Procalcitonina como marcador de sepsis en niños
Procalcitonin as a Biomarker for Sepsis in Children
DOI:
https://doi.org/10.15446/revfacmed.v64n2.50585Palabras clave:
Biomarcadores, Infección, Sepsis, Lactantes, Niños (es)Procalcitonin, Cultures, Infection, Sepsis, Children (en)
Introducción. La procalcitonina es un biomarcador de infección bacteriana severa y sepsis, con aplicación diagnóstica, para severidad y pronóstico, el cual muestra valores de sensibilidad, especificidad y puntos de corte variables en niños.
Materiales y métodos. Estudio retrospectivo, observacional y descriptivo. Se incluyeron niños de 7 días a 18 años, a quienes se les tomó procalcitonina y cultivo el mismo día. Se evaluaron otros biomarcadores como proteína C reactiva y los datos se tomaron de la historia clínica por medio de un formulario.
Resultados. Se incluyeron 274 muestras de procalcitonina y cultivos, correspondientes a 162 pacientes con edad promedio de 1.5 años —59% masculinos—. De los 274 cultivos, el 81% fueron hemocultivos, siendo positivos el 17%. La procalcitonina con punto de corte >0.5ng/ml mostró sensibilidad de 76%, especificidad de 46%, VPP de 23% y VPN de 90% para sepsis, con AUC 0.6899 (IC95%: 0.6059-0.774). Se encontró de forma estadísticamente significativa que a mayor valor de procalcitonina mayor mortalidad (p=0.003). La procalcitonina mostró mejor rendimiento que los otros biomarcadores para predecir sepsis.
Conclusión. La procalcitonina tiene un buen rendimiento diagnóstico como marcador de sepsis en niños —con mayor utilidad cuando toma valores negativos— y buen valor pronóstico al relacionarse con mortalidad.
Background. Procalcitonin is a biomarker of severe bacterial infection and sepsis, with diagnostic, monitoring, severity and prognosis applications, that shows values of sensitivity, specificity and variable cutoff in children.
Materials and Methods. Retrospective, observational and descriptive study. Patients from 7 days to 18 years old who were taken procalcitonin and cultures on the same day were included. Other biomarkers such as C-reactive protein were assessed. Data were taken from their medical records using an electronic formulary.
Results. 274 samples of procalcitonin and cultures were included, corresponding to 162 patients, 59% male, aged 19 days to 13 years (mean=1.5 years). The most common diagnosis was bacterial pneumonia (39%). Of the 274 cultures, 81% were blood cultures, of which 17% were positive. Procalcitonin with cutoff>0.5ng/ml showed sensitivity of 76%, specificity of 46%, PPV 23%, NPV 90% for sepsis, with an AUC 0.6899 (95% CI 0.6059 to 0774). Greater mortality with high values of procalcitonin (p=0.003) was found. Procalcitonin showed better performance than C-reactive protein, leukocyte and neutrophil count for sepsis prediction.
Conclusion. Procalcitonin has a good diagnostic performance as a marker of sepsis in children —with a higher usefulness with negative values— and has a good prognostic value for mortality.
INVESTIGACIÓN ORIGINAL
DOI: https://doi.org/10.15446/revfacmed.v64n2.50585
Procalcitonina como marcador de sepsis en niños
Procalcitonin as a Biomarker for Sepsis in Children
Diana González-Rangel1,2 • Germán Camacho-Moreno1,2 • Omar Quintero-Guevara1,2
Recibido: 11/05/2015 Aceptado: 29/10/2015
1 Fundación Hospital de la Misericordia de Bogotá - Departamento de Pediatría - Bogotá, D.C. - Colombia.
2 Universidad Nacional de Colombia - Sede Bogotá - Facultad de Medicina - Departamento de Pediatría - Bogotá, D.C. - Colombia.
Correspondencia: Diana Marcela González-Rangel. Carrera 68B No. 22A-71, torre 3, apartamento 712. Teléfono: +57 1 4276984; celular: +57 3203928741. Correo electrónico: dimagozz@hotmail.com.
| Resumen |
Introducción. La procalcitonina es un biomarcador de infección bacteriana severa y sepsis, con aplicación diagnóstica, para severidad y pronóstico, el cual muestra valores de sensibilidad, especificidad y puntos de corte variables en niños.
Materiales y métodos. Estudio retrospectivo, observacional y descriptivo. Se incluyeron niños de 7 días a 18 años, a quienes se les tomó procalcitonina y cultivo el mismo día. Se evaluaron otros biomarcadores como proteína C reactiva y los datos se tomaron de la historia clínica por medio de un formulario.
Resultados. Se incluyeron 274 muestras de procalcitonina y cultivos, correspondientes a 162 pacientes con edad promedio de 1.5 años —59% masculinos—. De los 274 cultivos, el 81% fueron hemocultivos, siendo positivos el 17%. La procalcitonina con punto de corte >0.5ng/ml mostró sensibilidad de 76%, especificidad de 46%, VPP de 23% y VPN de 90% para sepsis, con AUC 0.6899 (IC95%: 0.6059-0.774). Se encontró de forma estadísticamente significativa que a mayor valor de procalcitonina mayor mortalidad (p=0.003). La procalcitonina mostró mejor rendimiento que los otros biomarcadores para predecir sepsis.
