evaluación (7). Espiritualidad no significa lo mismo para todos los pacientes y es importante reconocer las diferencias culturales y las tradiciones religiosas para poder abordar el tema adecuadamente con cada paciente, siendo respetuosos con las creencias de cada uno y sin perder de vista que los pacientes responden de forma positiva cuando se le presta atención a este aspecto de su vida (8).
Se ha visto que aquellos pacientes con algún tipo de orientación espiritual resisten más las adversidades de la vida, incluyendo condiciones médicas como un ACV; de hecho, más del 40% de los pacientes de edad avanzada y crónicamente enfermos refieren en forma espontánea que la fe religiosa fue el factor más importante que contribuyó a su recuperación (9). Koenig HG et al. (10) citan a Emil Durkheim, quien planteó la posibilidad de consecuencias negativas para la salud cuando las personas no tenían vínculos religiosos. Sin embargo, la mayoría de los estudios posteriores se centraron en las prácticas particulares de cada grupo religioso. Hoy en día varios investigadores han comenzado a estudiar seriamente el vínculo entre asistencia espiritual y salud, intentando superar las limitaciones metodológicas que este tipo de estudios supone; ya que el objetivo primario de un proceso de rehabilitación es mejorar la calidad de vida (10-13).
Actualmente, se considera que los instrumentos que se deben emplear para hacer mediciones en salud deberían ser elegidos dependiendo de la pregunta de interés y teniendo en cuenta las propiedades clinimétricas del instrumento, en este caso de calidad de vida (14). Se debe tener en cuenta que en pacientes que han sufrido un ACV suele ocurrir un compromiso muy global, por lo tanto los dominios a evaluar deben incluir la mayoría de factores que puedan afectar a esta población (5). Existen varios instrumentos tradicionalmente utilizados en pacientes con ACV (14,16); entre ellos la escala ACVI-38, desarrollada y validada posteriormente durante el 2008 en Cuba para habla hispana (17).
El instrumento objeto del presente estudio es la HRQLISP-40, desarrollada en Nigeria por Ojo Owolabi, la cual incluye dentro de sus dominios preguntas específicas relacionadas con el componente espiritual, debido a que, en estudios previos, se encontró que para estos pacientes los dominios relacionados con la esfera espiritual fueron más importantes que los otros dominios (5,18,19). El mismo investigador corroboró sus hallazgos en un estudio publicado en 2013 (20), en el cual propone que intervenciones terapéuticas en este sentido pueden reducir el impacto biográfico que esta condición causa en los pacientes. Una de las razones por la cual es importante tener validado este instrumento en español es que este puede llegar a ser una herramienta de uso rutinario en pacientes víctimas de ACV, lo que permite a los clínicos comparar y hacer seguimiento en pacientes de habla hispana (5,20-22).
Llegado a este punto, hay que tener en cuenta que esta escala fue desarrollada en un idioma y en un contexto diferente al colombiano y no se cuenta con una versión en español. Entonces, se requiere de un proceso de adaptación transcultural para su uso en nuestro país, lo cual implica la traducción para garantizar la equivalencia tanto lingüística como conceptual entre la versión traducida y la original. Para esto se utilizaron como base las sugerencias propuestas por la European Organization for research and Treatment of Cancer (EORTC) —cuyo trabajo se desarrolla principalmente en cáncer— de plantear una guía de validación de escalas muy clara (23), así mismo se utilizó como apoyo la publicación en Colombia de una propuesta para este mismo proceso (24). Este estudio de adaptación transcultural hace parte de la validación de la escala para su posterior uso en Colombia en pacientes sobrevivientes de ACV.
Materiales y métodos
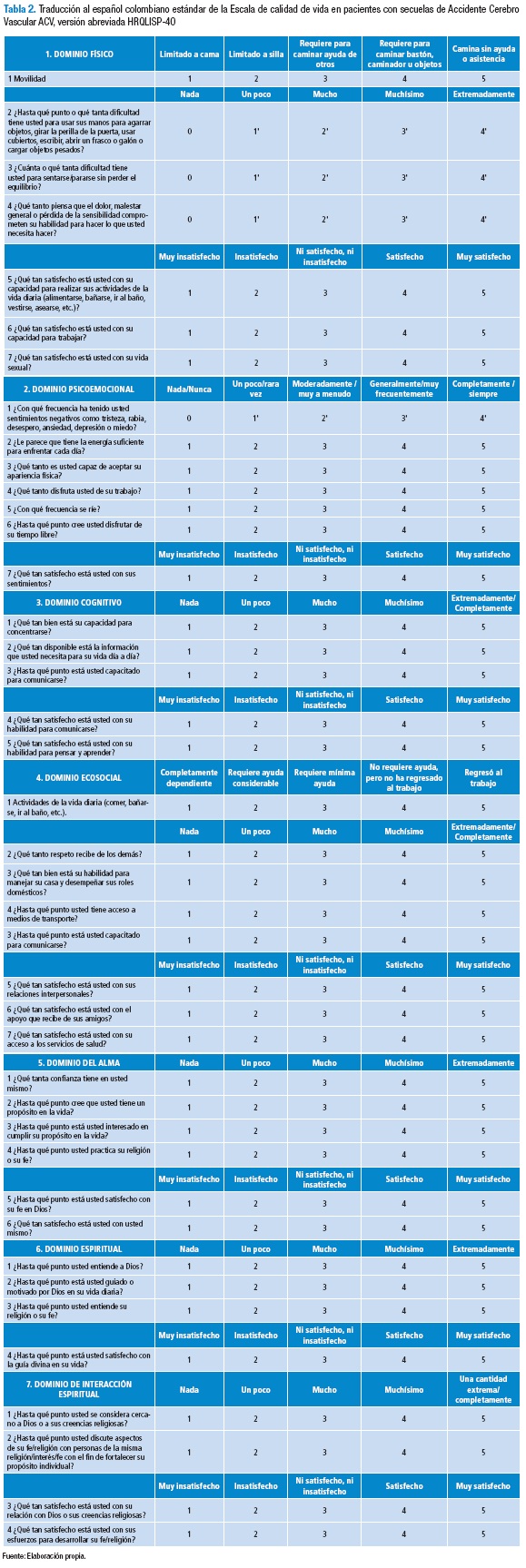
La escala para calidad de vida en pacientes con secuelas de accidente cerebrovascular (versión abreviada HRQLISP-40) consta de una sección de instrucciones y 40 ítems redactados en escala tipo Likert. En las instrucciones se explica que el instrumento está diseñado para evaluar las últimas dos semanas y pregunta por el estado de salud y calidad de vida, teniendo en cuenta los valores, esperanzas, gustos y preocupaciones del paciente.
