Uso de instrumentos clínicos para la evaluación de pacientes y resultados de tratamiento en trastornos por uso de sustancias (TUS)
Using clinical tools for assessing patients and treatment outcomes for Substance Use Disorders
DOI:
https://doi.org/10.15446/revfacmed.v64n4.54697Palabras clave:
Trastornos relacionados con sustancias, Resultado del tratamiento, Psicometría, Evaluación de Programas (es)Substance-Related Disorders, Treatment outcome, Psychometrics, Program Evaluation (en)
Introducción. En la actualidad resulta imprescindible contar con instrumentos que permitan evaluar los resultados de tratamiento en pacientes con trastornos por uso de sustancias.
Objetivo. Revisar la literatura científica de los últimos 10 años relacionada con la validación y el uso de instrumentos o de otros indicadores de resultado para la evaluación de tratamientos de trastornos por uso de sustancias.
Materiales y métodos. Se realizó una búsqueda de artículos científicos publicados entre 2005 y 2015 que abordaran el tema de instrumentos de medida de los trastornos por uso de sustancias y la efectividad de los tratamientos. Se utilizó la base de datos MEDLINE y se limitó la búsqueda a títulos, resúmenes y textos completos disponibles.
Resultados. Se seleccionaron 21 estudios de validación de instrumentos, 14 de evaluación de resultados utilizando instrumentos, 5 revisiones narrativas y 2 sistemáticas.
Conclusiones. Los instrumentos encontrados exploran diferentes áreas según el tipo de tratamiento y los objetivos propuestos, sin embargo no hay una prueba única que permita evaluar de manera íntegra los resultados del tratamiento debido a la complejidad del tema. Se recomienda continuar con el desarrollo y validación de instrumentos específicos para tratamientos complejos en instituciones que trabajan con modelos terapéuticos integrales.
Introduction: Having tools to assess the outcomes of treatment in patients with substance use disorders is highly important.
Objective: To review the last 10 years of scientific literature related to the validation and use of instruments or other performance measures in treatment evaluation.
Materials and methods: A search of scientific papers, published between 2005 and 2015, addressing measurement instruments for substance use disorders and effectiveness of treatments was performed. The MEDLINE database was used and the search was limited to titles, abstracts and full texts available.
Results: 21 instrument validation studies, 14 performance evaluations using instruments, 5 narrative reviews and 2 systematic reviews were selected.
Conclusions: The found instruments explore different areas depending on the type of treatment and proposed objectives; however, there is not a unique test to fully assess the results of treatment due to the complexity of the topic. It is recommended to continue the development and validation of specific tools for complex treatments in institutions working with comprehensive therapeutic models.artículo de revisión
DOI: https://doi.org/10.15446/revfacmed.v64n4.54697
Uso de instrumentos clínicos para la evaluación de pacientes y
resultados de tratamiento en trastornos por uso de sustancias (TUS)
Using clinical tools for assessing patients and treatment outcomes for Substance Use Disorders
Recibido: 15/12/2015. Aceptado: 31/03/2016.
Luis Fernando Giraldo-Ferrer1 • Juan David Velásquez-Tirado2 • Juan Carlos Restrepo-Medrano3 • Andrés Felipe Tirado-Otálvaro4
1 ESE Hospital CARISMA - Departamento de psiquiatría - Medellín - Colombia.
2 Universidad Pontificia Bolivariana - Sede Medellín - Facultad de Medicina - Grupo de Investigación Psiquiatría de Enlace - Medellín - Colombia.
3 Universidad de Antioquia - Sede Medellín - Facultad de Enfermería - Grupo de Investigación Emergencias y Desastres - Medellín - Colombia.
4 Universidad Pontificia Bolivariana - Sede Medellín - Facultad de Enfermería - Grupo de Investigación Cuidado - Medellín - Colombia
Correspondencia: Luis Fernando Giraldo-Ferrer. Departamento de Psiquiatría, ESE Hospital CARISMA. Carrera 93 No. 34AA-01, oficina 5. Teléfono: +57 4 4924000, ext.: 130. Medellín. Colombia. Correo electrónico: luisgiraldoferrer@yahoo.com.
| Resumen |
Introducción. En la actualidad resulta imprescindible contar con instrumentos que permitan evaluar los resultados de tratamiento en pacientes con trastornos por uso de sustancias.
Objetivo. Revisar la literatura científica de los últimos 10 años relacionada con la validación y el uso de instrumentos o de otros indicadores de resultado para la evaluación de tratamientos.
Materiales y métodos. Se realizó una búsqueda de artículos científicos publicados entre 2005 y 2015 que abordaran el tema de instrumentos de medida de los trastornos por uso de sustancias y la efectividad de los tratamientos. Se utilizó la base de datos MEDLINE y se limitó la búsqueda a títulos, resúmenes y textos completos disponibles.
Resultados. Se seleccionaron 21 estudios de validación de instrumentos, 14 de evaluación de resultados utilizando instrumentos, 5 revisiones narrativas y 2 sistemáticas.
Conclusiones. Los instrumentos encontrados exploran diferentes áreas según el tipo de tratamiento y los objetivos propuestos, sin embargo no hay una prueba única que permita evaluar de manera íntegra los resultados del tratamiento debido a la complejidad del tema. Se recomienda continuar con el desarrollo y validación de instrumentos específicos para tratamientos complejos en instituciones que trabajan con modelos terapéuticos integrales.
Palabras clave: Trastornos relacionados con sustancias; Resultado del tratamiento; Psicometría; Evaluación de Programas (DeCS).
Giraldo-Ferrer LF, Velásquez-Tirado JD, Restrepo-Medrano JC, Tirado-Otálvaro AF. Uso de instrumentos clínicos para la evaluación de pacientes y resultados de tratamiento en trastornos por uso de sustancias (TUS). Rev. Fac. Med. 2016;64(4):749-759. Spanish. doi: https://doi.org/10.15446/revfacmed.v64n4.54697.
| Abstract |
Introduction: Having tools to assess the outcomes of treatment in patients with substance use disorders is highly important.
Objective: To review the last 10 years of scientific literature related to the validation and use of instruments or other performance measures in treatment evaluation.
Materials and methods: A search of scientific papers, published between 2005 and 2015, addressing measurement instruments for substance use disorders and effectiveness of treatments was performed. The MEDLINE database was used and the search was limited to titles, abstracts and full texts available.
Results: 21 instrument validation studies, 14 performance evaluations using instruments, 5 narrative reviews and 2 systematic reviews were selected.
Conclusions: The found instruments explore different areas depending on the type of treatment and proposed objectives; however, there is not a unique test to fully assess the results of treatment due to the complexity of the topic. It is recommended to continue the development and validation of specific tools for complex treatments in institutions working with comprehensive therapeutic models.
Keywords: Substance-Related Disorders; Treatment outcome; Psychometrics; Program Evaluation (MeSH).
Giraldo-Ferrer LF, Velásquez-Tirado JD, Restrepo-Medrano JC, Tirado-Otálvaro AF. [Using clinical tools for assessing patients and treatment outcomes for Substance Use Disorders]. Rev. Fac. Med. 2016;64(4):749-759. Spanish. doi: https://doi.org/10.15446/revfacmed.v64n4.54697.
Introducción
Evaluar la efectividad de los tratamientos para trastornos por uso de sustancias (TUS) a través de investigaciones científicas es un paso previo para llevar a la práctica los hallazgos clínicos, lo cual deben traducirse en mejorías de calidad, contenido y duración de dichos tratamientos. Un ejemplo de esto es el llevado a cabo por la Red Nacional de Ensayos Clínicos para el Tratamiento de las Drogas de Estados Unidos (CTN, por sus siglas en inglés) del National Institute of Drug Abuse (NIDA), que emplea los centros de tratamiento comunitarios con diversas poblaciones de pacientes y condiciones para ajustar y estudiar protocolos que satisfagan las necesidades prácticas del tratamiento de la adicción (1).
La Organización Mundial de la Salud, el Programa de las Naciones Unidas para la Fiscalización Internacional de Drogas (PNUFID) y el Observatorio Europeo de las Drogas y las Toxicomanías (OEDT) publicaron conjuntamente en el año 2000 directrices en una serie de manuales sobre la evaluación del tratamiento para los TUS (2).
El Plan de Acción en Salud Mental para Europa, aprobado en la European Ministerial Conference on Mental Health de 2005, contempla en su área de acción número 12 la necesidad de evaluar la efectividad y generar nueva evidencia, acción imposible de emprender si no se dispone de los instrumentos de evaluación adecuados (3).
Los TUS se ubican en el grupo de trastornos crónicos y complejos (4), lo que implica que al momento de hacer la evaluación inicial de los pacientes y de medir los resultados del tratamiento se debe considerar no solo el consumo de sustancias, sino también las características y magnitud de los problemas relacionados, es decir que los instrumentos utilizados para evaluar y medir resultados deben reflejar el llamado concepto biaxial de las adicciones (5-7); este concepto debe ser tenido en cuenta al momento de diseñar tratamientos más eficaces (8).
El resultado de un tratamiento se define como la modificación de una conducta a través de una intervención determinada y guarda relación directa con el tiempo que dure el mismo (9); en el caso de los TUS, los resultados suelen incluir abstinencia o disminución del consumo, disminución de la criminalidad, mejoría de la salud física y de las habilidades sociales, entre otros, y pueden ser medidos al inicio, durante y al final del tratamiento o en uno o más momentos del seguimiento (10).
Tras décadas de acercamientos categoriales a los TUS, en la actualidad cobra importancia la integración de aproximaciones dimensionales en los instrumentos de evaluación (11); este planteamiento obliga a incorporar a la práctica clínica instrumentos que proporcionen puntuaciones de gravedad en las distintas dimensiones, las cuales permitirían identificar las áreas de mayor necesidad de tratamiento y ofrecer una medida objetiva de la severidad (12).
Long & Hollin (13) han descrito algunos de los principales instrumentos que miden aspectos generales del problema como se plantea en la Tabla 1.
Para Long & Hollin (13), los siguientes instrumentos se ocupan de medir aspectos particulares de los TUS (Tabla 2).
La evaluación de la efectividad de los tratamientos para los TUS ha sido una preocupación reciente para los sistemas de aseguramiento, el personal de salud y la comunidad en general. Tanto el estado como los prestadores de salud requieren herramientas que permitan evaluar los tratamientos de las adicciones para poder orientar planes de mejoramiento, comparar los resultados entre instituciones y cuantificar el efecto que tiene la incorporación de nuevas intervenciones con miras a definir políticas para su atención, orientar recursos, reglamentar el sector, definir características y logros mínimos y acreditar instituciones como prestadoras de estos servicios.
Tabla 1. Instrumentos que miden aspectos generales del problema.
|
Instrumento |
Año |
Numero de ítems |
Aspectos que evalúa |
|
The Health of the Nation Outcome Scales (HoNOS) (14) |
1998 |
12 |
Problemas conductuales, deterioro, síntomas, incapacidad y funcionamiento social |
|
Addiction Severity Index (ASI) (15-17) |
1979 |
257 |
Información general del paciente, salud física y mental, empleo, recursos, drogas y alcohol, situación legal, red familiar y social |
|
Christo Inventory for Substance-Misuse Services (CISS) (18-20) |
2000 |
10 |
Funcionamiento social, salud general, comportamientos de riesgo sexual y por inyección intravenosa, funcionamiento psicológico y ocupacional, participación en actividades criminales, uso de drogas y alcohol. |
|
Maudsley Addiction Profile (MAP) (21) |
1998 |
64 |
Abuso de sustancias, comportamientos de riesgo sexual y relacionados con inyección intravenosa, salud física y psicológica, contexto vital y funcionamiento social |
|
OTI (Opiate Treatment Index) (22) |
1991 |
110 |
Consumo de drogas, conducta de riesgo de contagio de VIH, funcionamiento social, actividad delictiva, estado de salud y ajuste psicológico |
Fuente: Elaboración propia.