Conclusión. La procalcitonina tiene un buen rendimiento diagnóstico como marcador de sepsis en niños —con mayor utilidad cuando toma valores negativos— y buen valor pronóstico al relacionarse con mortalidad.
Palabras clave: Biomarcadores; Infección; Sepsis; Lactantes; Niños (DeCS).
González-Rangel D, Camacho-Moreno G, Quintero-Guevara O. Procalcitonina como marcador de sepsis en niños. Rev. Fac. Med. 2016;64(2):215-21. Spanish. doi: https://doi.org/10.15446/revfacmed.v64n2.50585.
Abstract
Background. Procalcitonin is a biomarker of severe bacterial infection and sepsis, with diagnostic, monitoring, severity and prognosis applications, that shows values of sensitivity, specificity and variable cutoff in children.
Materials and Methods. Retrospective, observational and descriptive study. Patients from 7 days to 18 years old who were taken procalcitonin and cultures on the same day were included. Other biomarkers such as C-reactive protein were assessed. Data were taken from their medical records using an electronic formulary.
Results. 274 samples of procalcitonin and cultures were included, corresponding to 162 patients, 59% male, aged 19 days to 13 years (mean=1.5 years). The most common diagnosis was bacterial pneumonia (39%). Of the 274 cultures, 81% were blood cultures, of which 17% were positive. Procalcitonin with cutoff>0.5ng/ml showed sensitivity of 76%, specificity of 46%, PPV 23%, NPV 90% for sepsis, with an AUC 0.6899 (95% CI 0.6059 to 0774). Greater mortality with high values of procalcitonin
(p=0.003) was found. Procalcitonin showed better performance than C-reactive protein, leukocyte and neutrophil count for sepsis prediction.
Conclusion. Procalcitonin has a good diagnostic performance as a marker of sepsis in children —with a higher usefulness with negative values— and has a good prognostic value for mortality.
Keywords: Procalcitonin, Cultures; Infection; Sepsis; Children (MeSH).
González-Rangel D, Camacho-Moreno G, Quintero-Guevara O. [Procalcitonin as a Biomarker for Sepsis in Children]. Rev. Fac. Med. 2016;64(2):215-21. Spanish. doi: https://doi.org/10.15446/revfacmed.v64n2.50585.
Introducción
La procalcitonina (PCT) se ha posicionado como un importante biomarcador sanguíneo en el estudio de síndrome febril en niños (1,2) por su habilidad para predecir infecciones bacterianas localizadas o sistémicas como sepsis (3,4), neumonía (5,6), meningitis (5,7), artritis séptica (5) y pielonefritis (5,8); este es útil desde la edad neonatal hasta los adultos y en condiciones especiales como cáncer, trasplante y enfermedades autoinmunes (5).
La PCT ha mostrado tener alta eficacia diagnóstica al reportar valores de sensibilidad de 75% a 100%, especificidad de 70% a 100%, VPP del 55% a 100% y VPN de 56% a 100%. Esta variación en las características operativas de la PCT se debe a la variación en los puntos de corte, equipos y técnicas empleadas en su medición y el diseño de los estudios (3). La procalcitonina también ha mostrado utilidad como indicador de severidad y pronóstico, ya que sus niveles son un buen indicador de respuesta a tratamiento, severidad de la sepsis y mortalidad (3); hay estudios que han reportado que mediciones repetidas con elevación persistente de PCT se relacionan con falla multiorgánica y mortalidad en niños con sepsis bacteriana (4,5).
La PCT lleva dos décadas siendo estudiada a nivel mundial en el campo de la pediatría (5), y concretamente en la Fundación Hospital de la Misericordia de Bogotá (Fundación HOMI) es utilizada, desde el año 2010 hasta el momento, sin estudios locales que evalúen su impacto; razón por la cual el objetivo principal de este estudio es determinar el valor diagnóstico de la procalcitonina sérica como marcador de infección bacteriana comprobada por medio de cultivo en niños hospitalizados en dicha institución.
Materiales y métodos
Estudio retrospectivo, observacional y descriptivo de pruebas diagnósticas en el que se incluyeron pacientes entre los 7 días y los 18 años, hospitalizados con sospecha de infección bacteriana y a quienes se les tomó PCT y cultivos el mismo día en la institución pediátrica de tercer nivel Fundación HOMI durante el año 2010.
La prueba evaluada fue la procalcitonina sérica y el estándar de oro los cultivos bacterianos en cualquier muestra. Se aceptó que un paciente tuviera varios registros de PCT y cultivos si estos correspondían a mediciones solicitadas con intención diagnóstica y no de seguimiento y tomados en episodios de infección diferentes durante el mismo evento hospitalario o subsiguiente. Si una medición de PCT coincidía con la toma de varios cultivos en el mismo paciente —hemocultivo, urocultivo, cultivo de otro líquido corporal—, se incluían todos de forma separada. Se consideró infección bacteriana comprobada aquella con reporte positivo de cultivo.
