Manejo perioperatorio del paciente con síndrome de apnea-hipopnea obstructiva del sueño (SAHOS)
Perioperative management of patients with obstructive sleep apnea-hypopnea syndrome (OSAHS)
DOI:
https://doi.org/10.15446/revfacmed.v65n1Sup.59568Palabras clave:
Apnea del sueño obstructiva, Procedimientos quirúrgicos operativos, Complicaciones intraoperatorias, Anestesia, Hipnóticos y Sedantes. (es)Sleep Apnea, Obstructive, Surgical Procedures, Operative, Intraoperative Complications, Anesthesia, Hypnotics and Sedatives. (en)
Patients diagnosed with obstructive sleep apnea-hypopnea syndrome (OSAHS) can safely undergo a surgical procedure, even on an outpatient basis, if other comorbidities are adequately controlled. Continuous positive airway pressure (CPAP) treatment in patients with a confirmed diagnosis decreases the risk of long-term cardiovascular complications. Sedation should be done by an anesthesiologist, who must also monitor the patient and have the appropriate equipment to deal with emerging respiratory complications.
Procedures undergone by these patients should be performed in a hospital setting, in which a post-anesthetic care unit and staff are available for follow-up, at least for an hour after the procedure ends. CPAP treatment should be continued as ordered by the treating physician. Identifying patients with OSAHS risk during the preanesthetic evaluation is important to propose an anesthetic plan that reduces respiratory complications and improves airway management.
artículo de reflexión
DOI: https://doi.org/10.15446/revfacmed.v65n1Sup.59568
Manejo perioperatorio del paciente con síndrome de
apnea-hipopnea obstructiva del sueño (SAHOS)
Perioperative management of patients with obstructive sleep apnea-hypopnea syndrome (OSAHS)
Recibido: 12/08/2016. Aceptado: 12/05/2017.
Angélica Fajardo-Escolar1 • Ana Helena Perea-Bello1 • Patricia Hidalgo-Martínez2
1 Pontificia Universidad Javeriana - Hospital Universitario San Ignacio - Bogotá D.C. - Colombia.
2 Pontificia Universidad Javeriana - Hospital Universitario San Ignacio - Clínica del Sueño - Bogotá D. C. - Colombia.
Correspondencia: Patricia Hidalgo-Martínez. Clínica del Sueño, Hospital Universitario San Ignacio, Pontificia Universidad Javeriana. Carrera 7 No. 40-62, piso 9. Teléfono: +57 1 5946161, ext.: 3918. Bogotá D.C. Colombia. Correo electrónico: phidalgo@husi.org.co.
| Resumen |
Los pacientes con diagnóstico de síndrome de apnea-hipopnea obstructiva del sueño (SAHOS) pueden ser llevados de forma segura a cualquier procedimiento quirúrgico, incluso de manera ambulatoria si tienen control adecuado de sus otras comorbilidades. El tratamiento con presión positiva continúa en vía aérea (CPAP) en pacientes con diagnóstico confirmado disminuye el riesgo de presentar complicaciones cardiovasculares a largo plazo. La sedación debe ser hecha por un anestesiólogo, quien, además, debe vigilar al paciente y disponer del equipo adecuado para atender complicaciones respiratorias emergentes. Se sugiere que, en estos pacientes, los procedimientos sean hechos en el ámbito hospitalario, donde se tenga disponibilidad en la unidad de cuidados post-anestésicos y personal para monitoreo por al menos una hora tras finalizar el procedimiento. El tratamiento con CPAP debe continuar según sea ordenado por el médico tratante. Es importante que desde la valoración preanestésica se identifique a los pacientes con riesgo de SAHOS para lograr trazar un plan anestésico que disminuya las complicaciones a nivel respiratorio y del manejo de la vía área.
Palabras clave: Apnea del sueño obstructiva; Procedimientos quirúrgicos operativos; Complicaciones intraoperatorias; Anestesia; Hipnóticos y Sedantes (DeSC).
Fajardo-Escolar A, Perea-Bello AH, Hidalgo-Martínez P. Manejo peri-operatorio del paciente con síndrome de apnea-hipopnea obstructiva del sueño (SAHOS). Rev. Fac. Med. 2017;65:S81-5. Spanish. doi:
https://doi.org/10.15446/revfacmed.v65n1Sup.59568.
| Abstract |
Patients diagnosed with obstructive sleep apnea-hypopnea syndrome (OSAHS) can safely undergo a surgical procedure, even on an outpatient basis, if other comorbidities are adequately controlled. Continuous positive airway pressure (CPAP) treatment in patients with a confirmed diagnosis decreases the risk of long-term cardiovascular complications. Sedation should be done by an anesthesiologist, who must also monitor the patient and have the appropriate equipment to deal with emerging respiratory complications.
Procedures undergone by these patients should be performed in a hospital setting, in which a post-anesthetic care unit and staff are available for follow-up, at least for an hour after the procedure ends. CPAP treatment should be continued as ordered by the treating physician. Identifying patients with OSAHS risk during the preanesthetic evaluation is important to propose an anesthetic plan that reduces respiratory complications and improves airway management.
Keywords: Sleep Apnea, Obstructive; Surgical Procedures, Operative; Intraoperative Complications; Anesthesia; Hypnotics and Sedatives (MeSH).
Fajardo-Escolar A, Perea-Bello AH, Hidalgo-Martínez P. [Perioperative management of patients with obstructive sleep apnea-hypopnea syndrome (OSAHS)]. Rev. Fac. Med. 2017;65:S81-5. Spanish. doi:
https://doi.org/10.15446/revfacmed.v65n1Sup.59568.
Introducción
Los pacientes con diagnóstico de síndrome de apnea-hipopnea obstructiva del sueño (SAHOS), ya sea por esta enfermedad o por otra condición general con indicación quirúrgica, pueden ser llevados a procedimientos quirúrgicos y diagnósticos —ambulatorios u hospitalarios— que necesitan anestesia; por esto, el anestesiólogo debe estar en capacidad de evaluar y optimizar su estado preoperatorio, ajustar las condiciones perioperatorias, prevenir las posibles complicaciones intraoperatorias y detectar y tratar aquellas que lleguen a presentarse en la unidad de cuidados post-anestésicos (UCPA).
