Prevalencia de hipotiroidismo en una población dislipidémica mayor de 35 años de Manizales, Colombia
Prevalence of hypothyroidism in a dyslipidemic population over age 35 in Manizales, Colombia
DOI:
https://doi.org/10.15446/revfacmed.v64n4.53220Palabras clave:
Hipotiroidismo, Lípidos, Metabolismo (es)Hypothyroidism, Lipids, Metabolism (en)
Introducción. La hormona estimulante de la tiroides (TSH por Thyroid-Stimulating Hormone) actúa como reguladora de lípidos en el metabolismo y puede incidir en el desarrollo de enfermedades cardiovasculares y dislipidemias.
Objetivo. Determinar la prevalencia de hipotiroidismo en pacientes mayores de 35 años diagnosticados con alguna dislipidemia, con o sin tratamiento farmacológico.
Materiales y métodos. Se realizó un estudio transversal que analizó el perfil lipídico y tiroideo de 206 pacientes que presentaron alguna dislipidemia entre el 15 de enero y el 15 de junio de 2013 en una IPS de Manizales; esto, con previo consentimiento informado y diligenciamiento de encuesta.
Resultados. El 81.1% de los participantes presentaron hipercolesterolemia no controlada según referencia comercial y 49% se consideraron hipercolesterolémicos para el valor de referencia ATPIII. 2 de los participantes (0.97%) presentaron hipotiroidismo clínico por sus niveles bajos de T4L y 8 (3.9%), hipotiroidismo subclínico debido a que manifestaron niveles de TSH superiores a 6.16 μUI/ml.
Conclusiones. Se recomienda la valoración de los niveles de TSH en hombres y mujeres mayores de 35 años con alteraciones en el metabolismo de lípidos.
Introduction: The thyroid hormone acts as a regulator of lipids in metabolism and can affect the development of cardiovascular diseases and dyslipidemia.
Objective: To determine the prevalence of hypothyroidism in patients older than 35 years, diagnosed with some dyslipidemia, with or without pharmacotherapy.
Materials and methods: Cross-sectional study in which the lipid and thyroid profile of 206 patients, with some type of dyslipidemia, in a health delivery center of Manizales, was analyzed between January 15 and June 15, 2013; prior informed consent and completion of a survey were requested.
Results: 81.1% of participants had hypercholesterolemia that was not controlled with a commercial reference and 49% were considered hypercholesterolemic in relation to the ATP III reference value. Two participants (0.97%) had clinical hypothyroidism caused by low levels of FT4 and 8 (3.9%) had subclinical hypothyroidism due to TSH levels greater than 6.16 μIU/ml.
Conclusions: The valuation of TSH levels in men and women over 35, with alterations in lipid metabolism, is recommended.investigación original
DOI: https://doi.org/10.15446/revfacmed.v64n4.53220
Prevalencia de hipotiroidismo en una población dislipidémica
mayor de 35 años de Manizales, Colombia
Prevalence of hypothyroidism in a dyslipidemic population over age 35 in Manizales, Colombia
Recibido: 26/09/2015. Aceptado: 24/02/2016.
José Henry Osorio1,2 • César Augusto Aguirre2
1 Universidad de Caldas - Facultad de Ciencias para la Salud - Departamento de Ciencias Básicas de la Salud - Laboratorio de Investigación en Bioquímica Clínica y Patología Molecular - Manizales - Colombia.
2 Universidad de Manizales - Laboratorio de Investigación en Metabolismo - Manizales - Colombia.
Correspondencia: José Henry Osorio. Calle 65 No. 26-10. Teléfono: +57 3113653440. Manizales. Colombia. Correo electrónico:
jose.osorio_o@ucaldas.edu.co.
| Resumen |
Introducción. La hormona estimulante de la tiroides (TSH por Thyroid-Stimulating Hormone) actúa como reguladora de lípidos en el metabolismo y puede incidir en el desarrollo de enfermedades cardiovasculares y dislipidemias.
Objetivo. Determinar la prevalencia de hipotiroidismo en pacientes mayores de 35 años diagnosticados con alguna dislipidemia, con o sin tratamiento farmacológico.
Materiales y métodos. Se realizó un estudio transversal que analizó el perfil lipídico y tiroideo de 206 pacientes que presentaron alguna dislipidemia entre el 15 de enero y el 15 de junio de 2013 en una IPS de Manizales; esto, con previo consentimiento informado y diligenciamiento de encuesta.
Resultados. El 81.1% de los participantes presentaron hipercolesterolemia no controlada según referencia comercial y 49% se consideraron hipercolesterolémicos para el valor de referencia ATPIII. 2 de los participantes (0.97%) presentaron hipotiroidismo clínico por sus niveles bajos de T4L y 8 (3.9%), hipotiroidismo subclínico debido a que manifestaron niveles de TSH superiores a 6.16 µUI/ml.
Conclusiones. Se recomienda la valoración de los niveles de TSH en hombres y mujeres mayores de 35 años con alteraciones en el metabolismo de lípidos.
Palabras clave: Hipotiroidismo; Lípidos; Metabolismo (DeCS).
Osorio JH, Aguirre CA. Prevalencia de hipotiroidismo en una población dislipidémica mayor de 35 años de Manizales, Colombia. Rev. Fac. Med. 2016;64(4): 637-44. Spanish. doi: https://doi.org/10.15446/revfacmed.v64n4.53220.
| Abstract |
Introduction: The thyroid hormone acts as a regulator of lipids in metabolism and can affect the development of cardiovascular diseases and dyslipidemia.
Objective: To determine the prevalence of hypothyroidism in patients older than 35 years, diagnosed with some dyslipidemia, with or without pharmacotherapy.
Materials and methods: Cross-sectional study in which the lipid and thyroid profile of 206 patients, with some type of dyslipidemia, in a health delivery center of Manizales, was analyzed between January 15 and June 15, 2013; prior informed consent and completion of a survey were requested.
Results: 81.1% of participants had hypercholesterolemia that was not controlled with a commercial reference and 49% were considered hypercholesterolemic in relation to the ATP III reference value. Two participants (0.97%) had clinical hypothyroidism caused by low levels of FT4 and 8 (3.9%) had subclinical hypothyroidism due to TSH levels greater than 6.16 μIU/ml.
Conclusions: The valuation of TSH levels in men and women over 35, with alterations in lipid metabolism, is recommended.
Keywords: Hypothyroidism; Lipids; Metabolism (MeSH).
Osorio JH, Aguirre CA. [Prevalence of hypothyroidism in a dyslipidemic population over age 35 in Manizales, Colombia]. Rev. Fac. Med. 2016;64(4): 637-44. Spanish. doi: https://doi.org/10.15446/revfacmed.v64n4.53220.
Introducción
Las patologías asociadas con disfunción tiroidea se han correlacionado con el metabolismo de lípidos y la enfermedad cardiovascular aterosclerótica (1). La hormona estimulante de la tiroides (TSH por Thyroid-Stimulating Hormone), como reguladora del metabolismo de lípidos, puede protagonizar el desarrollo de enfermedad cardíaca coronaria; por esto, en la práctica, se puede observar una asociación de pacientes hipotiroideos clínicos y algunos hipotiroideos subclínicos con incremento en el riesgo de presentación de enfermedad cardiaca coronaria (2-4). En algunos pacientes con síndrome metabólico se observan niveles elevados de TSH y función tiroidea normal, por tal razón surgen interrogantes sobre la posible relación entre TSH y enfermedad cardiovascular (5-7).
