Propiedades psicométricas del Índice de Bienestar General-5 de la Organización Mundial de la Salud en pacientes parcialmente edéntulos
Psychometric properties of the WHO-5 Well-being index in partially edentulous patients
DOI:
https://doi.org/10.15446/revfacmed.v64n4.52235Palabras clave:
Análisis factorial, Estudios de validación, Reproducibilidad de resultados, Depresión (es)Factor Analysis, Validation Studies, Reproducibility of Results, Depression (en)
Introducción. La medición de bienestar en pacientes odontológicos posibilita la detección temprana de alteraciones emocionales.
Objetivo. Evaluar las propiedades psicométricas del Índice de Bienestar General de la Organización Mundial de la Salud (WHO-5 WBI) en pacientes parcialmente edéntulos.
Materiales y métodos. Estudio de validación de escalas y pruebas diagnósticas sin patrón de referencia realizado en 105 pacientes de un servicio de implantología oral. Se aplicó el WHO-5 WBI antes de iniciar el tratamiento y se realizó análisis factorial exploratorio para determinar el número de factores que explicaban el constructo, confirmatorio para su validez y su consistencia interna con el coeficiente alfa de Cronbach y la omega de McDonald.
Resultados. El análisis factorial exploratorio mostró solución de un solo factor que dio cuenta del 56.17% de la varianza. El análisis confirmatorio mostró índices de ajuste X2=1120.516; gl=10, p=0.04; RCMEA=0.134 (IC90%: 0.056-0.217); ICA=0.992; ITL=0.983 y RCMR=0.61.
Conclusiones. El WHO-5 WBI mostró aceptable reproducibilidad, estructura factorial unidimensional y cuestionable validez de constructo.
Introduction: Measuring well-being in dental patients allows early detection of emotional disorders.
Objective: To evaluate the psychometric properties of the Wellbeing index by the World Health Organization (WHO-5 WBI) in partially edentulous patients.
Materials and methods: Scale validation study and diagnostic tests without reference standard performed in 105 patients treated at an oral implantology service. The WHO-5 WBI was applied before treatment and an exploratory factor analysis was performed to determine the amount of factors in the construct that confirmed its validity and internal consistency through Cronbach’s alpha and McDonald’s omega.
Results: The exploratory factor analysis showed a single factor solution that accounted for 56.17% of the variance. The confirmatory analysis showed adjustment indexes X2=1120.516; df=10, p=0.04; RMSEA=0.134 (90% CI: 0.056-0.217); CFI=0.992; TLI=0.983 and WRMR= 0.61.
Conclusions: The WHO-5 WBI showed acceptable reproducibility, one-dimensional factor structure and questionable construct validity.
INVESTIGACIÓN ORIGINAL
DOI: https://doi.org/10.15446/revfacmed.v64n4.52235
Propiedades psicométricas del Índice de Bienestar General-5
de la Organización Mundial de la Salud en pacientes
parcialmente edéntulos
Psychometric properties of the WHO-5 Well-being index in partially edentulous patients
Recibido: 31/07/2015. Aceptado: 29/09/2015.
Miguel Simancas-Pallares1 • Shyrley Díaz-Cárdenas2 • Paola Barbosa-Gómez1 • María Buendía-Vergara3, • Luisa Arévalo-Tovar3
1 Universidad de Cartagena - Facultad de Odontología - Departamento de Investigaciones - Cartagena - Colombia.
2 Universidad de Cartagena - Facultad de Odontología - Departamento de Odontología Preventiva y Social - Cartagena - Colombia.
3 Universidad de Cartagena - Facultad de Odontología - Departamento de Medicina Oral y Cirugía - Cartagena - Colombia.
Correspondencia: Miguel Simancas-Pallares. Departamento de Investigación, Facultad de Odontología, Universidad de Cartagena. Calle 30 No. 48-152, oficina 301. Teléfono: +57 5 6698172, ext.: 110. Cartagena. Colombia. Correo electrónico: msimancasp@unicartagena.edu.co.
| Resumen |
Introducción. La medición de bienestar en pacientes odontológicos posibilita la detección temprana de alteraciones emocionales.
Objetivo. Evaluar las propiedades psicométricas del Índice de Bienestar General de la Organización Mundial de la Salud (WHO-5 WBI) en pacientes parcialmente edéntulos.
Materiales y métodos. Estudio de validación de escalas y pruebas diagnósticas sin patrón de referencia realizado en 105 pacientes de un servicio de implantología oral. Se aplicó el WHO-5 WBI antes de iniciar el tratamiento y se realizó análisis factorial exploratorio para determinar el número de factores que explicaban el constructo, confirmatorio para su validez y su consistencia interna con el coeficiente alfa de Cronbach y la omega de McDonald.
Resultados. El análisis factorial exploratorio mostró solución de un solo factor que dio cuenta del 56.17% de la varianza. El análisis confirmatorio mostró índices de ajuste X2=1120.516; gl=10, p=0.04; RCMEA=0.134 (IC90%: 0.056-0.217); ICA=0.992; ITL=0.983 y RCMR=0.61.
Conclusiones. El WHO-5 WBI mostró aceptable reproducibilidad, estructura factorial unidimensional y cuestionable validez de constructo.
Palabras clave: Análisis factorial; Estudios de validación; Reproducibilidad de resultados; Depresión (DeCS).
Simancas-Pallares M, Díaz-Cárdenas S, Barbosa-Gómez P, Buendía-Vergara M, Arévalo-Tovar L. Propiedades psicométricas del Índice de Bienestar General-5 de la Organización Mundial de la Salud en pacientes parcialmente edéntulos. Rev. Fac. Med. 2016;64(4):701-6. Spanish. doi:
https://doi.org/10.15446/revfacmed.v64n4.52235.
| Abstract |
Introduction: Measuring well-being in dental patients allows early detection of emotional disorders.
Objective: To evaluate the psychometric properties of the Well-being index by the World Health Organization (WHO-5 WBI) in partially edentulous patients.