Aunque no se dispone de evidencia que confirme que la presencia de SAHOS es un factor de riesgo independiente para morbimortalidad perioperatoria (1), sí hay estudios que sugieren que estos pacientes tienen mayor riesgo de complicaciones relacionadas con patologías como hipertensión arterial, diabetes, obesidad y alteraciones anatómicas y fisiológicas en la vía aérea superior (VAS)(2).
Desarrollo
Valoración preanestésica
Aunque cada vez es más frecuente la presencia de SAHOS, la mayoría de pacientes no están diagnosticados y, por ende, no reciben tratamiento, lo que los hace más vulnerables a presentar las complicaciones perioperatorias antes mencionadas. A partir de esta consideración, se puede dividir la población con SAHOS en dos grupos: aquellos con diagnóstico por polisomnograma (PSG) y aquellos con sospecha de diagnóstico (2,3).
La valoración preanestésica de los pacientes con sospecha de SAHOS debe iniciar con una historia clínica y un examen físico detallados. Las características físicas relacionadas con esta enfermedad (obesidad, cuello ancho, malformaciones craneofaciales que afectan la vía área (VA), obstrucción nasal anatómica e hipertrofia de adenoides y de amígdalas) tienen una sensibilidad y especificidad del 50-60% para el diagnóstico. De este modo, surge la importancia de conocer las diferentes herramientas clínicas que han sido estudiadas para identificar aquellos pacientes con alto riesgo de padecer este síndrome, entre ellas The Epworth Sleepiness Scale Score (ESS); el Cuestionario de Berlín, con sensibilidad del 69% y especificidad del 56% (4); la lista de chequeo recomendada por la Asociación Americana de Anestesiología (ASA), con sensibilidad del 79%, y el cuestionario STOP-Bang (5), recomendado por la Sociedad de Anestesia Ambulatoria (SAMBA, por sus siglas en inglés) y con sensibilidad del 93% y especificidad del 43% (2).
El cuestionario STOP-Bang es el más recomendado en la literatura por su facilidad en la aplicación, su buena sensibilidad y su correlación de acuerdo al puntaje obtenido con la severidad del SAHOS. Un puntaje de 0 a 2 se relaciona con bajo riesgo, de 3 a 4 con riesgo intermedio y de 5 a 8 con alto riesgo para SAHOS moderado/severo (6). Además, según nuevas guías de SAMBA, un puntaje >6 se correlaciona con la presencia de SAHOS moderado/severo (6,7) (Tabla 1). Sin embargo, es pertinente mencionar que algunas de estas herramientas no han sido validadas hasta el momento para uso perioperatorio y hay reportes en la literatura que mencionan que no siempre son confiables, por lo que se recomienda complementar el estudio con el uso de oximetría nocturna (8), en caso de que no sea posible la realización de un PSG —estándar de oro para el diagnóstico— (7).
Tabla 1. Puntaje STOP-Bang.
|
S |
¿Usted ronca duro (lo suficiente para ser escuchado a través de una puerta cerrada)? |
Sí |
No |
|
T |
¿Usted se siente frecuentemente cansado, fatigado o somnoliento durante el día? |
Sí |
No |
|
O |
¿Hay alguien que lo haya observado detener su respiración mientras duerme? |
Sí |
No |
|
P |
¿Usted tiene o está en tratamiento para la hipertensión arterial? |
Sí |
No |
|
B |
Índice de masa corporal >35 kg/m2 |
Sí |
No |
|
A |
>50 años |
Sí |
No |
|
N |
Circunferencia del cuello >40cm |
Sí |
No |
|
G |
Es hombre |
Sí |
No |
Nota: Riesgo bajo de SAHOS: Sí en menos de tres preguntas; riesgo medio de SAHOS: sí en tres o cuatro preguntas; riesgo alto de SAHOS: sí en cinco o más preguntas.
Fuente: Elaboración con base en Chung et al. (9).
En definitiva, todo paciente con sospecha de SAHOS y puntaje >6 en el cuestionario de STOP-Bang debe ser manejado como si tuviera un SAHOS moderado/severo y debe ser llevado a cirugía, teniendo en cuenta todas las posibles complicaciones que puede presentar. No obstante, si se trata de una cirugía diferible, se recomienda esperar la realización del PSG para confirmar el diagnóstico y tomar las medidas pertinentes (4,5)
En el caso del paciente con diagnóstico de SAHOS por PSG, el tratamiento con CPAP debe continuar en el perioperatorio y en el post-operatorio inmediato, ya que ningún estudio ha demostrado que su uso aumente el riesgo de complicaciones quirúrgicas (10) y, en cambio, se ha demostrado que disminuye el riesgo de arritmias cardíacas, la variabilidad de la presión arterial, el perfil hemodinámico y el colapso faríngeo. Por otro lado, en pacientes con diagnóstico reciente y sin tratamiento iniciado o iniciado recientemente no se encuentra evidencia del beneficio de iniciar este tratamiento previo a la cirugía, ya que no hay acuerdo en el tiempo que se debe usar antes del evento anestésico para reducir el riesgo perioperatorio (11).
Manejo anestésico
Vía aérea/intubación
En relación con la premedicación, no se recomienda el uso de benzodiacepinas u opioides; de ser necesario, se debe considerar el uso de alfa-2 agonistas como la dexmedetomidina o clonidina (12,13). Es importante contar siempre con dispositivos para manejo de una crisis potencial de la VA; tener en cuenta, a la hora de instrumentar la VA, que se debe optimizar la posición del paciente elevando la cabeza en posición de olfateo si el paciente es obeso, y realizar una preoxigenación adecuada, incluso con tratamiento con CPAP (12). Dado que los pacientes con SAHOS tienen mayor riesgo de presentar reflujo gastroesofágico, algunas guías de manejo recomiendan realizar profilaxis previa a la inducción de la anestesia general (14).
Anestesia general
Se debe tener en cuenta que los opioides están relacionados con depresión respiratoria, por lo que se recomienda minimizar su uso o preferir anestesias balanceadas con remifentanil (4,12). En la medida de lo posible, el mantenimiento anestésico debería ser con una mezcla de propofol/remifentanil o agentes inhalados poco liposolubles, como el desfluorane (2,7). Asimismo, es de suma importancia considerar una estrategia analgésica multimodal que incluya antiinflamatorios no esteroideos (AINES), esteroides, ketamina, dexmedetomidina y anestésicos locales, todo esto con el fin de reducir el uso de opioides potentes en el post-operatorio que puedan aumentar el riesgo de complicaciones respiratorias en estos pacientes (10,15,16).