El instrumento tiene los siguientes dominios: físico, psicoemocional, cognitivo, ecosocial, del alma, espiritual, y finalmente dominio de interacción espiritual. La escala tipo Likert consta de 5 opciones de respuesta para todos los ítems. En el ítem 1 las opciones son: "limitado a cama, limitado a silla, requiere para caminar ayuda de otros, requiere para caminar bastón, caminador u objetos, camina sin ayuda o asistencia". Para los ítems 2 a 4 del dominio físico, 1 a 3 del dominio cognitivo, 2 a 4 del dominio ecosocial, 1 a 4 del dominio del alma, 1 a 3 del dominio espiritual, y 1 y 2 del dominio interacción espiritual: "nada, un poco, mucho, muchísimo, extremadamente/completamente". Para los ítems 5 a 7 del dominio físico, 7 del dominio psicoemocional, 4 y 5 del dominio cognitivo, 5 a 7 del dominio ecosocial, 5 y 6 del dominio del alma, 4 del dominio espiritual, y 3 y 4 del dominio interacción espiritual: "muy insatisfecho, insatisfecho, ni satisfecho, ni insatisfecho, satisfecho, muy satisfecho". Para los ítems 1 a 6 del dominio psicoemocional: "nada/nunca, un poco/rara vez, moderadamente/muy a menudo, generalmente/muy frecuentemente, completamente/siempre". Para el ítem 1 del dominio ecosocial: "completamente dependiente, requiere ayuda considerable, requiere mínima ayuda, no requiere ayuda pero no ha regresado al trabajo, regresó al trabajo". Para la calificación los ítems 2, 3 y 4 del dominio físico y el ítem 1 del dominio psicoemocional, estos se puntúan como negativos; es decir, se registra -1; la puntuación de los dominios: sumatoria de los puntajes por ítem, son generados de tal manera que el máximo puntaje es transformado a 100 (19).
Procedimiento
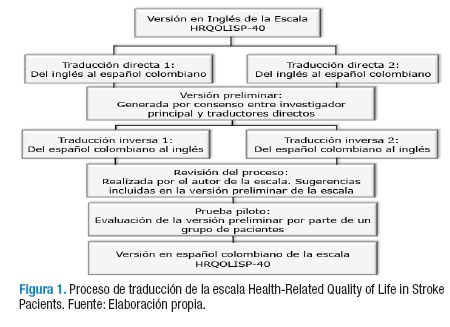
La autora del estudio contactó al autor de la escala Mayowa Ojo Owolabi en mayo de 2012, quien autorizó el uso de la misma. Una vez obtenida la escala, se siguieron las sugerencias de la EORTC para realizar el proceso de adaptación transcultural. Se llevaron a cabo las siguientes etapas:
Traducción directa
Dos colombianos con buen nivel de inglés —médicos, cursando estudios de especialización médico-quirúrgica en Estados Unidos—, de manera independiente, realizaron traducciones directas del inglés al español estándar colombiano de las instrucciones, de cada uno de los ítems y de las opciones de respuesta de la escala.
Versión preliminar
En reuniones de consenso, los dos traductores, un experto en validación de escalas y la coordinadora del estudio realizaron una comparación de las dos traducciones directas para discutir y resolver discrepancias entre las traducciones y generar una versión preliminar de la escala. La discusión tuvo en cuenta los siguientes criterios: si las traducciones fueron idénticas no se realizaron cambios; si existió alguna diferencia se eligió la traducción cuyo significado fue más cercano al original pero ajustándose al contexto cultural colombiano.
Traducción inversa
Dos traductores oficiales del inglés estadounidense con buena fluencia del español colombiano estándar realizaron, de manera independiente, las traducciones inversas del español colombiano al inglés a partir de la versión preliminar.
Revisión del autor
El autor de la escala Mayowa Ojo Owolabi revisó traducciones directas, versión preliminar y traducciones inversas y llevó a cabo comparaciones de las traducciones inversas con la versión original en inglés. Los ajustes propuestos fueron incluidos en la versión preliminar una vez revisados y considerados por los autores y el experto en validación de escalas.