Tabla 2. Instrumentos que miden aspectos particulares del problema.
|
Instrumentos |
Aspectos a evaluar |
|
Análisis funcional en personas con trastorno mental (autoeficacia, motivación para el cambio, marcadores biológicos, craving, habilidades de afrontamiento y resolución de problemas) |
|
Comorbilidad |
|
Impulsividad |
|
Calidad de vida |
|
Alianza Terapéutica |
Fuente: Elaboración propia.
Este artículo tiene como objetivo revisar la literatura científica de los últimos 10 años relacionada con la validación y el uso de instrumentos o de otros indicadores de resultado para la evaluación de tratamientos.
Materiales y métodos
Se realizó una búsqueda de los artículos científicos publicados en la literatura que abordan el tema de escalas o instrumentos de medida de los TUS y la efectividad o los resultados de los tratamientos para estos trastornos. Se utilizó la base de datos MEDLINE y la búsqueda se hizo a través del PubMed, limitándose a títulos, resúmenes y textos completos, en inglés o español, entre los años 2005 y 2015; también incluyó revisiones sistemáticas de la literatura, meta-análisis, ensayos clínicos, estudios de validación de instrumentos y revisiones narrativas. Se emplearon los conectores booleanos AND, OR y NOT para restringir la búsqueda al tema de la investigación. Para localizar los artículos de forma más precisa se buscó si el término existía en el tesauro de la base de datos por medio del MeSH Database.
Para la selección de los artículos se establecieron como criterios de inclusión que entre sus objetivos o hipótesis se abordara el desarrollo o análisis de un instrumento de medida de los TUS, la efectividad, los resultados de los tratamientos y el tipo de estudio. Los criterios de exclusión fueron artículos sin resumen disponible, editoriales, recensiones de libros y estudios en animales.
En principio se seleccionaron los textos por la pertinencia del título y el resumen. En aquellos que fueron elegidos de esta manera se analizó el texto completo de los artículos por parte de todos los investigadores para evaluar la calidad de las publicaciones y considerar su inclusión dentro de esta revisión. La información de interés para el estudio fue extraída mediante la aplicación de una planilla ad hoc que recogía información sobre características generales de los estudios: título, tipo de estudio, año de publicación, variables que evalúa, instrumento utilizado, forma en que se validó o desarrolló dicho instrumento y propiedades clinicométricas del mismo.
La primera estrategia de búsqueda se realizó de la siguiente manera: (“Assessment instruments”[All Fields] OR (“instrumentation”[Subheading] OR “instrumentation”[All Fields] OR “instruments”[All Fields])) AND (“treatment response”[All Fields] OR “treatment outcome”[All Fields] OR “Outcome response”[All Fields]) AND (“substance-related disorders”[MeSH Terms] OR “substance use disorder”[All Fields] OR “drug habituation”[All Fields] OR “drug addiction”[All Fields] OR “drug dependence”[All Fields]); en dicha búsqueda se encontraron 130 artículos, de los cuales 44 cumplieron los criterios de inclusión. Posterior a esto se realizó una segunda búsqueda utilizando la siguientes estrategias: ((((“substance-related disorders”[MeSH Terms] OR “substance use disorder”[All Fields] OR “drug addiction”[All Fields] OR “drug dependence”[All Fields] OR “drug abuse”[All Fields] OR “substance abuse”[All Fields])) AND psychometric[Title/Abstract])) AND (“Outcome and Process Assessment (Health Care)”[Mesh] OR “Outcome Assessment (Health Care)”[Mesh] OR “Treatment Outcome”[Mesh] OR “Treatment outcome” OR “outcome measurement”); en esta oportunidad se encontraron 87 resultados, de los cuales 19 cumplían con los criterios de inclusión.
Por último, se refinó la búsqueda incluyendo los siguientes términos: (psychometric[Title/Abstract] OR “Assessment instruments” OR instruments) AND (“treatment response” OR “treatment outcome” OR “Outcome response”) AND (“substance-related disorders”[MeSH Terms] OR “substance use disorder”[All Fields] OR “drug habituation”[All Fields] OR “drug addiction”[All Fields] OR “drug dependence”[All Fields]); encontrándose 176 artículos, de los cuales 13 fueron pertinentes para evaluar por los investigadores.
Los 76 artículos seleccionados se distribuyeron entre los investigadores vinculados al estudio, quienes diligenciaron la tabla que resumía las características más importantes de los mismos; a partir del análisis por parte del grupo en pleno se evaluó la pertinencia de las publicaciones para ingresar en esta revisión. Cada uno de los autores evaluó por separado los artículos según los criterios mencionados y se compararon cuando había discordancias, en cuyo caso se resolvió la situación por medio de un consenso entre los investigadores. Al final, se incluyeron 21 estudios de validación de instrumentos, 14 ensayos clínicos, 5 revisiones narrativas y 2 revisiones sistemáticas de la literatura. En la Figura 1 se muestra el proceso de selección de los artículos.
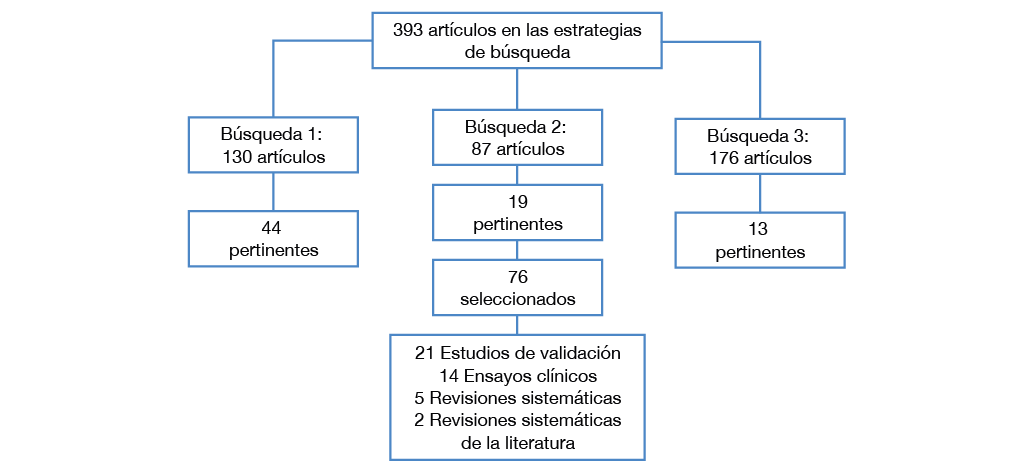
Figura 1. Proceso de selección de los estudios incluidos en la revisión. Fuente: Elaboración propia.
Resultados
Con la estrategia de búsqueda descrita se analizaron 21 estudios relacionados con validación de instrumentos y 14 ensayos clínicos de evaluación de resultados de tratamiento.
Los artículos encontrados se dividieron en dos grupos, en el primero se incluyeron estudios orientados a validar instrumentos que se ocupan de la evaluación y caracterización de los pacientes con TUS o a la evaluación de resultados de forma general y en el segundo los realizados con el objetivo de evaluar resultados de tratamiento con alguna forma determinada de intervención.
Estudios de validación
De los 21 estudios de validación solo 6 cumplían criterios para validar escalas de evaluación de tratamiento; de estos, 4 fueron desarrollados en Australia —Australia Treatment, Outcome Profile (ATOS) (37), Alcohol, Treatment Outcome Profile (ATOM) (38), Brief Treatment Outcome Measure (BTOM) (39)—, 1 en Nueva Zelanda —Metadone Treatment Index (MTI) (40)— y 1 en Suecia —Outcome Questionary (OQ45) (41)—.
Un estudio llevado a cabo en Estados Unidos por el Departamento de Salud y Servicios de Bienestar se ocupó del progreso de tratamiento en adolescentes en comunidad terapéutica utilizando el instrumento Dimensions of Change Instrument–Adolescent (DCI-A) (42).
Dos estudios se ocuparon de instrumentos para medir la calidad de vida, los cuales se pueden utilizar para evaluar resultados de tratamiento en determinadas condiciones o simplemente para caracterizar los pacientes con TUS o las personas que han realizado tratamientos. Estos artículos validan los instrumentos Alcohol Dependence Quality of life (ALQoL9) (43) y World Health Organization Quality of Life assessment (WHOQOL-BREF) (44).
Algunas investigaciones validaron instrumentos orientados en su mayoría a la determinación de algunas características del individuo con TUS, como son la determinación de la severidad de la dependencia a través de las escalas Severity of Dependence Scale (SDS) (45) y The Important People and Activities (IPA) (46), las cuales valoran relaciones familiares y redes sociales, salud y bienestar, soporte social, consumo (frecuencia, cantidad, tiempo usado en el consumo), fallas en el cumplimiento de obligaciones, consumo en situaciones físicamente riesgosas, sentimientos de culpa y fallas en la memoria.
Otros estudios se ocupan de las características de los adolescentes consumidores: problemas con los padres, en las relaciones personales y de empleo, rendimiento escolar, dependencia química, funcionamiento psicosocial, delincuencia, comportamiento de riesgo, uso del tiempo libre, comportamiento sexual, situación jurídica y salud mental. Los instrumentos utilizados para esto fueron Adolescent Cannabis Problems Questionnaire (CPQ-A) (47), Adolescent Severity Inventory (CASI) (48) y Adolescent Drug Abuse Diagnosis (ADAD) (49).
Uno de los estudios exploró la relación entre el ajuste a la filosofía y práctica de los 12 pasos de alcohólicos anónimos y los resultados en el tratamiento, evaluando la adherencia a este modelo y la relación con el pronóstico (50). Solo un estudio se ocupó de la satisfacción con el tratamiento, la cual fue explorada con el Treatment Satisfaction Questionnaire for Medication (TSQM) (51). Una investigación realizó la validación de una escala que permitía el seguimiento a una técnica terapéutica y el manejo de contingencias en su correcta realización, dicho estudio utilizó la escala 12-item CM Competence Scale (CMCS) (52).
La capacidad de pronóstico de algunos instrumentos fue evaluada con el Drug Taking Confidence Questionnaire (DTCQ) (53), que mide la autoeficacia para resistir el deseo de consumir y contiene ítems relacionados con situaciones de riesgo para el consumo como emociones agradables y desagradables, malestar físico, prueba de control personal, impulsos y tentaciones, conflictos con los demás, presión social para consumir y tiempos agradables con otros, situaciones que están en relación con la recaída luego del tratamiento.
Por último, una de las investigaciones empleó la Readiness to Change Questionnaire (RCQTV) y la Treatment Readiness Tool (TReaT) explorando la validez predictiva de las escalas e identificando consumos y problemas relacionados con estos (54).
En la Tabla 3 se sintetizan los 21 estudios de validación encontrados en esta investigación.
Ensayos clínicos
En la búsqueda realizada se encontraron 14 ensayos clínicos, de los cuales 6 evaluaron la efectividad de los tratamientos, 5 evaluaron programas de tratamiento, 1 evaluó la efectividad de uso de ayudas tecnológicas como el teléfono móvil, 1 los incentivos económicos y por último se incluyó 1 estudio de corte económico que analizó los beneficios del tratamiento con el Drug Abuse Treatment Cost Analysis Program (DATCAP) y el Addiction Severity Index (ASI).
De los 6 estudios que evaluaron terapias farmacológicas, 2 incluyeron naltrexona (59,60) y 1 naloxona (61), medicamentos para el tratamiento de problemas relacionados con el uso de alcohol, otro evaluó el biperideno en tratamiento de pacientes con uso de cocaína (62) y el restante realizó un seguimiento de cuatro años de pacientes en terapia con diacetilmorfina (63); dichos estudios analizaron variables como estado de ánimo, craving, empleo, tiempo libre, actividades criminales, dependencia y abstinencia. Para evaluar los desenlaces, estos estudios emplearon instrumentos como la escala de Minessota de ansiedad de consumo de cocaína, el inventario de depresión de Beck, el Alcohol Craving Questionnaire (ACQ), el Profile of Mood Scale (POMS), el Opiate Treatment Index (OTI-HSS), el Symptom Checklist-90-Revised (SCL-90-R) y el European Addiction Severity Index. Por las características mismas de estas investigaciones, no se realizó validación de los instrumentos ni se evaluaron sus propiedades clinicométricas.
