Prescripción del ejercicio físico y sus implicaciones en adultos que han sufrido quemaduras
Prescription of physical activity and its implications in adults who have experienced burns
DOI:
https://doi.org/10.15446/revfacmed.v67n1.66776Palabras clave:
Enfermedades de la piel, Modalidades de fisioterapia, Ejercicio (es)Skin Diseases, Physical Therapy Modalities, Exercise (en)
Introducción. La prescripción del ejercicio físico y sus implicaciones en pacientes que han sufrido quemaduras es objeto de estudio en diferentes investigaciones debido al impacto físico, psicológico y social que tiene en las personas.
Objetivo. Describir la prescripción de ejercicio físico y sus implicaciones en la población adulta que ha sufrido quemaduras.
Materiales y métodos. Se realizó una revisión de tema por medio de exploración de artículos de manera electrónica con filtros de búsqueda en distintas bases de datos con términos DeCS y MeSH.
Resultados. Se seleccionaron 11 artículos con intervención de ejercicio físico en fases aguda y crónica. Se incluyeron estrategias sobre la fuerza muscular en cinco de los artículos: tres de resistencia cardiovascular; dos de rango de movimiento, flexibilidad y características tróficas de la piel, y uno de dolor.
Conclusiones. Las variables de la prescripción se determinan de acuerdo a las características propias que presenta la persona con quemadura, las cuales se resumen en esta revisión.
Introduction: The prescription of physical activity and its implications in patients who have suffered burns is the object of study of different investigations due to the physical, psychological and social impact they have on people.
Objective: To describe the prescription of physical activity and its implications in adults with burn injury.
Materials and methods: A review of the topic was carried out by scanning articles electronically and using search filters in different databases with DeCS and MeSH terms.
Results: 11 articles about physical activity intervention in acute and chronic phases were selected. Strategies on muscle strength were included in six of the articles: three on cardiovascular resistance; two on range of motion, flexibility and trophic features of the skin; and one on pain.
Conclusions: The variables of the prescription are determined according to the characteristics of the person with the burn, which are summarized in this review.
Artículo de revisión
DOI: https://doi.org/10.15446/revfacmed.v67n1.66776
Prescripción del ejercicio físico y sus implicaciones en adultos que han sufrido quemaduras
Prescription of physical activity and its implications in adults who have experienced burns
Recibido: 01/08/2017. Aceptado: 24/10/2017.
Paula Andrea Betancourt-Cárdenas1 • Nubia Esperanza Camargo-Caldas1 • Diego Fabricio Rodríguez-Camacho1,2 • Estefanía Lozano-Rivera1 • Juan Felipe Correa3
1 Universidad de la Sabana - Facultad de Enfermería y Rehabilitación - Programa de Fisioterapia - Chía - Colombia.
2 Escuela Militar de Cadetes General José María Córdoba - Grupo de investigación RENFIMIL - Bogotá D.C. - Colombia.
3 Universidad Nacional de Colombia - Sede Bogotá - Facultad de Medicina - Departamento del Movimiento Corporal Humano - Grupo de Investigación de Análisis Mecánico y Neuromecánico del Movimiento Corporal Humano - Bogotá D.C. - Colombia.
Correspondencia: Diego Fabricio Rodríguez-Camacho. Grupo de investigación RENFIMIL, Escuela Militar de Cadetes General José María Córdoba. Calle 80 No. 30.00. Teléfono: +57 1 3770850. Bogotá D.C. Colombia. Correo electrónico: diegorodcam@unisabana.edu.co.
| Resumen |
Introducción. La prescripción del ejercicio físico y sus implicaciones en pacientes que han sufrido quemaduras es objeto de estudio en diferentes investigaciones debido al impacto físico, psicológico y social que tiene en las personas.
Objetivo. Describir la prescripción de ejercicio físico y sus implicaciones en la población adulta que ha sufrido quemaduras.
Materiales y métodos. Se realizó una revisión de tema por medio de exploración de artículos de manera electrónica con filtros de búsqueda en distintas bases de datos con términos DeCS y MeSH.
Resultados. Se seleccionaron 11 artículos con intervención de ejercicio físico en fases aguda y crónica. Se incluyeron estrategias sobre la fuerza muscular en cinco de los artículos: tres de resistencia cardiovascular; dos de rango de movimiento, flexibilidad y características tróficas de la piel, y uno de dolor.
Conclusiones. Las variables de la prescripción se determinan de acuerdo a las características propias que presenta la persona con quemadura, las cuales se resumen en esta revisión.
Palabras clave: Enfermedades de la piel; Modalidades de fisioterapia; Ejercicio (DeCS).
Betancourt-Cárdenas PA, Camargo-Caldas NE, Rodríguez-Camacho DF, Lozano-Rivera E, Correa JF. Prescripción del ejercicio físico y sus implicaciones en adultos que han sufrido quemaduras. Rev. Fac. Med. 2019;67(1):135-43. Spanish. doi: https://doi.org/10.15446/revfacmed.v67n1.66776.
| Abstract |
Introduction: The prescription of physical activity and its implications in patients who have suffered burns is the object of study of different investigations due to the physical, psychological and social impact they have on people.
Objective: To describe the prescription of physical activity and its implications in adults with burn injury.
Materials and methods: A review of the topic was carried out by scanning articles electronically and using search filters in different databases with DeCS and MeSH terms.
Results: 11 articles about physical activity intervention in acute and chronic phases were selected. Strategies on muscle strength were included in six of the articles: three on cardiovascular resistance; two on range of motion, flexibility and trophic features of the skin; and one on pain.
Conclusions: The variables of the prescription are determined according to the characteristics of the person with the burn, which are summarized in this review.
Keywords: Skin Diseases; Physical Therapy Modalities; Exercise (MeSH).
Betancourt-Cárdenas PA, Camargo-Caldas NE, Rodríguez-Camacho DF, Lozano-Rivera E, Correa JF. [Prescription of physical activity and its implications in adults who have experienced burns]. Rev. Fac. Med. 2019;67(1):135-43. Spanish. doi: https://doi.org/10.15446/revfacmed.v67n1.66776.
Introducción
La Organización Mundial de la Salud refiere que “las quemaduras constituyen un problema de salud pública a nivel mundial y provocan alrededor de 180 000 muertes al año, de las cuales la mayoría se produce en los países de ingresos económicos bajos y medios, y casi la mitad, en la región de Asia Sudoriental” (1). Además, esta lesión constituye una de las principales causas de morbilidad con diversos factores en la evolución de la patología como cambios morfofisiológicos, hospitalización prolongada y discapacidad, teniendo gran impacto sobre el rol social de la persona (2). Las quemaduras se encuentran entre las principales causas de años de vida ajustados por discapacidad (AVISA) perdidos en los países de ingresos bajos y medios.
En 2008 se produjeron más de 410 000 lesiones por quemaduras en EE. UU.; cerca de 40 000 requirieron hospitalización. En Bangladesh, Colombia, Egipto y Pakistán el 17% de los niños con quemaduras tiene una discapacidad temporal y el 18% tiene una discapacidad permanente (1). También en Colombia, durante el 2014, se hospitalizaron 402 pacientes quemados provenientes de 12 departamentos del país, 234 (58.2%) hombres y 168 (41.8%) mujeres, con edades de entre 6 días y 83 años. Las quemaduras comprometían entre el 1% y el 80% de la superficie corporal; el 95.5% de los pacientes tenían vinculación con el Sistema General de Seguridad Social Nacional. Los agentes causales incluyeron líquidos calientes (52.5%), fuego (10.0%), gasolina (9.2%), electricidad (7.5%), químicos (3.7%), entre otros, y produjeron quemaduras de segundo y tercer grado (3).
Por otro lado, las quemaduras severas causan secuelas físicas como cicatrices a largo plazo, amputación de alguna extremidad, secuelas estéticas y cambios en el color de la piel y en los perímetros del cuerpo, lo que desencadena como resultado afectaciones psicológicas relacionadas a cambios en la apariencia, disminución de la autoestima, inconformidad social, sentimientos de amenaza, ansiedad acerca del futuro y alteración de la imagen corporal (4,5).
Las quemaduras presentan una respuesta inflamatoria caracterizada por un periodo de estrés, inflamación e hipercatabolismo debido a una respuesta circulatoria hiperdinámica (6), la cual incluye respuesta mediada por citoquinas como factor de necrosis tumoral alfa (FNT) e interleucinas (IL); estas últimas guardan relación estrecha con los queratinocitos apoptóticos y activan la respuesta inmune (7). La vasoconstricción inicial se encuentra mediada por el tromboxano A2, de tal manera que se disminuye el flujo sanguíneo y luego se produce una vasodilatación a causa de los mediadores prostaglandina I2, prostaglandina E2, bradicinina e histamina, con lo que se aumenta la permeabilidad capilar (7,8).