Prueba piloto
La escala fue presentada a un grupo de 20 pacientes colombianos, mayores de 18 años, con diagnóstico de accidente cerebrovascular de cualquier etiología, quienes se encontraban en consultas de rehabilitación o en proceso integral de rehabilitación en la Clínica Universidad de La Sabana. Los pacientes leyeron la escala y rellenaron un cuestionario en el cual debían evaluar si las instrucciones y cada uno de los ítems fueron incomprensibles, confusos, ofensivos o molestos, si tenían palabras difíciles o si podían redactarse de una mejor forma. Una vez finalizado este proceso se obtuvo la versión en español colombiano de la escala HRQLISP-40.
Este estudio de adaptación transcultural de la escala HRQLISP-40 fue realizado como parte del proyecto de validación de la misma escala para su uso en Colombia, aprobado por la subcomisión de investigación y ética de la Universidad de La Sabana, previa revisión y aceptación como tesis en el doctorado de Investigación Médica Aplicada de la Universidad de Navarra, actualmente en curso.
Resultados
Proceso de traducción
Las traducciones directas fueron realizadas entre enero 23 y marzo 5 de 2013; la versión preliminar, obtenida a partir del consenso entre los autores de estas traducciones, se realizó en marzo 19 y las traducciones inversas se llevaron a cabo entre marzo 25 y abril 10 de este mismo año.
Instrucciones de la escala
Las dos traducciones fueron muy similares, sin embargo en la traducción de Please keep in mind your standards, hopes, pleasures and concerns, uno de los traductores empleó los términos "su nivel, esperanzas, preferencias y preocupaciones" mientras que el otro empleó los términos "sus valores, esperanzas, gustos y preocupaciones". En la reunión se acordó emplear "valores" y "gustos" dado que los dos términos se relacionan más con el propósito de la escala de calidad de vida. En las traducciones inversas se tradujo la palabra "instrumento" en un caso como "assessment" y en el otro como "tool", se acordó dejar la palabra "instrumento", dado que estamos hablando de una escala.
Opciones de respuesta de la escala
Las traducciones de las opciones de respuesta fueron diferentes en la opción Moderately, que fue traducida como "moderadamente", no obstante en el consenso se acordó el término "mucho" por ser una expresión más comprensible dentro de las opciones de respuesta que se estaban considerando. Las traducciones inversas fueron similares al original en todas las opciones de respuesta.
Ítems de la escala
En las traducciones directas del dominio físico los ítems 1, 2, 3, 6 y 7; del dominio psicoemocional los ítems 4, 5, 6 y 7; del dominio cognitivo los ítems 4 y 5; del dominio ecosocial los ítems 1, 2, 5, 6 y 7; del dominio del alma los ítems 1, 2, 3, 4, 5 y 6; del dominio espiritual el ítem 3 y del dominio interacción espiritual el ítem 4, se usaron las mismas palabras y la misma redacción, por lo tanto se consideró redacción idéntica.
Hubo algunos ítems en los cuales se emplearon las mismas palabras en las traducciones directas; aunque se encontraron variaciones en redacción estas no afectaron el significado en el contexto colombiano, por lo cual se eligió la que se consideró más fácil de comprender por los pacientes: dominio físico ítems 4 y 5; dominio psicoemocional ítems 1, 2 y 3; dominio cognitivo ítems 1, 2 y 3; dominio ecosocial ítem 3, dominio espiritual ítem 1 y 2 y dominio interacción espiritual ítem 2. De igual forma, se encontraron diferentes palabras en las traducciones del dominio ecosocial ítem 4; del dominio espiritual ítem 4; y del dominio interacción espiritual ítems 1 y 3, así:
Dominio ecosocial, ítem 4: transport facilities fue traducido como "facilidades de transporte" por el primer traductor y como "medios de transporte" por el segundo traductor. En consenso se acordó la segunda traducción por considerarse más apropiada en el contexto de rehabilitación.
Dominio espiritual, ítem 4: divine guidance in your life fue traducido como "intervención de Dios en su vida" por el primer traductor y como "guía divina en su vida" por el segundo traductor. En consenso se optó por la segunda traducción por ser más cercana a la versión original y considerarse más apropiada y clara conceptualmente para los pacientes.
Dominio interacción espiritual, ítem 1: close to God or your object of worship fue traducido como "cercano a Dios o a su objeto de devoción" por el primer traductor y como "cercano a Dios o a su objeto de adoración" por el segundo traductor. En consenso se acordó que "objeto de devoción" podría ser mejor entendido por los pacientes, sin embargo era una terminología poco empleada en contexto colombiano y en consenso se propuso "cercano a Dios o a sus creencias religiosas", lo cual fue aceptado por el autor original de la escala.
Dominio interacción espiritual, ítem 3: your relationship with God or your object of worship se presentó un caso similar al ítem anterior y se resolvió de la misma forma con el aval del autor de la escala, por considerarse más comprensible para los examinados.
Proceso de revisión de las traducciones directas e inversas
Después de obtener la versión preliminar de la escala se realizaron las dos traducciones inversas. Posteriormente se envió, al autor de la escala, la traducción para revisión en abril 15 de 2013, quien hizo algunas sugerencias, las cuales se tomaron en cuenta para la siguiente etapa.