Se excluyeron los neonatos menores de 7 días de vida y se establecieron como negativos los cultivos con aislamientos considerados por el médico tratante como contaminación o colonización.
La recolección de datos se realizó a través de un formulario electrónico mediante la revisión de historias clínicas, se incluyeron datos sobre características demográficas y clínicas de los pacientes, resultado de PCT y otros biomarcadores de infección como la proteína C reactiva (PCR), leucocitos y neutrófilos, resultado de cultivos, aislamientos microbiológicos, uso de antibiótico antes y después de la medición de PCT y mortalidad.
Se calculó un tamaño de muestra de 197 para un poder estadístico del 80% y un nivel de confianza del 95%. Se usaron los siguientes parámetros: poder estadístico (1-beta): 80%, nivel de confianza (1-alfa): 95%, área bajo la curva esperada: 0.8, valor de área bajo la curva para la hipótesis nula: 0.6 y probabilidad que un paciente con fiebre tenga un cultivo positivo: 30%. Se usó la fórmula de Hanley y McNeil para el cálculo utilizando la versión de prueba del programa MedCalc versión 12.3 —MedCalc Software, Mariakerke, Bélgica— (9)
En la Fundación HOMI se realiza medición de la PCT por electroquimioluminiscencia prueba Cobas Roche® con puntos de corte negativa <0.5ng/ml, dudosa 0.5-2ng/ml y positiva >2ng/ml; PCR por prueba cualitativa Spinreact® con punto corte 2.6mg/dl; la VSG es una prueba cualitativa manual con punto de corte 0-15mm/hr; el hemograma es de tercera generación de Roche XT1800® y los cultivos se procesan a través del sistema Bact Alert 3D y Vitek 2 Compact.
Para el análisis descriptivo de las variables se utilizaron medidas de tendencia central como promedio y porcentajes de acuerdo con la escala de medición de las variables. La prueba de hipótesis para la comparación del nivel de procalcitonina, según otras variables clínicas, se realizó con la prueba t-Student o el test de suma de rangos de Wilcoxon según la necesidad de estadística paramétrica o no paramétrica. La correlación entre los niveles de procalcitonina y los otros biomarcadores se expresó como el coeficiente de correlación de Spearman. Se calculó sensibilidad, especificidad y valores predictivos para los distintos puntos de corte de la procalcitonina sérica al tiempo que se generaron curvas ROC para establecer el mejor punto de corte. También se calcularon las características operativas de la PCR, leucocitos y neutrófilos según sus puntos de corte establecidos.
Para este estudio se contó con la aprobación del comité de ética de la Fundación HOMI.
Resultados
Se incluyeron 274 muestras de PCT y cultivos correspondientes a 162 pacientes y se excluyeron 126 mediciones de PCT por falta de cultivo. Del total de pacientes incluidos (n=162), la mediana de edad fue 1.5 años (19 días-3.8 años), el 59% fueron masculinos y el 41% femeninos. Del total de toma de muestras de PCT (n=274), el sitio más frecuente de solicitud fue en la Unidad de Cuidado Intensivo Pediátrico (62%) y el 11% de los pacientes fallecieron.
Los diagnósticos más frecuentes en el momento de la toma de la PCT fueron neumonía bacteriana (39%), sepsis (18%), bacteremia en paciente oncológico (10%), sepsis en paciente quemado (7.6%) y meningitis bacteriana (5.5%). De los 274 cultivos, el 81% fueron hemocultivos, 11% urocultivos, 3.6% cultivo de líquido cefalorraquídeo (LCR) y 3.6% cultivos de otros líquidos corporales. De todos los cultivos, 20% fueron positivos (n=55) y 80% negativos (n=219), de los cuales 5.5% fueron por contaminación (n=15).
Los principales gérmenes aislados en todos los cultivos fueron Escherichia coli (21.8%), Staphylococcus aureus (12.73%) y Pseudomonas aeruginosa (10.91%).
No se encontró diferencia significativa en los valores de PCT entre los gérmenes Gram negativos comparados con los Gram positivos (p=0.703). Al determinar la relación de los valores de PCT con el estado al momento del alta, se encontró de forma estadísticamente significativa que a mayor valor de PCT mayor mortalidad (Tabla 1).
Tabla 1. Relación de valores de PCT con estado al momento del alta.
|
PCT punto corte |
Muerto |
Vivo |
Total |
||
|
(n) |
(%) |
(n) |
(%) |
||
|
<0.5ng/ml |
2 |
2.7 |
71 |
97.3 |
73 |
|
0.5-2ng/ml |
5 |
13.2 |
33 |
86.8 |
38 |
|
>2ng/ml |
12 |
22.2 |
42 |
77.8 |
54 |
|
Total |
19 |
|
146 |
|
165 |
* Valor de p para las diferencias de porcentaje: 0.003 **Se presenta resultado del estado del alta de los 165 eventos hospitalarios correspondientes a los 162 pacientes incluidos, de los cuales 3 tuvieron mediciones en 2 hospitalizaciones. Fuente: Elaboración propia.