De la misma forma, se presenta disminución de la función inmunológica (6,9,10) debido a deficiencias en la activación de macrófagos y linfocitos, lo que genera una respuesta inflamatoria que se relaciona con la pérdida de la función inmunológica de la piel (11).
La piel, que es el órgano de mayor extensión del cuerpo humano (6), sufre alteraciones en tres zonas histológicamente marcadas: la zona de coagulación o necrosis irreversible, en la cual se detectan cambios en los vasos sanguíneos, células epiteliales, mesenquimales y destrucción del colágeno asociado a la formación de edema (12); la zona de estasis, donde se presenta daño microvascular y la cual, según la evolución, puede convertirse en zona de coagulación o hiperemia, siendo esta la zona más exterior que representa la fuga capilar y extravasación sanguínea (Figura 1); estos cambios histológicos se ven de acuerdo a la profundidad de la lesión (6,13).
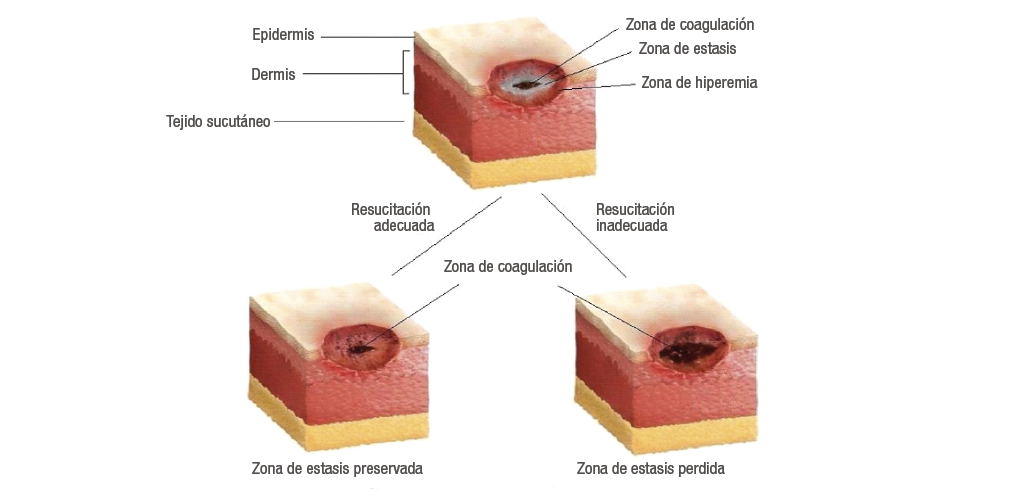
Figura 1. Zonas histológicas de la quemadura.
Fuente: Elaboración con base en Held et al. (12)
El almacenamiento de grasa, la regulación de temperatura y fluidos, el equilibrio electrolítico y la protección inmunológica se encuentran alteradas por los cambios fisiológicos, la elasticidad y la viscoelasticidad de la piel, además los melanocitos se regeneran lentamente y provocan variación en la coloración de la piel durante la recuperación de la quemadura (6,10).
Asimismo, se genera un aumento en la producción de glucagón, las reservas de glucógeno del músculo se dirigen al torrente sanguíneo y hay una pérdida de adenosín trifosfato que altera los puentes cruzados de miosina y actina (12), por esta razón y por el aumento del catabolismo del músculo hay una disminución de la masa corporal magra y de la capacidad oxidativa (11). Esto produce un incremento del consumo de oxígeno y del gasto energético e hiperglicemia sobre la persona con quemadura (14).
La tasa metabólica basal aumenta hasta tres veces su velocidad original; esto, junto con la hipoperfusión esplácnica, hace necesaria una alimentación enteral temprana y agresiva para disminuir el catabolismo y mantener la integridad intestinal (15). La tasa metabólica basal varía según los niveles en el tamaño de la quemadura: los valores en reposo en las quemaduras leves son menos del 10%, siendo niveles casi normales, sin embargo estas tasas se duplican rápidamente en quemaduras que exceden el 40% durante la admisión aguda (16).
Ahora bien, la respuesta hipermetabólica es el resultado de una serie de eventos desencadenados por un aumento significativo y persistente de las secreciones de catecolamina, cortisol, glucagón y dopamina (17). De hecho, la respuesta metabólica también se ve afectada de manera crónica, inclusive alterando el metabolismo de la glucosa hasta tres años después del accidente inicial. La lista de estos mediadores incluye interleucinas (IL) 1 y 6, factor activador de plaquetas (FAP), factor de necrosis tisular (TNF), especies reactivas de oxigeno (ROS) y cascadas de complemento. Por lo tanto, se ha encontrado que estas regulaciones metabólicas pueden ocurrir en dos fases: temprana y tardía. La fase temprana comienza inmediatamente después de una lesión térmica, tiene una duración de tres días con un estado hipometabólico característico asociado con circulación hipodinámica, disminución del consumo de oxígeno e hiperglucemia; estas variables más tarde comienzan a aumentar hasta alcanzar la fase tardía, la cual tiene una duración de hasta un año (18).
En la literatura reciente se ha evidenciado que un programa de ejercicio estructurado compuesto de entrenamiento oxidativo y resistencia muscular conduce a una mejora en cuanto la función y la funcionalidad (19,20). Asimismo, las personas que han realizado ejercicio requieren menos intervenciones quirúrgicas hasta dos años después de la rehabilitación, en comparación con un grupo control (20-22).
De esta manera, el ejercicio físico logra cambios que contrarrestan los efectos de la atrofia muscular y la inactividad, que están relacionados de forma directa con la lesión por quemadura (23,24). Además, algunos autores reportan que las tasas de supervivencia después de una quemadura grave han mejorado significativamente, lo que destaca la importancia de la rehabilitación a partir de la recuperación de las capacidades físicas básicas como lo son el aumento de 8.2 grados del rango de movimiento por semana y el aumento del 61% en la fuerza muscular medida en dinamometría. De igual manera, en la funcionalidad hay mejoras significativas según escalas validadas de actividades de la vida diaria en adultos quemados con respecto a grupos controles (25-27).
Sin embargo, aunque en la literatura se encuentran los efectos positivos del ejercicio físico sobre las personas que han sufrido quemadura, no son claros los parámetros de prescripción del ejercicio para dicha población. Estos parámetros deben contemplar la estructuración del programa de ejercicio en cuanto a tipo, intensidad, frecuencia, duración, densidad, ritmo de progresión y aplicación en el tipo de quemadura (28). Por lo tanto, la presente revisión pretende determinar cuáles son las implicaciones de la prescripción del ejercicio físico en la población adulta que ha sufrido quemadura.
Materiales y métodos
El estudio realizado es una revisión de tema, la cual busca indagar el estado del arte sobre las implicaciones de la prescripción de ejercicio físico en población adulta que ha sufrido quemaduras (29). Se incluyeron fuentes primarias de información a partir de la búsqueda de artículos originales de tipo experimental publicados en revistas académicas indexadas entre enero de 2012 y abril de 2017. La búsqueda se hizo en las bases de datos PubMed, ScienceDirect, LILACS, Proquest, Ovid, PEDro y Scopus a partir del uso de los descriptores DeCS y MeSH, unidos por los operadores boléanos AND y OR. Las fórmulas de búsqueda fueron [Burns AND Rehabilitation] OR [Adult AND Burns] AND [Exercise] [Burns AND Rehabilitation] OR [Exercise] y el recurso utilizado en la búsqueda fue la expresión “término exacto”.
Los criterios de inclusión fueron artículos que propusieran intervención en rehabilitación en adultos que sufrieron quemadura con intervención de ejercicio físico y su prescripción y estudios de tipo experimental. Los criterios de exclusión fueron intervención dirigida en animales, editoriales, libros, textos no evaluados por pares, estudios de tipo descriptivo y correlacional, investigaciones con fechas anteriores a enero del 2012 y estudios en menores de edad (Figura 2).