El valor de TSH por encima del rango de referencia normal se relaciona positivamente con el colesterol sérico total (8) y el colesterol-LDL se asocia negativamente con el colesterol-HDL (9). A su vez, se ha observado una disminución de la concentración del colesterol total y colesterol-LDL después de realizarse el tratamiento con la hormona tiroxina en individuos con referencia de TSH >10 µUI/ml (10).
La prevalencia de hipotiroidismo subclínico en la población general va del 1% al 10%, mientras que en los infantes, del 3.4% al 6% (11,12); en personas de edad avanzada se alcanza una prevalencia del 16% en varones con edad superior a los 70 años y del 20% en mujeres mayores de 60 (13). En casi todos los casos de hipotiroidismo subclínico (HSC), los valores de TSH son >10 mU/L (14). En adultos eutiroideos se ha demostrado una correlación entre TSH y lípidos en suero, influenciado quizá por la resistencia a la insulina. Por lo tanto, personas con elevada concentración de TSH en suero y resistencia a la insulina presentan mayor riesgo a desarrollar dislipidemia (15,16).
En lo que respecta al metabolismo de lípidos, las concentraciones de T4L siempre son inversamente proporcionales a las de colesterol total y colesterol LDL (17), debido a la disminución en la síntesis de receptores LDL. Además, la administración de levotiroxina tiene un efecto hipolipidémico en el paciente hipotiroideo con elevadas concentraciones de tirotropina, hormona destinada a compensar los bajos niveles de T4L; sin embargo, se presenta dificultad para identificar el corte umbral de asociación entre TSH y lípidos (18). En ese sentido, se ha establecido que el 4.3% de los pacientes hipercolesterolémicos han sido reportados como hipotiroideos (19).
El presente estudio se realizó con el propósito de conocer la prevalencia de hipotiroidismo tanto clínico como subclínico en pacientes dislipidémicos diagnosticados en una IPS de Manizales. Esto, para establecer si las dislipidemias en esta región eran o no secundarias a un desarreglo en el funcionamiento de la glándula tiroidea.
Materiales y métodos
Este estudio fue de tipo observacional, analítico y transversal. Se detectaron 206 pacientes dislipidémicos en un ámbito de atención primaria a través de historias clínicas. La información se obtuvo de las consultas realizadas en la IPS Médicos Internistas de Caldas en Manizales entre el 15 de enero y el 15 de junio del 2013. Una vez detectados los pacientes y revisadas sus historias clínicas, estos fueron invitados a hacer parte del estudio de manera voluntaria; para obtener el consentimiento informado por escrito se les explicó de forma verbal en qué consistía el estudio. A los pacientes incluidos en el estudio se les realizó recolección de datos clínicos a partir de los formatos propuestos y la historia clínica de la consulta médica como documento fuente. Luego, fueron citados para extraer muestras de sangre de la vena cubital después de un ayuno de 12 horas. Las muestras fueron tomadas entre las 7 y las 10 de la mañana en el laboratorio de microbiología de la Universidad de Caldas.
Los criterios de inclusión de los participantes fueron: hombre o mujer de 35 años o más, que hayan asistido a consulta médica a la IPS Médicos Internistas de Caldas en el periodo de estudio, que haya sido diagnosticado con cualquier tipo de dislipidemia y que se encuentren o no bajo medicación hipolipemiante. En ese sentido, los pacientes que participaron en este estudio tienen entre 35 y 89 años y pertenecen a ambos géneros.
Como criterio diagnóstico se tomaron valores >200 mg/dl para hipercolesterolemia, >150 mg/dl para hipertrigliceridemia, <60 mg/dl para dislipidemia por colesterol-HDL, >160 mg/dl para dislipidemia por Colesterol-LDL, <0.8 ng/dl de T4L para hipotiroidismo clínico y >6.16 µUI/ml de TSH para hipotiroidismo subclínico. Los valores de referencia para los lípidos se basaron en el estuche comercial utilizado para el diagnóstico en el laboratorio. Sin embargo, también se tuvieron en cuenta los valores según el criterio establecido por el Tercer Reporte del Comité Estadounidense del Programa de Educación en Colesterol (ATPIII), que define como dislipidemia la presencia de colesterol total ≥240 mg/dl, colesterol-HDL ≤40 mg/dl, colesterol-LDL ≤160 mg/dl y triglicéridos ≥200 mg/dl. También se tuvo en cuenta el índice aterosclerótico CT/HDL, cuyo valor de referencia es de alto riesgo si es >5 en los hombres y >4.5 en las mujeres (20).
A partir de las historias clínicas, se obtuvo la información de edad, peso, talla, medicamentos, antecedentes familiares y personales. Otras variables estudiadas fueron el consumo de medicamentos con efectos colaterales que pueden aumentar la TSH, como metoclopramida, domperidona, amioadorona, litio, yodo, interferón, furosemida y sulfonilureas.
Los criterios de exclusión fueron: pacientes que sufrieran de bocio u otras enfermedades tiroideas, tiroidectomía, tumores malignos, enfermedad hepática, diabetes no controlada, síndrome nefrótico, que consumieran medicamentos que alteraren la TSH como amiodarona, dopamina, litio, yoduro de potasio y prednisona y mujeres en gestación.
El colesterol total se midió con el método de colesterol oxidasa y los triglicéridos fueron cuantificados con la técnica de glicerofosfato oxidasa. A su vez, el colesterol-HDL fue cuantificado por método directo y el colesterol-LDL se calculó con ayuda de la fórmula de Friedewald.
La prueba de TSH se realizó por ensayo inmunoenzimométrico con microplacas y tuvo duración de dos horas (sensibilidad funcional de 0.095 µUI/ml). Se determinó la concentración de T4L en sangre a través de inmunoensayo de enzima con micro-placas.
Para el análisis estadístico, se utilizó el programa SPSS versión 19 y se elaboraron estadísticas descriptivas y análisis bivariados como comparaciones de medias, tablas de contingencia con su respectiva prueba chi cuadrado y correlaciones de Pearson. Con esto, se logró describir la información resultante y validar las relaciones teóricas entre diferentes variables como la TSH y el colesterol total. Al comparar el comportamiento de las variables en hombres y mujeres, se requirió determinar si el procedimiento de comparación era paramétrico o no con el fin de verificar si existían diferencias significativas desde el punto de vista estadístico y llevar a cabo la comparación. Para esto se realizaron pruebas de distribución normal y de homocedasticidad; esta última se realizó para determinar si los datos poseían la misma varianza para los dos grupos. Se utilizó el estadístico Kolmogorov-Smirnov para testear normalidad en los datos, ya que el número de observaciones fue mayor de 50.
Por otra parte, se encontró que solo las variables colesterol total y colesterol-LDL presentaban distribución normal en ambos géneros, razón por la cual se procedió a realizar las correspondientes pruebas de homocedasticidad. Se trabajó con una significancia del 5% y debido a que la de este estadístico fue mayor a 0.05 para las variables colesterol total y colesterol-LDL en los dos géneros, se utilizó para estas dos variables el estadístico de Levene, cuya significancia dio también cifras mayores a 0.05, lo que confirmó homocedasticidad. Al resultar positivas para normalidad y para homocedasticidad, se eligió el estadístico t para comparar las dos variables por géneros. Respecto a las demás variables, se empleó la prueba no paramétrica u de Mann-Whitney, que se utiliza cuando una de las dos variables no cumple normalidad u homocedasticidad. Ambas pruebas se usaron con el fin de comparar los promedios entre dos grupos.