El 52% de los pacientes recibieron tratamiento antibiótico antes y el 83% después de la toma de las muestras de PCT y cultivo, evidenciándose una tendencia significativa entre el resultado de la PCT y el porcentaje de pacientes a quienes se les inicia antibiótico (73% para <0.5ng/ml, 85.3% para
0.5-2ng/ml y 96.7% para >2ng/ml; p<0.001).
En cuanto a la relación de PCT y hemocultivo, se evidenció que la probabilidad de tener un hemocultivo positivo es mayor en la medida que aumenta el valor de PCT (9.6% para <0.5ng/ml, 17.3% para 0.5-2ng/ml y 27.3% para
>2ng/ml; p=0.01). Esta tendencia se mantuvo cuando se hizo el análisis en el subgrupo de pacientes que recibieron antibiótico previo a la toma de PCT y cultivos (9.5%, 24.2% y 30.9%, respectivamente; p=0.044). Los valores de sensibilidad, especificidad, valor predictivo positivo, valor predictivo negativo, LR positivo y LR negativo de PCT para sepsis se encuentran en la Tabla 2 con los puntos de corte estándar.
Tabla 2. Características operativas de PCT para sepsis.
|
Punto de corte |
>0.5ng/ml |
>2ng/ml |
|
Sensibilidad |
76.9 |
53.8 |
|
Especificidad |
46.2 |
69.6 |
|
Valor predictor positivo |
23.3 |
27.3 |
|
Valor predictor negativo |
90.4 |
87.7 |
|
LR + |
1.43 |
1.77 |
|
LR - |
0.5 |
0.663 |
|
Total |
19 |
146 |
*Área bajo la curva: 0.6899 (IC: 0.6059-0.774). Fuente: Elaboración propia.
La Figura 1 muestra la curva ROC de PCT para sepsis con el área bajo la curva de 0.6899 (IC95%: 0.6059-0.774). Teniendo en cuenta que la neumonía bacteriana fue el diagnóstico más frecuente, al evaluar las características operativas de la PCT como predictor de bacteremia en neumonía complicada y no complicada, se encontró que con un punto de corte >2ng/ml se alcanza sensibilidad del 53%, pero con especificidad del 69% y VPN de 91%.
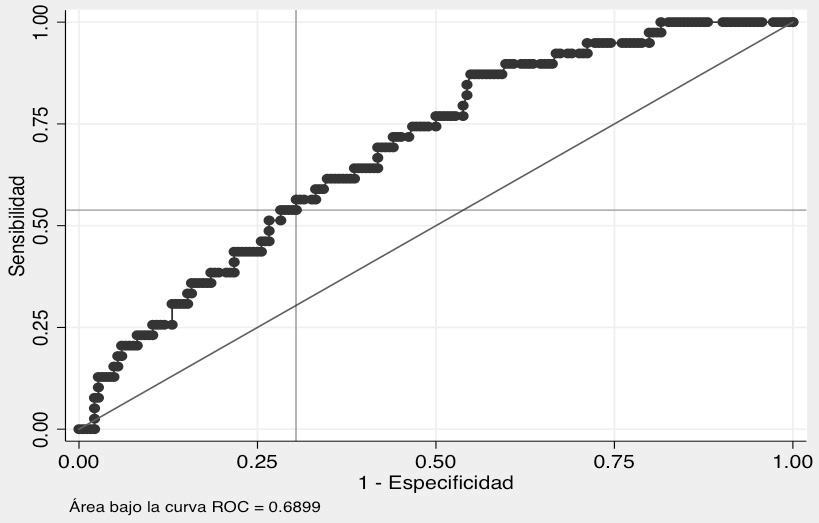
Figura 1. Curva ROC de PCT para sepsis. Fuente: Elaboración propia.
Se incluyeron 193 mediciones de proteína C reactiva (PCR), 13 de VSG y 108 de leucocitos y neutrófilos. Al establecer la correlación entre los valores de PCT y PCR, se encontró un coeficiente de correlación de Spearman de 0.3965 con un valor de p<0.0001. Sin embargo, al comparar los valores de PCT y PCR según los puntos de corte estándar del laboratorio (PCT >2ng/ml y PCR >2.8mg/dl), se encontró que el 96% de las PCR toman valores positivos, independiente de si la PCT es positiva o negativa.
En la Tabla 3 se muestran las características operativas de los cuatro biomarcadores evaluados con los diferentes puntos de corte comúnmente recomendados en la literatura. Para este estudio, se consideraron como puntos de corte óptimo valores de PCT >0.5ng/ml (S79%, E46%), PCR >40mg/dl (S76%, E35%), leucocitos >13.000 (S62%, E56%) y neutrófilos absolutos >6900 (S56% y E51%).