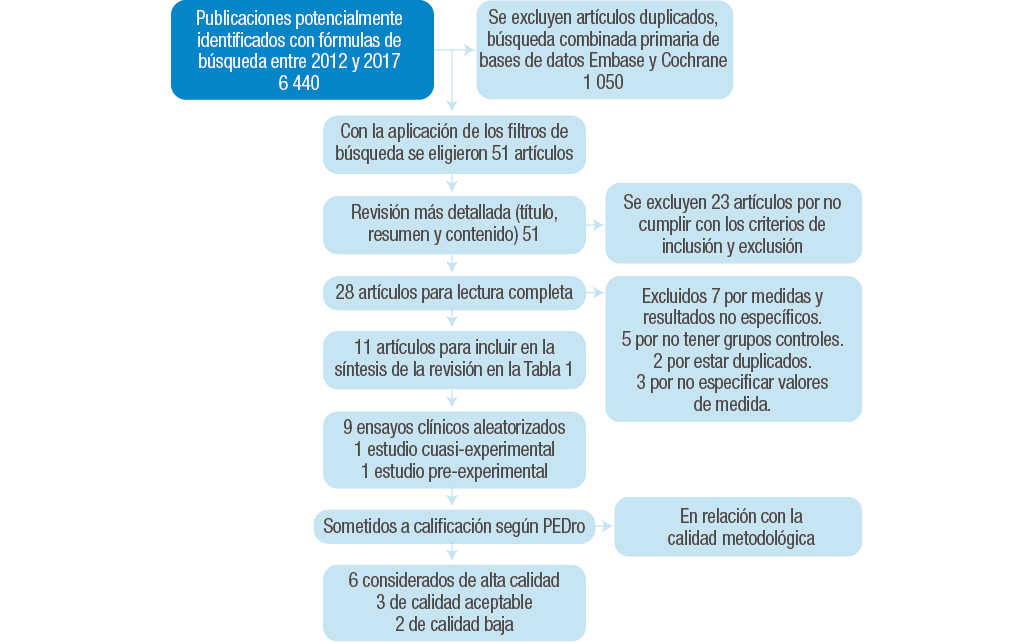
Figura 2. Diagrama de flujo de la selección de estudios.
Fuente: Elaboración propia.
Los estudios conformantes de la tabla de características de los estudios y evaluación y calidad metodológica fueron seleccionados según la escala de PEDro, la cual se basa en la calidad metodológica para la clasificación de los estudios: baja con una puntuación de 1 a 2, aceptable de 3 a 5 y alta de 6 a 10. La última modificación de la escala PEDro se realizó el 21 de junio de 1999 y la traducción al español finalizó el 30 de diciembre de 2012 (30).
Una de las limitaciones de esta revisión son los pocos estudios que cumplieron con los criterios de inclusión, lo que indica la necesidad de una mayor investigación en este campo de conocimiento. La mayoría de estos estudios tuvieron doble ciego y en los seleccionados los tratamientos y las medidas fueron variadas, lo que dificultó el análisis y la interpretación de los mismos.
Los estudios arrojados después del algoritmo (Tabla 1) no fueron analizados por jurados expertos independientes, sino por los mismos autores, lo que puede ser un sesgo en el momento de la selección adecuada de los artículos. Sin embargo, las ecuaciones de búsqueda y los criterios de inclusión y exclusión hacen que aumente la rigurosidad de los estudios analizados en esta revisión de tema.
Resultados
Después de realizar la búsqueda en las bases de datos, se identificaron
6 440 artículos de acuerdo con las fórmulas de búsqueda y el filtro
por fechas comprendidas entre enero de 2012 y abril de 2017. Luego se eliminaron artículos duplicados, donde se identificaron
1 050 artículos a través de la búsqueda combinada primaria de bases de datos Embase y Cochrane. Después de aplicar el filtro de las fórmulas de búsqueda se eligieron 51 artículos, de los cuales se leyó el resumen y el contenido para emplear los criterios de inclusión y exclusión, eligiendo 11 artículos de texto completo, los cuales fueron organizados en un formato que incluyó los parámetros autor, fecha de publicación, muestra, fase de la quemadura, superficie corporal total afectada, intervención y resultados de
la intervención.
Clasificación de los estudios seleccionados
De los estudios que fueron incluidos en esta revisión, nueve son ensayos clínicos aleatorizados, uno es un estudio cuasiexperimental y el otro es un estudio preexperimental. En relación con la calidad metodológica, seis son de alta calidad, tres de calidad aceptable y dos de baja calidad, según la clasificación PEDro (30).
Las intervenciones propuestas por los diferentes autores incluyeron estrategias sobre la fuerza muscular en cinco de los artículos, tres de resistencia cardiovascular, dos de rango de movimiento, flexibilidad y características tróficas de la piel y uno de dolor (Tabla 1) (23,31-40).
Tabla 1. Características de los estudios y evaluación de la calidad metodológica.
|
Estudio |
Muestra |
Fase |
Superficie corporal total quemada |
Intervención |
Resultados |
Clasificación PEDro |
|
Ebid et al. (23) 2012 |
Hombres y mujeres de 18 a 35 años n=20 control n=20 experimental Quemaduras de 2° y 3° grado No especifican cuántos hombres y cuántas mujeres |
Agudo |
35-55% |
Grupo experimental: Duración: 12 semanas Frecuencia: 3 semanas Ejercicios isocinéticos concéntricos al 60% con velocidad angular de 150° s1 con 3 minutos de descanso entre series. Grupo control: Terapia convencional |
Hubo diferencia significativa en fuerza de extensores de rodilla p<0.05 Grupo control: 66.45±9.3 Grupo experimental: 78.94±8.5 Flexores de rodilla p<0.05 Grupo control: 59.88±10.47 Grupo experimental: 66.4±6.85 Evaluación de la fuerza en newton por medio de dinamometría |
7/10 Calidad alta |
|
Grisbrook et al. (31) 2012 |
n=9 control (8 hombres y 1 mujer, edad: 38.67±9.07) n=9 experimental (8 hombres y 1 mujer, edad: 39±8.51) |
Crónico |
Al menos 20% |
Duración: 12 semanas Frecuencia: 3 sesiones/semana y 80 minutos/sesión - caminata en banda 30 minutos Intensidad: 65-70% de frecuencia cardiaca máxima. Se incrementó la intensidad cada semana |
El pico de VO2, ventilación minuto máxima y prueba de esfuerzo mejoró de forma significativa en ambos grupos, medido con ergoespirómetro Grupo control p<0.05. 31.97±6.95 pretest 38.08±5.90 postest. Grupo experimental p<0.05. 31.73±6.70 pretest 36.75±7.16 postest |
5/10 Calidad aceptable |
|
Ebid et al. (32) 2012 |
Adultos de 36 a 40 años con quemaduras de 2° y 3° grado en miembros inferiores n=15 grupo control (10 hombres 5 mujeres) n=16 grupo experimental (10 hombres 6 mujeres) |
Aguda |
36-45% |
Duración: 8 semanas Grupo de ejercicio: marcha, estiramientos, deambulación funcional, fuerza y resistencia Grupo de vibración: caminata 4 km/3 min, vibración 10 minutos/30 Hz, sentadillas 5 series/3 repeticiones/semana Metodología: ensayo clínico controlado aleatorizado. |
Aumento significativo de fuerza en extensores de rodilla Grupo control p>0.05. 168.40±5.06 pretest 190.07±3.99 postest Grupo experimental 168.47±5.43 pretest 233.40±5.74 postest Plantiflexores en ambos grupos p>0.05 Grupo control 101.40±1.45 pretest 116.13±3.24 postest El aumento de pico de torque de plantiflexores fue mayor en el grupo de vibración |
6/10 Calidad alta |
|
Grisbrook et al. (33). 2013 |
Adultos quemados y adultos sanos entre 24 y 55 años n=9 control (8 hombres 1 mujer) n=9 experimental (8 hombres 1 mujer) |
Crónico |
>20% |
Duración: 12 semanas Frecuencia: 3 sesiones/semana Duración: 80 minutos/sesión Modo: entrenamiento con Biodex Intensidad inicial: 50 al 60% de fuerza en 3 series de 10-15 repeticiones con progreso a pesas |
Todos los participantes completaron una serie de concéntricos isocinéticos Hubo aumento significativo en la fuerza de los grupos musculares del tren superior e inferior intragrupo, no hubo diferencia significativa entre los resultados de los dos grupos Flexión de hombro intragrupo p>0.03, entre grupos p>0.123 Extensión de hombro intragrupo p>0.020, entre grupos p>0.098 Flexión de codo intragrupo p>0.008, entre grupos p>0.108 Extensión de codo intragrupo p>0.004, entre grupos p>0.139 Flexión de cadera intragrupo p>0.001, entre grupos p>0.144 Extensión de cadera intragrupo p>0.064 entre grupos p>0.460 |
5/10 Calidad aceptable |
|
Godleski et al. (34) 2013 |
Adultos que requieren injertos de piel (n=9) n=6 hombres n=3 mujeres Edad entre 22 y 63 años |
Agudo |
10-50% |
Duración: 4 semanas Tipo: flexibilidad Modo: estiramiento pasivo desde rango submáximo y aumento progresivo Frecuencia: 1 sesión diaria en menos de 3 minutos Duración:30 min/sesión |
Hubo cambios significativos p<0.05 (no especifican el intervalo de confianza) en el rango de movilidad articular (medidos en grados de mejora en promedio por semana) durante las primeras cuatro semanas; el promedio de aumento por semana fue: Flexión de hombro: 10.1° Codo flexión: 2.6° Muñeca flexión: 4.6° Cadera flexión: 9.4° Rodilla extensión 5.3° |
3/10 Calidad pobre |
|
Sarı et al. (35) 2014 |
Quemaduras de 2° y 3° grado. Edades entre 24 y 55 años n=8 hombres n=4 mujeres |
Agudo |
No especifica |
Valoración pre y post Duración: 3 semanas Frecuencia: 5 días/semana Tipo: Flexibilidad, fuerza Modo: Hidromasaje: 15 minutos Ritmo matriz: 15-45 minutos Ejercicios de rango de movimiento activo y pasivo 15 minutos Ejercicios de estiramiento y fortalecimiento Facilitación neuromuscular propioceptiva: 15 minutos |