Materials and methods: Scale validation study and diagnostic tests without reference standard performed in 105 patients treated at an oral implantology service. The WHO-5 WBI was applied before treatment and an exploratory factor analysis was performed to determine the amount of factors in the construct that confirmed its validity and internal consistency through Cronbach’s alpha and McDonald’s omega.
Results: The exploratory factor analysis showed a single factor solution that accounted for 56.17% of the variance. The confirmatory analysis showed adjustment indexes X2=1120.516; df=10, p=0.04; RMSEA=0.134 (90% CI: 0.056-0.217); CFI=0.992; TLI=0.983 and WRMR= 0.61.
Conclusions: The WHO-5 WBI showed acceptable reproducibility, one-dimensional factor structure and questionable construct validity.
Keywords: Factor Analysis; Validation Studies; Reproducibility of Results; Depression (MeSH).
Simancas-Pallares M, Díaz-Cárdenas S, Barboza-Gómez P, Buendía-Vergara M, Arévalo-Tovar L. [Psychometric properties of the WHO-5 Well-being index in partially edentulous patients]. Rev. Fac. Med. 2016;64(4):701-6. Spanish. doi: https://doi.org/10.15446/revfacmed.v64n4.52235.
Introducción
El edentulismo se define como la falta de uno o más dientes (1). Esta condición afecta al 70.43% de los colombianos y presenta un marcado inicio a edades tempranas: 15.28% de los adolescentes presenta pérdida de algún diente (2). Sumada a la presencia de otras comorbilidades orales, la pérdida total o parcial de los dientes refleja un impacto negativo sobre el bienestar general y la calidad de vida (3), genera incapacidad laboral, incrementa los costos asociados a tratamientos recibidos, altera la vida social (4) y puede asociarse a síntomas depresivos en un individuo (5,6). Resulta imperativa la evaluación de bienestar emocional en pacientes atendidos en la consulta odontológica, dado que, con frecuencia, en la práctica clínica se considera a este como el mejor indicador de síntomas depresivos (7).
La salud bucal resulta de la interacción de factores económicos, sociales, biológicos y culturales, los cuales propician mayor permanencia de los dientes para un correcto funcionamiento del sistema estomatognático y de sus interrelaciones con los demás órganos del cuerpo, las cuales permiten la adecuada satisfacción de las necesidades psicosociales y físicas del individuo (8). El componente bucal de la salud constituye un aspecto fundamental en las condiciones de vida y de bienestar de la población (9). El concepto de bienestar incluye diferentes dominios relacionados al individuo y la sociedad; uno de estos dominios que puede verse comprometido con el estado de salud bucal corresponde al psicológico: la falta de dientes y la presencia de enfermedades bucales pueden comprometer el estado emocional del paciente y asociarse a síntomas como ánimo depresivo, ideas de minusvalía e insatisfacción personal y social, lo cual, a su vez, compromete su bienestar y calidad de vida (3).
La Organización Mundial de la Salud diseñó el Índice de Bienestar General (WHO WBI: World Health Organization Well-Being Index) para cuantificar el bienestar emocional, es decir, los síntomas depresivos (10). Este instrumento cuenta con versiones previas de 28, 22 y 10 ítems con aceptable desempeño; sin embargo, la versión más reciente y de mayor aplicación, dada su brevedad, es la de 5 ítems (WHO-5 WBI), que identifica posibles casos de episodio depresivo mayor en la población general (11-13) y en pacientes adultos con diferentes enfermedades (11,14-16). A pesar de su eficiencia, a la fecha solo un estudio describe el estado de bienestar emocional en pacientes que requieran atención odontológica empleando el WHO-5 WBI (17).
Se cuenta con informes de las propiedades psicométricas del WHO-5 WBI en personas adultas, pacientes con enfermedad de Parkinson, trastorno depresivo mayor y diabetes. De forma general, estos estudios reflejan adecuadas medidas: consistencia interna (0.91-0.93), confiabilidad prueba-reprueba (coeficiente de correlación intraclase: 0.613), validez de constructo (raíz del cuadrado medio del error de aproximación: 0.09, IC90%: 0.057-0.125, índice comparativo de ajuste: 0.99, índice de Tucker-Lewis: 0,97), discriminante (sin diferencias estadísticamente significativas entre las medias de los puntajes de WHO-5 WBI de acuerdo a características sociodemográficas) y concurrente (la correlación de Spearman entre los dominios de WHO-5 y WHOQOL-BREF fue >0.50, excepto en el dominio social: 0.37), lo que revela que esta escala es útil para el monitoreo del progreso individual de un paciente (14,15,18-23).
En Colombia se cuenta con un solo estudio sobre reproducibilidad y consistencia interna del WHO-5 WBI que reporta alpha de Cronbach de 0.668 (24). No obstante, aun cuando existen estudios en español de las propiedades psicométricas mencionadas con anterioridad (25), hasta el momento no hay investigaciones que empleen técnicas de análisis factorial confirmatorio (AFC) y evidencien la validez de constructo y la consistencia interna de esta escala en pacientes latinoamericanos que requieran tratamiento odontológico.
El objetivo de esta investigación fue evaluar las propiedades psicométricas —validez de constructo y consistencia interna— del WHO-5 WBI en pacientes parcialmente edéntulos que asistieron al servicio de implantología de una escuela de odontología en Cartagena, Colombia.
Materiales y métodos
Se diseñó un estudio de validación de escalas sin criterio de referencia del WHO-5 WBI que contó con aprobación del Comité de Ética en Investigación de la Universidad de Cartagena. Teniendo en cuenta las consideraciones éticas descritas en la Resolución 8430 para investigación en salud en Colombia y después de conocer los objetivos del estudio, los pacientes diligenciaron de forma anónima el instrumento y aceptaron su participación a través de la firma de un consentimiento informado escrito.