Prueba piloto
Se realizó entre agosto 1 y noviembre 20 de 2013. La prueba fue leída por 20 pacientes, cuya media de edad fue 49.5 años y desviación estándar 14.87 años; la mitad de la población fueron mujeres. Todos los pacientes estaban asistiendo o habían asistido previamente al servicio de rehabilitación de la Clínica Universidad de La Sabana. En la Tabla 1 se muestran las características de los pacientes que participaron en la prueba.
Algunos pacientes manifestaron confusión en el dominio físico, ítem 4, porque no tienen dolor, alteración en la sensibilidad o malestar general en el momento de la entrevista, a lo cual el autor de la escala respondió que deben señalar la opción que indica que no están limitados por ninguna de estas alteraciones. En el dominio ecosocial algunos no comprendieron a qué se refería en el 4 ítem acceso a medios de transporte, a lo cual el autor de la escala respondió que esta pregunta evalúa tanto la habilidad física, como los medios de transporte disponibles; y finalmente, otro paciente manifestó no comprender a qué se refería el ítem 1 del dominio espiritual Hasta qué punto usted entiende a Dios, a lo cual el autor respondió que si el paciente no lo entiende, debe señalar la opción que indica que no lo entiende, sabiendo que la pregunta tiene que ver con el concepto de Dios, pero también con su naturaleza y sus acciones.
Las inquietudes fueron planteadas al autor en noviembre 28 y en diciembre 9 respondió explicando lo anteriormente comentado. Terminado el proceso, se decidió dejar esta versión de la escala, considerada como la versión en español colombiano estándar de la escala HRQLISP-40 (Tabla 2).
Discusión
En este estudio, por medio de un proceso riguroso, se realizó la adaptación transcultural de la escala HRQLISP-40 de calidad de vida para pacientes con ACV y para uso en población colombiana. A partir de este estudio de adaptación transcultural, y una vez realizada la evaluación de sus propiedades psicométricas, la escala podrá utilizarse para valorar calidad de vida en pacientes colombianos con ACV; en este sentido, al incluir la esfera espiritual, como lo propone la escala HRQLISP-40, se podrá realizar una aproximación más multidimensional, dado que, como se comentó previamente, este factor ha mostrado relevancia en el pronóstico en pacientes con ACV y con diagnósticos similares (15,25).
Existen en la literatura instrumentos reconocidos, validados y que son utilizados para medir calidad de vida en pacientes con ACV (26,27). Lo importante es que en el escenario de un proceso de rehabilitación integral se deben utilizar todas las herramientas disponibles y que hayan demostrado resultados favorables en el pronóstico de los pacientes teniendo en cuenta que cada paciente se debe manejar en forma individual, pero abarcando en cada uno de ellos el espectro de posibilidades de apoyo para su recuperación.
Se espera que en el futuro los instrumentos diseñados para seguimiento en estos pacientes incluyan aspectos relacionados con la esfera espiritual, aunque esto equivalga a una evaluación compleja y requiera de su aplicación en conjunto con otros instrumentos que midan más a profundidad aspectos de la espiritualidad; estos instrumentos se vienen desarrollando actualmente en otras condiciones como diabetes, cáncer, hipertensión arterial, abuso de sustancias psicoactivas y sintomatología depresiva (28).
Los estudios han revelado, mediante la aplicación de diversos instrumentos, que existe una relación inversamente proporcional entre espiritualidad y depresión; se ha postulado que la espiritualidad probablemente causa una sensación significativa de paz interior que protege contra sentimientos y actitudes negativas, lo cual hace que los pacientes adquieran comportamientos de autocuidado, muy necesarios en los procesos de rehabilitación tanto institucional como en planes caseros (29,30).
Una de las complicaciones más frecuentes de los pacientes sobrevivientes a ACV son los síntomas emocionales; estos se han visto relacionados con la esfera espiritual en estudios de calidad de vida, por lo tanto, dentro de la valoración de pacientes que ingresan a un programa de rehabilitación se debe explorar si existe intereses o preocupaciones espirituales, de tal manera que este aspecto se pudiera intervenir al tiempo con el proceso (6,31). Previamente, se ha explorado la relación entre creencias religiosas y el estado de ánimo de los pacientes, y se ha encontrado que estas creencias influyen en la capacidad de enfrentar la vida después de un ACV, e incluso pueden actuar como un factor protector contra el estrés emocional.
La fe es un concepto global, la espiritualidad y la religiosidad son conceptos más específicos. La espiritualidad tiene que ver con el concepto de lo trascendente, se relaciona con el sentido de la vida, entendiendo que hay cosas que no se pueden entender o ver, como un poder fuera del mundo corporal. Por otro lado, la religiosidad implica una doctrina compartida por otras personas, en este sentido refiere al hecho de hacer participación social en los grupos religiosos, aceptar ciertas normas y tener estilos de vida particulares que pueden explicar los beneficios en cuanto a la salud de las personas se refiere; en realidad no hay investigaciones acerca de tratamientos de pacientes con ACV utilizando técnicas religiosas y una limitación de estos estudios es que los pacientes no diferencian fácilmente religiosidad de espiritualidad (32).