Los seis estudios centrados en programas de tratamiento evaluaron variables como tolerancia con el malestar, consumo, abuso y dependencia a sustancias, usos de servicios de salud y bienestar, craving y abstinencia. Dichos estudios incluyeron instrumentos como el Distress Tolerance Scale (DTS) (58), el Drug Stroop Protocol (DSP), el Implicit Relational Assessment Procedure (IRAP) (64), el Brief Michigan Alcoholism Screening Test, el Drinking Expectancy Profile (DEP) (65) y el Dimensions of Change Instrument (DCI) (66). De estos, solo 2, el DSP y el IRAP, tienen buenos resultados de fiabilidad que ponen de manifiesto la utilidad potencial de las medidas (64), mientras que el Measuring Changes in Client-Level Treatment Process in the Therapeutic Community (TC) with the Dimensions of Change Instrument (DCI) muestra valores adecuados de la fiabilidad, por lo cual los autores concluyen que se puede aplicar a los adolescentes, ya que dicho instrumento evalúa diferentes características de un programa de hospitalización como respuesta al tratamiento, seguridad, procesos de grupo, etc. (66).
En la Tabla 4 se sintetizan los 14 estudios de intervención encontrados en esta investigación.
Artículos de revisión
Entre los artículos de revisión encontrados, 5 corresponden a revisiones narrativas y 2 a revisiones sistemáticas.
El artículo escrito por Midanik et al. (74) analiza las propiedades psicométricas de los diversos instrumentos que se utilizan para medir la dependencia al alcohol y pone de manifiesto las categorías utilizadas por los diversos cuestionarios que miden dicha dependencia y sus principales características. En estos instrumentos las medidas más utilizadas son la severidad del consumo —frecuencia y cantidad— y las manifestaciones de dependencia. En el artículo se cuestionan los métodos empleados para la validación de los diversos instrumentos que analizan la dependencia al alcohol, por lo que los autores plantean la necesidad de seguir ahondando en la investigación sobre este tema.
Tabla 3. Estudios de validación incluidos en la revisión.
|
Título y año del artículo |
Instrumento utilizado |
Variables que evalúa |
Propiedades clinicométricas |
|
Reliability and validity of the severity of dependence scale in a chinese sample of treatment-seeking ketamine users (45). 2014 |
Chinese Severity of Dependence Scale for ketamine (C-SDS-K) |
Control del consumo, craving, preocupación con el uso, deseo de parar el consumo, dificultad para parar o mantenerse sin consumir |
α: 0.74; test-retest: 0.95; validez concurrente: 0.84 |
|
Psychometric evaluation, using Rasch analysis, of the WHOQOL-BREF in heroin-dependent people undergoing methadone maintenance treatment: further item validation (44). 2014 |
WHOQOL-BREF |
Dolor y malestar, energía y fatiga, movilidad, sueño, actividades de la vida diaria, capacidad de trabajo, sentimientos positivos, espiritualidad, creencias, imagen corporal, autoestima, sentimientos negativos, relaciones interpersonales, actividad sexual, soporte social, seguridad, ambiente físico, recursos financieros, diversión, servicios de salud y transporte |
α: 0.88 para el cuestionario total y 0.87-0.88 para cada una de las preguntas |
|
The psychometric development and initial validation of the DCI-A short form for adolescent therapeutic community treatment process (42). 2014 |
DCI-A-SF originado en el DCI-A |
Motivación para el tratamiento, desarrollo personal, reconocimiento del problema, relaciones familiares y redes sociales |
α: 0.72-0.91; DCI-A predictivo del tiempo de duración en el tratamiento |
|
Validation and implementation of the Australian Treatment Outcomes Profile in specialist drug and alcohol settings (37). 2013 |
ATOS |
Uso de sustancias, cantidad y frecuencia, uso de drogas intravenosas, salud física, salud mental, calidad de vida, alojamiento, empleo, estudio, arrestos, violencia, cuidado de los hijos |
Demostró aceptable validez concurrente y validez y fiabilidad interevaluador * |
|
Satisfaction with methadone as a medication: psychometric properties of the Spanish version of the treatment satisfaction questionnaire for medication (51). 2012 |
TSQM |
Satisfacción con la medicación, con el tiempo que tarda en actuar, efectos secundarios y molestias, afectación de la esfera mental, la calidad de vida y confianza en la medicación |
α: 0.78-0.89 |
|
The 12 Step Affiliation and Practices Scale: development and initial validation of a measure assessing 12 step affiliation (50). 2011 |
12 Step Affiliation and Practices Scale (TSAPS) |
Evolución durante el tratamiento en la práctica de los pasos y la creencia en ellos |
Consistencia interna muy alta. Las mediciones del TSAPS se incrementaron con el curso del tratamiento. Se encontró validez predictiva y convergente * |
|
Psychometric properties of the contingency management competence scale (52). 2010 |
12-item CM Competence Scale (CMCS) |
Manejo de contingencias de forma apropiada, monitoreo en orina y aliento, manejo de autorreportes, consecuencias de muestras positivas, reconocimiento de progresos, comunicación de confianza en el futuro y expresión de empatía |
La confiabilidad intercalificador para cada ítem y para la escala global estuvo en el rango de buena a excelente y la consistencia interna fue buena * |
|
The Swedish version of the Outcome Questionnaire (OQ-45): Reliability and factor structure in a substance abuse simple (41). 2010 |
OQ-45 |
Reducción de los síntomas y funcionamiento social. Tres dimensiones generales: problemas intraindividuales (síntomas angustiantes-SD), problemas en las relaciones con otros (relaciones interpersonales-IR) y problemas que el individuo tiene con la sociedad que lo rodea (rol social-SR) |
La consistencia interna fue satisfactoria en la puntuación total OQ y en las subescalas SD e IR, mientras que fue un poco bajo en la subescala SR * |
|
The Alcohol Treatment Outcome Measure (ATOM): a new clinical tool for standardizing outcome measurement for alcohol treatment (38). 2009 |
ATOM. |
Uso de sustancias, relaciones, aspectos económicos, crimen, salud física y psicológica |
Confiabilidad de buena a excelente en test-retest e intercalificadores; validez concurrente y confiabilidad interna satisfactorias. Capacidad para medir el cambio en el funcionamiento a través del tiempo * |
|
The performance of two motivation measures and outcome after alcohol detoxification (54). 2009 |
(RCQ[TV]) y (TReaT). |
Preparación para cambiar y disposición para buscar ayuda. Asignación según etapas de cambio: precontemplación, contemplación y acción |
Propiedades psicométricas satisfactorias para el TReaT[TV]. Validez predictiva para ambos instrumentos: RCQ [TV] predijo la abstinencia, mientras que TReaT[TV] predijo la búsqueda de ayuda formal 12 meses después de la desintoxicación * |
|
The Important People Drug and Alcohol interview: psychometric properties, predictive validity, and implications for treatment (46). 2009 |
IPA |
Soporte social en abstinencia a cocaína, influencias de la red social en la abstinencia al alcohol, aspectos de apoyo social a través de una amplia gama de relaciones |
Tres componentes con una consistencia interna aceptable: a) participación de la red social en el consumo de la sustancia, b) apoyo general y del tratamiento y c) apoyo para la abstinencia * |
|
Development of a brief treatment instrument for routine clinical use with methadone maintenance treatment clients: the methadone treatment index (40). 2008 |
MTI. |
Funcionamiento social y conductual, salud física y mental en pacientes con uso reciente de sustancias |
Correlación entre las puntuaciones de salud psicológica con la escala BDI y la escala t-ansiedad satisfactorias (0.83 y 0.84); test-retest (prácticas de inyección y sexuales, actividad criminal y salud física y psicológica) en un excelente rango * |
|
An improved brief measure of cannabis misuse: the Cannabis Use Disorders Identification Test-Revised (CUDIT-R) (55). 2010 |
CUDIT-R |
Consumo de Tetrahidrocanabinol (THC), frecuencia, cantidad, tiempo usado en el consumo, abuso, incumplimiento de obligaciones, uso en situaciones riesgosas, sentimientos de culpa, pensamientos sobre modificar el consumo y fallas en memoria |
Aunque se confirmó la adecuación psicométrica del CUDIT original, el CUDIT-R fue más corto y tuvo propiedades psicométricas equivalentes o superiores. Alta sensibilidad (91%) y especificidad (90%) * |
|
Coping self-efficacy against alcohol and other drugs use as treatment outcome predictor and its relation with personality dimensions: evaluation of a sample of addicts using DTCQ, VIP and MCM-II] (53). 2007 |
Drug Taking Confidence Questionnaire (DTCQ) |
Autoeficacia para resistir el deseo de consumir drogas en situaciones de riesgo, confianza con emociones desagradables, malestar físico, emociones agradables, intentos de control, tentaciones/urgencias de consumo, confrontación con otros y presión social |
α: 0.98 en todos los ítems. La puntuación obtenida en el DTCQ presenta correlación significativa con la evolución a los tres meses, pero no a los seis, ni a los nueve |
|
Development and validation of a brief instrument for routine outcome monitoring in opioid maintenance pharmacotherapy services: The brief treatment outcome measure (BTOM) (39). 2005 |
BTOM |
Severidad de la dependencia, riesgo de exposición a virus de transmisión sanguínea, consumo de drogas y alcohol, salud, funcionamiento psicológico y funcionamiento social |
Test-retest en todas las dimensiones por encima de 0.7, excepto la de drogas inyectables en diferentes evaluadores: 0.67; buena validez de contenido; validación concurrente con escalas similares con acuerdo aceptable; muestra sensibilidad al cambio a los tres meses * |
|
The drinking situations of adolescents treated for alcohol use disorders: A psychometric and alcohol-related outcomes investigation (56). 2005 |
Inventory of Drinking Situations (IDS) |
Episodios de recaída luego del tratamiento, emociones agradables y desagradables, malestar físico, control personal de impulsos y tentaciones, conflictos con los demás, presión social para consumir y tiempos agradables con otros |
Los tres factores que mejor se ajustaron fueron: situaciones negativas, situaciones sociales y tentación, con puntuaciones superiores al 0.5; niveles adecuados de fiabilidad para cada una de las tres subescalas: situaciones negativas y sociales: 0.47, situaciones negativas y tentación: 0.64 y situaciones sociales y tentación 0.42 * |
|
Predictive Validity of the RIASI: Alcohol and Drug Use and Problems Six Months Following Remedial Program Participation. Año 2006(57) |
Research Institute on Addictions Self-Inventory (RIASI). |
Consumo, recaídas, problemas relacionados con el uso de alcohol y otras drogas |
Consistencia interna con α: 0.59 y 0.79. |
|
ALQoL 9 for measuring quality of life in alcohol dependence (43). 2006 |
AlQoL9, obtenido de la SF36. |
Arreglos de vivienda, situación laboral, historia de alcohol, funcionamiento físico, dolor corporal, salud mental, energía/vitalidad, percepción de salud general, limitaciones por problemas físicos, limitaciones por problemas emocionales y funcionamiento social |
α: 0.85 en pacientes ambulatorios y 0.71 en pacientes hospitalizados; coeficientes intraclase test-retest: 0.81 para la puntuación global AlQoL 9 |
|
The Adolescent Cannabis Problems Questionnaire (CPQ-A): Psychometric properties (47). 2006 |
CPQ-A. |
Problemas con los padres, problemas en las relaciones personales, rendimiento escolar y problemas de empleo |
α: 0.88; correlación test-retest entre tiempo 1 y tiempo de 2 para el total CPQ-A: 0.91 |
|
Factor Structure of the Comprehensive Adolescent Severity Inventory (CASI): Results of Reliability, Validity, and Generalizability Analyses (48). 2006 |
CASI |
Dependencia química, funcionamiento psicosocial, delincuencia y comportamiento de riesgo, salud, eventos de la vida estresantes, educación, alcohol y consumo de drogas, uso del tiempo libre, relaciones con los compañeros, comportamiento sexual, relaciones familiares, situación jurídica y salud mental |
Todos los valores de consistencia interna superaron 0.70 y todos los coeficientes de estabilidad fueron estadísticamente significativos (p<0.0001) |
|
Examining psychometric properties of distress tolerance and its moderation of mindfulness-based relapse prevention effects on alcohol and other drug use outcomes (58). 2013 |
Distress Tolerance Scale (DTS). |
Tolerancia con el malestar y resultados de tratamiento en consumo de sustancias |
α: 0.95; las diferentes sub escalas tienen validez convergente |
α: Alfa de Cronbach.