Emplazamiento y características de la población
Se invitó a participar a todos los pacientes que asistieron a consulta requiriendo tratamiento odontológico en un servicio de implantes dentales entre febrero y junio de 2015. Se incluyeron 105 sujetos entre 22 y 83 años con un promedio de 54.98±9.9 años; el 70.4% eran mujeres y más de la mitad (53.3%) pertenecían a estrato 3. Respecto de las condiciones orales, la media de dientes presentes fue 21.78±4.0 y 41.9% presentaron estado de salud oral pobre.
Instrumento
El WHO-5 WBI es una escala que consta de cinco reactivos expresados de forma interrogativa que indagan sobre la presencia de aspectos relacionados con bienestar emocional medidos en un solo factor como ¿Me he sentido alegre y de buen ánimo? y ¿Mi vida diaria ha tenido cosas interesantes para mí? El tiempo total para la aplicación de esta escala requiere entre uno y tres minutos.
La puntuación de las respuestas tipo Likert permite conocer la frecuencia de aparición de los aspectos estudiados y varía en una escala de 0 (nunca) a 3 (siempre). Por tanto, los puntajes finales pueden variar desde 0 a 15; a mayor puntuación mayor bienestar o a menor puntuación más síntomas depresivos con importancia clínica (10).
Análisis estadístico
Se realizó análisis estadístico descriptivo; para las variables cualitativas se calcularon proporciones e intervalos de confianza al 95% y para las variables cuantitativas media y desviación estándar o mediana y rango intercuartílico dependiendo de la simetría de la distribución. La consistencia interna se estimó con el coeficiente alfa de Cronbach (26) y con omega de McDonald debido a las múltiples limitaciones del estadístico alfa cuando no se cumplió el principio de tau-equivalencia (27). La correlación de cada ítem de la puntuación total se realizó con el coeficiente de correlación de Pearson.
Para la evaluación de la validez de constructo se determinó la factorizabilidad de la matriz con la prueba de esfericidad de Barlett y la prueba de adecuación de la muestra de Kaiser-Meyer-Olkin; luego, se realizó análisis factorial exploratorio (AFE) para conocer la estructura de factores. El número de factores a extraer se determinó a través de los valores propios y un gráfico de sedimentación de Catell; para definir su conformación se tomaron en cuenta las cargas factoriales con valor ≥0.50. Asimismo Se empleó rotación oblicua (promax) puesto que se consideró que los posibles factores estarían correlacionados entre sí.
El AFC se realizó para confirmar la estructura de factores previamente determinada en el AFE y la validez de constructo a través de mínimos cuadrados parciales con media y varianza ajustada (MCPMVA). Para la evaluación del ajuste del modelo se realizó la evaluación de los siguientes valores según los criterios propuestos por Hu y Bentler: Chi cuadrado (X2), grados de libertad (gl), p-valor para X2>0.05, raíz del cuadrado medio del error de aproximación (RCEMA) ≤0.06 e intervalo de confianza al 90%, índice comparativo de ajuste (ICA) ≥0.95, índice de Tucker-Lewis (ITL) ≥0.95 y raíz del cuadrado medio del residual ponderado (RCMR) (28).
El análisis estadístico descriptivo y el AFE se realizaron en el paquete Stata v.13.2 para Windows (Statacorp, College Drive Station, TX, USA), mientras que el AFC se realizó en Mplus v.7.31 para Windows (Muthén & Muthén, Los Angeles, CA., USA).
Resultados
La media global para WHO-5 WBI fue 13.04. El mínimo valor encontrado fue 6 y el máximo 15. La estadística descriptiva de acuerdo a los ítems se plasmó en la Tabla 1.
Tabla 1. Estadística descriptiva para cada uno de los reactivos que conforman la escala.
|
Durante las últimas dos semanas… |
Media |
Desviación estándar |
CIPT |
|
¿Me he sentido alegre y de buen ánimo? |
2.580 |
0.616 |
0.520 |
|
¿Me he sentido tranquilo/a y relajado/a? |
2.533 |
0.651 |
0.790 |
|
¿Me he sentido activo/a y con energía? |
2.580 |
0.616 |
0.726 |
|
¿Me he levantado sintiéndome bien y descansado/a? |
2.609 |
0.642 |
0.803 |
|
¿Mi vida diaria ha tenido cosas interesantes para mí? |
2.742 |
0.537 |
0.804 |
CIPT: correlación ítem puntuación total. Fuente: Elaboración propia.
Consistencia interna
El coeficiente alfa de Cronbach para WHO-5 WBI fue 0.852. Al evaluar la consistencia interna se obtuvo mejora del coeficiente Alfa para el ítem ¿Mi vida diaria ha tenido cosas interesantes para mí? (0.863), seguido de ¿Me he sentido alegre y de buen ánimo? (0.859). Por su parte, el coeficiente omega de McDonald fue 0.877.
Validez de constructo
La prueba de esfericidad de Barlett en el AFE fue X2=277.580, gl=10 y p-valor=0.000 y la prueba de adecuación muestral de Kaiser-Meyer-Olkin 0.763. La estructura factorial sugirió un solo factor que agrupó los cinco ítems y mostró un autovalor de 2.808 que explicó el 56.17% de la varianza total, esto se evidenció en el gráfico de sedimentación de Catell de la Figura 1, mientras que en la Tabla 2 se plasmó la solución factorial obtenida.
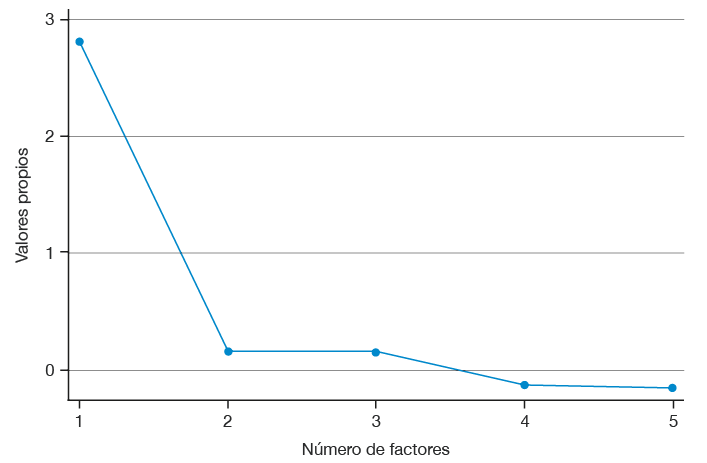
Figura 1. Gráfico de sedimentación Catell. Fuente: Elaboración propia.