Anestesia regional
Es clara la ventaja del uso de la anestesia regional en pacientes con SAHOS, ya que con esta técnica es posible contar con un individuo totalmente alerta en el post-operatorio inmediato, se reduce la dosis de opioides para manejo del dolor y se evita la manipulación de la VA y sus potenciales complicaciones. Por esto, debería ser la primera opción anestésica en los pacientes con esta entidad cuando la cirugía planeada lo permita (2).
Vía aérea/extubación
Al igual que la intubación, la extubación en personas con SAHOS puede estar asociada con falla en la ventilación y desaturación; por eso debe realizarse con el paciente completamente despierto (con apertura ocular espontánea y que sigue órdenes) y solo tras la reversión o recuperación completa del bloqueo neuromuscular (1,10). Se recomienda que el paciente sea extubado con la cabecera elevada a 30 grados, con una fracción inspirada de oxígeno del 100% y con presión de soporte positiva durante los siguientes dos minutos antes de su traslado a recuperación (13).
Unidad de cuidado post-anestésico
Una vez en la UCPA, el paciente con SAHOS debe ser monitorizado con pulso-oximetría, presión arterial no invasiva y electrocardiografía; también se debe mantener la cabecera elevada, si lo permite la cirugía, y, si es necesario, suministrar oxígeno complementario.
Lo que impacta en la incidencia de la aparición de obstrucción de la VAS, apneas y desaturación durante esta fase de recuperación es, sin lugar a dudas, el estado de conciencia; por eso, es imperativo que el paciente con antecedente o sospecha de SAHOS esté completamente despierto, alerta y sin efectos residuales de la anestesia. Según las recomendaciones de la ASA, estos pacientes deben permanecer mínimo 3 horas en la UCPA y al menos 7 horas si llegan a presentar un episodio de apnea (10).
Manejo post quirúrgico/post-anestésico
La mayoría de las complicaciones post-operatorias ocurren en las 72 horas posteriores al procedimiento quirúrgico, con un pico de incidencia en las primeras 24 horas, esto debido al efecto residual de los anestésicos, al manejo del dolor con opioides y a la cirugía misma (11). La presentación de complicaciones respiratorias está relacionada de forma directa con la severidad del SAHOS, la cual determina el tiempo de observación del paciente en la UCPA o, en los casos de mayor severidad y en cirugía mayor, la necesidad de monitoreo continuo en la unidad de cuidados intensivos (UCI) (8). Sin embargo, ante la falta de estudios y evidencia, la decisión del lugar de observación —UCPA o UCI— debe ser individualizada para cada paciente y cada institución, teniendo en cuenta la severidad del síndrome, las comorbilidades del paciente y la complejidad de la cirugía realizada.
Sedación para procedimientos diagnósticos y quirúrgicos menores
La práctica de la anestesiología describe cuatro grados de modificación farmacológica del estado de conciencia del paciente que van desde la sedación hasta la anestesia general: I: ansiolisis, II: sedación consciente, III: sedación profunda y IV: anestesia general (Tabla 2).
Tabla 2. Niveles de sedación.
|
Grado |
Característica |
|
I: ansiolisis |
El paciente obedece órdenes y está hemodinámicamente estable. Ventilación espontánea. |
|
II: sedación consciente |
El paciente genera respuesta al estímulo táctil o verbal fuerte y está hemodinámicamente estable. Se requiere conocimiento de maniobras básicas de manejo de vía aérea. |
|
III: sedación profunda |
El paciente genera respuesta a estímulos dolorosos y está hemodinámicamente estable. Se requiere entrenamiento en manejo de dispositivos para asegurar vía aérea. |
|
IV: anestesia general |
El paciente no genera respuesta a estímulos dolorosos y está hemodinámicamente estable o comprometido. Se requiere asegurar vía aérea con dispositivo. |
Fuente: Elaboración con base en (16) e Ibarra et al. (17).
El paso de un nivel a otro puede ocurrir brevemente comprometiendo la seguridad y la vida del paciente (18). Por eso, las sociedades de anestesiología del mundo (18,19) y, en específico, la Sociedad Colombiana de Anestesiología y Reanimación (SCARE) recomiendan que, en caso de que se planee una sedación para pacientes en condiciones especiales (como SAHOS), esta debe estar a cargo de personal con entrenamiento; es decir, anestesiólogos que puedan manejar las complicaciones derivadas de la sedación, ya que la mayoría de los procedimientos requieren como mínimo un grado II (19,20).
Los pacientes con SAHOS llevados a procedimientos bajo sedación deben estar monitorizados con presión arterial no invasiva, pulsoxímetro y electrocardiograma, además deben contar con un acceso venoso permeable. De igual forma, los profesionales tratantes tienen que contar con entrenamiento y dispositivos para asegurar la VA en caso de ser necesario (20).
Los medicamentos utilizados para sedación por su perfil farmacocinético (como el propofol), los opioides de corta acción (como el fentanil o el remifentanil) y las benzodiacepinas de vida media corta e hidrosolubles (como el midazolam) producen obstrucción de la VAS (6,21). Estudios con resonancia magnética han demostrado disminución en el área transversal de la VAS a medida que aumenta la profundidad anestésica con las dosis ascendentes de propofol (21); este síntoma también se ve afectado, junto con el alto riesgo de obstrucción, por el uso de midazolam, sin embargo hasta el momento no está claro del todo si el efecto es dosis dependiente (19,21). La combinación de fentanil y propofol ocasiona disminución de los reflejos laríngeos, siendo el más afectado el de la tos (21,22), uno de los principales reflejos protectores de la VA.
Sobre otros agentes, la dexmedetomidina, un alfa-2 agonista con efectos ansiolíticos, analgésicos y sedativos, preserva la ventilación espontánea y no produce obstrucción de la VA (21). No obstante, requiere un bolo que se infunde en 10 minutos, seguido de una infusión continua. Varios estudios demuestran que, como único agente, no alcanza el plano adecuado para la realización de los procedimientos y, en cambio, puede retrasar el alta (20,21). La ketamina no produce depresión respiratoria ni obstrucción de la VA y relaja la musculatura bronquial (21), aunque debe ser administrada en compañía de una benzodiacepina para contrarrestar los efectos disociativos (alucinaciones).