Resultados
En las pruebas de comparación, trabajando con una significancia del 5%, se observó que en la mayoría de las variables la significancia fue mayor a 0.05 y solo fue menor a este valor en el colesterol-HDL y el riesgo ateroesclerótico. Del mismo modo, se pudo deducir que los promedios son diferentes para ambos géneros respecto a estas dos variables.
El valor promedio del nivel de colesterol-HDL y el nivel de riesgo ateroesclerótico presentan diferencias estadísticamente significativas entre los géneros, siendo significativamente más elevado el valor promedio de colesterol-HDL en las mujeres. Esto establece una mayor protección vascular en el género femenino, lo que genera que el nivel de riesgo ateroesclerótico presente un valor promedio significativamente más elevado para los hombres —referencia normal en varones <5 y en mujeres <4.5, según ATPII—. Con los resultados obtenidos se concluye que los hombres poseen mayor riesgo ateroesclerótico (5.28) que las mujeres (4.47) mientras que el resto de variables se comportan de igual manera en ambos géneros.
Para analizar el comportamiento del índice de masa corporal (IMC) entre eutiroideos, hipotiroideos clínicos y subclínicos, se elaboró una tabla de contingencia, pues las dos variables a estudiar no son numéricas sino categóricas; esta tabla permitió determinar la no dependencia estadística entre las variables IMC e hipotiroidismo (p=0.73).
Se realizó el análisis entre el IMC frente a pacientes en tratamiento con hipolipemiante y pacientes sin tratamiento. Se detectó una significancia mayor a 0.05, es decir, no hubo diferencias entre pacientes con tratamiento hipolipemiante y pacientes sin tratamiento respecto a IMC. Con la prueba chi cuadrado se concluyó que las diferencias no son estadísticamente significativas y que el IMC se comporta de igual forma en pacientes dislipidémicos medicados y no medicados con hipolipemiante. Para realizar el análisis total de las variables cuantitativas se empleó la matriz de correlación de Pearson y no se encontró asociación entre las variables de interés.
La presencia de hipotiroidismo clínico en los participantes es muy baja (2 de 206; 0.97%), lo que evidencia que las diferentes dislipidemias en los demás pacientes no son causadas por la baja producción de la hormona T4L. De los 2 clasificados como hipotiroideos clínicos, 1 tiene niveles elevados de TSH (32.65 µUI/ml). Estos dos participantes presentan niveles de colesterol-HDL de 42 mg/dl y son reconocidos como dislipidémicos para colesterol-HDL en la referencia comercial (normal >60 mg/dl), pero normales para la referencia ATP III (≥40mg/dl). La presencia de ocho participantes con niveles de TSH por encima del nivel de referencia normal y con niveles de T4L normales los clasifica en la categoría de hipotiroidismo subclínico. Se pudo establecer que las diferentes dislipidemias encontradas en la mayoría de los participantes (199 de 206) no son consecuencia del hipotiroidismo subclínico.
Se encontró que los ocho participantes con hipotiroidismo subclínico manifestaron algún tipo de dislipidemia. 7 de 8 hipotiroideos subclínicos presentaron hipercolesterolemia tanto para el valor de referencia comercial como para el valor de referencia ATPIII. 4 de 8 hipotiroideos subclínicos presentaron elevadas cifras de triglicéridos para referencia comercial y 2, para referencia ATPIII. En cuanto al colesterol-HDL, 3 de 8 pacientes presentaron dislipidemia por bajas concentraciones de HDL según la referencia comercial y 1, en la referencia ATPIII. En lo que corresponde al colesterol VLDL, 1 de los 8 hipotiroideos subclínicos presentaron elevada concentración (>40 mg/dl) y en el colesterol-LDL, 7 de los 8 pacientes presentaron elevadas concentraciones: 5 en la categoría muy alto (>190 mg/dl) y 2 en la categoría alto (entre 160 y 189 mg/dl), según la referencia ATPIII. En cuanto al colesterol no HDL —correspondiente a la suma de VLDL y LDL— 6 de los 8 hipotiroideos subclínicos presentaron rangos elevados (referencia <189 mg/dl).
Debido al reducido número de participantes con HSC, no se puede confirmar la posible relación entre la elevación de las diferentes categorías lipídicas sanguíneas y este.
La edad promedio que presentó hipotiroidismo clínico fue de 66.5 años, mientras que en el hipotiroidismo subclínico fue de 61.88 años. Se encontró un promedio de peso normal en hipotiroidismo clínico, mientras que en hipotiroidismo subclínico y eutiroideos se encontró sobrepeso. Los niveles de colesterol en hipotiroidismo subclínico presentaron promedios, valores mínimos y máximos superiores al hipotiroidismo clínico. Al comparar hipotiroidismo subclínico con eutiroideos, se encuentran valores máximos muy similares; a pesar de lo anterior, los valores mínimos y el promedio en hipotiroidismo subclínico son más elevados.
En cuanto a los niveles de triglicéridos, los valores mínimos son superiores en el hipotiroidismo clínico respecto al subclínico y, a su vez, este es más elevado que en los eutiroideos. Sin embargo, los valores máximos y promedios más elevados se encontraron en eutiroideos y los valores máximos menos elevados se ubicaron en el hipotiroidismo clínico.
Respecto al colesterol-HDL, se presenta el mínimo menos elevado en los eutiroideos y el más elevado en los hipotiroideos clínicos. No obstante, los máximos más elevados se encontraron en los eutiroideos y los menos elevados en el hipotiroidismo clínico.
En relación al colesterol-LDL, los promedios más elevados se encontraron en hipotiroidismo subclínico. A la vez, el promedio del riesgo aterogénico es más elevado en hipotiroidismo subclínico que en eutiroideos. Así, el riesgo más bajo está en hipotiroideos clínicos.
La Tabla 1 muestra los datos estadísticos descriptivos de acuerdo a la condición tiroidea, teniendo en cuenta la edad, el IMC, los niveles séricos de T4L y TSH, los niveles de perfil lipídico y el riesgo respectivo entre los participantes que resultaron normales con hipotiroidismo clínico en la evaluación de las hormonas T4L y TSH (T4L <0.8 ng/dl y TSH ≥6.14 µUI/ml).
Gracias al bajo número de observaciones en los pacientes denominados como clínicos, no fue posible emplear pruebas de normalidad a este grupo de datos. Por esto, se dificultó el análisis y se procedió entonces a agrupar las categorías clínico y subclínico en una sola categoría a fin de compararlas con los pacientes normales de las variables referentes al perfil de lípidos.
En el análisis se encontraron los siguientes resultados: el promedio, el valor mínimo y máximo de colesterol son más elevados en hipotiroidismo que en eutiroideos; los valores máximos y promedios más elevados de triglicéridos se presentaron en eutiroideos; los valores máximos y mínimos más elevados se observan en eutiroideos respecto a colesterol-HDL, y los valores máximos y mínimos promedios más elevados para el colesterol-LDL se observan en hipotiroideos agrupados. Por último, el promedio de riesgo aterogénico es levemente superior en hipotiroideos agrupados que en eutiroideos. La Tabla 2 muestra los datos estadísticos descriptivos para hipotiroidismo clínico y subclínico agrupado comparado con eutiroideos, teniendo en cuenta la edad, el IMC, los niveles séricos de T4L y TSH, los niveles de perfil lipídico y el riesgo respectivo.