Tabla 2. Cargas factoriales y comunalidades para la solución obtenida del Índice de Bienestar General-5.
|
Durante las últimas dos semanas… |
Factor |
Comunalidad |
|
¿Me he sentido alegre y de buen ánimo? |
0.566 |
0.3989 |
|
¿Me he sentido tranquilo/a y relajado/a? |
0.843 |
0.7395 |
|
¿Me he sentido activo/a y con energía? |
0.834 |
0.7708 |
|
¿Me he levantado sintiéndome bien y descansado/a? |
0.878 |
0.8079 |
|
¿Mi vida diaria ha tenido cosas interesantes para mí? |
0.556 |
0.4006 |
Fuente: Elaboración propia.
El AFC arroja como resultado los siguientes índices de ajuste: X2=1120.516; gl=10, p-valor=0.04; RCEMA=0.134 (IC90%: 0.056-0.217); ICA=0.992; ITL=0.983 y RCMR=0.61 y no se detectan índices de modificación. La Figura 1 sugiere retener un solo factor como respuesta a la estructura factorial de la escala; allí se muestra solo uno de los valores propios por encima del punto de inflexión de la línea del número de factores desde donde esta se vuelve estable (2).
Discusión
Los pacientes parcialmente edéntulos y que requieren atención odontológica pueden no comunicar al profesional, de manera efectiva, el estado actual de su situación emocional. Por tanto, la evaluación de síntomas de depresión —a través de WHO-5 WBI— como parte integral de su tratamiento se convierte en una herramienta factible para lograr un verdadero y profundo impacto positivo sobre la calidad de vida del paciente (29,30) en conjunto con el tratamiento dental. Esta situación propendería incluso a mejorar las tasas de aceptación y efectividad de los tratamientos, más aun, en aquellos en donde se requiera adherencia a protocolos (31).
Diversas investigaciones dan cuenta de las propiedades psicométricas del WHO-5 WBI en distintos idiomas. Se cuenta con reportes de consistencia interna en español con valores de 0.66 (24) y 0.86 (25), en inglés de 0.91 (32), en tailandés de 0.87 (15) y en japonés de 0.89 (33); estimadores que son consistentes con los reportados en la presente investigación. No todos los estudios realizados hasta la fecha informan resultados de análisis factorial tanto exploratorio (AFE) como confirmatorio (AFC) para informar propiedades psicométricas de un instrumento de medición.
En consonancia con lo anterior, los hallazgos de la presente investigación son consistentes con otros estudios realizados por Campo-Arias (24) en Colombia, Lucas-Carrasco (25) en España, Hajos et al. (32) en Holanda, Saipanish et al. (15) en Tailandia, Guethmundsdottir et al. (34) en Islandia y Awata et al. (18) en Japón al encontrar un solo factor subyacente al constructo de bienestar emocional a través del WHO-5 WBI.
Los datos estadísticos derivados del AFC sugieren pobre ajuste del instrumento y, por tanto, cuestionable validez de constructo. Al comparar los resultados del AFC encontrados en el presente estudio, se puede observar que entre los tres países en los que se ha evaluado validez de constructo (VC) con AFC —Colombia, Islandia y Holanda—, el único en donde se encuentra adecuado ajuste de las medidas obtenidas de VC es Holanda.
Los hallazgos de Guethmundsdottir et al. (34) en Islandia y del presente estudio se dieron en pacientes pertenecientes a centros de cuidado primario y sistémicamente sanos, mientras que el estudio de Hajos et al. (32) en Holanda, al aplicar el instrumento en inglés, fue realizado en pacientes con diabetes mellitus (DM). Así, la existencia de una enfermedad sistémica crónica puede suponer un mejor desempeño del instrumento, debido a que el deterioro a la integridad física, y por tanto el cambio en el bienestar emocional causado por la DM, puede ser fácilmente detectable, evidenciando así la adecuada validez de constructo de la escala (5).
Aun cuando los resultados del presente estudio sugieren validez de constructo cuestionable, el WHO-5 WBI representa un instrumento adecuado para el tamizaje de síntomas depresivos en población adulta y su uso puede incrementar la capacidad de detectar estos síntomas, generados por la condición dental del paciente en centros de atención primaria (19). El WHO-5 WBI resulta entonces de amplia utilidad y de fácil interpretación para todos los profesionales del área de la salud, y de la atención odontológica para este caso específico.
A menudo se necesitan escalas que reflejen mediciones con adecuada validez y confiabilidad y que permitan el empleo apropiado a través de diversas poblaciones y situaciones. El desarrollo de nuevas escalas (p. ej. debido a su uso en nuevas poblaciones) es un proceso costoso y que demanda mucho tiempo; así, una opción adecuada es emplear escalas ya existentes estudiando con antelación su desempeño psicométrico. En este contexto, el AFC se puede emplear para examinar si el constructo original de la escala se está midiendo en esta población (35). El AFC es una herramienta estadística poderosa para examinar la naturaleza y las relaciones entre diversos constructos y que, a diferencia del AFE, prueba a priori hipótesis explícitas acerca de relaciones entre variables observadas y variables latentes o factores. Esta última es, a menudo, la herramienta analítica de elección para el desarrollo y refinamiento de instrumentos de medición —escalas—, identificación de efectos de métodos y evaluación de invariancia entre grupos y tiempo (36).