Es importante tener en cuenta que la medición de calidad de vida —en términos del acceso a procesos de rehabilitación física o recuperación de la discapacidad— implica que probablemente con el tiempo se encuentren cambios en las respuestas a los instrumentos empleados, como consecuencia de los avances en calidad y resultados de las intervenciones relacionados con procesos de adaptación o cambios en la percepción de la discapacidad —tiempo y envejecimiento—. Lo anterior incrementa las dificultades metodológicas para obtener un instrumento fiable en el tiempo, dado que cada evento futuro puede afectar la puntuación inicial que en su momento se dio; en este caso, a alguno de los ítems del instrumento de evaluación de calidad de vida en ACV (33).
Aunque es muy importante individualizar a los pacientes en el momento de realizar intervenciones —dado que muchos conceptos, independiente de la cultura, son difíciles de medir en una escala y se requiere más de una entrevista en profundidad con cada paciente, más si se tiene en cuenta lo multidimensional del concepto de calidad de vida (34)—, no hay que perder de vista que estas herramientas ayudan a medir ciertos aspectos generales, permiten a los clínicos tomar decisiones en el trabajo diario con los pacientes y promueven una investigación con resultados fiables.
Conflicto de intereses
Ninguno declarado por los autores.
Financiación
Docencia e Investigación de la Universidad de La Sabana. Clínica Universidad de La Sabana.
Agradecimientos
Los autores agradecen a Ojo Owolabi, autor de la escala, quien autorizó el uso del instrumento y realizó el proceso de revisión de las traducciones directas, versión preliminar y traducciones inversas. A Michelle Benítez y Mattew Brigmon quienes realizaron las traducciones directas. A Eulalia Monton y a Yady González quienes llevaron a cabo las traducciones inversas. Y a los pacientes del servicio de rehabilitación de la Clínica Universidad de La Sabana quienes participaron en la realización de la prueba piloto de la escala.
Referencias
1. Truelsen T, Heuschmann PU, Bonita R, Arjundas G, Dalal P, Damasceno A, et al. Standard method for developing stroke registers in low-income and middle-income countries: experiences from a feasibility study of a stepwise approach to stroke surveillance (STEPS Stroke). Lancet Neurol. 2007 [cited 2015 mar 26];6(2):134-9. http://doi.org/dvxcbr.
2. Abubakar SA, Isezuo SA. Health related quality of life of stroke survivors: experience of a stroke unit. Int J Biomed Sci. 2012 [cited 2015 mar 26];8(3):183-7. Available from: http://goo.gl/kH05Xc.
3. World Health Organisation. Cancer. WHO Definition of Palliative Care. 2012 [cited 2015 mar 26]. Available from: http://goo.gl/N4AyWE.
4. Carod-Artal FJ. [Specific scales for rating quality of life after stroke]. Rev Neurol. 2004 [cited 2015 mar 26];39(11):1052-62. Spanish. Available from: http://goo.gl/HoirLs.
5. Owolabi MO. Impact of stroke on health-related quality of life in diverse cultures: the Berlin-Ibadan multicenter international study. Health Qual Life Outcomes. 2011 [cited 2015 mar 26];9(1):1-11. http://doi.org/dqk4q7.
6. Howitt SC, Jones MP, Jusabani A, Gray WK, Aris E, Mugusi F, et al. A cross-sectional study of quality of life in incident stroke survivors in rural northern Tanzania. J Neurol. 2011 [cited 2015 mar 26];258(8):1422-30. http://doi.org/ckggz4.
7. Steinhauser KE, Christakis NA, Clipp EC, McNeilly M, McIntyre L, Tulsky JA. Factors considered important at the end of life by patients, family, physicians, and other care providers. JAMA. 2000 [cited 2015 mar 26];284(19):2476-82. http://doi.org/c9377z.
8. Creutzfeldt CJ, Holloway RG, Walker M. Symptomatic and palliative care for stroke survivors. J Gen Intern Med. 2012 [cited 2015 mar 26];27(7):853-60. http://doi.org/fzj3zb.
9. Giaquinto S, Giachetti I, Spiridigliozzi C, Nolfe G. Quality of life after stroke in a rehabilitation setting. Clin Exp Hypertens. 2010 [cited 2015 mar 26];32(7):426-30. http://doi.org/d3pqvp.
10. Koenig HG, Hays JC, Larson DB, George LK, Cohen HJ, McCullough ME, et al. Does religious attendance prolong survival? A six-year follow-up study of 3,968 older adults. J Gerontol A Biol Sci Med Sci. 1999 [cited 2015 mar 26];54(7):M370-6. http://doi.org/bds6cn.
11. Oman D, Reed D. Religion and mortality among the community-dwelling elderly. Am J Public Health. 1998 [cited 2015 mar 26];88(10):1469-75. Available from: http://goo.gl/ypbxxr.
12. Van Ness PH, Kasl SV. Religion and cognitive dysfunction in an elderly cohort. J Gerontol B Psychol Sci Soc Sci. 2003 [cited 2015 mar 26];58(1):S21-9. http://doi.org/c7t54r.
13. Ones K, Yilmaz E, Cetinkaya B, Caglar N. Quality of life for patients poststroke and the factors affecting it. J Stroke Cerebrovasc Dis. 2005 [cited 2015 mar 26];14(6):261-6. Available from: http://goo.gl/ZL3v9b.
14. Cerniauskaite M, Quintas R, Koutsogeorgou E, Meucci P, Sattin D, Leonardi M, et al. Quality-of-life and disability in patients with stroke. Am J Phys Med Rehabil. 2012 [cited 2015 mar 26];91(13 Suppl 1):S39-47. http://doi.org/fz37zt.