El uso de tratamiento de ritmo matriz señaló mejora en los grados de movimiento activos p>0.03 con valor z=-2.934, mejora en grados de movimiento pasivos p>0.05 con valor z=-2.803 No hubo diferencia significativa en los valores de dolor, fuerza muscular (dinamómetro) y flexibilidad (milímetros) |
3/10 Calidad pobre |
|
Ali et al. (36) 2015 |
Quemaduras de 2° grado Años grupo control: 29.5±6.6 Años grupo experimental: 27.9±7.3 n=15 control n=15 experimental No especifican género |
Agudo |
20-40% |
Grupo intervención: Duración: 12 semanas Modo: ejercicio en banda Frecuencia: 3 sesiones/semana Duración: 20 a 40 minutos Intensidad: 70-85% del VO2 máx. Grupo control: Terapia convencional |
Hubo diferencias estadísticamente significativas entre VO2 máx (ergoespirómetro) y tiempo en la caminadora en ambos grupos. El VO2 (ml/m/kg) en el grupo control pretest fue 22.4±1.9 y postest 25.8±2, p>0.05, y en el grupo de estudio 21.8±2.3 y 33.9±3.8, respectivamente, p>0.05 El tiempo de caminadora en el grupo control fue 10.9±1.7 pretest y 13.8±1.2 postest y en el grupo de estudio 11.1±1.8 pretest y 18.7±1.8 postest, Ambos grupos tuvieron valor p<0.001 |
7/10 Calidad alta |
|
Parker et al. (37) 2016 |
Personas que han sufrido quemaduras con rango de edad de 16 a 59 años. n=10 control (3 mujeres y 7 hombres) n=12 intervención (4 mujeres y 8 hombres) |
Agudo |
<10% |
Grupo intervención: Duración: 7 días Modo: Sesiones de Nintendo Wii más terapia convencional Frecuencia: 2 veces/día Duración: 20-30 minutos/sesión Grupo control: Terapia convencional |
La diferencia a nivel grupal en las puntuaciones de dolor registradas antes y después de cada sesión de ejercicio mostró una mejoría estadísticamente significativa en el grupo de intervención: IC95%: 0.584-0.298, p=0.019 |
6/10 Calidad alta |
|
Grisbrook et al. (38) 2017 |
Personas con quemaduras en edades entre 19 y 50 años n=10 control (9 hombres y 1 mujer) n=10 experimental (9 hombres y 1 mujer) |
Agudo |
6-40%, media de 16% |
Grupo resistencia: Duración: 4 semanas Frecuencia: 3 veces/semana Calentamiento: 10 minutos con cicloergómetro Tipo: ejercicio de resistencia Intensidad: 3 series de 8-12 repeticiones al 70% de su contracción isométrica voluntaria máxima diaria para miembros superiores e inferiores. Grupo control: Misma duración, tipo, frecuencia y calentamiento. Intensidad: 3 series de 10 repeticiones con resistencia de 1kg en MMSS y 10kg en MMII, tiempo de descanso entre series no definido |
El grupo de ejercicios, el volumen de sesión y el dolor antes del ejercicio influyeron independientemente en la carga de entrenamiento. Por cada kilogramo de aumento en el volumen de sesión hubo un aumento de 0.01 en la carga de entrenamiento (p=0.026). Por cada aumento de un punto en el dolor antes del ejercicio hubo un aumento de 11.88 puntos en la carga de entrenamiento (p=0.007) |
7/10 Calidad alta |
|
Paratz et al. (39) 2012 |
Adultos con quemaduras Edad promedio en grupo control de 42.64±14.6 años y en grupo experimental de 30.4±10.1. n=14 control (10 hombres y 4 mujeres) n=16 experimental (15 hombres y 1 mujer) |
crónico |
42.9% (±13.3%) |
Se realizó un diseño cuasi experimental después del injerto final Ambos grupos completaron el estiramiento y el grupo de intervención se sometió a un programa combinado de ejercicios aeróbicos o de resistencia de alta intensidad (80% de frecuencia cardíaca máxima y 70% de tres repeticiones) durante seis semanas Se tomaron medidas de resultado al inicio, a las seis semanas y a los tres meses por medio de ergoespirómetro |
El grupo de estudio tuvo una diferencia significativa en el pico de VO2 (L/min) con respecto al grupo control a las seis semanas (p=0.04) y a los tres meses (p=0.006). |
5/10 Calidad aceptable |
|
Cho et al. (40) 2014 |
Cicatrices hipertróficas posterior a quemadura (n=146) n=70 control (50 hombres y 20 mujeres) n=76 experimental (61 hombres y 15 mujeres) Edad promedio grupo control: 47.21 años Edad promedio grupo experimental: 46.06 años |
Crónico |
Media de 37.2% |
Grupo control: Terapia estándar: ejercicios de amplitud de movimiento, aplicación de gel de silicona y terapia de presión. Grupo intervención con masaje: Frecuencia: 3 veces/semana Duración: 30 minutos/sesión Modo: effleurage, fricción y amasamiento Metodología: ensayo clínico controlado aleatorizado |
En ambos grupos se encontraron diferencias significativas en la escala análoga verbal y escala de picazón, sin embargo hubo una diferencia significativa en el grupo experimental ajustada al grupo control, en cuanto a que la escala análoga verbal tuvo puntaje de 1.36 (0.69-2.02), p<0.001, y la escala de picazón de 0.38 (0.01-0.75), p=0.04. |
6/10 Calidad alta |
Fuente: Elaboración propia.
Discusión
En relación con los programas de entrenamiento encontrados en la revisión, la fase preparatoria tuvo una duración de 5 a 10 minutos de calentamiento (23,31,32,35,36), resultados que son acordes con los propuestos por el American Collage of Sports Medicine (ACSM), que recomienda esta duración debido a que facilita la transición del reposo a la actividad, aumenta el flujo sanguíneo, eleva la temperatura corporal y favorece la tasa metabólica (38) y la activación del sistema de suministro de fuentes energéticas (41).
En cuanto a los estudios que han evaluado la eficacia de programas de entrenamiento de fuerza muscular a través del ejercicio isocinético, la información recopilada recomienda una duración de entre 8 y 12 semanas. Con este tiempo se generan adaptaciones neurales asociadas a mejoras en el aprendizaje motor, la sincronización intramuscular, la coordinación intermuscular, el aumento de los impulsos nerviosos transmitidos hacia las unidades motoras y la función muscular (23,24,42).
Estos hallazgos están asociados con intervenciones que tras un programa de entrenamiento de ocho semanas producen aumento en la fuerza dinámica sin producir cambios significativos en la fibra muscular, pues durante las primeras semanas de entrenamiento se originan adaptaciones neurales que permiten cambios en la proteína muscular y los entrenamientos de mayor duración producen hipertrofia muscular (43-45). Cabe mencionar que la variable de duración entre los programas de ejercicio físico enfocado al aumento de la fuerza muscular difiere entre autores debido a la diversidad en el tamaño de las muestras, la superficie corporal total afectada, la duración de estancia hospitalaria, la edad, el enfoque de entrenamiento de la fuerza y la etiología de la quemadura (23).
En relación con las intensidades propuestas en los artículos seleccionados para esta revisión, las cuales van del 50% al 70% de la fuerza, hay que anotar que el ACSM recomienda de forma semejante que los programas enfocados a fuerza muscular deben iniciarse a partir del 60% de la resistencia máxima y para principiantes a partir del 50% (28). Sin embargo, Jiang et al. (42) afirman que una baja intensidad combinada con alto nivel de esfuerzo mental puede aumentar significativamente la fuerza; esto es un dato de gran valor clínico, sobre todo para la población que ha sufrido quemaduras ya que en muchas ocasiones tiene dificultades para practicar ejercicios de alta intensidad debido a la proteólisis muscular producida por el estado catabólico característico de esta lesión (24,42). Con referencia a lo anterior, Grisbrook et al. (38) realizan una comparación de la carga de trabajo en relación con el dolor, encontrando que el aumento de este se asocia con mayor intensidad del entrenamiento.