Este estudio presenta algunas limitaciones:
1) se condujo en el servicio de una clínica odontológica universitaria de la ciudad de Cartagena, por tanto los respondientes pueden no reflejar completamente las condiciones de cuidado primario observadas en áreas rurales en donde los estilos de vida pueden ser más tranquilos. Un estilo de vida más tranquilo puede influenciar el puntaje de los ítems dos y cinco, los cuales indagan por sentirse más tranquilo y relajado y cosas interesantes en la vida diaria.
2) las características clínicas odontológicas de estos pacientes al momento de responder el cuestionario pueden no reflejar un estado que represente carga de enfermedad bucal; lo anterior debido a que los pacientes que buscan atención con implantes dentales han sido tratados con anterioridad por otras condiciones como caries, enfermedad periodontal o enfermedad endodóncica, lo cual puede generar un transitorio estado de “buena salud bucal” y probablemente los pacientes no sientan el mismo grado de decaimiento emocional.
Las consecuencias de ignorar el componente emocional de los pacientes en la práctica se han enfatizado por varios autores, por tanto, la práctica odontológica no debe estar aislada y debe incorporar entre sus medidas de monitoreo instrumentos como el WHO-5 WBI a fin de ofrecer tratamientos integrales a los pacientes.
Conclusiones
El WHO-5 WBI es un instrumento sencillo, fácil y de corto tiempo de administración con estructura factorial simple, sólida y de adecuada consistencia interna que puede ser usado en la atención odontológica. No obstante, se requieren futuras investigaciones que prueben esta herramienta con la forma de respuesta originalmente sugerida y se comparen los índices de ajuste derivados de AFC para realizar conclusiones sobre su validez de contenido en poblaciones de Latinoamérica.
Se requieren estudios que puedan evaluar su validez discriminante comparando los puntajes obtenidos del WHO-5 WBI y la invariancia de su estructura factorial en pacientes edéntulos y dentados y así realizar conclusiones adecuadas y generales sobre la validez del instrumento.
Conflicto de intereses
Ninguno declarado por los autores.
Financiación
Ninguna declarada por los autores.
Agradecimientos
A la auxiliar de odontología Patricia Cabarcas por su invaluable ayuda al contactar los pacientes sujetos de estudio.
Referencias
1. American Dental Association. Chicago: ADA; 2015 [cited 2015 Jul 6]. Availble from: https://goo.gl/v5jyy3.
2. Ministerio de Salud y Protección Social. IV Estudio Nacional de Salud Bucal. Situación de Salud Bucal. Bogotá, D.C.: Minsalud; 2015.
3. Díaz-Cárdenas S, Arrieta-Vergara K, Ramos-Martínez K. Impacto de la salud oral en la calidad de vida de adultos mayores. Rev. Clín. Med. Fam. 2012;5(1):9-16. http://doi.org/br3z.
4. Gil-Montoya JA, de Mello AL, Barrios R, González-Moles MA, Bravo M. Oral health in the elderly patient and its impact on general well-being: a nonsystematic review. Clin. Interv. Aging. 2015;10:461-7. http://doi.org/br32.
5. Fiest KM, Currie SR, Williams JV, Wang J. Chronic conditions and major depression in community-dwelling older adults. J. Affect Disord. 2011;131(1-3):172-8. http://doi.org/dnhvq8.
6. Friedman PK, Kaufman LB, Karpas SL. Oral Health Disparity in Older Adults: Dental Decay and Tooth Loss. Dent. Clin. North Am. 2014;58(4):757-70. http://doi.org/br33.
7. Kumar A, Kardkal A, Debnath S, Lakshminarayan J. Association of periodontal health indicators and major depressive disorder in hospital outpatients. J. Indian Soc. Periodontol. 2015;19(5):507-11. http://doi.org/br34.
8. Higashida B. Odontología preventiva. 2nd ed. México, D.F.: McGraw-Hill; 2000.
9. Vettore MV, Faerstein E, Baker SR. Social position, social ties and adult’s oral health: 13 year cohort study. J. Dent. 2016;44:50-6 http://doi.org/br35.
10. World Health Organization. Wellbeing measures in primary health care: the DepCare project: report on a WHO meeting. Stockholm: WHO; 1998.
11. Bech P, Gudex C, Staehr Johansen KS. The WHO (Ten) well-being index: validation in diabetes. Psychother Psychosom. 1996;65(4):183-90.
12. Bradley C. Handbook of psychology and diabetes: a guide to psychological measurement in diabetes research and practice. Harwood: Routledge; 2013.
13. Henkel V, Mergl R, Kohnen R, Allgaier AK, Möller HJ, Hegerl U. Use of brief depression screening tools in primary care: consideration of heterogeneity in performance in different patient groups. Gen Hosp Psychiatry. 2004;26(3):190-8. http://doi.org/fvpv65.
14. Awata S, Bech P, Koizumi Y, Seki T, Kuriyama S, Hozawa A, et al. Validity and utility of the Japanese version of the WHO-Five Well-Being Index in the context of detecting suicidal ideation in elderly community. residents. Int. Psychogeriatr. 2007;19(01):77-88. http://doi.org/c65jrz
15. Saipanish R, Lotrakul M, Sumrithe S. Reliability and validity of the Thai version of the WHO-Five Well-Being Index in primary care patients. Psychiatry Clin Neurosci. 2009;63(2):141-6. http://doi.org/cx5f9c.
16. Phillips CM, Perry IJ. Depressive symptoms, anxiety and well-being among metabolic health obese subtypes. Psychoneuroendocrinology. 2015;62:47-53. http://doi.org/br5t.
17. Peeran SW, Kumar NP, Azaruk FAA, Alsaid FM, Abdalla KA, Mugrabi MH, et al. Association between mental well-being, depression, and periodontal attachment level among young adults of the postwar Sebha city, Libya: A pilot study. J. Nat. Sci. Biol. Med. 2014;5(2):308-12. http://doi.org/br5v
18. Awata S, Bech P, Yoshida S, Hirai M, Suzuki S, Yamashita M, et al. Reliability and validity of the Japanese version of the world health organization-five well-being index in the context of detecting depression in diabetic patients. Psychiatry Clin. Neurosci. 2007;61(1):112-9. http://doi.org/bvcfqw.