Tabla 1. Estadísticos descriptivos de acuerdo a condición tiroidea.
|
Condición tiroidea |
Mínimo |
Máximo |
Media |
Desviación estándar |
|
|
Edad |
Eutiroideos |
35 |
89 |
57.51 |
10.277 |
|
Subclínico |
47 |
73 |
61.88 |
8.887 |
|
|
Clínico |
65 |
68 |
66.5 |
2.121 |
|
|
IMC |
Eutiroideos |
19.4 |
38.9 |
26.08 |
3.92 |
|
Subclínico |
21.2 |
34.5 |
25.16 |
4.32 |
|
|
Clínico |
21.8 |
22.6 |
22.2 |
0.57 |
|
|
T4L (ng/dl) |
Eutiroideos |
0.8 |
2.08 |
1.27 |
0.29 |
|
Subclínico |
0.86 |
1.79 |
1.21 |
0.31 |
|
|
Clínico |
0.53 |
0.66 |
0.6 |
0.1 |
|
|
TSH (µUI/ml) |
Eutiroideos |
- |
5.91 |
1.98 |
1.22 |
|
Subclínico |
6.22 |
15.83 |
8.52 |
3.24 |
|
|
Clínico |
4.9 |
32.65 |
18.78 |
19.63 |
|
|
COL (mg/dl) |
Eutiroideos |
123 |
378 |
239.52 |
48.02 |
|
Subclínico |
200 |
352 |
275.25 |
47.17 |
|
|
Clínico |
183 |
193 |
188 |
7.07 |
|
|
TG (mg/dl) |
Eutiroideos |
50 |
650 |
204.94 |
110.32 |
|
Subclínico |
92 |
233 |
155.88 |
51.99 |
|
|
Clínico |
119 |
152 |
135.5 |
23.33 |
|
|
HDL (mg/dl) |
Eutiroideos |
17 |
127 |
55.11 |
17.01 |
|
Subclínico |
32 |
76 |
60.88 |
16.2 |
|
|
Clínico |
42 |
42 |
42 |
- |
|
|
VLDL (mg/dl) |
Eutiroideos |
10 |
130 |
40.99 |
22.06 |
|
Subclínico |
18.4 |
46.6 |
31.18 |
10.4 |
|
|
Clínico |
23.8 |
30.4 |
27.1 |
4.67 |
|
|
LDL (mg/dl) |
Eutiroideos |
26.6 |
283.2 |
143.42 |
44.68 |
|
Subclínico |
92.4 |
243.8 |
183.2 |
44.96 |
|
|
Clínico |
110.6 |
127.2 |
118.9 |
11.74 |
|
|
Riesgo |
Eutiroideos |
1.94 |
17.47 |
4.7 |
1.72 |
|
Subclínico |
2.70 |
7.56 |
4.84 |
1.51 |
|
|
Clínico |
4.36 |
4.6 |
4.48 |
0.17 |
|
Fuente: Elaboración propia.
Tabla 2. Estadísticos descriptivos para hipotiroidismo clínico y subclínico agrupado comparado con eutiroideos.
|
Hipotiroidismo agrupado |
Media |
Desviación estándar |
Coeficiente de variación |
Mínimo |
Máximo |
n |
|
|
Edad |
Eutiroideo |
57.51 |
10.28 |
18% |
35 |
89 |
196 |
|
Subclínico y Clínico |
62.8 |
8.11 |
13% |
47 |
73 |
10 |
|
|
IMC |
Eutiroideo |
26.08 |
3.92 |
15% |
19.4 |
38.9 |
196 |
|
Subclínico y Clínico |
24.57 |
4.01 |
16% |
21.2 |
34.5 |
10 |
|
|
T4L |
Eutiroideo |
1.27 |
0.29 |
23% |
0.8 |
2.08 |
196 |
|
Subclínico y Clínico |
1.09 |
0.38 |
35% |
0.53 |
1.79 |
10 |
|
|
TSH |
Eutiroideo |
1.98 |
1.22 |
61% |
0 |
5.91 |
196 |
|
Subclínico y Clínico |
10.57 |
8.35 |
79% |
4.9 |
32.65 |
10 |
|
|
COL |
Eutiroideo |
239.52 |
48.02 |
20% |
123 |
378 |
196 |
|
Subclínico y Clínico |
257.8 |
55.59 |
22% |
183 |
352 |
10 |
|
|
TG |
Eutiroideo |
204.94 |
110.32 |
54% |
50 |
650 |
196 |
|
Subclínico y Clínico |
151.8 |
47.29 |
31% |
92 |
233 |
10 |
|
|
HDL |
Eutiroideo |
55.11 |
17.01 |
31% |
17 |
127 |
196 |
|
Subclínico y Clínico |
57.1 |
16.35 |
29% |
32 |
76 |
10 |
|
|
VLDL |
Eutiroideo |
40.99 |
22.06 |
54% |
10 |
130 |
196 |
|
Subclínico y Clínico |
30.36 |
9.46 |
31% |
18.4 |
46.6 |
10 |
|
|
LDL |
Eutiroideo |
143.42 |
44.68 |
31% |
26.6 |
283.2 |
196 |
|
Subclínico y Clínico |
170.34 |
48.19 |
28% |
92.4 |
243.8 |
10 |
|
|
Riesgo |
Eutiroideo |
4.7 |
1.72 |
37% |
1.94 |
17.47 |
196 |
|
Subclínico y Clínico |
4.77 |
1.34 |
28% |
2.7 |
7.56 |
10 |
|
Fuente: Elaboración propia.
Se realizaron pruebas de normalidad y homocedasticidad con el fin de determinar los procedimientos para realizar comparación. Para testear normalidad se utilizaron los estadísticos de Kolmogorov-Smirnov (muestras ≥50) y de Shapiro-Wilk (muestras <50); como las muestras para hipotiroideos fueron menores a 50, se trabajó con el segundo. Se requirió determinar si el proceso de comparación de comportamiento de las variables entre hipotiroidismo agrupado y eutiroidismo era o no paramétrico. Esto, para verificar si existen diferencias significativas desde el punto de vista estadístico y llevar a cabo la comparación, por lo que se realizaron pruebas de distribución normal y de homocedasticidad.
La homocedasticidad tenía el fin de señalar si los datos poseían la misma varianza para los dos grupos. Se utilizó el estadístico Kolmogorov-Smirnov para testear normalidad en la información de eutiroidismo, dado que el número de observaciones de esta variable fue mayor a 50. El estadístico Shapiro-Wilk se utilizó para hipotiroidismo agrupado, ya que el número de datos de esta variable fue inferior a 50. En la comparación entre la categoría eutiroideos y los hipotiroideos agrupados, se encontraron evidentes diferencias entre los promedios de las variables TSH, colesterol total y colesterol-LDL, lo que quiere decir que estas variables son significativamente más elevadas en pacientes hipotiroideos agrupados que en pacientes eutiroideos.
Discusión
Se ha descrito que personas con elevada concentración de TSH en suero y resistencia a la insulina presentan mayor riesgo de desarrollar dislipidemia (15,21). Además, existe evidencia de que los niveles de TSH por encima del rango de referencia normal se correlacionan de manera positiva con el colesterol sérico total (8) y el colesterol-LDL y se asocian negativamente con el colesterol-HDL (9); en ese sentido, disminuyen la concentración del colesterol total y colesterol-LDL después de realizarse tratamiento con tiroxina en individuos con referencia de TSH por encima de 10 μU/ml (10).
En lo que respecta al metabolismo de lípidos y gracias a la disminución en la síntesis de receptores LDL, las concentraciones de T4L siempre se encuentran inversamente asociadas con las concentraciones de colesterol total y colesterol-LDL (22). La administración de levotiroxina tiene un efecto hipolipidémico en el paciente hipotiroideo con elevadas concentraciones de TSH, hormona destinada a compensar los bajos niveles de T4L. Sin embargo, se presenta dificultad para identificar el corte umbral de asociación entre TSH y lípidos (18).