15. Harrison JK, McArthur KS, Quinn TJ. Assessment scales in stroke: clinimetric and clinical considerations. Clin Interv Aging. 2013 [cited 2015 mar 26];8:201-11. http://doi.org/27m.
16. Boosman H, Passier PE, Visser-Meily JM, Rinkel GJ, Post MW. Validation of the Stroke Specific Quality of Life scale in patients with aneurysmal subarachnoid haemorrhage. J Neurol Neurosurg Psychiatry. 2010 [cited 2015 mar 27];81(5):485-9. http://doi.org/d66mr2.
17. Fernández-Concepción O, Ramírez-Pérez E, Álvarez MA, Buergo-Zuáznabar MA. [Validation of the stroke-specific quality of life scale (ECVI-38)]. Rev Neurol. 2008 [cited 2015 mar 27];46(3):147-52. Spanish. Available from: http://goo.gl/MJYxwF.
18. Pickard AS, Johnson JA, Feeny DH. Responsiveness of generic health-related quality of life measures in stroke. Qual Life Res. 2005 [cited 2015 mar 27];14(1):207-19. http://doi.org/dgc4t2.
19. Owolabi MO. Psychometric properties of the HRQOLISP-40: a novel, shortened multiculturally valid holistic stroke measure. Neurorehabil Neural Repair. 2010 [cited 2015 mar 27];24(9):814-25. http://doi.org/dc5qkb.
20. Owolabi MO. Consistent determinants of post-stroke health-related quality of life across diverse cultures: Berlin-Ibadan study. Acta Neurol Scand. 2013 [cited 2015 mar 27];128(5):311-20. http://doi.org/277.
21. Owolabi MO. What are the consistent predictors of generic and specific post-stroke health-related quality of life? Cerebrovasc Dis. 2010 [cited 2015 mar 27];29(2):105-10. http://doi.org/ds9d45.
22. Owolabi MO. Which is more valid for stroke patients: generic or stroke-specific quality of life measures? Neuroepidemiology. 2010 [cited 2015 mar 27];34(1):8-12. http://doi.org/bvjffq.
23. Dewolf L, Koller M, Velikova G, Johnson C, Scott N, Bottomley A, et al. Traslation Procedure. EORTC. 3 ed. Brussels: EORTC QUALITY OF LIFE GROUP; 2009 [cited 2015 mar 27]. Available from: http://goo.gl/Xo1C58.
24. Sánchez R, Echeverry J. Validating scales used for measuring factors in medicine. Rev. Salud Pública. 2004 [cited 2015 mar 27];6(3):302-18. Spanish. http://doi.org/c6kjh7.
25. Fleck MP, Borges ZN, Bolognesi G, da Rocha NS. Development of WHOQOL spirituality, religiousness and personal beliefs module. Rev Saude Publica. 2003 [cited 2015 mar 27];37(4):446-55. http://doi.org/dbxt5r.
26. Liwocha M, Galus K, Kozak-Szkopek E, Kowal R. [Assessment of the influence of rehabilitation in patients treated in a hospital rehabilitation ward due to consequences of neurological diseases]. Pol Merkur Lekarski. 2013 [cited 2015 mar 27];35(205):22-7. Availablr from: http://goo.gl/36Vhmj.
27. Takemasa S, Nakagoshi R, Murakami M, Uesugi M, Inoue Y, Gotou M, et al. Factors affecting quality of life of the homebound elderly hemiparetic stroke patients. J Phys Ther Sci. 2014 [cited 2015 mar 27];26(2):301-3. http://doi.org/279.
28. Mueller PS, Plevak DJ, Rummans TA. Religious involvement, spirituality, and medicine: implications for clinical practice. Mayo Clin Proc. 2001 [cited 2015 mar 27];76(12):1225-35. http://doi.org/fj22bn.
29. Johnstone B, McCormack G, Yoon DP, Smith ML. Convergent/Divergent validity of the brief multidimensional measure of religiousness/spirituality: empirical support for emotional connectedness as a "spiritual" construct. J Relig Health. 2012 [cited 2015 mar 27];51(2):529-41. http://doi.org/dc363p.
30. Lynch CP, Hernández-Tejada MA, Strom JL, Egede LE. Association between spirituality and depression in adults with type 2 diabetes. Diabetes Educ. 2012 [cited 2015 mar 27];38(3):427-35. http://doi.org/28b.
31. Buijck BI, Zuidema SU, Spruit-van Eijk M, Bor H, Gerritsen DL, Koopmans RT. Determinants of geriatric patients' quality of life after stroke rehabilitation. Aging Ment Health. 2014 [cited 2015 mar 27];18(8):980-5. http://doi.org/28c.
32. Giaquinto S, Spiridigliozzi C, Caracciolo B. Can faith protect from emotional distress after stroke? Stroke. 2007 [cited 2015 mar 27];38(3):993-7. http://doi.org/d992hn.
33. Barclay R, Tate RB. Response shift recalibration and reprioritization in health-related quality of life was identified prospectively in older men with and without stroke. J Clin Epidemiol. 2014 [cited 2015 mar 27];67(5):500-7. http://doi.org/28d.
34. Bernheim JL. How to get serious answers to the serious question: "How have you been?": subjective quality of life (QOL) as an individual experiential emergent construct. Bioethics. 1999 [cited 2015 mar 27];13(3-4):272-87. http://doi.org/d48s43.