Los pacientes con SAHOS tienen mayor riesgo de tener complicaciones respiratorias por las condiciones mencionadas con anterioridad; los medicamentos utilizados para sedación ocasionan, en menor o mayor grado dependiendo de la dosis, obstrucción de la VA por inhibición de los reflejos de esta y del centro respiratorio, por lo que esta población debe ser manejada por anestesiólogos que puedan anticipar y corregir cualquier complicación. Es recomendación de la ASA que los pacientes con SAHOS sometidos a sedación sean observados al menos por tres horas, pero no hay estudios que soporten esta recomendación hecha en consenso de expertos (23,24).
Para procedimiento bajo anestesia general/sedación IV
Pacientes con diagnóstico de SAHOS: pueden ser llevados de manera segura a cualquier procedimiento quirúrgico, incluso de manera ambulatoria si tienen control adecuado de sus otras comorbilidades. El tratamiento con CPAP en pacientes con diagnóstico confirmado disminuye el riesgo de presentar complicaciones cardiovasculares a largo plazo (2,15,25), pero, hasta el momento, no es claro el beneficio del inicio de este tratamiento en pacientes con reciente diagnóstico antes de ser llevados a un procedimiento quirúrgico.
Paciente con riesgo de SAHOS: es importante, desde la valoración pre-anestésica, identificar al paciente que está en riesgo de SAHOS para lograr trazar un plan anestésico que disminuya las complicaciones a nivel respiratorio y del manejo de la VA. No es necesario, con el nivel de evidencia actual, suspender o diferir el procedimiento por este motivo, sino más bien procurar llevar al paciente a cirugía bajo las mismas condiciones de un paciente ya diagnosticado con SAHOS (4,12,26) y, luego, direccionarlo para que se le estudie y documente su condición de forma apropiada.
Para procedimiento bajo sedación (sedación grados II-III)
Pacientes con diagnóstico de SAHOS: pueden ser llevados de manera segura a cualquier procedimiento bajo sedación (endoscopia, colonoscopia, broncoscopia, odontología, etc.) si se tiene el control adecuado de sus comorbilidades. La sedación debe ser hecha y vigilada por un anestesiólogo y este debe disponer del equipo necesario para manejar complicaciones respiratorias emergentes. Se sugiere que en estos pacientes los procedimientos sean hechos en el ámbito hospitalario, donde se tenga disponibilidad de UCPA y personal para monitoreo por al menos una hora tras el final del procedimiento. El tratamiento con CPAP debe continuar según sea ordenado por el médico tratante.
Paciente con riesgo de SAHOS: de nuevo, desde la valoración pre-anestésica, se debería identificar al paciente que está en riesgo para lograr trazar un plan de sedación que minimice la probabilidad de complicaciones respiratorias. No es necesario suspender o diferir el procedimiento bajo sedación por una sospecha de SAHOS, sino más bien se debe procurar llevar al paciente al procedimiento bajo las mismas condiciones de un paciente ya diagnosticado (4,12,27). En estos pacientes, los procedimientos pueden ser hechos en un consultorio, pero bajo la supervisión de un anestesiólogo y con monitoreo por al menos 1 hora después del procedimiento (Figura 1).
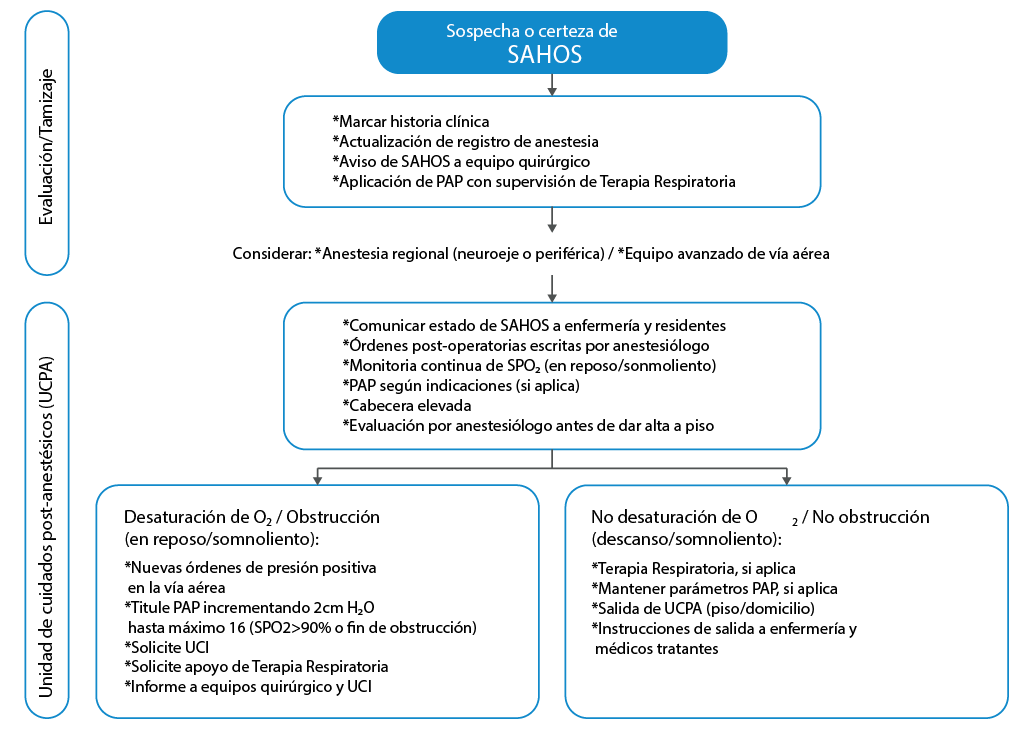
Figura 1. Guía para valoración y manejo peri-operatorio de SAHOS.
SAHOS: síndrome de apnea-hipopnea del sueño; PAP: presión aérea positiva; UCI: unidad de cuidados intensivos.
Fuente: Elaboración con base en Phoromayon et al. (28).
Conflicto de intereses
Ninguno declarado por los autores.
Financiación
Ninguna declarada por los autores.
Agradecimientos
A la Asociación Colombiana de Medicina Interna (ACMI® - Médicos para adultos), la Asociación Colombiana de Neurología (ACN) y la Asociación Colombiana de Sociedades Científicas (ACSC) por permitir a los autores usar sus instalaciones como lugar de reunión de trabajo.
Referencias
1.Abrishami A, Khajehdehi A, Chunq F. A systematic review of screening questionnaires for obstructive sleep apnea. Can J Anaesth. 2010;57(5):423-38. http://doi.org/djsmwr.