* No presentan datos de la consistencia interna a través del Alpha de Cronbach.
Fuente: Elaboración propia.
El artículo de Chinet et al. (49) corresponde a una revisión del instrumento Adolescent Drug Abuse Diagnosis (ADAD), el cual fue aplicado en un estudio longitudinal de cuatro años de duración; en este se analizaron las principales características para aplicarlo de forma correcta. Aunque se desglosan los diversos aspectos a tener en cuenta en el momento de su uso, al final del artículo no queda clara la validez y confiabilidad del mismo. También se analizan las diversas categorías y subcategorías de medida y cómo realizar el análisis al momento de medirlas, así como los problemas identificados durante su aplicación.
Uno de los principales indicadores de resultado en la atención en salud en los pacientes opiodependientes fue la calidad de vida, bajo este precepto se realizó una revisión sistemática de la literatura en 2011 por De Maeyer et al. (75), donde se quiso establecer el nivel de calidad de vida de estos pacientes después de terminar su tratamiento; aunque la búsqueda se realizó de forma amplia, la información obtenida no permitió cuantificar claramente el nivel de calidad de vida, comparando con el de la población general.
La terapia conductual fue abordada por Ruff et al. (76), quienes realizaron una revisión sistemática de esta para parejas casadas o en convivencia en las que habían pacientes con TUS. Se realizó una revisión de 23 estudios, los cuales dieron soporte a la terapia comportamental de parejas, tomando como parámetros de mejoría disminución en el consumo de sustancias, ajuste diádico, resultados psicosociales de los niños y reducción de la violencia con el compañero. Se evaluó la versión de la terapia desarrollada por O’Farrell, Fals-Stewart y colaboradores. Las medidas de evaluación fueron: ajuste marital, consumo de sustancias y controles en orina y sangre semanales, además se midieron encarcelamientos, hospitalizaciones y días en alojamientos protegidos.
En la Tabla 5 se sintetizan los siete artículos de revisión encontrados en esta investigación.
Tabla 4. Estudios de intervención incluidos en la revisión.
|
Título y año del artículo |
Instrumento utilizado |
Variables que evalúa |
|
Effects of biperiden on the treatment of cocaine/crack addiction: a randomised, double-blind, placebo-controlled trial (62). 2014 |
Escala de Minessota de ansiedad de consumo de cocaína, inventario de depresión de Beck y un cuestionario sobre la cantidad de droga usada |
Reducción de craving y del consumo |
|
Pharmacological challenge with naloxone and cue exposure in alcohol dependence: results of a randomized, double-blind placebo-controlled trial (61). 2013 |
ACQ y POMS |
Estado de ánimo (afecto) y deseo de consumo de alcohol |
|
Social integration after 4 years of heroin-assisted treatment (63). Año 2013 |
OTI-HSS y SCL-90-R. Tóxicos en orina y variables compuestas del European Addiction Severity Index. |
Empleo, situación de vida, actividades del tiempo libre, actividades criminales |
|
Case management in aftercare of involuntarily committed patients with substance abuse. A randomized trial (67). 2013 |
No se mencionan instrumentos |
Consumo de sustancias, uso de los servicios de salud y bienestar |
|
A pilot study of the DBT coach: an interactive mobile phone application for individuals with borderline personality disorder and substance use disorder (68). 2011 |
No se mencionan instrumentos |
Intensidad de las emociones craving, depresión y malestar, usabilidad y utilidad de la tecnología |
|
Open-label pilot study of extended-release naltrexone to reduce drinking and driving among repeat offenders (59). 2011 |
Sin instrumento. Dispositivo ubicado en el vehículo para identificar intentos de conducir luego de haber ingerido alcohol |
Beber e intentos de manejar luego de haber bebido, bebidas por día, días de abstinencia |
|
Alcohol expectancy changes over a 12-week cognitive-behavioral therapy program are predictive of treatment success (65). 2011 |
Brief Michigan Alcoholism Screening Test. The Drinking Expectancy Profile (DEP) |
Abstinencia, expectativa y autoeficacia de negarse a beber |
|
Effects of varying the monetary value of voucher-based incentives on abstinence achieved during and following treatment among cocaine-dependent outpatients (69). 2006 |
Vermont Structured Diagnostic Interview modificada para el DSMIV, ASI, the Beck Depression Inventory, the Michigan Alcohol Screening Test y un cuestionario de historia de uso de drogas |
Vales económicos dependiendo de los resultados de análisis de orina cocaína negativo durante las primeras 12 y 24 semanas de tratamiento |
|
Measures of Attentional Bias and Relational Responding Are Associated with Behavioral Treatment Outcome for Cocaine Dependence (64). 2012 |
Drug Stroop protocol and an Implicit Relational Assessment Procedure (IRAP) |
Abuso de sustancias, uso de cocaína, dependencia, reducción del craving y cantidad consumida |
|
Benefit-Cost Analysis of Addiction Treatment: Methodological Guidelines and Empirical Application Using the DATCAP and ASI (70). 2000 |
Abuse Treatment Cost Analysis Program (DATCAP) y ASI |
Todas las variables del ASI y del DATCAP |
|
Results of a double-blind, placebo-controlled pharmacotherapy trial in alcoholism conducted in Germany and comparison with the US COMBINE study (71). 2013 |
Escalas múltiples: AUDIT, SDS y escala de medición de autoeficacia |
Tiempo de duración en abstinencia hasta el primer consumo de licor |
|
A follow up study on the efficacy of metadoxine in the treatment of alcohol dependence (72). 2006 |
Michigan Alcohol Screening Test, transaminasas y volumen corpuscular medio (VCM) |
Abstinencia total de alcohol a los tres meses |
|
A 25-year follow-up of patients admitted to methadone treatment for the first time: Mortality and gender differences (73). 2011 |
Escala de impresión clínica global |
Mortalidad, diagnóstico de VIH, hepatitis B y C, uso actual de heroína y permanencia en el programa de mantenimiento de metadona |
|
Measuring Changes in Client-Level Treatment Process in the Therapeutic Community (TC) with the Dimensions of Change Instrument (DCI) (66). 2007 |
DCI |
Percepción de las interacciones en el ambiente, desarrollo personal y cambio en habilidades psicológicas y cognitivas |
Fuente: Elaboración propia.
Discusión
Se realizó una revisión narrativa estructurada con el objetivo de ilustrar un panorama general del uso de instrumentos e indicadores de resultados de tratamiento, la cual identificó diversas herramientas de medición con parámetros de evaluación heterogéneos para medir dichos resultados.
Se encontró que en los últimos 10 años se han desarrollado y validado múltiples instrumentos relacionados con diferentes aspectos de la evaluación de tratamientos, no obstante la utilización de estos podría verse limitada por la diversidad de culturas y ambientes terapéuticos.
La mayoría de los centros de atención en drogodependencias emplean modelos que en general son complejos e incluyen intervenciones variadas —farmacológicas, psicoterapéuticas, psicosociales, etc.—; sumado a esto, no existe, según el NIDA, un único tratamiento de los TUS que pueda ser recomendado para todas las personas (1), debido, entre otros factores, a la heterogeneidad de los pacientes y los centros de tratamiento.
Los TUS son un tema complejo y multidimensional (80) que requiere abordajes de tratamiento bajo estándares de calidad y evidencia científica (81). Existen lineamientos sobre las diferentes intervenciones que han demostrado una mayor efectividad en áreas específicas del tratamiento, sin embargo no hay un consenso acerca de cuál de ellas es la más recomendada (82). Por tanto, una vez que una institución formula su modelo está en la obligación de validarlo clínicamente con un instrumento adecuado a su esquema de tratamiento y que incluya todos los aspectos sobre los que se lleva a cabo alguna intervención (83).
Aunque muchos instrumentos han sido publicados, muy pocos tienen una adecuada evaluación de la aceptabilidad del usuario y no todos presentan el resultado de medición de sus propiedades psicométricas.
La medición en diferentes momentos del tratamiento del uso de sustancias, la estabilidad psicosocial, la criminalidad, el riesgo de contagio de virus sanguíneos y la salud física y psicológica son aspectos comunes en los instrumentos revisados, sin embargo se encuentran diferencias relacionadas con la combinación de dominios, la escogencia de escalas, el tiempo y el método de compleción. Estas características deben ser consideradas por el clínico o la institución a la hora de elegir un instrumento en particular.
Tabla 5. Artículos de revisión incluidos.
|
Título y año del artículo |
instrumento utilizado |
Variables que evalúa |
|
Factors associated with the outcome of drug addiction treatment (77). 2013 |
ASI, MAP, TOP |
Factores predictores de respuesta: disposición para cambio en estilo de vida, relación de confianza con el terapeuta y permanencia del usuario en tratamiento por un tiempo determinado |
|
Dual diagnosis clients' treatment satisfaction - a systematic review (78). 2011 |
Client Satisfaction Questionnaire (CSQ-8). Treatment Perceptions Questionnaire (TPQ) |
Satisfacción de los pacientes: se encontraron niveles altos con tratamientos integrales |
|
Assessing comorbid substance use in detained psychiatric patients: issues and instruments for evaluating treatment outcome (13). 2009 |
Diferentes pruebas diagnósticas, priorizando la brevedad y facilidad de administración y utilidad para la planificación del tratamiento |
Indicación adecuada de los instrumentos para población psiquiátrica |
|
Adolescent Substance-Use Assessment: Methodological Issues in the Use of the ADAD (49). 2005 |
The Adolescent Drug Abuse Diagnosis (ADAD). Versión francesa |
Nueve áreas problemáticas: académicas (colegio), empleo, vida y relaciones sociales, familiares y psicológicas, delincuencia y criminalidad, uso de drogas y alcohol |
|
Quality of Life as an Outcome Measure in Alcoholism Treatment Research (79). 2005 |
Medical Outcome Study (MOS) y Encuestas de Calidad de Vida en Salud (SF-36, SF-20 y SF-12) |
No se mencionan variables específicas, solo dominios generales como el bienestar físico, psicológico, emocional y ocupacional |
|
Behavioral Couples Therapy for the Treatment of Substance Abuse: A Substantive and Methodological Review of O’Farrell, Fals-Stewart, and Colleagues’ Program of Research (76). 2010 |
Terapia Conductual de Pareja versión de O’Farrell, Fals-Stewart y colaboradores |
Eficacia de la terapia conductual de pareja a la hora de mejorar el comportamiento de consumo de sustancias, adaptación diádica, resultados psicosociales en los niños y disminución de la violencia en la pareja |
|
Addiction sciences and its psychometrics: the measurement of alcohol-related problems (75). 2007 |
Estudio teórico de análisis de las medidas para dependencia al alcohol. Se analiza el ASI |
Consumo de alcohol, severidad de la dependencia, dependencia, fiabilidad y validez de los instrumentos |
Fuente: Elaboración propia.