19. Henkel V, Mergl R, Kohnen R, Maier W, Möller HJ, Hegerl U. Identifying depression in primary care: a comparison of different methods in a prospective cohort study. Bmj. 2003;326(7382):200-1. http://doi.org/c9fxtj.
20. Bonsignore M, Barkow K, Jessen F, Heun R. Validity of the five-item WHO Well-Being Index (WHO-5) in an elderly population. Eur. Arch Psychiatry Clin. Neurosci. 2001;251(Suppl 2):27-31. http://doi.org/dk33zj.
21. Heun R, Burkart M, Maier W, Bech P. Internal and external validity of the WHO Well-Being Scale in the elderly general population. Acta Psychiatr. Scand. 1999;99(3):171-8. http://doi.org/cqchjk.
22. Löwe B, Spitzer RL, Gräfe K, Kroenke K, Quenter A, Zipfel S, et al. Comparative validity of three screening questionnaires for DSM-IV depressive disorders and physicians’ diagnoses. J. Affect. Disord. 2004;78(2):131-40. http://doi.org/d86zh2.
23. Newnham EA, Hooke GR, Page AC. Progress monitoring and feedback in psychiatric care reduces depressive symptoms. J. Affect. Disord. 2010;127(1-3):139-46. http://doi.org/c4v7sm.
24. Campo-Arias A, Miranda-Tapia GA, Cogollo Z, Herazo E. Reproducibilidad del Índice de Bienestar General (WHO-5 WBI) en estudiantes adolescentes. Salud Uninorte. 2015;31(1):18-24.
25. Lucas-Carrasco R. Reliability and validity of the Spanish version of the World Health Organization-Five Well-Being Index in elderly. Psychiatry Clinl Neurosci. 2012;66(6):508-13. http://doi.org/br5w.
26. Campo-Arias A, Oviedo HC. Propiedades psicométricas de una escala: la consistencia interna. Rev. Salud Pública. 2008;10(5):831-9.
http://doi.org/bz8q2z.
27. McDonald RP. The theoretical foundations of principal factor analysis, canonical factor analysis, and alpha factor analysis. Br. J. Math. Stat Psychol. 1970;23(1):1-21. http://doi.org/fqg277.
28. Hu Lt, Bentler PM. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Structural equation modeling: a multidisciplinary journal. 1999;6(1):1-55. http://doi.org/dbt.
29. Yuen HK, Hant FN, Hatfield C, Summerlin LM, Smith EA, Silver RM. Factors associated with oral hygiene practices among adults with systemic sclerosis. Int J. Dent. Hyg. 2014;12(3):180-6. http://doi.org/br5x.
30. Zheng J, Wong MC, Lam CL. Key factors associated with oral health-related quality of life (OHRQOL) in Hong Kong Chinese adults with orofacial pain. J. Dent. 2011;39(8):564-71. http://doi.org/c54cvk.
31. Janardhanan T, Cohen CI, Kim S, Rizvi BF. Dental care and associated factors among older adults with schizophrenia. J. Am. Dent. Assoc. 2011;142(1):57-65. http://doi.org/br5z.
32. Hajos T, Pouwer F, Skovlund SE, Den Oudsten BL, Geelhoed-Duijvestijn PH, Tack CJ, et al. Psychometric and screening properties of the WHO-5 well-being index in adult outpatients with Type 1 or Type 2 diabetes mellitus. Diabet Med. 2013;30(2):e63-e9. http://doi.org/br52.
33. Guðmundsdóttir HB, Olason DP, Guðmundsdottir DG, Sigurðsson JF. A psychometric evaluation of the Icelandic version of the WHO-5. Scand. J. Psychol. 2014;55(6):567-72. http://doi.org/br53.
34. Harrington D. Confirmatory factor analysis. Oxford: Oxford University Press; 2008.
35. Brown TA. Confirmatory factor analysis for applied research. New York: Guilford Publications; 2015.
36. Russell DW. In search of underlying dimensions: The use (and abuse) of factor analysis in Personality and Social Psychology Bulletin. Pers. Soc. Psychol Bull. 2002;28(12):1629-46. http://doi.org/c9fn3m.
César Alexander Eslava Franco
“Mapas anatómicos”
Universidad Nacional de Colombia
Referencias
American Dental Association. Chicago: ADA; 2015 [cited 2015 Jul 6]. Availble from: https://goo.gl/v5jyy3.
Ministerio de Salud y Protección Social. IV Estudio Nacional de Salud Bucal. Situación de Salud Bucal. Bogotá, D.C.: Minsalud; 2015.
Díaz-Cárdenas S, Arrieta-Vergara K, Ramos-Martínez K. Impacto de la salud oral en la calidad de vida de adultos mayores. Rev. Clín. Med. Fam. 2012;5(1):9-16. http://doi.org/br3z.
Gil-Montoya JA, de Mello AL, Barrios R, González-Moles MA, Bravo M. Oral health in the elderly patient and its impact on general well-being: a nonsystematic review. Clin. Interv. Aging. 2015;10:461-7. http://doi.org/br32.
Fiest KM, Currie SR, Williams JV, Wang J. Chronic conditions and major depression in community-dwelling older adults. J. Affect Disord. 2011;131(1-3):172-8. http://doi.org/dnhvq8.
Friedman PK, Kaufman LB, Karpas SL. Oral Health Disparity in Older Adults: Dental Decay and Tooth Loss. Dent. Clin. North Am. 2014;58(4):757-70. http://doi.org/br33.
Kumar A, Kardkal A, Debnath S, Lakshminarayan J. Association of periodontal health indicators and major depressive disorder in hospital outpatients. J. Indian Soc. Periodontol. 2015;19(5):507-11. http://doi.org/br34.
Higashida B. Odontología preventiva. 2nd ed. México, D.F.: McGraw-Hill; 2000.
Vettore MV, Faerstein E, Baker SR. Social position, social ties and adult’s oral health: 13 year cohort study. J. Dent. 2016;44:50-6 http://doi.org/br35.