Se ha establecido que el 4.3% de los pacientes hipercolesterolémicos han sido reportados como hipotiroideos (19). Así mismo, un factor contribuyente a que los niveles de colesterol se presenten elevados en hipotiroidismo es la presencia de niveles bajos de T3L. Bajo condiciones normales, el T3L tiene control sobre la proteína -1 de unión al elemento regulador de esteroles (SREBP-1), un importante paso para la expresión del receptor LDL. No obstante, a diferencia de SREBP-2 (22), el T3L también actúa de forma directa e induce al menos dos tipos de receptores LDL a través de elementos de respuesta a tiroxina (ERT) en el hígado (23). Además, el T3L y el T4L inducen aumento en la secreción de sales biliares, lo que incide en la disminución de los niveles de colesterol plasmáticos, debido al incremento de las necesidades de colesterol proveniente de las lipoproteínas para la síntesis de sales biliares. Sin embargo, este efecto es contrarrestado por un incremento en la síntesis de colesterol endógeno (24).
Por otra parte, la relación entre el funcionamiento de la tiroides y el síndrome metabólico se ha convertido en un tema de interés a investigar en los últimos años (25) y, con base en lo antes mencionado, se puede concluir que los niveles bajos de T4L contribuyen a aumentar el riesgo cardiovascular asociado con anormalidades en el perfil lipídico en personas con síndrome metabólico (26). Es importante mencionar que la edad no parece afectar los niveles de T3L y de T4L en el ser humano (27).
En algunas investigaciones se ha encontrado relación entre la disfunción tiroidea y la disfunción lipídica en pacientes con diabetes tipo 2. Esta relación no se tiene en cuenta en el manejo clínico de pacientes con diabetes mellitus, ya que la respuesta de la proteína de unión al elemento de respuesta al carbohidrato (Ch-REBP) —un nuevo factor de transcripción identificado y sensible a la glucosa que controla lipogénesis hepática— es controlado positivamente por T3L en mamíferos a través de su unión al receptor β1 de la tiroides (28).
En el presente trabajo se encontró una prevalencia relativamente baja de hipotiroidismo clínico (2/206=0.97%), lo que coincide con los datos obtenidos por otros autores en los que se evidencia que el hipotiroidismo en la población general es del 2% en mujeres y del 0.01% en varones (29).
Algunos investigadores han encontrado que, en general, la prevalencia de hipotiroidismo subclínico oscila del 1% al 10% según las fuentes, la edad y el nivel de corte de la prueba TSH y que la prevalencia es más alta en mujeres mayores de 60 años y tiende a igualarse en ambos géneros a partir de los 75 años (30). La presente investigación se correlaciona con esta prevalencia, pues se encuentra dentro del intervalo del 1% al 10% de la muestra (8/206=3.88%). En cuanto a género, de los 9 pacientes que presentaron TSH >6.16 μUI/ml, 5 corresponden al género femenino (5/206=2.42%) y 3 al género masculino (3/206=1.45%). Esto concuerda con una mayor prevalencia en el género femenino y en las edades de los pacientes con hipotiroidismo subclínico que oscilan entre los 47 y los 73 años.
Según estudios realizados por Cooper (31), cerca del 20% de pacientes con TSH >6 μUI/m desarrollarán hipotiroidismo clínico en los cinco años siguientes, siendo la progresión a hipotiroidismo el manifiesto más frecuente si el valor inicial de TSH es >10 μUI/m (31). En el presente estudio, se encontraron tres valores >10 μUI/m (muestras 12, 124 y 178), correspondientes al 1.46% de la muestra (3/206=1.46%) y al 33.33% de los pacientes pertenecientes a la muestra —cuyo dato numérico de TSH fue >6 μUI/m (3/9=33.33%)—, los cuales podrían presentar hipotiroidismo manifiesto en los próximos cinco años.
La informaciòn obtenida apoya la recomendación de los expertos de la Asociación Americana de Tiroides sobre el cribaje para disfunción tiroidea en adultos mayores de 35 años mediante un examen de TSH cada cinco años, ya que se observó una elevada prevalencia de hipotiroidismo subclínico tanto en hombres como en mujeres que puede progresar a hipotiroidismo clínico y que puede estar asociado a hipercolesterolemia y deterioro cognitivo. Además, con el paso de los años pueden presentarse disfunciones tiroideas no detectadas en la exploración clínica (32).
La prevalencia del hipotiroidismo subclínico de entre el 3% y el 10% de la población general encontrada por Moradian (33) concuerda en el presente trabajo con la población dislipidémica; sin embrago, en ese caso la prevalencia no fue mayor en el género femenino: se presentó en iguales proporciones en los dos géneros, con un valor máximo más elevado en varones (32.7 µUI/ml) que en mujeres (15.8 µUI/ml).
Los datos encontrados en los pacientes dislipidémicos concuerdan con los del estudio de Hernández et al. (34) en lo que respecta a TSH, en donde se encontró una relación moderada entre TSH con las manifestaciones metabólicas. La totalidad de los pacientes con HSC fueron positivos para algún tipo de dislipidemia, sin lograr apreciar la efectividad del tratamiento hipolipemiante, ya que 7 de los 8 pacientes con HSC habían abandonado el tratamiento medicamentoso hipolipemiante. Solo 1 de los 8 pacientes con HSC presentó cifras elevadas en el perfil lipídico, a pesar de no haber abandonado el tratamiento.
Cabe anotar que ninguno de los pacientes presentaba evaluación paraclínica de TSH y, por tanto, era desconocido el diagnóstico de HSC. La mayoría de los pacientes que presentaron HSC se encontraban en edades superiores a los 54 años de edad, lo que concuerda con lo observado en pacientes españoles (35). Sin embargo, en la presente investigación, uno de los pacientes con HSC de género masculino de 49 años de edad presentó antecedentes de exposición temprana a radiaciones ionizantes en la zona de cabeza y cuello.
Conclusiones
La frecuencia de hipotiroidismo subclínico es superior a la frecuencia de hipotiroidismo clínico en pacientes dislipidémicos, pero esta disminución de hormonas tiroideas no es la causa de las alteraciones del perfil lipídico en la mayoría de los participantes (95.7%). A su vez, el IMC y el hipotiroidismo, tanto clínico como subclínico, se comportan de igual manera entre eutiroideos, hipotiroideos clínicos y subclínicos. No hay evidencia de una fuerte relación entre las variables del perfil lipídico y el perfil tiroideo.
En patologías relacionadas con el metabolismo de lípidos, es indispensable la realización de valoraciones paraclínicas de TSH y T4L antes de indicar un tratamiento medicamentoso hipolipemiante. Además, pacientes sometidos a tratamientos periódicos con radiaciones ionizantes deben tener un seguimiento del perfil tiroideo a través del tiempo para prevenir complicaciones del metabolismo lipídico. En hombres y mujeres mayores de 35 años y con alteraciones en el metabolismo de lípidos se deben valorar los niveles de TSH, ya que, por lo regular, los pacientes con HSC pueden presentar este tipo de alteraciones. Estos resultados podrían ser de ayuda para la evaluación de respuesta al tratamiento. Es importante también que en pacientes dislipidémicos en general se realicen cribados tiroideos a fin de evitar complicaciones clínicas inherentes al hipotiroidismo clínico o subclínico.