Referencias
Truelsen T, Heuschmann PU, Bonita R, Arjundas G, Dalal P, Damasceno A, et al. Standard method for developing stroke registers in low-income and middle-income countries: experiences from a feasibility study of a stepwise approach to stroke surveillance (STEPS Stroke). Lancet Neurol. 2007 [cited 2015 mar 26];6(2):134-9. http://doi.org/dvxcbr.
Abubakar SA, Isezuo SA. Health related quality of life of stroke survivors: experience of a stroke unit. Int J Biomed Sci. 2012 [cited 2015 mar 26];8(3):183-7. Available from: http://goo.gl/kH05Xc.
World Health Organisation. Cancer. WHO Definition of Palliative Care. 2012 [cited 2015 mar 26]. Available from: http://goo.gl/N4AyWE.
Carod-Artal FJ. [Specific scales for rating quality of life after stroke]. Rev Neurol. 2004 [cited 2015 mar 26];39(11):1052-62. Spanish. Available from: http://goo.gl/HoirLs.
Owolabi MO. Impact of stroke on health-related quality of life in diverse cultures: the Berlin-Ibadan multicenter international study. Health Qual Life Outcomes. 2011 [cited 2015 mar 26];9(1):1-11. http://doi.org/dqk4q7.
Howitt SC, Jones MP, Jusabani A, Gray WK, Aris E, Mugusi F, et al. A cross-sectional study of quality of life in incident stroke survivors in rural northern Tanzania. J Neurol. 2011 [cited 2015 mar 26];258(8):1422-30. http://doi.org/ckggz4.
Steinhauser KE, Christakis NA, Clipp EC, McNeilly M, McIntyre L, Tulsky JA. Factors considered important at the end of life by patients, family, physicians, and other care providers. JAMA. 2000 [cited 2015 mar 26];284(19):2476-82. http://doi.org/c9377z.
Creutzfeldt CJ, Holloway RG, Walker M. Symptomatic and palliative care for stroke survivors. J Gen Intern Med. 2012 [cited 2015 mar 26];27(7):853-60. http://doi.org/fzj3zb.
Giaquinto S, Giachetti I, Spiridigliozzi C, Nolfe G. Quality of life after stroke in a rehabilitation setting. Clin Exp Hypertens. 2010 [cited 2015 mar 26];32(7):426-30. http://doi.org/d3pqvp.
Koenig HG, Hays JC, Larson DB, George LK, Cohen HJ, McCullough ME, et al. Does religious attendance prolong survival? A six-year follow-up study of 3,968 older adults. J Gerontol A Biol Sci Med Sci. 1999 [cited 2015 mar 26];54(7):M370-6. http://doi.org/bds6cn.
Oman D, Reed D. Religion and mortality among the community-dwelling elderly. Am J Public Health. 1998 [cited 2015 mar 26];88(10):1469-75. Available from: http://goo.gl/ypbxxr.
Van Ness PH, Kasl SV. Religion and cognitive dysfunction in an elderly cohort. J Gerontol B Psychol Sci Soc Sci. 2003 [cited 2015 mar 26];58(1):S21-9. http://doi.org/c7t54r.
Ones K, Yilmaz E, Cetinkaya B, Caglar N. Quality of life for patients poststroke and the factors affecting it. J Stroke Cerebrovasc Dis. 2005 [cited 2015 mar 26];14(6):261-6. Available from: http://goo.gl/ZL3v9b.
Cerniauskaite M, Quintas R, Koutsogeorgou E, Meucci P, Sattin D, Leonardi M, et al. Quality-of-life and disability in patients with stroke. Am J Phys Med Rehabil. 2012 [cited 2015 mar 26];91(13 Suppl 1):S39-47. http://doi.org/fz37zt.
Harrison JK, McArthur KS, Quinn TJ. Assessment scales in stroke: clinimetric and clinical considerations. Clin Interv Aging. 2013 [cited 2015 mar 26];8:201-11. http://doi.org/27m.
Boosman H, Passier PE, Visser-Meily JM, Rinkel GJ, Post MW. Validation of the Stroke Specific Quality of Life scale in patients with aneurysmal subarachnoid haemorrhage. J Neurol Neurosurg Psychiatry. 2010 [cited 2015 mar 27];81(5):485-9. http://doi.org/d66mr2.
Fernández-Concepción O, Ramírez-Pérez E, Álvarez MA, Buergo-Zuáznabar MA. [Validation of the stroke-specific quality of life scale (ECVI-38)]. Rev Neurol. 2008 [cited 2015 mar 27];46(3):147-52. Spanish. Available from: http://goo.gl/MJYxwF.
Pickard AS, Johnson JA, Feeny DH. Responsiveness of generic health-related quality of life measures in stroke. Qual Life Res. 2005 [cited 2015 mar 27];14(1):207-19. http://doi.org/dgc4t2.
Owolabi MO. Psychometric properties of the HRQOLISP-40: a novel, shortened multiculturally valid holistic stroke measure. Neurorehabil Neural Repair. 2010 [cited 2015 mar 27];24(9):814-25. http://doi.org/dc5qkb.
Owolabi MO. Consistent determinants of post-stroke health-related quality of life across diverse cultures: Berlin-Ibadan study. Acta Neurol Scand. 2013 [cited 2015 mar 27];128(5):311-20. http://doi.org/277.