Tabla 3. Características operativas de PCT, PCR, leucocitos y RAN con puntos de corte comúnmente recomendados.
|
Biomarcador |
Sensibilidad |
Especificidad |
LR+ |
LR- |
|
PCT>0.5 |
79% |
46% |
1.48 |
0.44 |
|
PCT>1 |
64% |
60% |
1.62 |
0.6 |
|
PCT>2 |
53% |
69% |
1.77 |
0.66 |
|
PCR>20 |
90% |
17% |
1.08 |
0.58 |
|
PCR>40 |
76% |
35% |
1.18 |
0.66 |
|
PCR>80 |
53% |
58% |
1.2 |
0.79 |
|
Leu>15000 |
37% |
65% |
1.1 |
0.94 |
|
Leu>20000 |
21% |
86% |
1.6 |
0.9 |
|
RAN>12000 |
31% |
70% |
1.07 |
0.969 |
|
RAN>15000 |
15% |
85% |
1.1 |
0.98 |
RAN: Recuento absoluto de neutrófilos. Fuente: Elaboración propia.
En la Figura 2 se muestran las curvas ROC de los cuatro biomarcadores como predictores de sepsis. Al comparar el área bajo la curva de los cuatro biomarcadores, basándose en los datos de los 150 pacientes que tienen medición de los cuatro laboratorios, se encuentra que el área bajo la curva para PCT es 0.71, para PCR 0.59, para leucocitos 0.53 y para neutrófilos absolutos 0.56, con una diferencia estadísticamente significativa entre ellas (p=0.0309).
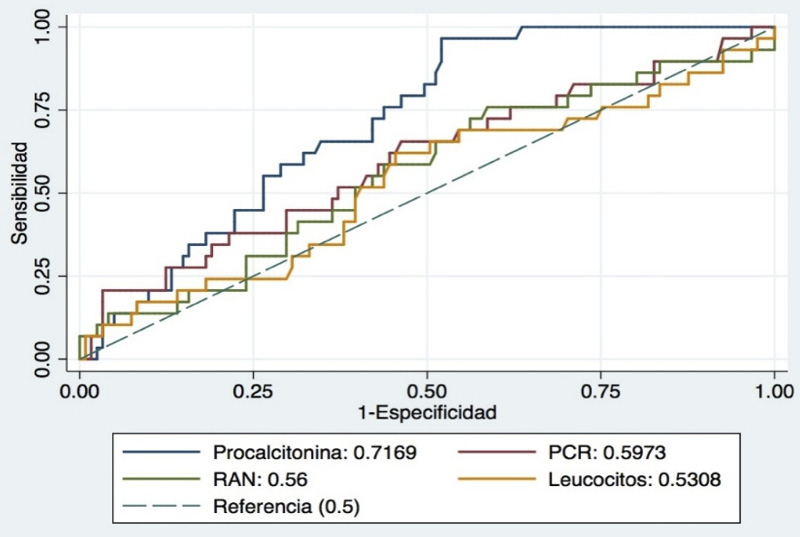
Figura 2. Curva ROC para PCT, PCR y leucocitos RAN como predictores de sepsis. Fuente: Elaboración propia.
Discusión
Al compararlo con PCR, conteo de leucocitos y neutrófilos absolutos, la PCT es un biomarcador eficiente como predictor de sepsis comprobada en niños hospitalizados.
La mortalidad general de los pacientes incluidos fue de 11%, cifra importantemente alta; es probable que esto se correlacione con que el sitio más frecuente de solicitud de la PCT fue la Unidad de Cuidado Intensivo Pediátrico, donde se maneja la mayor complejidad clínica de la institución. Además, se encontró mayor mortalidad en los pacientes con valores elevados de PCT de forma estadísticamente significativa, lo que se relaciona con varios estudios (4,5) que corroboran el papel de la procalcitonina como indicador de severidad y pronóstico.
En cuanto a los diagnósticos, se encontró que el más frecuente fue sospecha de neumonía bacteriana, lo que refleja la carga que tiene la patología respiratoria en nuestro medio. De forma similar a lo reportado en la literatura, las infecciones respiratorias bajas son de las patologías más frecuentes de aplicación de la procalcitonina como herramienta para tratar de distinguir etiología viral de bacteriana, así como para identificar las neumonías bacterémicas (4,5,10,11).
Los cultivos en general mostraron una tasa de positividad de 20% y en el caso de los hemocultivos de 17%, lo que supera la tasa reportada a nivel mundial de 15% (12). En concordancia con el último reporte del GREBO (13), los gérmenes Gram negativos son los principales aislamientos microbiológicos en las unidades de cuidado intensivo pediátrico, encabezando la lista Escherichia coli (12%), al igual que en el presente estudio con 21.8%.