Por último, se deben realizar estudios de tamizaje de HSC en otras ciudades de Colombia, pues la prevalencia de este depende de varios aspectos, entre ellos la ubicación geográfica. A la vez, estas investigaciones en otras regiones deben incluir una mayor cantidad de pacientes para detectar alteraciones tiroideas y prevenir la aparición de complicaciones relacionadas de esta manera.
Conflicto de intereses
Ninguno declarado por los autores.
Financiación
El trabajo se realizó con recursos de la Universidad de Caldas.
Agradecimientos
A la IPS Médicos Internistas de Caldas, donde se realizó el muestreo del presente trabajo.
Referencias
1. Klein I, Ojamaa K. Thyroid hormone and the cardiovascular system. Curr. Opin. Endocrinol. Diabetes Obes. 1997;4(5):341-6. http://doi.org/fvpnc6.
2. Biondi B, Palmieri EA, Lombardi G, Fazio S. Effects of subclinical thyroid dysfunction on the heart. Ann. Intern. Med. 2002;137(11):904-14. http://doi.org/bt78.
3. Biondi B. Cardiovascular effects of mild hypothyroidism. Thyroid. 2007;17(7):625-30. http://doi.org/dbchrd.
4. Feldt-Rasmussen U. Is the treatment of subclinical hypothyroidism beneficial? Nat. Rev. Endocrinol. 2009;5(2):86-7. http://doi.org/d3522x.
5. Reaven GM. Role of insulin resistance in human disease. Diabetes. 1988;37(12):1595-607. http://doi.org/bm28.
6. Mykkänen L, Haffner SM, Rönnemaa T, Bergman RN, Laakso M. Low insulin sensitivity is associated with clustering of cardiovascular disease risk factors. Am. J. Epidemiol. 1997;146(4):315-21. http://doi.org/bvdd.
7. Genest J Jr, Cohn JS. Clustering of cardiovascular risk factors: targeting high-risk individuals. Am. J. Cardiol. 1995;76(2):8A-20A. http://doi.org/bs2bdv.
8. Pallas D, Koutras DA, Adamopoulos P, Marafelia P, Souvatzoglou A, Piperingos G, et al. Increased mean serum thyrotropin in apparently euthyroidhypercholesterolemic patients: does it mean occult hypothyroidism? J. Endocrinol. Invest. 1991;14(9):743-6. http://doi.org/bvdf.
9. Bakker SJ, ter Maaten JC, Popp-Snijders C, Slaets JP, Heine RJ, Gans RO. The relationship between thyrotropin and low density lipoprotein cholesterol is modified by insulin sensitivity in healthy euthyroid subjects. J. Clin. Endocrinol. Metab. 2001;86(3):1206-11. http://doi.org/bvdg.
10. Michalopoulou G, Alevizaki M, Piperingos G, Mitsibounas D, Mantzos E, Adamopoulos P, et al. High serum cholesterol levels in persons with “high-normal” TSH levels: should one extend the definition of subclinical hypothyroidism? Eur. J. Endocrinol. 1998;138(2):141-5. http://doi.org/fqqcf7.
11. Ayala A, Danese M, Ladenson P. When to treat mild hypothyroidism. Endocrinol. Metabol. Clin. North Am. 2000;29(2):399-415. http://doi.org/cwcq9t.
12. Paoli-Valeri M, Mamán-Alvarado D, Jiménez-López V, Arias-Ferreira A, Bianchi G, Arata-Bellabarba G. Frecuencia de hipotiroidismo subclínico en niños sanos y con alteraciones neurológias en el estado Mérida-Venezuela. Invest. Clín. 2003;44(3):209-18.
13. Karlin NJ, Weintraub N, Chopra IJ. Current controversies in endocrinology: screening of asymptomatic elderly for subclinical hypothyroidism. J. Am. Med. Dir. Assoc. 2004;5(5):333-6. http://doi.org/dtpwdh.
14. Díez JJ, Iglesias P, Burman KD. Spontaneous normalization of thyrotropin concentrations in patients with subclinical hypothyroidism. J. Clin. Endocrinol. Metab. 2005;90(7):4124-7. http://doi.org/b632v4.
15. Chubb SAP, Davis WA, Davis TME. Interactions among thyroid function, insulin sensitivity, and serum lipid concentrations: the Fremantle diabetes study. J. Clin. Endocrinol. Metab. 2005;90(9):5317-20. http://doi.org/dn3cm2.
16. Strollo F, Carucci I, Morè M, Marico G, Strollo G, Masini MA, et al. Free triiodothyronine and cholesterol levels in euthyroid elderly T2DM patients. Int. J. Endocrinol. 2012;2012:1-7. http://doi.org/bvhb.
17. Celi FS, Zemskova M, Linderman JD, Smith S, Drinkard B, Sachdev V, et al. Metabolic effects of Liothyronine Therapy in hypothyroidism: a randomized, double-blind, crossover trial of Liothyronine versus Levothyroxine. J. Clin. Endocrinol. Metab. 2011;96(11):3466-74. http://doi.org/bmp48h.
18. Barbagallo CM, Averna MR, Liotta A, La Grutta S, Maggio C, Casimiro L, et al. Plasma levels of lipoproteins and apolipoproteins in congenital hypothyroidism: effects of l-thyroxine substitution therapy. Metabolism. 1995;44(10):1283-7. http://doi.org/ffd294.
19. Tagami T, Madison LD, Nagaya T, Jameson JL. Nuclear receptor corepressors activate rather than suppress basal transcription of genes that are negatively regulated by thyroid hormone. Mol. Cell. Biol. 1997;17(5):2642-8.http://doi.org/bvdh.
20. Tong PC, Kong AP, So WY, Yang X, Ho CS, Ma RC, et al. The usefulness of the International Diabetes Federation and the National Cholesterol Education Program’s Adult Treatment Panel III definitions of the metabolic syndrome in predicting coronary heart disease in subjects with type 2 diabetes. Diabetes Care. 2007;30(5):1206-11.http://doi.org/c985s4.
21. Risal P, Maharjan BR, Koju R, Makaju RK, Gautam M. Variation of total serum cholesterol among the patient with thyroid dysfunction. Kathmandu Univ. Med. J. 2010;8(30):265-8.http://doi.org/c7g9qp.
22. Gnoni GV, Rochira A, Leone A, Damiano F, Marsigliante S, Siculella L. 3,5,3’triiodo-L-thyronine induces SREBP-1 expression by non-genomic actions in human HEP G2 cells. J. Cell. Physiol. 2012;227(6):2388-97. http://doi.org/dwbhhn.
23. Lopez D, Abisambra-Socarrás JF, Bedi M, Ness GC. Activation of the hepatic LDL receptor promoter by thyroid hormone. Biochim. Biophys. Acta. 2007;1771(9):1216-25. http://doi.org/c8sggj.
24. Walton KW, Scott PJ, Dykes PW, Davies JW. The significance of alterations in serum lipids in thyroid dysfunction. II. Alterations of the metabolism and turnover of 131-I-low-density lipoproteins in hypothyroidism and thyrotoxicosis. Clin. Sci. 1965;29(2):217-38.
25. Kumar HK, Yadav RK, Prajapati J, Reddy CV, Raghunath M, Modi KD. Association between thyroid hormones, insulin resistance, and metabolic syndrome. Saudi Med. J. 2009;30(7):907-11.
26. Taneichi H, Sasai T, Ohara M, Honma H, Nagasawa K, Takahashi T, et al. Higher serum free triiodothyronine levels within the normal range are associated with metabolic syndrome components in type 2 diabetic subjects with euthyroidism. Tohoku J. Exp. Med. 2011;224(3):173-8. http://doi.org/bkbp4b.