2.Young T, Hutton R, Finn L, Badr S, Palta M. The gender bias in sleep apnea diagnosis. Are women missed because they have different symptoms? Arch Intern Med. 1996;156(21):2445-51. http://doi.org/dbvfjm.
3.Young T, Evans L, Finn L, Palta M. Estimation of the clinically diagnosed proportion of sleep apnea syndrome in middle-aged men and women. Sleep. 1996;20(9):705-6.
4.Selim B, Won C, Yaggi HK. Cardiovascular consequences of sleep apnea. Clin Chest Med. 2010;31(2):203-20. http://doi.org/fmn5rf.
5.Chang ET, Yang MC, Wang H, Lai L. Snoring in a sitting position and neck circumference are predictors of sleep apnea in Chinese patients. Sleep Breath. 2014;18(1):133-6. http://doi.org/bnkb.
6.Chung SA, Yuan H, Chung F. A systemic review of obstructive sleep apnea and its implications for anesthesiologists. Anesth Analg. 2008;107(5):1543-63. http://doi.org/fgwn2k.
7.Vasu TS, Doghramji K, Cavallazzi R, Grewal R, Hirani A, Leiby B, et al. Obstructive sleep apnea syndrome and postoperative complications: a systematic review of the literature. Arch Otolaryngol Head Neck Surg. 2015;136(10):1020-4. http://doi.org/bn3r.
8.Degache F, Sforza E, Dauphinot V, Celle S, Garcin A, Collet P, et al. Relation of central fat mass to obstructive sleep apnea in the elderly. Sleep. 2013;36(4):501-7. http://doi.org/bn3s.
9.Chung F, Subramanyam R, Liao P, Sasaki E, Shapiro C, Sun Y. High STOP-Bang score indicates a high probability of obstructive sleep apnoea. Br J Anaesth. 2012;108(5):768-75. http://doi.org/bnq5.
10.Arnaud C, Dematteis M, Pepin JL, Baguet JP, Lévy P. Obstructive sleep apnea, immuno-inflammation, and atherosclerosis. Semin Immunopathol. 2009;31(1):113-25. http://doi.org/bzrkpz.
11.Isono S. Obstructive Sleep Apnea of obese Adults: pathophysiology and perioperative airway management. Anesthesiology. 2009;110(4):908-21. http://doi.org/dttvcb.
12.Del Olmo-Arroyo F, Hernandez-Castillo R, Soto A, Martínez J, Rodríguez-Cintrón W. Perioperative management of obstructive sleep apnea: a survey of Puerto Rico anesthesia providers. Sleep Breath. 2015;19(4):1141-6. http://doi.org/bn3t.
13.Raveendran R, Chung F. Perioperative consideration of obstructive sleep apnea in ambulatory surgery. Anesthesiol Clin. 2014;32(2):321-8. http://doi.org/bn3v.
14.Joshi GP, Ankichetty SP, Gan TJ, Chung F. Society for ambulatory anesthesia consensus statement on preoperative selection of adult patients with obstructive sleep apnea scheduled for ambulatory surgery. Anesth Analg. 2012;115(5):1060-8. http://doi.org/bn3w.
15.Woolf SH, Aron LY. The US health disadvantage relative to other high-income countries: findings from a National Research Council/Institute of Medicine report. JAMA. 2013;309(8):771-2. http://doi.org/bn3x.
16.American Society of Anesthesiologists Task Force on Sedation and Analgesia by Non-Anesthesiologists. Practice guidelines for sedation and analgesia by non-anesthesiologists. Anesthesiology. 2002;96(4):1004-17. http://doi.org/dqst27.
17.Ibarra P, Galindo M, Molano A, Niño C, Rubiano A, Echeverry P, et al. Recomendaciones para la sedación y la analgesia por médicos no anestesiólogos y odontólogos de pacientes mayores de 12 años. Revista Colombiana de Anestesiología. 2012;40(1):67-74. http://doi.org/f2fjnc.
18.Ankichetty S, Chung F. Considerations for patients with obstructive sleep apnea undergoing ambulatory surgery. Curr Opin Anaesthesiol. 2011;24(6):605-11. http://doi.org/cc67q6.
19.Chung F, Elsaid H. Screening for obstructive sleep apnea before surgery: why is it important? Curr Opin Anaesthesiol. 2009;22(3):405-11. http://doi.org/drpn5b.
20.Seet E, Chung F. Obstructive sleep apnea: preoperative assessment. Anesthesiol Clin. 2010;28(2):199-215. http://doi.org/fmpzbq.
21.Porhomayon J, Nader ND, Leissner KB, El-Solh AA. Respiratory Perioperative Management of Patients With Obstructive Sleep Apnea. J Intensive Care Med. 2012;29(3):145-53. http://doi.org/bn3z.
22.Liao P, Yegneswaran B, Vairavanathan S, Zilberman P, Chung F. Postoperative complications in patients with obstructive sleep apnea: a retrospective matched cohort study. Can J Anesth. 2009;56(11):819-28. http://doi.org/fgp374.
23.Apfelbaum JL, Silverstein JH, Chung FF, Connis RT, Fillmore RB, Hunt SE, et al. Practice guidelines for postanesthetic care: an updated report by the American Society of Anesthesiologists Task Force on Postanesthetic Care. Anesthesiology. 2013;118(2):291-307. http://doi.org/bn32.
24.Seet E, Chung F. Obstructive Sleep Apnea: Preoperative Assessment. Anesthesioliogy Clin. 2010;28(2):199-215. http://doi.org/fmpzbq.
25.Grupo español de sueño (GES). Documento de consenso Nacional sobre el síndrome de Apneas-hipoapneas del sueño (SAHS). Arch Bronconeumol. 2005;41(Supl 4):7-9.
26.Hillman DR, Platt PR, Eastwood PR. Anesthesia, Sleep, and Upper Airway Collapsibility. Anesthesiol Clin. 2010;28(3):443-55. http://doi.org/dcbbzh.
27.Chung F, Liao P, Fazel H, Elsaid H, Amirshahi B, Shapiro C, et al. What Are the Factors Predicting the Postoperative Apnea-Hypopnea Index? Chest. 2010;138(4):703A. http://doi.org/cs69xm.
28.Phoromayon J, El-Slh A, Chhangani S, Nader ND. The management of surgical patients with obstructive sleep apnea. Lung. 2011;189(5):359-67. http://doi.org/c9bv7w.