Se identificaron instrumentos como el ATOS (36), que por su brevedad en cuanto al tiempo de administración y la inclusión de variables dimensionales (psicológica, salud física y calidad de vida) y otras como días de consumo, días de trabajo o estudio y número de días de inyección en una semana facilitan el trabajo del evaluador.
Instrumentos más amplios como el BTOM (38), que incluye escalas para severidad de la dependencia, riesgo de exposición a virus sanguíneos, uso de drogas en 30 días, salud general, bienestar psicológico y funcionamiento social, aportan una información más detallada acerca de la condición del paciente, sin embargo su tiempo de administración es mayor.
Llama la atención que instrumentos clásicos y reconocidos a nivel mundial como el ASI (17) y el MAD (21) no aparecen referenciados con la frecuencia que se esperaría. A pesar de que el área de la evaluación de los tratamientos es fundamental en la atención de los pacientes con TUS, no existe un consenso claro sobre qué categorías deben ser incluidas en la medición. La mayoría de instrumentos incluyen ítems y subescalas que presentan variabilidad en sus propiedades psicométricas; además, algunos de estos ítems y subescalas funcionan mejor que otros por lo que es difícil encontrar un instrumento que evalúe todos los aspectos del tratamiento de manera integral.
La evaluación de los tratamientos no solo incluye aspectos objetivamente cuantificables como abstinencia, reducción del consumo, mejoría de síntomas físicos, número de orinas negativas, ente otros, sino que también involucra variables subjetivas como capacidad de control sobre el consumo, espiritualidad, motivación para el tratamiento, relaciones familiares, satisfacción con el tratamiento, etc., lo cual complejiza aún más la aproximación al tema.
Un buen instrumento debe tener una variable de medida relevante para la población a la que va dirigida, un método de evaluación simple y de fácil acceso y aplicación, niveles de medida que reflejen una puntuación ordinal de la evaluación teniendo presente que una correcta definición aumenta la fiabilidad interevaluador y múltiples informantes para garantizar respuestas más confiables, objetivar cambios derivados del tratamiento y usar medidas de resultado libres de sesgos (84).
La decisión de usar un instrumento en lugar de otro debe considerar la disponibilidad de los mismos, los objetivos del tratamiento, el tipo de formato, su confiabilidad y validez, además de otros aspectos de conveniencia como la separación en módulos, la disponibilidad en formatos electrónicos, el idioma y los requerimientos en entrenamiento para su uso (85). Un instrumento no solo debe tener facilidad de uso y coherencia de estilo sino además adaptarse a las necesidades de los equipos clínicos; a pesar de esto, la presente revisión ha encontrado poca evidencia para apoyar este enfoque.
Conclusiones
Luego de la revisión de la literatura se observa que en los últimos 10 años se han desarrollado y validado múltiples instrumentos relacionados con diferentes aspectos de los TUS; no obstante, la utilización de estos es limitada por la diversidad de ambientes y tipos de terapia, lo que genera la necesidad de realizar ajustes y validaciones de los instrumentos de acuerdo al modelo de tratamiento empleado.
Existe una tendencia general hacia la formulación de instrumentos regionales de valoración de resultados de tratamiento o hacia la adaptación de instrumentos clásicos, así como a la simplificación de los mismos, la particularización sobre determinados aspectos del problema y el uso de escalas dimensionales.
No existe una prueba única que permita evaluar de manera integral los resultados del tratamiento para los TUS. Se señala la necesidad de continuar con la investigación, el desarrollo y la validación de instrumentos específicos que evalúen tratamientos complejos en instituciones que trabajan con modelos terapéuticos integrales.
Conflicto de intereses
Ninguno declarado por los autores.
Financiación
Este artículo se deriva del proyecto Desarrollo y Validación de un Índice de Medida para la Evaluación de la Efectividad del Tratamiento a la Dependencia de Drogas y/o Alcohol, el cual cuenta con el apoyo financiero Centro de Investigación para el Desarrollo y la Innovación (CIDI) de la Universidad Pontificia Bolivariana.
Agradecimientos
A los Doctores Diana Paola Cuesta Castro y José Julián Aristizábal por su apoyo en la realización de esta revisión.
Referencias
1. Instituto Nacional sobre el Abuso de Drogas. Principios de tratamientos para la drogadicción. Una guía basada en las investigaciones. Kentucky: Institutos Nacionales de la Salud, Departamento de Salud y Servicios Humanos de los EE.UU; 2010 [cited 2016 Nov 24]. Available from: https://goo.gl/LwaZEw.
2. World Health Organization. Workbook 3 : Needs Assessment. Evaluation of Psychoactive Substance Use Disorder Treatment. Washington, D.C.: WHO; 2000.
3. World Health Organization. WHO European Ministerial Conference on Mental Health. Facing the Challenges, Building Solutions. Helsinki: WHO; 2005 [cited 2016 Nov 24]. Available from: https://goo.gl/nxH85c.
4. National Institute on Drug Abuse. Understanding Drug Abuse and Addiction. Understanding Drug Abuse and Addiction. Washington, D.C.: drugabuse.gov; 2012 [cited 2016 Nov 24]. Available from: https://goo.gl/N77uxV.
5. Pérez J, Valderrama J, Cervera G, Rubio G, editors. Tratado SET de trastornos adictivos. Madrid: Editorial Médica Panamericana; 2006.
6. De Wilde J, Broekaert E, Rosseel Y. Problem severity profiles of clients in European therapeutic communities: Gender differences in various areas of functioning. Eur. Addict Res. 2006;12(3):128-37. http://doi.org/bm8xwv.
7. Leonard KE, Homish GG. Predictors of heavy drinking and drinking problems over the first 4 years of marriage. Psychol. Addict Behav. 2008;22(1):25-35. http://doi.org/b64cg2.
8. McLellan AT, Cacciola JC, Alterman AI, Rikoon SH, Carise D. The Addiction Severity Index at 25: origins, contributions and transitions. Am. J. Addict. 2006;15(2):113-24. http://doi.org/dnxzcv.
9. National Institute on Drug Abuse. Enfoques para el tratamiento de la drogadicción. Washington, D.C.: drugabuse.gov; 2009 [cited 2016 Nov 24]. Available from: https://goo.gl/WJG6Iu.
10. Butler Center for Research. Outcomes of alcohol/Other drugs dependency treatment. Minnesota: Butler center of research; 2011.
11. López MF, Compton WM, Grant BF, Breiling JP. Dimensional approaches in diagnostic classification: a critical appraisal. Int. J. Methods Psychiatr. Res. 2007;16(Suppl 1):S6-7. http://doi.org/fnpkzx.
12. Helzer JE, Bucholz KK, Gossop M. A dimensional option for the diagnosis of substance dependence in DSM-V. Int. J. Methods Psychiatr. Res. 2007;16(Suppl 1):S24-33. http://doi.org/bbcdc6.
13. Long CG, Hollin CR. Assessing comorbid substance use in detained psychiatric patients: issues and instruments for evaluating treatment outcome. Subst. Use Misuse. 2009;44(11):1602-41. http://doi.org/d9m8nb.
14. Wing JK, Beevor AS, Curtis RH, Park SB, Hadden S, Burns A. Health of the Nation Outcome Scales (HoNOS). Research and development. Br. J. Psychiatry. 1998;172(1):11-8. http://doi.org/cgmw2r.
15. McLellan AT, Luborsky L, Woody GE, O’Brien CP. An improved diagnostic evaluation instrument for substance abuse patients. The Addiction Severity Index. J. Nerv. Ment. Dis. 1980;168(1):26-33. http://doi.org/bszrdn.
16. Kessler F, Cacciola J, Alterman A, Faller S, Souza-Formigoni ML, Cruz MS, et al. Psychometric properties of the sixth version of the Addiction Severity Index (ASI-6) in Brazil. Rev. Bras. Psiquiatr. 2012;34(1):24-33. http://doi.org/f26qv2.
17. McLellan AT, Kushner H, Metzger D, Peters R, Smith I, Grissom G, et al. The fifth edition of the Addiction Severity Index. J. Subst. Abuse Treat. 1992;9(3):199-213. http://doi.org/dqnzd9.
18. Christo G, Spurrell S, Alcorn R. Validation of the Christo Inventory for Substance-misuse Services (CISS): a simple outcome evaluation tool. Drug Alcohol Depend. 2000;59(2):189-97. http://doi.org/b9vd7c.
19. Shwartz M, Mulvey KP, Woods D, Brannigan P, Plough A. Length of stay as an outcome in an era of managed care: An empirical study. J. Subst. Abuse Treat. 1997;14(1):11-8. http://doi.org/b3ksd7.
20. Toumbourou JW, Hamilton M, Fallon B. Treatment level progress and time spent in treatment in the prediction of outcomes following drug-free therapeutic community treatment. Addiction. 1998;93(7):1051-64. http://doi.org/bxrwz4.
21. Marsden J, Gossop M, Stewart D, Best D, Farrell M, Lehmann P, et al. The Maudsley Addiction Profile (MAP): a brief instrument for assessing treatment outcome. Addiction. 1998;93(12):1857-67. http://doi.org/dwgb95.
22. González-Saiz FM, Salvador-Carulla L, Martínez-Delgado JM, López-Cárdenas A, Ruz-Franzi I, Guerra-Díaz D. Indicador del tratamiento de la adicción a opiáceos. Cádiz: Servicio de Publicaciones de la Universidad de Cádiz; 1997.
23. Mueser KT, Drake RE, Clark RE, McHugo GJ, Mercer-MacFadden C, Ackerson TH. Toolkit for evaluating substance abuse in persons with severe mental illness. Cambridge: Evaluation Center@ HSRI; 1995.
24. Annis H, Graham JM, Foundation OAR. Situational confidence questionnaire (SCQ): User’s guide. Addiction Research Foundation; 1988.
25. Biener L, Abrams DB. The Contemplation Ladder: validation of a measure of readiness to consider smoking cessation. Health Psychol. 1991;10(5):360-5. http://doi.org/bpqbqt.
26. Litt MD, Kadden RM, Cooney NL, Kabela E. Coping skills and treatment outcomes in cognitive-behavioral and interactional group therapy for alcoholism. J. Consult. Clin. Psychol. 2003;71(1):118-28. http://doi.org/bs8pf5.
27. D’Zurilla TJ, Nezu AM, Maydeu-Olivares A. Social problem-solving inventory-revised: Technical manual. North Tonawanda, NY: Multi-Health Syst; 2002.
28. Tiffany ST, Singleton E, Haertzen CA, Henningfield JE. The development of a cocaine craving questionnaire. Drug Alcohol Depend. 1993;34(1):19-28. http://doi.org/fm2q2j.
29. Derogatis LR, Melisaratos N. The brief symptom inventory: an introductory report. Psychol Med. 1983;13(3):595-605. http://doi.org/dsdqw9.
30. Overall JE, Gorham DR. The brief psychiatric rating scale. Psychol Rep. 1962;10(3):799-812. http://doi.org/cjn2g5.
31. Hasin DS, Trautman KD, Miele GM, Samet S, Smith M, Endicott J. Psychiatric Research Interview for Substance and Mental Disorders (PRISM): reliability for substance abusers. Am. J. Psychiatry. 1996;153(9):1195-201. http://doi.org/btp5.
32. First MB, Spitzer RL, Gibbon M, Williams JB. Structured clinical interview for DSM-IV axis I disorders-patient edition (SCID-I/P, Version 2.0). New York: Biometrics Research, New York State Psychiatric Institute. 1995.
33. Patton JH, Stanford MS, Barratt ES. Factor structure of the Barratt impulsiveness scale. J. Clin. Psychol. 1995;51(6):768-74. http://doi.org/gsd.
34. Skevington SM, Lotfy M, O’Connell KA. The World Health Organization’s WHOQOL-BREF quality of life assessment: psychometric properties and results of the international field trial. A report from the WHOQOL group. Qual Life Res. 2004;13(2):299-310. http://doi.org/cgg6d6.