27. Kadiyala R, Peter R, Okosieme OE. Thyroid dysfunction in patients with diabetes: clinical implications and screening strategies. Int. J. Clin. Pract. 2010;64(8):1130-9. http://doi.org/dcd765.
28. Iizuka K, Takeda J, Horikawa Y. Glucose induces FGF21 mRNA expression through ChREBP activation in rat hepatocytes. FEBS Lett. 2009;583(17):2882-6. http://doi.org/fgbgr3.
29. Ortiz-Pérez L, de la Espriella M. Thyroid hormones and mood disorders. Rev. Colomb. Psiquiatr. 2004;33(1):98-107.
30. Attia J, Margetts P, Guyatt G. Diagnosis of thyroid disease in hospitalized patients: a systematic review. Arch. Intern. Med. 1999;159(7):658-65. http://doi.org/fk6pjh.
31. Cooper DS. Subclinical hypothyroidism. N. Eng. J. Med. 2001;345(4):260-5. http://doi.org/cgk8qc.
32. Papaleontiou M, Haymart MR. Approach to and treatment of thyroid disorders in the elderly. Med. Clin. North Am. 2012;96(2):297-310. http://doi.org/bvdj.
33. Mooradian AD. Subclinical hypothyroidism in the elderly: to treat or not to treat? Am. J. Ther. 2011;18(6):477-86. http://doi.org/bqkcz6.
34. Hernández A, López LE, Hernández A, Mesa A. Hipotiroidismo subclínico en el anciano ambulatorio. Rev. Biomed. 2007;18(3):162-6.
35. Medicina Interna de Galicia. Lugo: Sociedad Gallega de Medicina interna; 2016 [cited 2016 Dic 6]. De Suárez B. Hipotiroidismo subclínico: ¿controversia o consenso? Available from: http://goo.gl/HzkXH0.
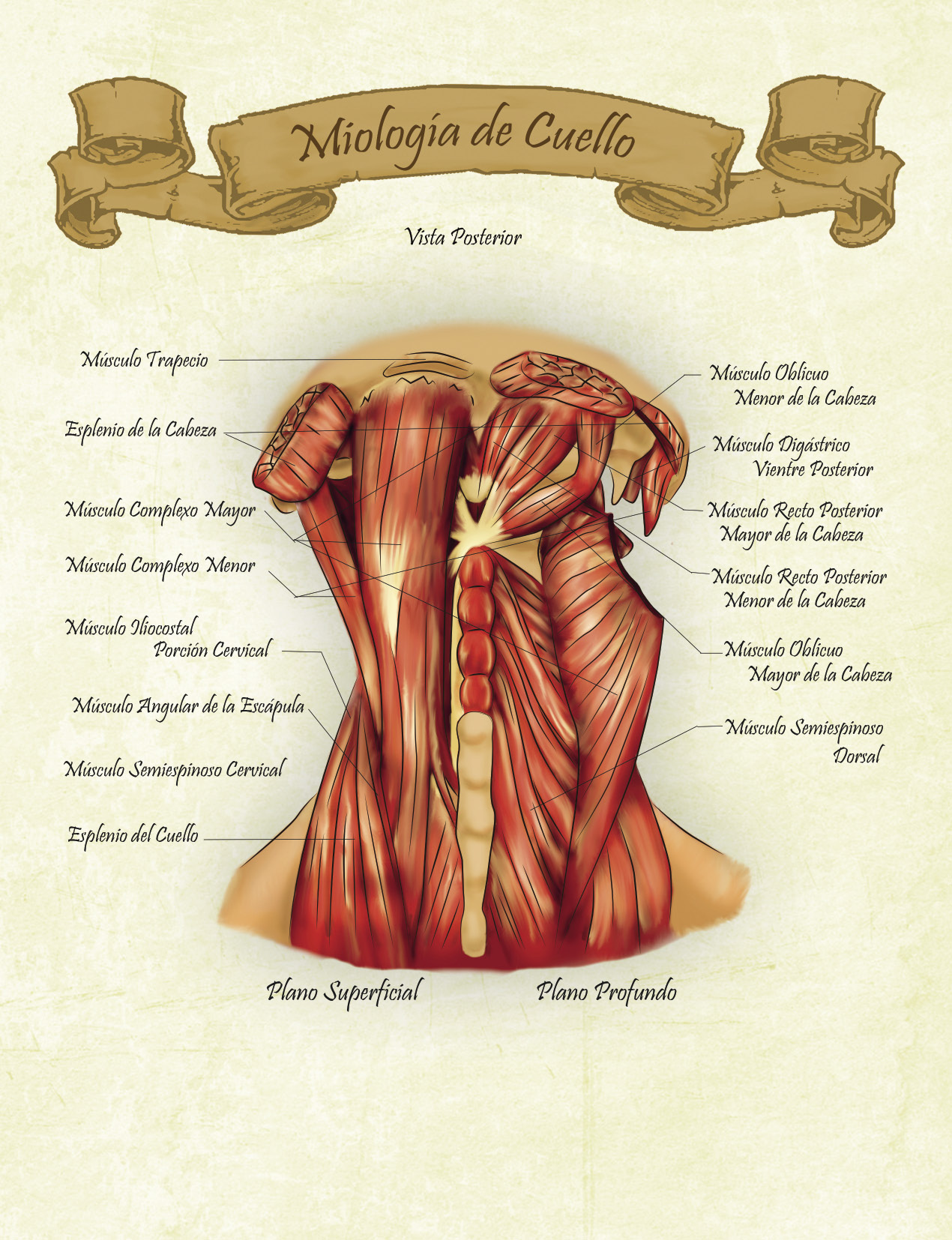
César Alexander Eslava Franco
“Mapas anatómicos”
Universidad Nacional de Colombia
Referencias
Klein I, Ojamaa K. Thyroid hormone and the cardiovascular system. Curr. Opin. Endocrinol. Diabetes Obes. 1997;4(5):341-6. http://doi.org/fvpnc6.
Biondi B, Palmieri EA, Lombardi G, Fazio S. Effects of subclinical thyroid dysfunction on the heart. Ann. Intern. Med. 2002;137(11):904- 14. http://doi.org/bt78.
Biondi B. Cardiovascular effects of mild hypothyroidism. Thyroid. 2007;17(7):625-30. http://doi.org/dbchrd.
Feldt-Rasmussen U. Is the treatment of subclinical hypothyroidism beneficial? Nat. Rev. Endocrinol. 2009;5(2):86-7. http://doi.org/d3522x.
Reaven GM. Role of insulin resistance in human disease. Diabetes. 1988;37(12):1595-607. http://doi.org/bm28.
Mykkänen L, Haffner SM, Rönnemaa T, Bergman RN, Laakso M. Low insulin sensitivity is associated with clustering of cardiovascular disease risk factors. Am. J. Epidemiol. 1997;146(4):315-21. http://doi.org/bvdd.
Genest J Jr, Cohn JS. Clustering of cardiovascular risk factors: targeting high- risk individuals. Am. J. Cardiol. 1995;76(2):8A-20A. http://doi.org/bs2bdv.
Pallas D, Koutras DA, Adamopoulos P, Marafelia P, Souvatzoglou A, Piperingos G, et al. Increased mean serum thyrotropin in apparently euthyroidhypercholesterolemic patients: does it mean occult hypothyroidism? J. Endocrinol. Invest. 1991;14(9):743-6. http://doi.org/bvdf.