Jeison Malagón
“Paradisomnia”
Universidad Nacional de Colombia
Recibido: 12 de agosto de 2016; Aceptado: 12 de mayo de 2017
Resumen
Los pacientes con diagnóstico de síndrome de apnea-hipopnea obstructiva del sueño (SAHOS) pueden ser llevados de forma segura a cualquier procedimiento quirúrgico, incluso de manera ambulatoria si tienen control adecuado de sus otras comorbilidades. El tratamiento con presión positiva continúa en vía aérea (CPAP) en pacientes con diagnóstico confirmado disminuye el riesgo de presentar complicaciones cardiovasculares a largo plazo. La sedación debe ser hecha por un anestesiólogo, quien, además, debe vigilar al paciente y disponer del equipo adecuado para atender complicaciones respiratorias emergentes. Se sugiere que, en estos pacientes, los procedimientos sean hechos en el ámbito hospitalario, donde se tenga disponibilidad en la unidad de cuidados post-anestésicos y personal para monitoreo por al menos una hora tras finalizar el procedimiento. El tratamiento con CPAP debe continuar según sea ordenado por el médico tratante. Es importante que desde la valoración preanestésica se identifique a los pacientes con riesgo de SAHOS para lograr trazar un plan anestésico que disminuya las complicaciones a nivel respiratorio y del manejo de la vía área.
Palabras clave:
Apnea del sueño obstructiva, Procedimientos quirúrgicos operativos, Complicaciones intraoperatorias, Anestesia, Hipnóticos y Sedantes (DeSC).Abstract
Patients diagnosed with obstructive sleep apnea-hypopnea syndrome (OSAHS) can safely undergo a surgical procedure, even on an outpatient basis, if other comorbidities are adequately controlled. Continuous positive airway pressure (CPAP) treatment in patients with a confirmed diagnosis decreases the risk of long-term cardiovascular complications. Sedation should be done by an anesthesiologist, who must also monitor the patient and have the appropriate equipment to deal with emerging respiratory complications.
Procedures undergone by these patients should be performed in a hospital setting, in which a post-anesthetic care unit and staff are available for follow-up, at least for an hour after the procedure ends. CPAP treatment should be continued as ordered by the treating physician. Identifying patients with OSAHS risk during the preanesthetic evaluation is important to propose an anesthetic plan that reduces respiratory complications and improves airway management.
Keywords:
Sleep Apnea, Obstructive, Surgical Procedures, Operative, Intraoperative Complications, Anesthesia, Hypnotics and Sedatives (MeSH).Introducción
Los pacientes con diagnóstico de síndrome de apnea-hipopnea obstructiva del sueño (SAHOS), ya sea por esta enfermedad o por otra condición general con indicación quirúrgica, pueden ser llevados a procedimientos quirúrgicos y diagnósticos -ambulatorios u hospitalarios- que necesitan anestesia; por esto, el anestesiólogo debe estar en capacidad de evaluar y optimizar su estado preoperatorio, ajustar las condiciones perioperatorias, prevenir las posibles complicaciones intraoperatorias y detectar y tratar aquellas que lleguen a presentarse en la unidad de cuidados post-anestésicos (UCPA).
Aunque no se dispone de evidencia que confirme que la presencia de SAHOS es un factor de riesgo independiente para morbimortalidad perioperatoria 1, sí hay estudios que sugieren que estos pacientes tienen mayor riesgo de complicaciones relacionadas con patologías como hipertensión arterial, diabetes, obesidad y alteraciones anatómicas y fisiológicas en la vía aérea superior (VAS)2.
Desarrollo
Valoración preanestésica
Aunque cada vez es más frecuente la presencia de SAHOS, la mayoría de pacientes no están diagnosticados y, por ende, no reciben tratamiento, lo que los hace más vulnerables a presentar las complicaciones perioperatorias antes mencionadas. A partir de esta consideración, se puede dividir la población con SAHOS en dos grupos: aquellos con diagnóstico por polisomnograma (PSG) y aquellos con sospecha de diagnóstico 2,3.
La valoración preanestésica de los pacientes con sospecha de SAHOS debe iniciar con una historia clínica y un examen físico detallados. Las características físicas relacionadas con esta enfermedad (obesidad, cuello ancho, malformaciones craneofaciales que afectan la vía área (VA), obstrucción nasal anatómica e hipertrofia de adenoides y de amígdalas) tienen una sensibilidad y especificidad del 50-60% para el diagnóstico. De este modo, surge la importancia de conocer las diferentes herramientas clínicas que han sido estudiadas para identificar aquellos pacientes con alto riesgo de padecer este síndrome, entre ellas The Epworth Sleepiness Scale Score (ESS); el Cuestionario de Berlín, con sensibilidad del 69% y especificidad del 56% 4; la lista de chequeo recomendada por la Asociación Americana de Anestesiología (ASA), con sensibilidad del 79%, y el cuestionario STOP-Bang 5, recomendado por la Sociedad de Anestesia Ambulatoria (SAMBA, por sus siglas en inglés) y con sensibilidad del 93% y especificidad del 43% 2.
El cuestionario STOP-Bang es el más recomendado en la literatura por su facilidad en la aplicación, su buena sensibilidad y su correlación de acuerdo al puntaje obtenido con la severidad del SAHOS. Un puntaje de 0 a 2 se relaciona con bajo riesgo, de 3 a 4 con riesgo intermedio y de 5 a 8 con alto riesgo para SAHOS moderado/severo 6. Además, según nuevas guías de SAMBA, un puntaje >6 se correlaciona con la presencia de SAHOS moderado/severo 6,7 (Tabla 1). Sin embargo, es pertinente mencionar que algunas de estas herramientas no han sido validadas hasta el momento para uso perioperatorio y hay reportes en la literatura que mencionan que no siempre son confiables, por lo que se recomienda complementar el estudio con el uso de oximetría nocturna 8, en caso de que no sea posible la realización de un PSG -estándar de oro para el diagnóstico- 7.
Nota: Riesgo bajo de SAHOS: S׳'en menos de tres preguntas; riesgo medio de SAHOS: s׳'en tres o cuatro preguntas; riesgo alto de SAHOS: s׳'en cinco o más preguntas. Fuente: Elaboración con base en Chung et al. 9.Tabla 1: Puntaje STOP-Bang.