Por otro lado, la frecuencia de un programa de entrenamiento de fuerza aplicado tres veces a la semana se asocia directamente con lo propuesto por López-Chicharro & López-Mojares (46), quienes recomiendan la misma frecuencia para tener periodos de descanso de 48 horas entre sesiones; esta es recomendada para grupos musculares individuales y pretende alcanzar adaptaciones neurales en primera instancia, seguidas de adaptaciones producidas por hipertrofia (46,47).
El trabajo con fuentes energéticas oxidativas se contempla como un componente importante en los programas de rehabilitación, ya que se ha encontrado relación de las fuentes oxidativas sobre el estado funcional, no solo en personas con lesión por quemadura sino también en personas con diferentes condiciones de salud (36,48). Por lo tanto, se ha estudiado la aplicación de programas de entrenamiento asociados con el trabajo de fuentes oxidativas en diferentes etapas de la lesión por quemadura (31).
En cuanto a la prescripción del ejercicio, Grisbrook et al. (31) plantean en estadio crónico un programa de ejercicio de intervalo sumado a ejercicios de resistencia, mientras que Ali et al. (36) en pacientes con quemadura aguda sugieren la aplicación de un programa de resistencia cardiovascular, además de ejercicios de respiración diafragmática. Esta diferencia está relacionada con el impacto del estado hipermetabólico, que si bien disminuye con el tiempo, los autores refieren que es una respuesta que permanece hasta dos años después de la quemadura.
Los autores que proponen un entrenamiento de intervalo en personas que han sufrido quemadura en estadio crónico indican este ejercicio por medio de intervalos medianos entre 60% y 80% del VO2 máximo con duración de entre 2 y 7 minutos, que pretende soportar trabajos a elevadas intensidades con objetivos funcionales y efectos como el metabolismo del glucógeno y mejora de la capacidad de fuentes energéticas oxidativas, favoreciendo a su vez el aumento y resistencia cardiovascular, lo que intensifica la tasa metabólica (36,49,50).
Al aumentase la intensidad del ejercicio, los pulmones sanos responden a la acidosis por la bomba de protones que se genera en la contracción muscular, aumentando aún más la ventilación minuto, lo que disminuye el CO2 arterial y mantiene el pH de la sangre a niveles normales. Además, el ejercicio basado en el trabajo con fuentes oxidativas mejora la función respiratoria y produce un aumento en el volumen sistólico del corazón por el efecto del ejercicio regular. Estas adaptaciones respiratorias facilitan el suministro de oxígeno y nutrientes a los tejidos y con esto se logra una mayor eficiencia en cuanto a la función de los tejidos afectados (31,36).
En lo que respecta a flexibilidad, el tamaño de las muestras entre los dos artículos incluidos difiere en cantidad; sin embargo, en general los sujetos mostraron una mejoría significativa en el rango de movimiento. Estos resultados se correlacionan con los encontrados por Zhang et al. (51), quienes comparan diferentes intervenciones de estiramiento mecánico en personas con quemaduras y resaltan intervenciones enfocadas en el estiramiento analítico, así como las diferentes técnicas de masaje, encontrando que ambas tienen resultados positivos en cuanto a la mejora del rango de movimiento y en cuanto a las propiedades mecánicas de las cicatrices posteriores al trauma.
Godleski et al. (34) sugieren que los estiramientos deben ser intensos, una hora diaria en las áreas activas de la contractura, y comentan que estos pueden no ser factibles en todos los planos de movimiento por heridas resultantes de la quemadura o por vendaje bultoso. No obstante, esto difiere de lo sugerido por Schmitt et al. (52), quienes en un estudio con niños con quemaduras concluyen que los estiramientos deben darse en todos los planos de movimiento de la articulación involucrada, iniciando de forma lenta y de proximal a distal. Ambas investigaciones utilizan estiramientos estáticos pasivos con duración mínima de tres minutos por cada grupo muscular (34,52). Asimismo, en la revisión de Ayala et al. (53) se realizó una comparación entre los diferentes métodos de intervención para mejorar la flexibilidad y el rango de movimiento, encontrando que todas las técnicas incluidas tienen cambios significativos sobre la flexibilidad.
Por su parte, Cho et al. (40) destacan el uso de masaje como complemento a los estiramientos, pues si bien ambos grupos de intervención mejoraron de forma significativa, el grupo que además incluyó masaje mejoró las características propias de la piel. Estos datos son comparables con los obtenidos por Schneider et al. (54), quienes afirman que con este tipo de intervención no solo se obtienen mejorías en rango de movimiento, sino incluso en la funcionalidad del segmento.
Schmitt et al. (52) y Omar et al. (55) describen que adicional a los estiramientos es indispensable realizar ejercicios combinados de flexibilidad, destacando el movimiento de piel, mediante el masaje en esta población (40,51). Cabe anotar que han surgido intervenciones como la propuesta por Parker et al. (37) con estrategias para aumentar el rango de movimiento, las cuales involucran el uso de tecnología; sin embargo, este estudio no mostró resultados significativos en cuanto al aumento del rango de movimiento, pero sí disminución de dolor.
De acuerdo con lo anterior, mediante el uso de la consola Nintendo Wii en juegos individuales con 20 a 30 minutos 5 días a la semana, Parker et al. (37) demostraron disminuciones significativas del dolor y disminución de la ansiedad por dolor. De forma similar, Parry et al. (56) muestran en su investigación disminución del dolor con el uso de videojuegos por medio del uso de kinect en el transcurso de un mes, con una frecuencia de 2 veces a la semana; allí se obtiene como producto final el reintegro de los sujetos a sus actividades de la vida diaria y a sus tareas funcionales.
Conclusiones
Las personas que han sufrido quemaduras presentan alteraciones morfológicas, fisiológicas, psicológicas y sociales asociadas a las características propias de la lesión, en donde el manejo por parte de un equipo interdisciplinario, del cual hace parte el fisioterapeuta, busca generar cambios positivos sobre la persona para disminuir las limitaciones funcionales y en sus capacidades físicas básicas.
En relación con la prescripción del ejercicio físico, se concluye que variables como el modo, la frecuencia, la intensidad y la duración están determinadas a partir de las características de la población en relación con la etiología de la quemadura, la superficie corporal total quemada, el grado de la quemadura, el estadio de recuperación y las deficiencias funcionales, lo cual debe tenerse en cuenta para programas de entrenamiento.
Se requiere, por un lado, de al menos 8 a 12 semanas de duración de los programas de entrenamiento en fuerza muscular de personas con quemaduras para generar adaptaciones neurales y, por el otro, un programa mayor a 12 semanas para producir cambios o adaptaciones relacionadas a hipertrofia muscular, siendo más funcional las adaptaciones generadas en las primeras semanas, ya que mediante las adaptaciones neurales se mejora la función muscular.
El método de entrenamiento para mejorar la resistencia cardiovascular implica que en las primeras semanas se trabaje por medio de ejercicio de resistencia y que 6 meses posteriores a la quemadura el entrenamiento sea por medio de ejercicio de intervalos, ya que estos programas de entrenamiento generan resultados en la resistencia cardiovascular tras 12 semanas, independiente de la fase de la quemadura en la que se encuentre la persona.
En lo referente al rango de movimiento, la literatura reportó que tanto los estiramientos musculares como el masaje generan resultados estadísticamente significativos, aunque en cuanto a la duración de los estiramientos no se ha definido un tiempo específico ya que todos los tipos de estiramiento propuestos en la literatura han logrado mejorías, sin embargo se recomiendan estiramientos combinados con otro tipo de técnicas complementarias.
Por último, el presente estudio resume las variables más importantes a tener en cuenta para la prescripción del ejercicio en el paciente con quemaduras, así como sus beneficios en las capacidades físicas básicas y en su funcionalidad, logrando un consenso en la literatura y en la práctica de la fisioterapia. No obstante, se requieren más estudios experimentales en este campo del conocimiento.
Conflicto de intereses
Ninguno declarado por los autores.
Financiación
Ninguna declarada por los autores.
Agradecimientos
A la Universidad de la Sabana por contribuir al acceso en bases de datos y obtención de los artículos utilizados para la presente revisión y al Grupo de Investigación de Movimiento Corporal Humano de la Facultad de Enfermería y Rehabilitación del programa de Fisioterapia de la Universidad de la Sabana por su apoyo y orientación durante el proceso de investigación.
Referencias
1.Burns. Geneve: World Health Organization; 2018 [cited 2018 May 13]. Available from: https://goo.gl/zjSyus.
2.Porter C, Hardee JP, Herndon DN, Suman OE. The role of exercise in the rehabilitation of patients with severe burns. Exerc Sport Sci Rev. 2015;43(1):34-40. http://doi.org/cw94.
3.Ramírez-Blanco CE, Ramírez-Rivero CE, Díaz-Martínez LA. Causas y sobrevida en pacientes quemados en el centro de referencia del nororiente de Colombia. Cir plást iberolatinoam. 2017;43(1):59-67.