En esta investigación, la tasa de contaminación fue del 5%, también dentro del rango esperado, siendo los cocos coagulasa negativos los contaminantes más frecuentes (12). Al igual que lo reportado en estudios previos (3,14,15), no se encontró relación de los valores de PCT y el tipo de agente microbiológico identificado en los cultivos. Puede pensarse que es más sensible para identificar gérmenes Gram negativos, pero dado que este grupo es el más aislado pude tratarse de un sesgo de confusión.
Respecto a las características operativas de la PCT para evaluar sepsis, y teniendo en cuenta los diferentes puntos de corte planteados en la literatura, se encontró que con valores menores de 0.5ng/ml se logran identificar a los pacientes con bajo riesgo de bacteremia, ya que se alcanza una sensibilidad del 76% y un VPN del 90% —valores que se encuentran dentro de los rangos reportados en la literatura— (3).
Por el contrario, valores mayores a 2ng/ml ayudan a identificar los pacientes con alto riesgo de bacteremia, ya que este punto de corte muestra una especificidad mayor (69%), manteniendo un VPN de 87%. Al evaluar la curva ROC de PCT como predictor de sepsis, se encuentra que los valores tienen el comportamiento esperado: a mayor valor de procalcitonina mayor su especificidad y menor su sensibilidad.
A pesar de que no todos los pacientes incluidos tenían medición de los otros biomarcadores, se pudo identificar que la PCR es uno de los más utilizados para evaluar infección. En general, la proteína C reactiva ha mostrado ser un buen marcador de seguimiento por su descenso lento ante el uso de antibióticos, pero con menor eficacia diagnóstica que la PCT (16,17). En este estudio, se encontró una correlación adecuada entre PCR y PCT, no solo de forma numérica sino en relación a sus puntos de corte, ya que el 100% de las PCR positivas se correlacionan con una PCT positiva. Sin embargo, cabe resaltar que igualmente se encontró que el 96% de las PCR toman valores positivos, independiente de si la PCT es negativa o positiva, lo que sugiere que, a pesar de la significancia, la correlación diagnóstica no es tan buena y que con los puntos de referencia del laboratorio la PCR tiene una alta tasa de falsos positivos que se ven reflejados en su alta sensibilidad pero con especificidad muy baja para este punto de corte.
Al comparar las características operativas de la PCT, PCR, conteo de leucocitos y neutrófilos con diferentes puntos de corte, se encontró que aumentan su especificidad a medida que aumenta su valor, sin embargo la PCT y PCR tienen valores de sensibilidad más altos, comparado con leucocitos y neutrófilos. De igual forma, al evaluar las curvas ROC de los cuatro biomarcadores como predictores de sepsis, se encontró que la PCT tiene mayor área bajo la curva con una diferencia significativa entre ellas, corroborando el mayor rendimiento de la PCT respecto a los demás reactantes, así como lo encontrado en la literatura (6,18,19).
En cuanto a las limitaciones de este estudio, pueden incluirse los sesgos de selección e información por su carácter retrospectivo. El amplio rango de edad de los pacientes incluidos también puede influir en los resultados, ya que el desempeño diagnóstico de la PCT puede variar según la edad y el tipo de patología.
Respecto al posible efecto que tiene el uso de antibiótico previo a la toma de las muestras, se encontró que la relación entre el resultado de la PCT y la positividad del hemocultivo se mantuvo en el grupo que recibió antibiótico previo, lo que puede sugerir que esta terapia afecta a ambas medidas de forma similar. En otros estudios se ha encontrado que la PCT disminuye rápidamente en respuesta a la terapia antibiótica, normalizándose a los 2 o 3 días, pero que puede mantenerse elevada en pacientes con infección no controlada, al igual que los hemocultivos (3,20). Sin embargo, este trabajo no pudo evaluar el comportamiento de la PCT en respuesta al antibiótico porque no se incluyeron mediciones de seguimiento.
Respecto a los otros cultivos —urocultivos, cultivo de LCR— no se contó con muestras suficientes para establecer las características operativas de la PCT para estos.
En conclusión, la PCT tiene un buen rendimiento diagnóstico como marcador de sepsis en niños hospitalizados en la Fundación HOMI, ya que por su mayor sensibilidad tiene más utilidad con valores negativos; también tiene un buen valor pronóstico al relacionarse con la mortalidad.
Conflicto de intereses
Ninguno declarado por los autores.
Financiación
Ninguna declarada por los autores.
Agradecimientos
Ninguno declarado por los autores.
Referencias
1. Correa-Velez JA. Fiebre en niños. Precop SCP. 2001 [cited 2015 Mar 18];1:17-31. Available from: https://goo.gl/29ZarI.
2. Hsiao AL, Baker MD. Fever in the new millennium: a review of recent studies of markers of serious bacterial infection in febrile children. Curr. Opin Pediatr. 2005;17(1):56-61.
http://doi.org/c782nk.
3. Chan T, Gu F. Early diagnosis of sepsis using serum biomarkers. Expert. Rev. Mol. Diagn. 2011;11(5):487-96.
http://doi.org/ch8tdt.