Bakker SJ, ter Maaten JC, Popp-Snijders C, Slaets JP, Heine RJ, Gans RO. The relationship between thyrotropin and low density lipoprotein cholesterol is modified by insulin sensitivity in healthy euthyroid subjects. J. Clin. Endocrinol. Metab. 2001;86(3):1206-11. http://doi.org/bvdg.
Michalopoulou G, Alevizaki M, Piperingos G, Mitsibounas D, Mantzos E, Adamopoulos P, et al. High serum cholesterol levels in persons with “high- normal” TSH levels: should one extend the definition of subclinical hypothyroidism? Eur. J. Endocrinol. 1998;138(2):141-5. http://doi.org/fqqcf7.
Ayala A, Danese M, Ladenson P. When to treat mild hypothyroidism. Endocrinol. Metabol. Clin. North Am. 2000;29(2):399-415. http://doi.org/cwcq9t.
Paoli-Valeri M, Mamán-Alvarado D, Jiménez-López V, Arias-Ferreira A, Bianchi G, Arata-Bellabarba G. Frecuencia de hipotiroidismo subclínico en niños sanos y con alteraciones neurológias en el estado Mérida-Venezuela. Invest. Clín. 2003;44(3):209-18.
Karlin NJ, Weintraub N, Chopra IJ. Current controversies in endocrinology: screening of asymptomatic elderly for subclinical hypothyroidism. J. Am. Med. Dir. Assoc. 2004;5(5):333-6. http://doi.org/dtpwdh.
Díez JJ, Iglesias P, Burman KD. Spontaneous normalization of thyrotropin concentrations in patients with subclinical hypothyroidism. J. Clin. Endocrinol. Metab. 2005;90(7):4124-7. http://doi.org/b632v4.
Chubb SAP, Davis WA, Davis TME. Interactions among thyroid function, insulin sensitivity, and serum lipid concentrations: the Fremantle diabetes study. J. Clin. Endocrinol. Metab. 2005;90(9):5317-20. http://doi.org/dn3cm2.
Strollo F, Carucci I, Morè M, Marico G, Strollo G, Masini MA, et al. Free triiodothyronine and cholesterol levels in euthyroid elderly T2DM patients. Int. J. Endocrinol. 2012;2012:1-7. http://doi.org/bvhb.
Celi FS, Zemskova M, Linderman JD, Smith S, Drinkard B, Sachdev V, et al. Metabolic effects of Liothyronine Therapy in hypothyroidism: a randomized, double-blind, crossover trial of Liothyronine versus Levothyroxine. J. Clin. Endocrinol. Metab. 2011;96(11):3466-74. http://doi.org/bmp48h.
Barbagallo CM, Averna MR, Liotta A, La Grutta S, Maggio C, Casimiro L, et al. Plasma levels of lipoproteins and apolipoproteins in congenital hypothyroidism: effects of l-thyroxine substitution therapy. Metabolism. 1995;44(10):1283-7. http://doi.org/ffd294.
Tagami T, Madison LD, Nagaya T, Jameson JL. Nuclear receptor corepressors activate rather than suppress basal transcription of genes that are negatively regulated by thyroid hormone. Mol. Cell. Biol. 1997;17(5):2642-8.http://doi.org/bvdh.
Tong PC, Kong AP, So WY, Yang X, Ho CS, Ma RC, et al. The usefulness of the International Diabetes Federation and the National Cholesterol Education Program’s Adult Treatment Panel III definitions of the metabolic syndrome in predicting coronary heart disease in subjects with type 2 diabetes. Diabetes Care. 2007;30(5):1206-11.http://doi.org/c985s4.
Risal P, Maharjan BR, Koju R, Makaju RK, Gautam M. Variation of total serum cholesterol among the patient with thyroid dysfunction. Kathmandu Univ. Med. J. 2010;8(30):265-8.http://doi.org/c7g9qp.
Gnoni GV, Rochira A, Leone A, Damiano F, Marsigliante S, Siculella L. 3,5,3’triiodo-L-thyronine induces SREBP-1 expression by non-genomic actions in human HEP G2 cells. J. Cell. Physiol. 2012;227(6):2388- 97. http://doi.org/dwbhhn.
Lopez D, Abisambra-Socarrás JF, Bedi M, Ness GC. Activation of the hepatic LDL receptor promoter by thyroid hormone. Biochim. Biophys. Acta. 2007;1771(9):1216-25. http://doi.org/c8sggj.
Walton KW, Scott PJ, Dykes PW, Davies JW. The significance of alterations in serum lipids in thyroid dysfunction. II. Alterations of the metabolism and turnover of 131-I-low-density lipoproteins in hypothyroidism and thyrotoxicosis. Clin. Sci. 1965;29(2):217-38.
Kumar HK, Yadav RK, Prajapati J, Reddy CV, Raghunath M, Modi KD. Association between thyroid hormones, insulin resistance, and metabolic syndrome. Saudi Med. J. 2009;30(7):907-11.
Taneichi H, Sasai T, Ohara M, Honma H, Nagasawa K, Takahashi T, et al. Higher serum free triiodothyronine levels within the normal range are associated with metabolic syndrome components in type 2 diabetic subjects with euthyroidism. Tohoku J. Exp. Med. 2011;224(3):173-8. http://doi.org/bkbp4b.
Kadiyala R, Peter R, Okosieme OE. Thyroid dysfunction in patients with diabetes: clinical implications and screening strategies. Int. J. Clin. Pract. 2010;64(8):1130-9. http://doi.org/dcd765.
Iizuka K, Takeda J, Horikawa Y. Glucose induces FGF21 mRNA expression through ChREBP activation in rat hepatocytes. FEBS Lett. 2009;583(17):2882-6. http://doi.org/fgbgr3.
Ortiz-Pérez L, de la Espriella M. Thyroid hormones and mood disorders. Rev. Colomb. Psiquiatr. 2004;33(1):98-107.
Attia J, Margetts P, Guyatt G. Diagnosis of thyroid disease in hospitalized patients: a systematic review. Arch. Intern. Med. 1999;159(7):658-65. http://doi.org/fk6pjh.
Cooper DS. Subclinical hypothyroidism. N. Eng. J. Med. 2001;345(4):260- 5. http://doi.org/cgk8qc.
Papaleontiou M, Haymart MR. Approach to and treatment of thyroid disorders in the elderly. Med. Clin. North Am. 2012;96(2):297-310. http://doi.org/bvdj.
Mooradian AD. Subclinical hypothyroidism in the elderly: to treat or not to treat? Am. J. Ther. 2011;18(6):477-86. http://doi.org/bqkcz6.
Hernández A, López LE, Hernández A, Mesa A. Hipotiroidismo subclínico en el anciano ambulatorio. Rev. Biomed. 2007;18(3):162-6. 35. Medicina Interna de Galicia. Lugo: Sociedad Gallega de Medicina interna; 2016 [cited 2016 Dic 6]. De Suárez B. Hipotiroidismo subclínico: ¿controversia o consenso? Available from: http://goo.gl/HzkXH0.
Medicina Interna de Galicia. Lugo: Sociedad Gallega de Medicina in-terna; 2016 [cited 2016 Dic 6]. De Suárez B. Hipotiroidismo subclínico: ¿controversia o consenso? Available from: http://goo.gl/HzkXH0
Cómo citar
APA
ACM
ACS
ABNT
Chicago
Harvard
IEEE
MLA
Turabian
Vancouver
Descargar cita
Licencia
Derechos de autor 2017 Revista de la Facultad de Medicina

Esta obra está bajo una licencia Creative Commons Reconocimiento 3.0 Unported.
-





