Owolabi MO. What are the consistent predictors of generic and specific post-stroke health-related quality of life? Cerebrovasc Dis. 2010 [cited 2015 mar 27];29(2):105-10. http://doi.org/ds9d45.
Owolabi MO. Which is more valid for stroke patients: generic or stroke-specific quality of life measures? Neuroepidemiology. 2010 [cited 2015 mar 27];34(1):8-12. http://doi.org/bvjffq.
Dewolf L, Koller M, Velikova G, Johnson C, Scott N, Bottomley A, et al. Traslation Procedure. EORTC. 3 ed. Brussels: EORTC QUALITY OF LIFE GROUP; 2009 [cited 2015 mar 27]. Available from: http://goo.gl/Xo1C58.
Sánchez R, Echeverry J. Validating scales used for measuring factors in medicine. Rev. Salud Pública. 2004 [cited 2015 mar 27];6(3):302-18. Spanish. http://doi.org/c6kjh7.
Fleck MP, Borges ZN, Bolognesi G, da Rocha NS. Development of WHOQOL spirituality, religiousness and personal beliefs module. Rev Saude Publica. 2003 [cited 2015 mar 27];37(4):446-55. http://doi.org/dbxt5r.
Liwocha M, Galus K, Kozak-Szkopek E, Kowal R. [Assessment of the influence of rehabilitation in patients treated in a hospital rehabilitation ward due to consequences of neurological diseases]. Pol Merkur Lekarski. 2013 [cited 2015 mar 27];35(205):22-7. Availablr from: http://goo.gl/36Vhmj.
Takemasa S, Nakagoshi R, Murakami M, Uesugi M, Inoue Y, Gotou M, et al. Factors affecting quality of life of the homebound elderly hemiparetic stroke patients. J Phys Ther Sci. 2014 [cited 2015 mar 27];26(2):301-3. http://doi.org/279.
Mueller PS, Plevak DJ, Rummans TA. Religious involvement, spirituality, and medicine: implications for clinical practice. Mayo Clin Proc. 2001 [cited 2015 mar 27];76(12):1225-35. http://doi.org/fj22bn.
Johnstone B, McCormack G, Yoon DP, Smith ML. Convergent/Divergent validity of the brief multidimensional measure of religiousness/spirituality: empirical support for emotional connectedness as a "spiritual" construct. J Relig Health. 2012 [cited 2015 mar 27];51(2):529-41. http://doi.org/dc363p.
Lynch CP, Hernández-Tejada MA, Strom JL, Egede LE. Association between spirituality and depression in adults with type 2 diabetes. Diabetes Educ. 2012 [cited 2015 mar 27];38(3):427-35. http://doi.org/28b.
Buijck BI, Zuidema SU, Spruit-van Eijk M, Bor H, Gerritsen DL, Koopmans RT. Determinants of geriatric patients' quality of life after stroke rehabilitation. Aging Ment Health. 2014 [cited 2015 mar 27];18(8):980-5. http://doi.org/28c.
Giaquinto S, Spiridigliozzi C, Caracciolo B. Can faith protect from emotional distress after stroke? Stroke. 2007 [cited 2015 mar 27];38(3):993-7. http://doi.org/d992hn.
Barclay R, Tate RB. Response shift recalibration and reprioritization in health-related quality of life was identified prospectively in older men with and without stroke. J Clin Epidemiol. 2014 [cited 2015 mar 27];67(5):500-7. http://doi.org/28d.
Bernheim JL. How to get serious answers to the serious question: "How have you been?": subjective quality of life (QOL) as an individual experiential emergent construct. Bioethics. 1999 [cited 2015 mar 27];13(3-4):272-87. http://doi.org/d48s43.
Cómo citar
APA
ACM
ACS
ABNT
Chicago
Harvard
IEEE
MLA
Turabian
Vancouver
Descargar cita
CrossRef Cited-by
1. Fabiola Moscoso Alvarado, Johana Alejandra Bohórquez Garcia, Lina Marcela Rincón Ortiz, Steffanny Escobar Soto, Edgar Debray Hernández Alvarez. (2020). Translation and cross-cultural adaptation of the Wheelchair Skills Test (WST) version 4.3 form from English to Colombian Spanish. Disability and Rehabilitation: Assistive Technology, 15(5), p.521. https://doi.org/10.1080/17483107.2019.1594404.
2. Lisieux E. De Borba Telles, Franklin Escobar Córdoba. (2015). Revista de la Facultad de Medicina y Ciência Latinoamericana. Revista de la Facultad de Medicina, 63(4), p.561. https://doi.org/10.15446/revfacmed.v63n4.54223.
3. Yahira Rossini Guzmán Sabogal, Jorge Pla Vidal, Ricardo Sánchez Pedraza, Felipe Ortuño Sánchez-Pedreño, María Catalina Gómez Guevara. (2016). Health-related quality of life in stroke patients questionnaire, short version (HRQOLISP-40): validation for its use in Colombia. BMC Neurology, 16(1) https://doi.org/10.1186/s12883-016-0770-5.
Dimensions
PlumX
Visitas a la página del resumen del artículo
Descargas
Licencia
Derechos de autor 2015 Revista de la Facultad de Medicina

Esta obra está bajo una licencia Creative Commons Reconocimiento 3.0 Unported.
-