4.Wasiak J, Lee SJ, Paul E, Shen A, Tan H, Cleland H, et al. Female patients display poorer burn-specific quality of life 12 months after a burn injury. Injury. 2017;48(1):87-93. http://doi.org/f9jcj2.
5.Caltran MP, Freitas NO, Dantas RA, Farina JA, Rossi LA. Satisfaction With Appearance Scale-SWAP: Adaptation and validation for Brazilian burn victims. Burns. 2016;42(6):1331-9. http://doi.org/gdxv2g.
6.Townsend CM, Beauchamp RD, Evers BM, Mattox KL. Sabiston. Tratado de cirugía: fundamentos biológicos de la práctica quirúrgica moderna. 18th ed. Madrid: Elsevier; 2009.
7.Gragnani A, Cezillo MV, da Silva ID, de Noronha SM, Correa-Noronha SA, Ferreira LM. Gene expression profile of cytokines and receptors of inflammation from cultured keratinocytes of burned patients. Burns. 2014;40(5):947-56. http://doi.org/f59zx3.
8.Coert JH. Pathophysiology of nerve regeneration and nerve reconstruction in burned patients. Burns. 2010;36(5):593-8. http://doi.org/d6psf3.
9.Rodríguez-Acosta M, González-Plana G. Respuesta Inmunitaria en el Paciente Quemado. Rev Cub Med Milit. 2001;30(Suppl 5):56-62.
10.Ramírez CE, Ramírez-Blanco CE, González LF, Ramírez N, Vélez K. Fisiopatología del paciente quemado. Rev Salud UIS. 2010 [cited 2018 Nov 11];42(1). Available from: https://goo.gl/7YDF6W.
11.Huang G, Liang B, Liu G, Liu K, Ding Z. Low dose of glucocorticoid decreases the incidence of complications in severely burned patients by attenuating systemic inflammation. J Crit Care. 2015;30(2):436.e7-11. http://doi.org/f27rfq.
12.Held M, Rahmanian-Schwarz A, Rothenberger J, Schiefer J, Janghorban-Esfahani B, Schaller HE, et al. Alteration of biomechanical properties of burned skin. Burns. 2015;41(4):789-95. http://doi.org/f7cxhx.
13.Goutos I, Tyler M. Early management of paediatric burn injuries. Paediatr Child Health. 2013;23(9):391-6. http://doi.org/cw96.
14.Nielson CB, Duethman NC, Howard JM, Moncure M, Wood JG. Burns: Pathophysiology of Systemic Complications and Current Management. J Burn Care Res. 2017;38(1):e469-81. http://doi.org/f9k77d.
15.Hettiaratchy S, Dziewulski P. Pathophysiology and types of burns. BMJ. 2004;328(7453):1427-9. http://doi.org/dbmx45.
16.Kaddoura I, Abu-Sittah G, Ibrahim A, Karamanoukian R, Papazian N. Burn injury: review of pathophysiology and therapeutic modalities in major burns. Ann Burns Fire Disasters. 2017;30(2):95-102.
17.Guillory AN, Porter C, Suman OE, Zapata-Sirvent RL, Finnerty CC, Herndon DN. Modulation of the Hypermetabolic Response after Burn Injury. In: Herndon DN, editor. Total Burn Care. Elsevier; 2018 [cited 2018 No 22]. Available from: https://goo.gl/57yWVv.
18.Jeschke MG, Chinkes DL, Finnerty CC, Kulp G, Suman OE, Norbury WB, et al. Pathophysiologic Response to Severe Burn Injury. Am Surg. 2008;248(3):387-401. http://doi.org/cbpq2h.
19.Grisbrook TL, Reid SL, Edgar DW, Wallman KE, Wood FM, Elliott CM. Exercise training to improve health related quality of life in long term survivors of major burn injury: A matched controlled study. Burns. 2012;38(8):1165-73. http://doi.org/f4gbkh.
20.Stoddard FJ, Ryan CM, Schneider JC. Physical and psychiatric recovery from burns. Surg Clin North Am. 2014;94(4):863-78. http://doi.org/f6f7pj.
21.Saeman MR, DeSpain K, Liu MM, Carlson BA, Song J, Baer LA, et al. Effects of exercise on soleus in severe burn and muscle disuse atrophy. J Surg Res. 2015;198(1):19-26. http://doi.org/f7qjv8.
22.De Lateur BJ, Magyar-Russell G, Bresnick MG, Bernier FA, Ober MS, Krabak BJ, et al. Augmented Exercise in the Treatment of Deconditioning From Major Burn Injury. Arch Phys Med Rehabil. 2007;88(12 Suppl 2):S18-23. http://doi.org/d3dbnj.
23.Ebid AA, Omar MT, Abd-El Baky AM. Effect of 12-week isokinetic training on muscle strength in adult with healed thermal burn. Burns. 2012;38(1):61-8. http://doi.org/cs49t2.
24.Ebid AA, El-Shamy SM, Draz AH. Effect of isokinetic training on muscle strength, size and gait after healed pediatric burn: A randomized controlled study. Burns. 2014;40(1):97-105. http://doi.org/brvw.
25.Cronan T, Hammond J, Ward CG. The value of isokinetic exercise and testing in burn rehabilitation and determination of back-to-work status. J Burn Care Rehabil. 1990;11(3):224-7. http://doi.org/d4krfb.
26.Tang D, Li-Tsang CWP, Au RKC, Li K, Yi X, Liao L, et al. Functional Outcomes of Burn Patients With or Without Rehabilitation in Mainland China. Hong Kong J Occup Ther. 2015;26(1):15-23. http://doi.org/cw97.
27.Wolf SE, Phelan HA, Arnoldo BD. The year in burns 2013. Burns. 2014;40(8):1421-32. http://doi.org/f6rhkj.
28.Lopategui-Corsino E. Prescripción de Ejercicio - delineamientos más recientes. American College of Sports Medicine; 2012 [cited 2018 Nov 22]. Available from: https://goo.gl/KqsJ7r.
29.Merino-Trujillo A. Como escribir documentos científicos (Parte 3). Artículo de revisión. Salud en Tabasco. 2011;17(1-2):36-40.
30.Escala PEDro. Sídney: Physiotherapy Evidence Database PEDro; 2012 [cited 2018 May 14]. Available from: https://goo.gl/bi4my2.
31.Grisbrook TL, Wallman KE, Elliott CM, Wood FM, Edgar DW, Reid SL. The effect of exercise training on pulmonary function and aerobic capacity in adults with burn. Burns. 2012;38(4):607-13. http://doi.org/cw99.
32.Ebid AA, Ahmed MT, Mahmoud Eid M, Mohamed MS. Effect of whole body vibration on leg muscle strength after healed burns: A randomized controlled trial. Burns. 2012;38(7):1019-26. http://doi.org/f4cr4z.
33.Grisbrook TL, Elliott CM, Edgar DW, Wallman KE, Wood FM, Reid SL. Burn-injured adults with long term functional impairments demonstrate the same response to resistance training as uninjured controls. Burns. 2013;39(4):680-6. http://doi.org/f42w33.
34.Godleski M, Oeffling A, Bruflat AK, Craig E, Weitzenkamp D, Lindberg G. Treating Burn-Associated Joint Contracture: Results of an Inpatient Rehabilitation Stretching Protocol. J Burn Care Res. 2013;34(4):420-6. http://doi.org/f5q26c.
35.Sarı Z, Polat MG, Özgül B, Aydoğdu O, Camcıoğlu B, Acar AH, et al. The application of matrix rhythm therapy as a new clinical modality in burn physiotherapy programmes. Burns. 2014;40(5):909-14. http://doi.org/f59rcg.
36.Ali ZM, El-Refay BH, Ali RR. Aerobic exercise training in modulation of aerobic physical fitness and balance of burned patients. J Phys Ther Sci. 2015;27(3):585-9. http://doi.org/cxbb.
37.Parker M, Delahunty B, Heberlein N, Devenish N, Wood FM, Jackson T, et al. Interactive gaming consoles reduced pain during acute minor burn rehabilitation: A randomized, pilot trial. Burns. 2016;42(1):91-6. http://doi.org/cxbc.
38.Grisbrook TL, Gittings PM, Wood FM, Edgar DW. The effectiveness of session rating of perceived exertion to monitor resistance training load in acute burns patients. Burns. 2017;43(1):169-75. http://doi.org/f9k6c3.
39.Paratz JD, Stockton K, Plaza A, Muller M, Boots RJ. Intensive exercise after thermal injury improves physical, functional, and psychological outcomes: J Trauma Acute Care Surg. 2012;73(1):186-94. http://doi.org/cxs3.