En definitiva, todo paciente con sospecha de SAHOS y puntaje >6 en el cuestionario de STOP-Bang debe ser manejado como si tuviera un SAHOS moderado/severo y debe ser llevado a cirugía, teniendo en cuenta todas las posibles complicaciones que puede presentar. No obstante, si se trata de una cirugía diferible, se recomienda esperar la realización del PSG para confirmar el diagnóstico y tomar las medidas pertinentes 4,5
En el caso del paciente con diagnóstico de SAHOS por PSG, el tratamiento con CPAP debe continuar en el perioperatorio y en el postoperatorio inmediato, ya que ningún estudio ha demostrado que su uso aumente el riesgo de complicaciones quirúrgicas 10 y, en cambio, se ha demostrado que disminuye el riesgo de arritmias cardíacas, la variabilidad de la presión arterial, el perfil hemodinámico y el colapso faríngeo. Por otro lado, en pacientes con diagnóstico reciente y sin tratamiento iniciado o iniciado recientemente no se encuentra evidencia del beneficio de iniciar este tratamiento previo a la cirugía, ya que no hay acuerdo en el tiempo que se debe usar antes del evento anestésico para reducir el riesgo perioperatorio 11.
Manejo anestésico
Vía aérea/intubación
En relación con la premedicación, no se recomienda el uso de benzodiacepinas u opioides; de ser necesario, se debe considerar el uso de alfa-2 agonistas como la dexmedetomidina o clonidina 12,13. Es importante contar siempre con dispositivos para manejo de una crisis potencial de la VA; tener en cuenta, a la hora de instrumentar la VA, que se debe optimizar la posición del paciente elevando la cabeza en posición de olfateo si el paciente es obeso, y realizar una preoxigenación adecuada, incluso con tratamiento con CPAP 12. Dado que los pacientes con SAHOS tienen mayor riesgo de presentar reflujo gastroesofágico, algunas guías de manejo recomiendan realizar profilaxis previa a la inducción de la anestesia general 14.
Anestesia general
Se debe tener en cuenta que los opioides están relacionados con depresión respiratoria, por lo que se recomienda minimizar su uso o preferir anestesias balanceadas con remifentanil 4,12. En la medida de lo posible, el mantenimiento anestésico debería ser con una mezcla de propofol/remifentanil o agentes inhalados poco liposolubles, como el desfluorane 2,7. Asimismo, es de suma importancia considerar una estrategia analgésica multimodal que incluya antiinflamatorios no esteroideos (AINES), esteroides, ketamina, dexmedetomidina y anestésicos locales, todo esto con el fin de reducir el uso de opioides potentes en el post-operatorio que puedan aumentar el riesgo de complicaciones respiratorias en estos pacientes 10,15,16.
Anestesia regional
Es clara la ventaja del uso de la anestesia regional en pacientes con SAHOS, ya que con esta técnica es posible contar con un individuo totalmente alerta en el post-operatorio inmediato, se reduce la dosis de opioides para manejo del dolor y se evita la manipulación de la VA y sus potenciales complicaciones. Por esto, debería ser la primera opción anestésica en los pacientes con esta entidad cuando la cirugía planeada lo permita 2.
Vía aérea/extubación
Al igual que la intubación, la extubación en personas con SAHOS puede estar asociada con falla en la ventilación y desaturación; por eso debe realizarse con el paciente completamente despierto (con apertura ocular espontánea y que sigue órdenes) y solo tras la reversión o recuperación completa del bloqueo neuromuscular 1,10. Se recomienda que el paciente sea extubado con la cabecera elevada a 30 grados, con una fracción inspirada de oxígeno del 100% y con presión de soporte positiva durante los siguientes dos minutos antes de su traslado a recuperación 13.
Unidad de cuidado post-anestésico
Una vez en la UCPA, el paciente con SAHOS debe ser monitorizado con pulso-oximetría, presión arterial no invasiva y electrocardiografía; también se debe mantener la cabecera elevada, si lo permite la cirugía, y, si es necesario, suministrar oxígeno complementario.
Lo que impacta en la incidencia de la aparición de obstrucción de la VAS, apneas y desaturación durante esta fase de recuperación es, sin lugar a dudas, el estado de conciencia; por eso, es imperativo que el paciente con antecedente o sospecha de SAHOS esté completamente despierto, alerta y sin efectos residuales de la anestesia. Según las recomendaciones de la ASA, estos pacientes deben permanecer mínimo 3 horas en la UCPA y al menos 7 horas si llegan a presentar un episodio de apnea 10.
Manejo post quirúrgico/post-anestésico
La mayoría de las complicaciones post-operatorias ocurren en las 72 horas posteriores al procedimiento quirúrgico, con un pico de incidencia en las primeras 24 horas, esto debido al efecto residual de los anestésicos, al manejo del dolor con opioides y a la cirugía misma 11. La presentación de complicaciones respiratorias está relacionada de forma directa con la severidad del SAHOS, la cual determina el tiempo de observación del paciente en la UCPA o, en los casos de mayor severidad y en cirugía mayor, la necesidad de monitoreo continuo en la unidad de cuidados intensivos (UCI) 8. Sin embargo, ante la falta de estudios y evidencia, la decisión del lugar de observación -UCPA o UCI- debe ser individualizada para cada paciente y cada institución, teniendo en cuenta la severidad del síndrome, las comorbilidades del paciente y la complejidad de la cirugía realizada.
Sedación para procedimientos diagnósticos y quirúrgicos menores
La práctica de la anestesiología describe cuatro grados de modificación farmacológica del estado de conciencia del paciente que van desde la sedación hasta la anestesia general: I: ansiolisis, II: sedación consciente, III: sedación profunda y IV: anestesia general (Tabla 2).
Tabla 2: Niveles de sedación.

El paso de un nivel a otro puede ocurrir brevemente comprometiendo la seguridad y la vida del paciente 18. Por eso, las sociedades de anestesiología del mundo 18,19 y, en específico, la Sociedad Colombiana de Anestesiología y Reanimación (SCARE) recomiendan que, en caso de que se planee una sedación para pacientes en condiciones especiales (como SAHOS), esta debe estar a cargo de personal con entrenamiento; es decir, anestesiólogos que puedan manejar las complicaciones derivadas de la sedación, ya que la mayoría de los procedimientos requieren como mínimo un grado II 19,20.