35. Horvath AO, Greenberg LS. Development of the Working Alliance Inventory. In: The Psychotherapeutic process: A research handbook. New York: Guilford; 1986. p. 529-556.
36. Gaston L. Reliability and criterion-related validity of the California Psychotherapy Alliance Scales - patient version. J. Consult. Clin. Psychology. 1991;3(1):68-74.
37. Ryan A, Holmes J, Hunt V, Dunlop A, Mammen K, Holland R, et al. Validation and implementation of the Australian treatment outcomes profile in specialist drug and alcohol settings. Drug Alcohol Rev. 2014;33(1):33-42. http://doi.org/btp9.
38. Simpson M, Lawrinson P, Copeland J, Gates P. The Alcohol Treatment Outcome Measure (ATOM): A new clinical tool for standardising outcome measurement for alcohol treatment. Addict Behav. 2009;34(1):121-4. http://doi.org/d4w5s4.
39. Lawrinson P, Copeland J, Indig D. Development and validation of a brief instrument for routine outcome monitoring in opioid maintenance pharmacotherapy services: The brief treatment outcome measure (BTOM). Drug Alcohol Depend. 2005;80(1):125-33. http://doi.org/bpq7rb.
40. Deering DE, Sellman JD, Adamson SJ, Horn J, Frampton CM. Development of a brief treatment instrument for routine clinical use with methadone maintenance treatment clients: The Methadone Treatment Index. Subst. Use Misuse. 2008;43(11):1666-80. http://doi.org/ff8sbj.
41. Wennberg P, Philips B, Jong K. The Swedish version of the Outcome Questionnaire (OQ-45): Reliability and factor structure in a substance abuse sample. Psychol. Psychother. 2010;83(3):325-9. http://doi.org/bnkwn5.
42. Stucky BD, Edelen MO, Vaughan CA, Tucker JS, Butler J. The psychometric development and initial validation of the DCI-A short form for adolescent therapeutic community treatment process. J. Subst. Abuse Treat. 2014;46(4):516-21. http://doi.org/btqc.
43. Malet L, Llorca PM, Beringuier B, Lehert P, Falissard B. AlQoL 9 for measuring quality of life in alcohol dependence. Alcohol Alcohol. 2006;41(2):181-7. http://doi.org/dwnk5w.
44. Chang KC, Wang JD, Tang HP, Cheng CM, Lin CY. Psychometric evaluation, using Rasch analysis, of the WHOQOL-BREF in heroin-dependent people undergoing methadone maintenance treatment: further item validation. Health Qual. Life Outcomes. 2014;12(1):148. http://doi.org/btqd.
45. Tung CK, Yeung SW, Chiang TP, Xu K, Lam M. Reliability and validity of the severity of dependence scale in a Chinese sample of treatment-seeking Ketamine users. East Asian Archives of Psychiatry. 2014 [cited 2015 Oct 13];24(4):456-64. Available from: https://goo.gl/XPpMHJ.
46. Zywiak WH, Neighbors CJ, Martin RA, Johnson JE, Eaton CA, Rohsenow DJ. The Important People Drug and Alcohol interview: Psychometric properties, predictive validity, and implications for treatment. J. Subst. Abuse Treat. 2009;36(3):321-30. http://doi.org/fbj6xc.
47. Martin G, Copeland J, Gilmour S, Gates P, Swift W. The adolescent cannabis problems questionnaire (CPQ-A): psychometric properties. Addict Behav. 2006;31(12):2238-48. http://doi.org/ddkhhw.
48. Meyers K, Hagan TA, McDermott P, Webb A, Randall M, Frantz J. Factor structure of the Comprehensive Adolescent Severity Inventory (CASI): Results of reliability, validity, and generalizability analyses. Am. J. Drug Alcohol Abuse. 2006;32(3):287-310. http://doi.org/d2fw6w.
49. Chinet L, Plancherel B, Bolognini M, Holzer L, Halfon O. Adolescent substance-use assessment: methodological issues in the use of the Adolescent Drug Abuse Diagnosis (ADAD). Subst. Use Misuse. 2007;42(10):1505-25. http://doi.org/bvxhnh.
50. Klein AA, Slaymaker VJ, Kelly JF. The 12 Step Affiliation and Practices Scale: Development and initial validation of a measure assessing 12 step affiliation. Addict Behav. 2011;36(11):1045-51. http://doi.org/btmww2.
51. Trujols J, Iraurgi I, Sinol N, Portella MJ, Pérez V, de los Cobos J. Satisfaction with methadone as a medication: psychometric properties of the Spanish version of the treatment satisfaction questionnaire for medication. J. Clin. Psychopharmacol. 2012;32(1):69-74. http://doi.org/fzn8kx.
52. Petry NM, Alessi SM, Ledgerwood DM, Sierra S. Psychometric properties of the contingency management competence scale. Drug Alcohol Depend. 2010;109(1-3):167-74. http://doi.org/c93q2h.
53. Chicharro-Romero J, Pedrero-Perez E, Perez-López M. Autoeficacia para resistirse al consumo de sustancias como predictora de resultados de tratamiento y su relación con variables de personalidad: estudio de una muestra de adictos con eñ DTCQ, el VIP y el MCMI-II. Adicciones. 2007 [cited 2015 Oct 13];19(2):141-52. Available from: https://goo.gl/dx43V5.
54. Freyer-Adam J, Coder B, Ottersbach C, Tonigan JS, Rumpf HJ, John U, et al. The performance of two motivation measures and outcome after alcohol detoxification. Alcohol Alcohol. 2009;44(1):77-83. http://doi.org/cd8b5b.
55. Adamson SJ, Kay-Lambkin FJ, Baker AL, Lewin TJ, Thornton L, Kelly BJ, et al. An improved brief measure of cannabis misuse: the Cannabis Use Disorders Identification Test-Revised (CUDIT-R). Drug Alcohol Depend. 2010;110(1-2):137-43. http://doi.org/d4vqcb.
56. Parra GR, Martin CS, Clark DB. The drinking situations of adolescents treated for alcohol use disorders: A psychometric and alcohol-related outcomes investigation. Addict Behav. 2005;30(9):1725-36. http://doi.org/fm89mt.
57. Shuggi R, Mann RE, Zalcman RF, Chipperfield B, Nochajski T. Predictive validity of the RIASI: alcohol and drug use and problems six months following remedial program participation. Am. J. Drug Alcohol Abuse. 2006;32(1):121-33. http://doi.org/dgtdr8.
58. Hsu SH, Collins SE, Marlatt GA. Examining psychometric properties of distress tolerance and its moderation of mindfulness-based relapse prevention effects on alcohol and other drug use outcomes. Addict Behav. 2013;38(3):1852-8. http://doi.org/btqg.
59. Lapham SC, McMillan GP. Open-label pilot study of extended-release naltrexone to reduce drinking and driving among repeat offenders. J. Addict Med. 2011;5(3):163-9. http://doi.org/c4zx3q.
60. Mann K, Kiefer F, Smolka M, Gann H, Wellek S, Heinz A. Searching for responders to acamprosate and naltrexone in alcoholism treatment: rationale and design of the PREDICT study. Alcohol Clin. Exp. Res. 2009;33(4):674-83. http://doi.org/bcpjfm.
61. Lieb M, Palm U, Chiang S, Laubender RP, Nothdurfter C, Sarubin N, et al. Pharmacological challenge with naloxone and cue exposure in alcohol dependence: Results of a randomized, double-blind placebo-controlled trial. World J. Biol. Psychiatry. 2013;14(7):539-46. http://doi.org/btqh.
62. Dieckmann LH, Ramos AC, Silva EA, Justo LP, Sabioni P, Frade IF, et al. Effects of biperiden on the treatment of cocaine/crack addiction: A randomised, double-blind, placebo-controlled trial. Eur. Neuropsychopharmacol. 2014;24(8):1196-202. http://doi.org/btqj.
63. Verthein U, Schäfer I, Degkwitz P. Soziale Integration nach 4 Jahren Diamorphinbehandlung. Rehabilitation. 2013;52(4):243-50. http://doi.org/btqk.
64. Carpenter KM, Martinez D, Vadhan NP, Barnes-Holmes D, Nunes EV. Measures of attentional bias and relational responding are associated with behavioral treatment outcome for cocaine dependence. Am. J. Drug Alcohol Abuse. 2012;38(2):146-54. http://doi.org/fxpzn6.
65. Young RM, Connor JP, Feeney GF. Alcohol expectancy changes over a 12-week cognitive–behavioral therapy program are predictive of treatment success. J. Subst. Abuse Treat. 2011;40(1):18-25. http://doi.org/b4hv32.
66. Paddock SM, Edelen MO, Wenzel SL, Ebener P, Mandell W, Dahl J. Measuring changes in client-level treatment process in the therapeutic community (TC) with the Dimensions of Change Instrument (DCI). Am. J. Drug Alcohol Abuse. 2007;33(4):537-46. http://doi.org/dsndm8.
67. Lindahl ML, Berglund M, Tönnesen H. Case management in aftercare of involuntarily committed patients with substance abuse. A randomized trial. Nord. J. Psychiatry. 2013;67(3):197-203. http://doi.org/f24dcg.
68. Rizvi SL, Dimeff LA, Skutch J, Carroll D, Linehan MM. A pilot study of the DBT coach: an interactive mobile phone application for individuals with borderline personality disorder and substance use disorder. Behav. Ther. 2011;42(4):589-600. http://doi.org/bgjhhp.
69. Higgins ST, Heil SH, Dantona R, Donham R, Matthews M, Badger GJ. Effects of varying the monetary value of voucher-based incentives on abstinence achieved during and following treatment among cocaine-dependent outpatients. Addiction. 2007;102(2):271-81. http://doi.org/d3q592.
70. French MT, Salomé HJ, Sindelar JL, McLellan AT. Benefit-Cost Analysis of Addiction Treatment: Methodological Guidelines and Empirical Application Using the DATCAP and ASI. Health Serv. Res. 2002;37(2):433-55. http://doi.org/d9qjw4.
71. Mann K, Lemenager T, Hoffmann S, Reinhard I, Hermann D, Batra A, et al. Results of a double-blind, placebo-controlled pharmacotherapy trial in alcoholism conducted in Germany and comparison with the US COMBINE study. Addict Biol. 2013;18(6):937-46. http://doi.org/btqn.
72. Guerrini I, Gentili C, Nelli G, Guazzelli M. A follow up study on the efficacy of metadoxine in the treatment of alcohol dependence. Subst. Abuse Treat. Prev. Policy. 2006;1(1):35. http://doi.org/dhz48m.
73. Jimenez-Treviño L, Saiz PA, García-Portilla MP, Díaz-Mesa EM, Sánchez-Lasheras F, Burón P, et al. A 25-year follow-up of patients admitted to methadone treatment for the first time: mortality and gender differences. Addict Behav. 2011;36(12):1184-90. http://doi.org/d3p65v.
74. Midanik LT, Greenfield TK, Bond J. Addiction sciences and its psychometrics: the measurement of alcohol-related problems. Addiction. 2007;102(11):1701-10. http://doi.org/cwvgk4.
75. De Maeyer J, Vanderplasschen W, Lammertyn J, van Nieuwenhuizen C, Sabbe B, Broekaert E. Current quality of life and its determinants among opiate-dependent individuals five years after starting methadone treatment. Qual. Life Res. 2011;20(1):139-50. http://doi.org/cks6cx.
76. Ruff S, McCOMB JL, Coker CJ, Sprenkle DH. Behavioral Couples Therapy for the Treatment of Substance Abuse: A Substantive and Methodological Review of O’Farrell, Fals-Stewart, and Colleagues’ Program of Research. Fam Process. 2010;49(4):439-56. http://doi.org/c3hkg9.