40.Cho YS, Jeon JH, Hong A, Yang HT, Yim H, Cho YS, et al. The effect of burn rehabilitation massage therapy on hypertrophic scar after burn: A randomized controlled trial. Burns. 2014;40(8):1513-20. http://doi.org/f6q8v4.
41.Platonov VN. Teoría general del entrenamiento deportivo. Barcelona: Paidotribo; 2001.
42.Jiang CH, Ranganathan VK, Siemionow V, Yue GH. The level of effort, rather than muscle exercise intensity determines strength gain following a six-week training. Life Sci. 2017;178:30-4. http://doi.org/gbh8t6.
43.Baechle TR, Earle RW. Principios del entrenamiento de la fuerza y del acondicionamiento físico. 2nd ed. Madrid: Editorial Médica Panamericana; 2007.
44.Heyward VH. Evaluación de la aptitud física y prescripción del ejercicio. 5th ed. Madrid: Editorial Médica Panamericana; 2008.
45.Sánchez-Blanco I, Ferrero-Médez A, Aguilar-Naranjo JJ, Climent-Barerá JM, Conejero-Casares JA, Flórez-García MT, et al. Manual SERMEF de rehabilitación y medicina física. Madrid: Editorial Médica Panamericana; 2008.
46.López-Chicharro J, López-Mojares LM. Fisiología Clínica del ejercicio. Madrid: Editorial Médica Panamericana; 2008.
47.Ortíz-Cervera V. Entrenamiento de fuerza y explosividad para la actividad física y el deporte de competición. 2nd ed. Barcelona: Inde Publicaciones; 1999.
48.Ambrosy AP, Cerbin LP, DeVore AD, Greene SJ, Kraus WE, O’Connor CM, et al. Aerobic exercise training and general health status in ambulatory heart failure patients with a reduced ejection fraction-Findings from the Heart Failure and A Controlled Trial Investigating Outcomes of Exercise Training (HF-ACTION)trial. Am Heart J. 2017;186:130-8. http://doi.org/cxbd.
49.Hernández C. Manual práctico para el entrenamiento. Bloomington: Palibrio; 2012.
50.Wilber K, Patten T, Leonard A, Morelli M. La práctica integral de la vida. Programa orientado al desarrollo de la salud física, el equilibrio emocional, la lucidez mental y el despertar espiritual del ser humano del siglo XXI. 2nd ed. Barcelona: Editorial Kairós; 2010.
51.Zhang Y, Li-Tsang CWP, Au RKC. A Systematic Review on the Effect of Mechanical Stretch on Hypertrophic Scars after Burn Injuries. Hong Kong J Occup Ther. 2017;29(1):1-9. http://doi.org/cxbf.
52.Schmitt YS, Hoffman HG, Blough DK, Patterson DR, Jensen MP, Soltani M, et al. A randomized, controlled trial of immersive virtual reality analgesia, during physical therapy for pediatric burns. Burns. 2011;37(1):61-8. http://doi.org/bndr3v.
53.Ayala F, Sainz-de Baranda P, Cejudo A. El entrenamiento de la flexibilidad: técnicas de estiramiento. Rev Andal Med Deporte. 2012;
5(3):83-121.
54.Schneider JC, Qu HD, Lowry J, Walker J, Vitale E, Zona M. Efficacy of inpatient burn rehabilitation: A prospective pilot study examining range of motion, hand function and balance. Burns. 2012;38(2):164-71. http://doi.org/cz4gqz.
55.Omar MT, Hegazy FA, Mokashi SP. Influences of purposeful activity versus rote exercise on improving pain and hand function in pediatric burn. Burns. 2012;38(2):261-8. http://doi.org/bdxjbv.
56.Parry I, Carbullido C, Kawada J, Bagley A, Sen S, Greenhalgh D, et al. Keeping up with video game technology: Objective analysis of Xbox KinectTM and PlayStation 3 MoveTM for use in burn rehabilitation. Burns. 2014;40(5):852-9. http://doi.org/f593k4.

Claude Bernard (1813-1878)
“Précis iconographique de médicine operatoire
et d´anatomie chirurgicale”
Referencias
Burns. Geneve: World Health Organization; 2018 [cited 2018 May 13]. Available from: https://goo.gl/zjSyus.
Porter C, Hardee JP, Herndon DN, Suman OE. The role of exercise in the rehabilitation of patients with severe burns. Exerc Sport Sci Rev. 2015;43(1):34-40. http://doi.org/cw94.
Ramírez-Blanco CE, Ramírez-Rivero CE, Díaz-Martínez LA. Causas y sobrevida en pacientes quemados en el centro de referencia del nororiente de Colombia. Cir plást iberolatinoam. 2017;43(1):59-67.
Wasiak J, Lee SJ, Paul E, Shen A, Tan H, Cleland H, et al. Female patients display poorer burn-specific quality of life 12 months after a burn injury. Injury. 2017;48(1):87-93. http://doi.org/f9jcj2.
Caltran MP, Freitas NO, Dantas RA, Farina JA, Rossi LA. Satisfaction With Appearance Scale-SWAP: Adaptation and validation for Brazilian burn victims. Burns. 2016;42(6):1331-9. http://doi.org/gdxv2g.
Townsend CM, Beauchamp RD, Evers BM, Mattox KL. Sabiston. Tratado de cirugía: fundamentos biológicos de la práctica quirúrgica moderna. 18th ed. Madrid: Elsevier; 2009.
Gragnani A, Cezillo MV, da Silva ID, de Noronha SM, Correa-Noronha SA, Ferreira LM. Gene expression profile of cytokines and receptors of inflammation from cultured keratinocytes of burned patients. Burns. 2014;40(5):947-56. http://doi.org/f59zx3.
Coert JH. Pathophysiology of nerve regeneration and nerve reconstruction in burned patients. Burns. 2010;36(5):593-8. http://doi.org/d6psf3.
Rodríguez-Acosta M, González-Plana G. Respuesta Inmunitaria en el Paciente Quemado. Rev Cub Med Milit. 2001;30(Suppl 5):56-62.
Ramírez CE, Ramírez-Blanco CE, González LF, Ramírez N, Vélez K. Fisiopatología del paciente quemado. Rev Salud UIS. 2010 [cited 2018 Nov 11];42(1). Available from: https://goo.gl/7YDF6W.
Huang G, Liang B, Liu G, Liu K, Ding Z. Low dose of glucocorticoid decreases the incidence of complications in severely burned patients by attenuating systemic inflammation. J Crit Care. 2015;30(2):436.e7-11. http://doi.org/f27rfq.
Held M, Rahmanian-Schwarz A, Rothenberger J, Schiefer J, Janghorban-Esfahani B, Schaller HE, et al. Alteration of biomechanical properties of burned skin. Burns. 2015;41(4):789-95. http://doi.org/f7cxhx.
Goutos I, Tyler M. Early management of paediatric burn injuries. Paediatr Child Health. 2013;23(9):391-6. http://doi.org/cw96.
Nielson CB, Duethman NC, Howard JM, Moncure M, Wood JG. Burns: Pathophysiology of Systemic Complications and Current Management. J Burn Care Res. 2017;38(1):e469-81. http://doi.org/f9k77d.
Hettiaratchy S, Dziewulski P. Pathophysiology and types of burns. BMJ. 2004;328(7453):1427-9. http://doi.org/dbmx45.
Kaddoura I, Abu-Sittah G, Ibrahim A, Karamanoukian R, Papazian N. Burn injury: review of pathophysiology and therapeutic modalities in major burns. Ann Burns Fire Disasters. 2017;30(2):95-102.
Guillory AN, Porter C, Suman OE, Zapata-Sirvent RL, Finnerty CC, Herndon DN. Modulation of the Hypermetabolic Response after Burn Injury. In: Herndon DN, editor. Total Burn Care. Elsevier; 2018 [cited 2018 No 22]. Available from: https://goo.gl/57yWVv.
Jeschke MG, Chinkes DL, Finnerty CC, Kulp G, Suman OE, Norbury WB, et al. Pathophysiologic Response to Severe Burn Injury. Am Surg. 2008;248(3):387-401. http://doi.org/cbpq2h.
Grisbrook TL, Reid SL, Edgar DW, Wallman KE, Wood FM, Elliott CM. Exercise training to improve health related quality of life in long term survivors of major burn injury: A matched controlled study. Burns. 2012;38(8):1165-73. http://doi.org/f4gbkh.
Stoddard FJ, Ryan CM, Schneider JC. Physical and psychiatric recovery from burns. Surg Clin North Am. 2014;94(4):863-78. http://doi.org/f6f7pj.
Saeman MR, DeSpain K, Liu MM, Carlson BA, Song J, Baer LA, et al. Effects of exercise on soleus in severe burn and muscle disuse atrophy. J Surg Res. 2015;198(1):19-26. http://doi.org/f7qjv8.