World Health Organization. Wellbeing measures in primary health care: the DepCare project: report on a WHO meeting. Stockholm: WHO; 1998.
Bech P, Gudex C, Staehr Johansen KS. The WHO (Ten) well-being index: validation in diabetes. Psychother Psychosom. 1996;65(4):183-90.
Bradley C. Handbook of psychology and diabetes: a guide to psychological measurement in diabetes research and practice. Harwood: Routledge; 2013.
Henkel V, Mergl R, Kohnen R, Allgaier AK, Möller HJ, Hegerl U. Use of brief depression screening tools in primary care: consideration of heterogeneity in performance in different patient groups. Gen Hosp Psychiatry. 2004;26(3):190-8. http://doi.org/fvpv65.
Awata S, Bech P, Koizumi Y, Seki T, Kuriyama S, Hozawa A, et al. Validity and utility of the Japanese version of the WHO-Five Well-Being Index in the context of detecting suicidal ideation in elderly community residents. Int. Psychogeriatr. 2007;19(01):77-88. http://doi.org/c65jrz
Saipanish R, Lotrakul M, Sumrithe S. Reliability and validity of the Thai version of the WHO-Five Well-Being Index in primary care patients. Psychiatry Clin Neurosci. 2009;63(2):141-6. http://doi.org/cx5f9c.
Phillips CM, Perry IJ. Depressive symptoms, anxiety and well-being among metabolic health obese subtypes. Psychoneuroendocrinology. 2015;62:47-53. http://doi.org/br5t.
Peeran SW, Kumar NP, Azaruk FAA, Alsaid FM, Abdalla KA, Mugrabi MH, et al. Association between mental well-being, depression, and periodontal attachment level among young adults of the postwar Sebha city, Libya: A pilot study. J. Nat. Sci. Biol. Med. 2014;5(2):308-12. http://doi.org/br5v.
Awata S, Bech P, Yoshida S, Hirai M, Suzuki S, Yamashita M, et al. Reliability and validity of the Japanese version of the world health organization- five well-being index in the context of detecting depression in diabetic patients. Psychiatry Clin. Neurosci. 2007;61(1):112-9. http://doi.org/bvcfqw.
Henkel V, Mergl R, Kohnen R, Maier W, Möller HJ, Hegerl U. Identifying depression in primary care: a comparison of different methods in a prospective cohort study. Bmj. 2003;326(7382):200-1. http://doi.org/c9fxtj.
Bonsignore M, Barkow K, Jessen F, Heun R. Validity of the five-item WHO Well-Being Index (WHO-5) in an elderly population. Eur. Arch Psychiatry Clin. Neurosci. 2001;251(Suppl 2):27-31. http://doi.org/dk33zj.
Heun R, Burkart M, Maier W, Bech P. Internal and external validity of the WHO Well-Being Scale in the elderly general population. Acta Psychiatr. Scand. 1999;99(3):171-8. http://doi.org/cqchjk.
Löwe B, Spitzer RL, Gräfe K, Kroenke K, Quenter A, Zipfel S, et al. Comparative validity of three screening questionnaires for DSMIV depressive disorders and physicians’ diagnoses. J. Affect. Disord. 2004;78(2):131-40. http://doi.org/d86zh2.
Newnham EA, Hooke GR, Page AC. Progress monitoring and feedback in psychiatric care reduces depressive symptoms. J. Affect. Disord. 2010;127(1-3):139-46. http://doi.org/c4v7sm.
Campo-Arias A, Miranda-Tapia GA, Cogollo Z, Herazo E. Reproducibilidad del Índice de Bienestar General (WHO-5 WBI) en estudiantes adolescentes. Salud Uninorte. 2015;31(1):18-24.
Lucas-Carrasco R. Reliability and validity of the Spanish version of the World Health Organization-Five Well-Being Index in elderly. Psychiatry Clinl Neurosci. 2012;66(6):508-13. http://doi.org/br5w.
Campo-Arias A, Oviedo HC. Propiedades psicométricas de una escala: la consistencia interna. Rev. Salud Pública. 2008;10(5):831-9. http://doi.org/bz8q2z.
McDonald RP. The theoretical foundations of principal factor analysis, canonical factor analysis, and alpha factor analysis. Br. J. Math. Stat Psychol. 1970;23(1):1-21. http://doi.org/fqg277.
Hu Lt, Bentler PM. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Structural equation modeling: a multidisciplinary journal. 1999;6(1):1-55. http://doi.org/dbt.
Yuen HK, Hant FN, Hatfield C, Summerlin LM, Smith EA, Silver RM. Factors associated with oral hygiene practices among adults with systemic sclerosis. Int J. Dent. Hyg. 2014;12(3):180-6. http://doi.org/br5x.
Zheng J, Wong MC, Lam CL. Key factors associated with oral health- related quality of life (OHRQOL) in Hong Kong Chinese adults with orofacial pain. J. Dent. 2011;39(8):564-71. http://doi.org/c54cvk.
Janardhanan T, Cohen CI, Kim S, Rizvi BF. Dental care and associated factors among older adults with schizophrenia. J. Am. Dent. Assoc. 2011;142(1):57-65. http://doi.org/br5z.
Hajos T, Pouwer F, Skovlund SE, Den Oudsten BL, Geelhoed- Duijvestijn PH, Tack CJ, et al. Psychometric and screening properties of the WHO-5 well-being index in adult outpatients with Type 1 or Type 2 diabetes mellitus. Diabet Med. 2013;30(2):e63-e9. http://doi.org/br52.
Guðmundsdóttir HB, Olason DP, Guðmundsdottir DG, Sigurðsson JF. A psychometric evaluation of the Icelandic version of the WHO-5. Scand. J. Psychol. 2014;55(6):567-72. http://doi.org/br53.
Harrington D. Confirmatory factor analysis. Oxford: Oxford University Press; 2008.
Brown TA. Confirmatory factor analysis for applied research. New York: Guilford Publications; 2015.