77. Delic M, Pregelj P. Factors associated with the outcome of drug addiction treatment. Psychiatr. Danub. 2013;25(Suppl 2):S337-40.
78. Schulte SJ, Meier PS, Stirling J. Dual diagnosis clients’ treatment satisfaction - a systematic review. BMC Psychiatry. 2011;11(1):64. http://doi.org/c4527s.
79. Donovan D, Mattson ME, Cisler RA, Longabaugh R, Zweben A. Quality of life as an outcome measure in alcoholism treatment research. J. Stud. Alcohol Suppl. 2005;(15):119-39. http://doi.org/btqp.
80. Nateras-Domínguez A, Natero-Domíngues JO. El uso social de drogas: una mirada desconstruccionista. Iztapalapa. 2005;35:113-130.
81. Metaal P, Corda A, Galante A, Rossi D, Rose G, Boiteux L. En busca de los derechos: Usuarios de drogas y las respuestas estatales en América Latina. México, D.F.: Colectivo de Estudios Droga y Derechos; 2014.
82. Gates PJ, Sabioni P, Copeland J, Le Foll B, Gowing L. Psychosocial interventions for cannabis use disorder. Cochrane Database Syst. Rev. 2016;(5): CD005336. http://doi.org/btqq.
83. Klimas J, Field CA, Cullen W, O’Gorman CS, Glynn LG, Keenan E, et al. Psychosocial interventions to reduce alcohol consumption in concurrent problem alcohol and illicit drug users. Cochrane Database Syst. Rev. 2012;11: CD009269. http://doi.org/btqr.
84. Sánchez-Hervás E. Tratamientos psicológicos en adicciones: eficacia, limitaciones y propuestas para mejorar su implantación. Papeles del Psicólogo. In: Tratado SET de Trastornos Adictivos. Madrid: Editorial Médica Panamericana; 2004. p. 34-44.
85. Samet S, Waxman R, Hatzenbuehler M, Hasin DS. Assessing addiction: Concepts and instruments. Addict Sci. Clin. Pract. 2007;4(1):19-31. http://doi.org/df7pmx.
César Alexander Eslava Franco
“Mapas anatómicos”
Universidad Nacional de Colombia
Referencias
Instituto Nacional sobre el Abuso de Drogas. Principios de tratamientos para la drogadicción. Una guía basada en las investigaciones. Kentucky: Institutos Nacionales de la Salud, Departamento de Salud y Servicios Humanos de los EE.UU; 2010 [cited 2016 Nov 24]. Available from: https://goo.gl/LwaZEw.
World Health Organization. Workbook 3 : Needs Assessment. Evaluation of Psychoactive Substance Use Disorder Treatment. Washington, D.C.: WHO; 2000.
World Health Organization. WHO European Ministerial Conference on Mental Health. Facing the Challenges, Building Solutions. Helsinki: WHO; 2005 [cited 2016 Nov 24]. Available from: https://goo.gl/nxH85c.
National Institute on Drug Abuse. Understanding Drug Abuse and Addiction. Understanding Drug Abuse and Addiction. Washington, D.C.: drugabuse.gov; 2012 [cited 2016 Nov 24]. Available from: https://goo.gl/N77uxV.
Pérez J, Valderrama J, Cervera G, Rubio G, editors. Tratado SET de trastornos adictivos. Madrid: Editorial Médica Panamericana; 2006.
De Wilde J, Broekaert E, Rosseel Y. Problem severity profiles of clients in European therapeutic communities: Gender differences in various areas of functioning. Eur. Addict Res. 2006;12(3):128-37. http://doi.org/bm8xwv.
Leonard KE, Homish GG. Predictors of heavy drinking and drinking problems over the first 4 years of marriage. Psychol. Addict Behav. 2008;22(1):25-35. http://doi.org/b64cg2.
McLellan AT, Cacciola JC, Alterman AI, Rikoon SH, Carise D. The Addiction Severity Index at 25: origins, contributions and transitions. Am. J. Addict. 2006;15(2):113-24. http://doi.org/dnxzcv.
National Institute on Drug Abuse. Enfoques para el tratamiento de la drogadicción. Washington, D.C.: drugabuse.gov; 2009 [cited 2016 Nov 24]. Available from: https://goo.gl/WJG6Iu.
Butler Center for Research. Outcomes of alcohol/Other drugs dependency treatment. Minnesota: Butler center of research; 2011.
López MF, Compton WM, Grant BF, Breiling JP. Dimensional approaches in diagnostic classification: a critical appraisal. Int. J. Methods Psychiatr. Res. 2007;16(Suppl 1):S6-7. http://doi.org/fnpkzx.
Helzer JE, Bucholz KK, Gossop M. A dimensional option for the diagnosis of substance dependence in DSM-V. Int. J. Methods Psychiatr. Res. 2007;16(Suppl 1):S24-33. http://doi.org/bbcdc6.
Long CG, Hollin CR. Assessing comorbid substance use in detained psychiatric patients: issues and instruments for evaluating treatment outcome. Subst. Use Misuse. 2009;44(11):1602-41. http://doi.org/d9m8nb.
Wing JK, Beevor AS, Curtis RH, Park SB, Hadden S, Burns A. Health of the Nation Outcome Scales (HoNOS). Research and development. Br. J. Psychiatry. 1998;172(1):11-8. http://doi.org/cgmw2r.
McLellan AT, Luborsky L, Woody GE, O’Brien CP. An improved diagnostic evaluation instrument for substance abuse patients. The Addiction Severity Index. J. Nerv. Ment. Dis. 1980;168(1):26-33. http://doi.org/bszrdn.
Kessler F, Cacciola J, Alterman A, Faller S, Souza-Formigoni ML, Cruz MS, et al. Psychometric properties of the sixth version of the Addiction Severity Index (ASI-6) in Brazil. Rev. Bras. Psiquiatr. 2012;34(1):24-33. http://doi.org/f26qv2.
McLellan AT, Kushner H, Metzger D, Peters R, Smith I, Grissom G, et al. The fifth edition of the Addiction Severity Index. J. Subst. Abuse Treat. 1992;9(3):199-213. http://doi.org/dqnzd9.
Christo G, Spurrell S, Alcorn R. Validation of the Christo Inventory for Substance-misuse Services (CISS): a simple outcome evaluation tool. Drug Alcohol Depend. 2000;59(2):189-97. http://doi.org/b9vd7c.
Shwartz M, Mulvey KP, Woods D, Brannigan P, Plough A. Length of stay as an outcome in an era of managed care: An empirical study. J. Subst. Abuse Treat. 1997;14(1):11-8. http://doi.org/b3ksd7.
Toumbourou JW, Hamilton M, Fallon B. Treatment level progress and time spent in treatment in the prediction of outcomes following drugfree therapeutic community treatment. Addiction. 1998;93(7):1051-64. http://doi.org/bxrwz4.
Marsden J, Gossop M, Stewart D, Best D, Farrell M, Lehmann P, et al. The Maudsley Addiction Profile (MAP): a brief instrument for assessing treatment outcome. Addiction. 1998;93(12):1857-67. http://doi.org/dwgb95.
González-Saiz FM, Salvador-Carulla L, Martínez-Delgado JM, López-Cárdenas A, Ruz-Franzi I, Guerra-Díaz D. Indicador del tratamiento de la adicción a opiáceos. Cádiz: Servicio de Publicaciones de la Universidad de Cádiz; 1997.
Mueser KT, Drake RE, Clark RE, McHugo GJ, Mercer-MacFadden C, Ackerson TH. Toolkit for evaluating substance abuse in persons with severe mental illness. Cambridge: Evaluation Center@ HSRI; 1995.
Annis H, Graham JM, Foundation OAR. Situational confidence questionnaire (SCQ): User’s guide. Addiction Research Foundation; 1988.
Biener L, Abrams DB. The Contemplation Ladder: validation of a measure of readiness to consider smoking cessation. Health Psychol. 1991;10(5):360-5. http://doi.org/bpqbqt.
Litt MD, Kadden RM, Cooney NL, Kabela E. Coping skills and treatment outcomes in cognitive-behavioral and interactional group therapy for alcoholism. J. Consult. Clin. Psychol. 2003;71(1):118-28. http://doi.org/bs8pf5.
D’Zurilla TJ, Nezu AM, Maydeu-Olivares A. Social problem-solving inventory-revised: Technical manual. North Tonawanda, NY: Multi- Health Syst; 2002.
Tiffany ST, Singleton E, Haertzen CA, Henningfield JE. The development of a cocaine craving questionnaire. Drug Alcohol Depend. 1993;34(1):19-28. http://doi.org/fm2q2j.
Derogatis LR, Melisaratos N. The brief symptom inventory: an introductory report. Psychol Med. 1983;13(3):595-605. http://doi.org/dsdqw9.
Overall JE, Gorham DR. The brief psychiatric rating scale. Psychol Rep. 1962;10(3):799-812. http://doi.org/cjn2g5.
Hasin DS, Trautman KD, Miele GM, Samet S, Smith M, Endicott J. Psychiatric Research Interview for Substance and Mental Disorders (PRISM): reliability for substance abusers. Am. J. Psychiatry. 1996;153(9):1195-201. http://doi.org/btp5.
First MB, Spitzer RL, Gibbon M, Williams JB. Structured clinical interview for DSM-IV axis I disorders-patient edition (SCID-I/P, Version 2.0). New York: Biometrics Research, New York State Psychiatric Institute. 1995.
Patton JH, Stanford MS, Barratt ES. Factor structure of the Barratt impulsiveness scale. J. Clin. Psychol. 1995;51(6):768-74. http://doi.org/gsd.
Skevington SM, Lotfy M, O’Connell KA. The World Health Organization’s WHOQOL-BREF quality of life assessment: psychometric properties and results of the international field trial. A report from the WHOQOL group. Qual Life Res. 2004;13(2):299-310. http://doi.org/cgg6d6.
Horvath AO, Greenberg LS. Development of the Working Alliance Inventory. In: The Psychotherapeutic process: A research handbook. New York: Guilford; 1986. p. 529-556.
Gaston L. Reliability and criterion-related validity of the California Psychotherapy Alliance Scales - patient version. J. Consult. Clin. Psychology. 1991;3(1):68-74.
Ryan A, Holmes J, Hunt V, Dunlop A, Mammen K, Holland R, et al. Validation and implementation of the Australian treatment outcomes profile in specialist drug and alcohol settings. Drug Alcohol Rev. 2014;33(1):33-42. http://doi.org/btp9.
Simpson M, Lawrinson P, Copeland J, Gates P. The Alcohol Treatment Outcome Measure (ATOM): A new clinical tool for standardising outcome measurement for alcohol treatment. Addict Behav. 2009;34(1):121-4. http://doi.org/d4w5s4.
Lawrinson P, Copeland J, Indig D. Development and validation of a brief instrument for routine outcome monitoring in opioid maintenance pharmacotherapy services: The brief treatment outcome measure (BTOM). Drug Alcohol Depend. 2005;80(1):125-33. http://doi.org/bpq7rb.
Deering DE, Sellman JD, Adamson SJ, Horn J, Frampton CM. Development of a brief treatment instrument for routine clinical use with methadone maintenance treatment clients: The Methadone Treatment Index. Subst. Use Misuse. 2008;43(11):1666-80. http://doi.org/ff8sbj.
Wennberg P, Philips B, Jong K. The Swedish version of the Outcome Questionnaire (OQ-45): Reliability and factor structure in a substance abuse sample. Psychol. Psychother. 2010;83(3):325-9. http://doi.org/bnkwn5.
Stucky BD, Edelen MO, Vaughan CA, Tucker JS, Butler J. The psychometric development and initial validation of the DCI-A short form for adolescent therapeutic community treatment process. J. Subst. Abuse Treat. 2014;46(4):516-21. http://doi.org/btqc.