De Lateur BJ, Magyar-Russell G, Bresnick MG, Bernier FA, Ober MS, Krabak BJ, et al. Augmented Exercise in the Treatment of Deconditioning From Major Burn Injury. Arch Phys Med Rehabil. 2007;88(12 Suppl 2):S18-23. http://doi.org/d3dbnj.
Ebid AA, Omar MT, Abd-El Baky AM. Effect of 12-week isokinetic training on muscle strength in adult with healed thermal burn. Burns. 2012;38(1):61-8. http://doi.org/cs49t2.
Ebid AA, El-Shamy SM, Draz AH. Effect of isokinetic training on muscle strength, size and gait after healed pediatric burn: A randomized controlled study. Burns. 2014;40(1):97-105. http://doi.org/brvw.
Cronan T, Hammond J, Ward CG. The value of isokinetic exercise and testing in burn rehabilitation and determination of back-to-work status. J Burn Care Rehabil. 1990;11(3):224-7. http://doi.org/d4krfb.
Tang D, Li-Tsang CWP, Au RKC, Li K, Yi X, Liao L, et al. Functional Outcomes of Burn Patients With or Without Rehabilitation in Mainland China. Hong Kong J Occup Ther. 2015;26(1):15-23. http://doi.org/cw97.
Wolf SE, Phelan HA, Arnoldo BD. The year in burns 2013. Burns. 2014;40(8):1421-32. http://doi.org/f6rhkj.
Lopategui-Corsino E. Prescripción de Ejercicio - delineamientos más recientes. American College of Sports Medicine; 2012 [cited 2018 Nov 22]. Available from: https://goo.gl/KqsJ7r.
Merino-Trujillo A. Como escribir documentos científicos (Parte 3). Artículo de revisión. Salud en Tabasco. 2011;17(1-2):36-40.
Escala PEDro. Sídney: Physiotherapy Evidence Database PEDro; 2012 [cited 2018 May 14]. Available from: https://goo.gl/bi4my2.
Grisbrook TL, Wallman KE, Elliott CM, Wood FM, Edgar DW, Reid SL. The effect of exercise training on pulmonary function and aerobic capacity in adults with burn. Burns. 2012;38(4):607-13. http://doi.org/cw99.
Ebid AA, Ahmed MT, Mahmoud Eid M, Mohamed MS. Effect of whole body vibration on leg muscle strength after healed burns: A randomized controlled trial. Burns. 2012;38(7):1019-26. http://doi.org/f4cr4z.
Grisbrook TL, Elliott CM, Edgar DW, Wallman KE, Wood FM, Reid SL. Burn-injured adults with long term functional impairments demonstrate the same response to resistance training as uninjured controls. Burns. 2013;39(4):680-6. http://doi.org/f42w33.
Godleski M, Oeffling A, Bruflat AK, Craig E, Weitzenkamp D, Lindberg G. Treating Burn-Associated Joint Contracture: Results of an Inpatient Rehabilitation Stretching Protocol. J Burn Care Res. 2013;34(4):420-6. http://doi.org/f5q26c.
Sarı Z, Polat MG, Özgül B, Aydoğdu O, Camcıoğlu B, Acar AH, et al. The application of matrix rhythm therapy as a new clinical modality in burn physiotherapy programmes. Burns. 2014;40(5):909-14. http://doi.org/f59rcg.
Ali ZM, El-Refay BH, Ali RR. Aerobic exercise training in modulation of aerobic physical fitness and balance of burned patients. J Phys Ther Sci. 2015;27(3):585-9. http://doi.org/cxbb.
Parker M, Delahunty B, Heberlein N, Devenish N, Wood FM, Jackson T, et al. Interactive gaming consoles reduced pain during acute minor burn rehabilitation: A randomized, pilot trial. Burns. 2016;42(1):91-6. http://doi.org/cxbc.
Grisbrook TL, Gittings PM, Wood FM, Edgar DW. The effectiveness of session rating of perceived exertion to monitor resistance training load in acute burns patients. Burns. 2017;43(1):169-75. http://doi.org/f9k6c3.
Paratz JD, Stockton K, Plaza A, Muller M, Boots RJ. Intensive exercise after thermal injury improves physical, functional, and psychological outcomes: J Trauma Acute Care Surg. 2012;73(1):186-94. http://doi.org/cxs3.
Cho YS, Jeon JH, Hong A, Yang HT, Yim H, Cho YS, et al. The effect of burn rehabilitation massage therapy on hypertrophic scar after burn: A randomized controlled trial. Burns. 2014;40(8):1513-20. http://doi.org/f6q8v4.
Platonov VN. Teoría general del entrenamiento deportivo. Barcelona: Paidotribo; 2001.
Jiang CH, Ranganathan VK, Siemionow V, Yue GH. The level of effort, rather than muscle exercise intensity determines strength gain following a six-week training. Life Sci. 2017;178:30-4. http://doi.org/gbh8t6.
Baechle TR, Earle RW. Principios del entrenamiento de la fuerza y del acondicionamiento físico. 2nd ed. Madrid: Editorial Médica Panamericana; 2007.
Heyward VH. Evaluación de la aptitud física y prescripción del ejercicio. 5th ed. Madrid: Editorial Médica Panamericana; 2008.
Sánchez-Blanco I, Ferrero-Médez A, Aguilar-Naranjo JJ, Climent-Barerá JM, Conejero-Casares JA, Flórez-García MT, et al. Manual SERMEF de rehabilitación y medicina física. Madrid: Editorial Médica Panamericana; 2008.
López-Chicharro J, López-Mojares LM. Fisiología Clínica del ejercicio. Madrid: Editorial Médica Panamericana; 2008.
Ortíz-Cervera V. Entrenamiento de fuerza y explosividad para la actividad física y el deporte de competición. 2nd ed. Barcelona: Inde Publicaciones; 1999.
Ambrosy AP, Cerbin LP, DeVore AD, Greene SJ, Kraus WE, O’Connor CM, et al. Aerobic exercise training and general health status in ambulatory heart failure patients with a reduced ejection fraction-Findings from the Heart Failure and A Controlled Trial Investigating Outcomes of Exercise Training (HF-ACTION)trial. Am Heart J. 2017;186:130-8. http://doi.org/cxbd.
Hernández C. Manual práctico para el entrenamiento. Bloomington: Palibrio; 2012.
Wilber K, Patten T, Leonard A, Morelli M. La práctica integral de la vida. Programa orientado al desarrollo de la salud física, el equilibrio emocional, la lucidez mental y el despertar espiritual del ser humano del siglo XXI. 2nd ed. Barcelona: Editorial Kairós; 2010.
Zhang Y, Li-Tsang CWP, Au RKC. A Systematic Review on the Effect of Mechanical Stretch on Hypertrophic Scars after Burn Injuries. Hong Kong J Occup Ther. 2017;29(1):1-9. http://doi.org/cxbf.
Schmitt YS, Hoffman HG, Blough DK, Patterson DR, Jensen MP, Soltani M, et al. A randomized, controlled trial of immersive virtual reality analgesia, during physical therapy for pediatric burns. Burns. 2011;37(1):61-8. http://doi.org/bndr3v.
Ayala F, Sainz-de Baranda P, Cejudo A. El entrenamiento de la flexibilidad: técnicas de estiramiento. Rev Andal Med Deporte. 2012;5(3):83-121.
Schneider JC, Qu HD, Lowry J, Walker J, Vitale E, Zona M. Efficacy of inpatient burn rehabilitation: A prospective pilot study examining range of motion, hand function and balance. Burns. 2012;38(2):164-71. http://doi.org/cz4gqz.
Omar MT, Hegazy FA, Mokashi SP. Influences of purposeful activity versus rote exercise on improving pain and hand function in pediatric burn. Burns. 2012;38(2):261-8. http://doi.org/bdxjbv.
Parry I, Carbullido C, Kawada J, Bagley A, Sen S, Greenhalgh D, et al. Keeping up with video game technology: Objective analysis of Xbox KinectTM and PlayStation 3 MoveTM for use in burn rehabilitation. Burns. 2014;40(5):852-9. http://doi.org/f593k4.
Cómo citar
APA
ACM
ACS
ABNT
Chicago
Harvard
IEEE
MLA
Turabian
Vancouver
Descargar cita
CrossRef Cited-by
1. Laura Catalina Martínez Roa, Betty Astrid Velásquez Silva. (2025). Fisioterapia en quemaduras de tercer grado. Movimiento científico, 19(1), p.21. https://doi.org/10.33881/2011-7191.mtc.19103.
Dimensions
PlumX
Visitas a la página del resumen del artículo
Descargas
Licencia
Derechos de autor 2019 Revista de la Facultad de Medicina

Esta obra está bajo una licencia Creative Commons Reconocimiento 3.0 Unported.
-





