4. Van Rossum AM, Wulkan RW, Oudesluys-Murphy AM. Procalcitonin as an early marker of infection in neonates and children. Lancet. Infect. Dis. 2004;4(10):620-30. http://doi.org/dkzpfc.
5. Pacifico L, Osborn JF, Natale F, Ferraro F, De Curtis M, Chiesa C. Procalcitonin in pediatrics. Adv. Clin. Chem. 2013;59:203-63. http://doi.org/bdhj.
6. Irwin AD, Carrol ED. Procalcitonin. Arch. Dis. Child. Educ. Pract. Ed. 2011;96(6):228-33. http://doi.org/bkkcnh.
7. Dubos F, Korczowski B, Aygun DA, Martinot A, Prat C, Galetto-Lacour A, et al. Serum Procalcitonin Level and Other Biological Markers to Distinguish Between Bacterial and Aseptic Meningitis in Children: a European multicenter case cohort study. Arch. Pediatr. Adolesc. Med. 2008;162(12):1157-63.
http://doi.org/fcdmdj.
8. Nikfar R, Khotaee G, Ataee N, Shams S. Usefulness of procalcitonin rapid test for the diagnosis of acute pyelonephritis in children in the emergency department. Pediatr. Int. 2010;52(2):196-8. http://doi.org/fchhwx.
9. Obuchowski NA. Sample size calculations in studies of test accuracy. Stat. Methods Med. Res. 1998;7(4):371-92. http://doi.org/d7f5cr.
10. Don M, Valent F, Korppi M, Canciani M. Differentiation of bacterial and viral community-acquired pneumonia in children. Pediatr. Int. 2009;51(1):91-6. http://doi.org/fgkhtm.
11. Khan DA, Rahman A, Khan FA. Is procalcitonin better than C-reactive protein for early diagnosis of bacterial pneumonia in children? J. Clin. Lab. Anal. 2010;24(1):1-5. http://doi.org/dnrw27.
12. Doern G. Blood cultures for the detection of bacteremia. UpToDate; 2009 [updated 2015 Nov 03; cited 2016 Mar 18]. Available from: http://goo.gl/RUcgwe.
13. Grupo para el control de la resistencia bacteriana de Bogotá. Análisis de la vigilancia de la resistencia bacteriana año 2013. Componente pediátrico y adulto. Bol Inf GREBO. Bogotá, Colombia; 2014 [cited 2016 Mar 3];(6):40.3-8 Available from: http://goo.gl/zPrjdv.
14. Fleischhack G, Cipic D, Juettner J, Hasan C, Bode U. Procalcitonin-a sensitive inflammation marker of febrile episodes in neutropenic children with cancer. Intensive Care Med. 2000;26 (Suppl 2):S202-11. http://doi.org/ch53cm.
15. Sakr Y, Sponholz C, Tuche F, Brunkhorst F, Reinhart K. The role of procalcitonin in febrile neutropenic patients: review of the literature. Infection. 2008;36(5):396-407. http://doi.org/fk8378.
16. Alqahtani MF, Marsillio LE, Rozenfeld RA. A review of biomarkers and physiomarkers in pediatric sepsis. Clin. Pediatr. Emerg. Med. 2014;15(2):177-84. http://doi.org/bdhm.
17. Celik IH, Demirel FG, Uras N, Oguz SS, Erdeve O, Biyikli Z, et al. What are the cut-off levels for IL-6 and CRP in neonatal sepsis? J. Clin. Lab. Anal. 2010;24(6):407–12. http://doi.org/cmsb9m.
18. Kaplan JM, Wong HR. Biomarker discovery and development in pediatric critical care medicine. Pediatr. Crit. Care. Med. 2011 Mar [cited 2014 Oct 7];12(2):165–73. http://doi.org/bfsq39.
19. Smith K, Bigham MT. Biomarkers in Pediatric Sepsis. The Open Inflammation Journal. 2011;24-30. http://doi.org/cf2ghk.
20. Galetto-Lacour A, Zamora SA, Gervaix A. Bedside Procalcitonin and C-Reactive Protein Tests in Children With Fever Without Localizing Signs of Infection Seen in a Referral Center. Pediatrics. 2003 [cited 2012 Nov 4];112(5):1054-60. Available from: http://goo.gl/FDdOFM.
Ingrid Yoryeth Bastidas Pedreros
“Ejercicios de ilustración anatómica”
Universidad Nacional de Colombia
Referencias
Correa-Velez JA. Fiebre en niños. Precop SCP. 2001 [cited 2015 Mar 18];1:17-31. Available from: https://goo.gl/29ZarI.
Hsiao AL, Baker MD. Fever in the new millennium: a review of recent studies of markers of serious bacterial infection in febrile children. Curr. Opin Pediatr. 2005;17(1):56-61. http://doi.org/c782nk.
Chan T, Gu F. Early diagnosis of sepsis using serum biomarkers. Expert. Rev. Mol. Diagn. 2011;11(5):487-96. http://doi.org/ch8tdt.