Malet L, Llorca PM, Beringuier B, Lehert P, Falissard B. AlQoL 9 for measuring quality of life in alcohol dependence. Alcohol Alcohol. 2006;41(2):181-7. http://doi.org/dwnk5w.
Chang KC, Wang JD, Tang HP, Cheng CM, Lin CY. Psychometric evaluation, using Rasch analysis, of the WHOQOL-BREF in heroin-dependent people undergoing methadone maintenance treatment: further item validation. Health Qual. Life Outcomes. 2014;12(1):148. http://doi.org/btqd.
Tung CK, Yeung SW, Chiang TP, Xu K, Lam M. Reliability and validity of the severity of dependence scale in a Chinese sample of treatment-seeking Ketamine users. East Asian Archives of Psychiatry. 2014 [cited 2015 Oct 13];24(4):456-64. Available from: https://goo.gl/XPpMHJ.
Zywiak WH, Neighbors CJ, Martin RA, Johnson JE, Eaton CA, Rohsenow DJ. The Important People Drug and Alcohol interview: Psychometric properties, predictive validity, and implications for treatment. J. Subst. Abuse Treat. 2009;36(3):321-30. http://doi.org/fbj6xc.
Martin G, Copeland J, Gilmour S, Gates P, Swift W. The adolescent cannabis problems questionnaire (CPQ-A): psychometric properties. Addict Behav. 2006;31(12):2238-48. http://doi.org/ddkhhw.
Meyers K, Hagan TA, McDermott P, Webb A, Randall M, Frantz J. Factor structure of the Comprehensive Adolescent Severity Inventory (CASI): Results of reliability, validity, and generalizability analyses. Am. J. Drug Alcohol Abuse. 2006;32(3):287-310. http://doi.org/d2fw6w.
Chinet L, Plancherel B, Bolognini M, Holzer L, Halfon O. Adolescent substance-use assessment: methodological issues in the use of the Adolescent Drug Abuse Diagnosis (ADAD). Subst. Use Misuse. 2007;42(10):1505-25. http://doi.org/bvxhnh.
Klein AA, Slaymaker VJ, Kelly JF. The 12 Step Affiliation and Practices Scale: Development and initial validation of a measure assessing 12 step affiliation. Addict Behav. 2011;36(11):1045-51. http://doi.org/btmww2.
Trujols J, Iraurgi I, Sinol N, Portella MJ, Pérez V, de los Cobos J. Satisfaction with methadone as a medication: psychometric properties of the Spanish version of the treatment satisfaction questionnaire for medication. J. Clin. Psychopharmacol. 2012;32(1):69-74. http://doi.org/fzn8kx.
Petry NM, Alessi SM, Ledgerwood DM, Sierra S. Psychometric properties of the contingency management competence scale. Drug Alcohol Depend. 2010;109(1-3):167-74. http://doi.org/c93q2h.
Chicharro-Romero J, Pedrero-Perez E, Perez-López M. Autoeficacia para resistirse al consumo de sustancias como predictora de resultados de tratamiento y su relación con variables de personalidad: estudio de una muestra de adictos con eñ DTCQ, el VIP y el MCMI-II. Adicciones. 2007 [cited 2015 Oct 13];19(2):141-52. Available from: https://goo.gl/dx43V5.
Freyer-Adam J, Coder B, Ottersbach C, Tonigan JS, Rumpf HJ, John U, et al. The performance of two motivation measures and outcome after alcohol detoxification. Alcohol Alcohol. 2009;44(1):77-83. http://doi.org/cd8b5b.
Adamson SJ, Kay-Lambkin FJ, Baker AL, Lewin TJ, Thornton L, Kelly BJ, et al. An improved brief measure of cannabis misuse: the Cannabis Use Disorders Identification Test-Revised (CUDIT-R). Drug Alcohol Depend. 2010;110(1-2):137-43. http://doi.org/d4vqcb.
Parra GR, Martin CS, Clark DB. The drinking situations of adolescents treated for alcohol use disorders: A psychometric and alcohol-related outcomes investigation. Addict Behav. 2005;30(9):1725-36. http://doi.org/fm89mt.
Shuggi R, Mann RE, Zalcman RF, Chipperfield B, Nochajski T. Predictive validity of the RIASI: alcohol and drug use and problems six months following remedial program participation. Am. J. Drug Alcohol Abuse. 2006;32(1):121-33. http://doi.org/dgtdr8.
Hsu SH, Collins SE, Marlatt GA. Examining psychometric properties of distress tolerance and its moderation of mindfulness-based relapse prevention effects on alcohol and other drug use outcomes. Addict Behav. 2013;38(3):1852-8. http://doi.org/btqg.
Lapham SC, McMillan GP. Open-label pilot study of extended-release naltrexone to reduce drinking and driving among repeat offenders. J. Addict Med. 2011;5(3):163-9. http://doi.org/c4zx3q.
Mann K, Kiefer F, Smolka M, Gann H, Wellek S, Heinz A. Searching for responders to acamprosate and naltrexone in alcoholism treatment: rationale and design of the PREDICT study. Alcohol Clin. Exp. Res. 2009;33(4):674-83. http://doi.org/bcpjfm.
Lieb M, Palm U, Chiang S, Laubender RP, Nothdurfter C, Sarubin N, et al. Pharmacological challenge with naloxone and cue exposure in alcohol dependence: Results of a randomized, double-blind placebo-controlled trial. World J. Biol. Psychiatry. 2013;14(7):539-46. http://doi.org/btqh.
Dieckmann LH, Ramos AC, Silva EA, Justo LP, Sabioni P, Frade IF, et al. Effects of biperiden on the treatment of cocaine/crack addiction: A randomised, double-blind, placebo-controlled trial. Eur. Neuropsychopharmacol. 2014;24(8):1196-202. http://doi.org/btqj.
Verthein U, Schäfer I, Degkwitz P. Soziale Integration nach 4 Jahren Diamorphinbehandlung. Rehabilitation. 2013;52(4):243-50. http://doi.org/btqk.
Carpenter KM, Martinez D, Vadhan NP, Barnes-Holmes D, Nunes EV. Measures of attentional bias and relational responding are associated with behavioral treatment outcome for cocaine dependence. Am. J. Drug Alcohol Abuse. 2012;38(2):146-54. http://doi.org/fxpzn6.
Young RM, Connor JP, Feeney GF. Alcohol expectancy changes over a 12-week cognitive–behavioral therapy program are predictive of treatment success. J. Subst. Abuse Treat. 2011;40(1):18-25. http://doi.org/b4hv32.
Paddock SM, Edelen MO, Wenzel SL, Ebener P, Mandell W, Dahl J. Measuring changes in client-level treatment process in the therapeutic community (TC) with the Dimensions of Change Instrument (DCI). Am. J. Drug Alcohol Abuse. 2007;33(4):537-46. http://doi.org/dsndm8.
Lindahl ML, Berglund M, Tönnesen H. Case management in aftercare of involuntarily committed patients with substance abuse. A randomized trial. Nord. J. Psychiatry. 2013;67(3):197-203. http://doi.org/f24dcg.
Rizvi SL, Dimeff LA, Skutch J, Carroll D, Linehan MM. A pilot study of the DBT coach: an interactive mobile phone application for individuals with borderline personality disorder and substance use disorder. Behav. Ther. 2011;42(4):589-600. http://doi.org/bgjhhp.
Higgins ST, Heil SH, Dantona R, Donham R, Matthews M, Badger GJ. Effects of varying the monetary value of voucher-based incentives on abstinence achieved during and following treatment among cocaine-dependent outpatients. Addiction. 2007;102(2):271-81. http://doi.org/d3q592.
French MT, Salomé HJ, Sindelar JL, McLellan AT. Benefit-Cost Analysis of Addiction Treatment: Methodological Guidelines and Empirical Application Using the DATCAP and ASI. Health Serv. Res. 2002;37(2):433-55. http://doi.org/d9qjw4.
Mann K, Lemenager T, Hoffmann S, Reinhard I, Hermann D, Batra A, et al. Results of a double-blind, placebo-controlled pharmacotherapy trial in alcoholism conducted in Germany and comparison with the US COMBINE study. Addict Biol. 2013;18(6):937-46. http://doi.org/btqn.
Guerrini I, Gentili C, Nelli G, Guazzelli M. A follow up study on the efficacy of metadoxine in the treatment of alcohol dependence. Subst. Abuse Treat. Prev. Policy. 2006;1(1):35. http://doi.org/dhz48m.
Jimenez-Treviño L, Saiz PA, García-Portilla MP, Díaz-Mesa EM, Sánchez-Lasheras F, Burón P, et al. A 25-year follow-up of patients admitted to methadone treatment for the first time: mortality and gender differences. Addict Behav. 2011;36(12):1184-90. http://doi.org/d3p65v.
Midanik LT, Greenfield TK, Bond J. Addiction sciences and its psychometrics: the measurement of alcohol-related problems. Addiction. 2007;102(11):1701-10. http://doi.org/cwvgk4.
De Maeyer J, Vanderplasschen W, Lammertyn J, van Nieuwenhuizen C, Sabbe B, Broekaert E. Current quality of life and its determinants among opiate-dependent individuals five years after starting methadone treatment. Qual. Life Res. 2011;20(1):139-50. http://doi.org/cks6cx.
Ruff S, McCOMB JL, Coker CJ, Sprenkle DH. Behavioral Couples Therapy for the Treatment of Substance Abuse: A Substantive and Methodological Review of O’Farrell, Fals-Stewart, and Colleagues’ Program of Research. Fam Process. 2010;49(4):439-56. http://doi.org/c3hkg9.
Delic M, Pregelj P. Factors associated with the outcome of drug addiction treatment. Psychiatr. Danub. 2013;25(Suppl 2):S337-40.
Schulte SJ, Meier PS, Stirling J. Dual diagnosis clients’ treatment satisfaction - a systematic review. BMC Psychiatry. 2011;11(1):64. http://doi.org/c4527s.
Donovan D, Mattson ME, Cisler RA, Longabaugh R, Zweben A. Quality of life as an outcome measure in alcoholism treatment research. J. Stud. Alcohol Suppl. 2005;(15):119-39. http://doi.org/btqp.
Nateras-Domínguez A, Natero-Domíngues JO. El uso social de drogas: una mirada desconstruccionista. Iztapalapa. 2005;35:113-130.
Metaal P, Corda A, Galante A, Rossi D, Rose G, Boiteux L. En busca de los derechos: Usuarios de drogas y las respuestas estatales en América Latina. México, D.F.: Colectivo de Estudios Droga y Derechos; 2014.
Gates PJ, Sabioni P, Copeland J, Le Foll B, Gowing L. Psychosocial interventions for cannabis use disorder. Cochrane Database Syst. Rev. 2016;(5): CD005336. http://doi.org/btqq.
Klimas J, Field CA, Cullen W, O’Gorman CS, Glynn LG, Keenan E, et al. Psychosocial interventions to reduce alcohol consumption in concurrent problem alcohol and illicit drug users. Cochrane Database Syst. Rev. 2012;11: CD009269. http://doi.org/btqr.
Sánchez-Hervás E. Tratamientos psicológicos en adicciones: eficacia, limitaciones y propuestas para mejorar su implantación. Papeles del Psicólogo. In: Tratado SET de Trastornos Adictivos. Madrid: Editorial Médica Panamericana; 2004. p. 34-44.
Samet S, Waxman R, Hatzenbuehler M, Hasin DS. Assessing addiction: Concepts and instruments. Addict Sci. Clin. Pract. 2007;4(1):19-31. http://doi.org/df7pmx.
Cómo citar
APA
ACM
ACS
ABNT
Chicago
Harvard
IEEE
MLA
Turabian
Vancouver
Descargar cita
Licencia
Derechos de autor 2017 Revista de la Facultad de Medicina

Esta obra está bajo una licencia Creative Commons Reconocimiento 3.0 Unported.
-





