Russell DW. In search of underlying dimensions: The use (and abuse) of factor analysis in Personality and Social Psychology Bulletin. Pers. Soc. Psychol Bull. 2002;28(12):1629-46. http://doi.org/c9fn3m.
Cómo citar
APA
ACM
ACS
ABNT
Chicago
Harvard
IEEE
MLA
Turabian
Vancouver
Descargar cita
CrossRef Cited-by
1. Nikolai M. Rodas-Vera. (2025). The loving reciprocity scale: Internal structure, factorial invariance, reliability, and convergent validity. Acta Psychologica, 257, p.105128. https://doi.org/10.1016/j.actpsy.2025.105128.
2. Diego Armando León Rodríguez, María Paula Tobar Herrera, María Olga Hodeg Fernández de Castro, Oscar Mauricio Aguilar Mejía. (2022). Empatía, redes sociales e indicadores de salud mental durante las crisis sociales en Colombia. Universitas Psychologica, 21, p.1. https://doi.org/10.11144/Javeriana.upsy21.ersi.
3. Daniel E. Suárez, Andres C. Cardozo, Miguel E. Villarreal, Elena M. Trujillo. (2021). Non-Heterosexual Medical Students Are Critically Vulnerable to Mental Health Risks: The Need to Account for Sexual Diversity in Wellness Initiatives. Teaching and Learning in Medicine, 33(1), p.1. https://doi.org/10.1080/10401334.2020.1805324.
4. José Fernando Pérez Zarate, Yermin Yolanda Tuesta Chamorro, Jacqueline Iraida Quispe Plaza. (2021). Propiedades psicométricas de la escala de Inteligencia Emocional TMMS-24 en adultos de Lima Metropolitana, 2020. PSIQUEMAG/ Revista Científica Digital de Psicología, 9(2), p.60. https://doi.org/10.18050/psiquemag.v9i2.2657.
5. Yeison David Gallo-Barrera , Laura Vanessa Fuentes Vanegas, Ediltrudis Ramos-De La Cruz. (2023). Propiedades psicométricas del Índice de Bienestar General en mujeres gestantes colombianas. Avances en Enfermería, 41(2) https://doi.org/10.15446/av.enferm.v41n2.105068.
6. Y. Manrique-Anaya, Z. Cogollo Milanés, M. Simancas Pallares. (2021). Adaptación transcultural y validez de un pictograma para evaluar necesidades de comunicación en adultos con vía aérea artificial en cuidados intensivos. Enfermería Intensiva, 32(4), p.198. https://doi.org/10.1016/j.enfi.2021.01.001.
7. Izara Maité Mondragón Moreno, Yazmín María Lucila Cadena Camargo, Isabela Osorio Jaramillo, Andrés Duarte Osorio, Carlos Gómez-Restrepo. (2024). Prostitución en migrantes: ¿afecta solo la salud sexual de la mujer? Revisión de la literatura y descripción de la situación de salud mental de un grup de mujeres migrantes prostituidas y sus hijos. Revista Colombiana de Psiquiatría, https://doi.org/10.1016/j.rcp.2024.09.003.
8. Diego Armando León Rodríguez, Oscar Mauricio Aguilar Mejía. (2024). La medición del uso de redes sociales y su impacto sobre la salud mental durante las crisis sociales. Universitas Psychologica, 23, p.1. https://doi.org/10.11144/Javeriana.upsy23.murs.
9. Esvin Aldair Guevara-Tantalean, Anthony Brayham Tantaleán-Arteaga, Bruno Francesco Arévalo-García, Denis Frank Cunza-Aranzábal. (2025). Development and Psychometric Properties of a Scale to Measure the Meaning of Life (MLS). European Journal of Investigation in Health, Psychology and Education, 15(9), p.174. https://doi.org/10.3390/ejihpe15090174.
10. Renzo Felipe Carranza Esteban, Oscar Mamani-Benito, Julio Cjuno, Madona Tito-Betancur, Susana K. Lingán-Huamán, Dennis Arias-Chávez. (2023). Translation and validation of the WHO-5 General well-being index into native language Quechua of the Peruvian South. Heliyon, 9(6), p.e16843. https://doi.org/10.1016/j.heliyon.2023.e16843.
11. Y. Manrique-Anaya, Z. Cogollo Milanés, M. Simancas Pallares. (2021). Transcultural adaptation and validity of a pictogram to assess communication needs in adults with artificial airway in intensive care. Enfermería Intensiva (English ed.), 32(4), p.198. https://doi.org/10.1016/j.enfie.2021.01.002.
12. Patricia del Pilar Díaz Gamarra, Fernando Joel Rosario Quiroz, Erika Roxana Estrada Alomía, Noemí Edith Iparraguirre Yaurivilca, Miguel Angel Misare Condori. (2025). Psychometric evidence of the WHO-5 well-being index in a sample of participants from hospitals and older adults care centers in Peru. Frontiers in Public Health, 13 https://doi.org/10.3389/fpubh.2025.1670429.
13. Calixto Tapullima Mori, Brigitte Raquel Chávez Castañeda. (2021). Escala de estrés, ansiedad y depresión (DASS-21): propiedades psicométricas en adultos de la provincia de San Martín. PSIQUEMAG/ Revista Científica Digital de Psicología, 11(1), p.73. https://doi.org/10.18050/psiquemag.v11i1.2575.
14. Clara Vergara-Hernández, Miguel Simancas-Pallares, Zoila Carbonell-Muñoz. (2019). Psychometric properties of the revised two-factor study process questionnaire r-spq-2f - spanish version. Duazary, 16(2), p.205. https://doi.org/10.21676/2389783X.2744.
Dimensions
PlumX
Visitas a la página del resumen del artículo
Descargas
Licencia
Derechos de autor 2017 Revista de la Facultad de Medicina

Esta obra está bajo una licencia Creative Commons Reconocimiento 3.0 Unported.
-





