Van Rossum AM, Wulkan RW, Oudesluys-Murphy AM. Procalcitonin as an early marker of infection in neonates and children. Lancet. Infect. Dis. 2004;4(10):620-30. http://doi.org/dkzpfc.
Pacifico L, Osborn JF, Natale F, Ferraro F, De Curtis M, Chiesa C. Procalcitonin in pediatrics. Adv. Clin. Chem. 2013;59:203-63. http://doi.org/bdhj.
Irwin AD, Carrol ED. Procalcitonin. Arch. Dis. Child. Educ. Pract. Ed. 2011;96(6):228-33. http://doi.org/bkkcnh.
Dubos F, Korczowski B, Aygun DA, Martinot A, Prat C, Galetto-Lacour A, et al. Serum Procalcitonin Level and Other Biological Markers to Distinguish Between Bacterial and Aseptic Meningitis in Children: a European multicenter case cohort study. Arch. Pediatr. Adolesc. Med. 2008;162(12):1157-63. http://doi.org/fcdmdj.
Nikfar R, Khotaee G, Ataee N, Shams S. Usefulness of procalcitonin rapid test for the diagnosis of acute pyelonephritis in children in the emergency department. Pediatr. Int. 2010;52(2):196-8. http://doi.org/fchhwx.
Obuchowski NA. Sample size calculations in studies of test accuracy. Stat. Methods Med. Res. 1998;7(4):371-92. http://doi.org/d7f5cr.
Don M, Valent F, Korppi M, Canciani M. Differentiation of bacterial and viral community-acquired pneumonia in children. Pediatr. Int. 2009;51(1):91-6. http://doi.org/fgkhtm.
Khan DA, Rahman A, Khan FA. Is procalcitonin better than C-reactive protein for early diagnosis of bacterial pneumonia in children? J. Clin. Lab. Anal. 2010;24(1):1-5. http://doi.org/dnrw27.
Doern G. Blood cultures for the detection of bacteremia. UpToDate; 2009 [updated 2015 Nov 03; cited 2016 Mar 18]. Available from: http://goo.gl/RUcgwe.
Grupo para el control de la resistencia bacteriana de Bogotá. Análisis de la vigilancia de la resistencia bacteriana año 2013. Componente pediátrico y adulto. Bol Inf GREBO. Bogotá, Colombia; 2014 [cited 2016 Mar 3];(6):40.3-8 Available from: http://goo.gl/zPrjdv.
Fleischhack G, Cipic D, Juettner J, Hasan C, Bode U. Procalcitonin-a sensitive inflammation marker of febrile episodes in neutropenic children with cancer. Intensive Care Med. 2000;26 (Suppl 2):S202-11. http://doi.org/ch53cm.
Sakr Y, Sponholz C, Tuche F, Brunkhorst F, Reinhart K. The role of procalcitonin in febrile neutropenic patients: review of the literature. Infection. 2008;36(5):396-407. http://doi.org/fk8378.
Alqahtani MF, Marsillio LE, Rozenfeld RA. A review of biomarkers and physiomarkers in pediatric sepsis. Clin. Pediatr. Emerg. Med. 2014;15(2):177-84. http://doi.org/bdhm.
Celik IH, Demirel FG, Uras N, Oguz SS, Erdeve O, Biyikli Z, et al. What are the cut-off levels for IL-6 and CRP in neonatal sepsis? J. Clin. Lab. Anal. 2010;24(6):407-12. http://doi.org/cmsb9m.
Kaplan JM, Wong HR. Biomarker discovery and development in pediatric critical care medicine. Pediatr. Crit. Care. Med. 2011 Mar [cited 2014 Oct 7];12(2):165-73. http://doi.org/bfsq39.
Smith K, Bigham MT. Biomarkers in Pediatric Sepsis. The Open Inflammation Journal. 2011;24-30. http://doi.org/cf2ghk.
Galetto-Lacour A, Zamora SA, Gervaix A. Bedside Procalcitonin and C-Reactive Protein Tests in Children With Fever Without Localizing Signs of Infection Seen in a Referral Center. Pediatrics. 2003 [cited 2012 Nov 4];112(5):1054-60. Available from: http://goo.gl/FDdOFM.
Cómo citar
APA
ACM
ACS
ABNT
Chicago
Harvard
IEEE
MLA
Turabian
Vancouver
Descargar cita
CrossRef Cited-by
1. Paola Andrea Yasnó-Navia, Luisa Fernanda Zuñiga-Ceron, Jhan Sebastián Saavedra-Torres, María Virginia Pinzón-Fernández. (2019). Endotoxins and the importance of procalcitonin. Revista de la Facultad de Medicina, 67(1), p.169. https://doi.org/10.15446/revfacmed.v67n1.69593.
Dimensions
PlumX
Visitas a la página del resumen del artículo
Descargas
Licencia
Derechos de autor 2016 Revista de la Facultad de Medicina

Esta obra está bajo una licencia Creative Commons Reconocimiento 3.0 Unported.
-





