Los pacientes con SAHOS llevados a procedimientos bajo sedación deben estar monitorizados con presión arterial no invasiva, pulsoxímetro y electrocardiograma, además deben contar con un acceso venoso permeable. De igual forma, los profesionales tratantes tienen que contar con entrenamiento y dispositivos para asegurar la VA en caso de ser necesario 20.
Los medicamentos utilizados para sedación por su perfil farmacocinético (como el propofol), los opioides de corta acción (como el fentanil o el remifentanil) y las benzodiacepinas de vida media corta e hidrosolubles (como el midazolam) producen obstrucción de la VAS 6,21. Estudios con resonancia magnética han demostrado disminución en el área transversal de la VAS a medida que aumenta la profundidad anestésica con las dosis ascendentes de propofol 21; este síntoma también se ve afectado, junto con el alto riesgo de obstrucción, por el uso de midazolam, sin embargo hasta el momento no está claro del todo si el efecto es dosis dependiente 19,21. La combinación de fentanil y propofol ocasiona disminución de los reflejos laríngeos, siendo el más afectado el de la tos 21,22, uno de los principales reflejos protectores de la VA.
Sobre otros agentes, la dexmedetomidina, un alfa-2 agonista con efectos ansiolíticos, analgésicos y sedativos, preserva la ventilación espontánea y no produce obstrucción de la VA 21. No obstante, requiere un bolo que se infunde en 10 minutos, seguido de una infusión continua. Varios estudios demuestran que, como único agente, no alcanza el plano adecuado para la realización de los procedimientos y, en cambio, puede retrasar el alta 20,21. La ketamina no produce depresión respiratoria ni obstrucción de la VA y relaja la musculatura bronquial 21, aunque debe ser administrada en compañía de una benzodiacepina para contrarrestar los efectos disociativos (alucinaciones).
Los pacientes con SAHOS tienen mayor riesgo de tener complicaciones respiratorias por las condiciones mencionadas con anterioridad; los medicamentos utilizados para sedación ocasionan, en menor o mayor grado dependiendo de la dosis, obstrucción de la VA por inhibición de los reflejos de esta y del centro respiratorio, por lo que esta población debe ser manejada por anestesiólogos que puedan anticipar y corregir cualquier complicación. Es recomendación de la ASA que los pacientes con SAHOS sometidos a sedación sean observados al menos por tres horas, pero no hay estudios que soporten esta recomendación hecha en consenso de expertos 23,24.
Para procedimiento bajo anestesia general/sedación IV
Pacientes con diagnóstico de SAHOS: pueden ser llevados de manera segura a cualquier procedimiento quirúrgico, incluso de manera ambulatoria si tienen control adecuado de sus otras comorbilidades. El tratamiento con CPAP en pacientes con diagnóstico confirmado disminuye el riesgo de presentar complicaciones cardiovasculares a largo plazo 2,15,25, pero, hasta el momento, no es claro el beneficio del inicio de este tratamiento en pacientes con reciente diagnóstico antes de ser llevados a un procedimiento quirúrgico.
Paciente con riesgo de SAHOS: es importante, desde la valoración pre-anestésica, identificar al paciente que está en riesgo de SAHOS para lograr trazar un plan anestésico que disminuya las complicaciones a nivel respiratorio y del manejo de la VA. No es necesario, con el nivel de evidencia actual, suspender o diferir el procedimiento por este motivo, sino más bien procurar llevar al paciente a cirugía bajo las mismas condiciones de un paciente ya diagnosticado con SAHOS 4,12,26 y, luego, direccionarlo para que se le estudie y documente su condición de forma apropiada.
Para procedimiento bajo sedación (sedación grados II-III)
Pacientes con diagnóstico de SAHOS: pueden ser llevados de manera segura a cualquier procedimiento bajo sedación (endoscopia, colonoscopia, broncoscopia, odontología, etc.) si se tiene el control adecuado de sus comorbilidades. La sedación debe ser hecha y vigilada por un anestesiólogo y este debe disponer del equipo necesario para manejar complicaciones respiratorias emergentes. Se sugiere que en estos pacientes los procedimientos sean hechos en el ámbito hospitalario, donde se tenga disponibilidad de UCPA y personal para monitoreo por al menos una hora tras el final del procedimiento. El tratamiento con CPAP debe continuar según sea ordenado por el médico tratante.
Paciente con riesgo de SAHOS: de nuevo, desde la valoración pre-anestésica, se debería identificar al paciente que está en riesgo para lograr trazar un plan de sedación que minimice la probabilidad de complicaciones respiratorias. No es necesario suspender o diferir el procedimiento bajo sedación por una sospecha de SAHOS, sino más bien se debe procurar llevar al paciente al procedimiento bajo las mismas condiciones de un paciente ya diagnosticado 4,12,27. En estos pacientes, los procedimientos pueden ser hechos en un consultorio, pero bajo la supervisión de un anestesiólogo y con monitoreo por al menos 1 hora después del procedimiento (Figura 1).
Figura 1: Guia para valoración y manejo peri-operatorio de SAHOS. SAHOS: s'ndrome de apnea-hipopnea del sueño; PAP: presión aérea positiva; UCI: unidad de cuidados intensivos.
Conflicto de intereses
Ninguno declarado por los autores.
Financiación
Ninguna declarada por los autores.
Agradecimientos
A la Asociación Colombiana de Medicina Interna (ACMI® -Médicos para adultos), la Asociación Colombiana de Neurología (ACN) y la Asociación Colombiana de Sociedades Científicas (ACSC) por permitir a los autores usar sus instalaciones como lugar de reunión de trabajo.
Referencias
Referencias
Abrishami A, Khajehdehi A, Chunq F. A systematic review of screening questionnaires for obstructive sleep apnea. Can J Anaesth. 2010;57(5):423-38. http://doi.org/djsmwr.
Young T, Hutton R, Finn L, Badr S, Palta M. The gender bias in sleep apnea diagnosis. Are women missed because they have different symptoms? Arch Intern Med. 1996;156(21):2445-51. http://doi.org/dbvfjm.
Young T, Evans L, Finn L, Palta M. Estimation of the clinically diagnosed proportion of sleep apnea syndrome in middle-aged men and women. Sleep. 1996;20(9):705-6.
Selim B, Won C, Yaggi HK. Cardiovascular consequences of sleep apnea. Clin Chest Med. 2010;31(2):203-20. http://doi.org/fmn5rf.
Chang ET, Yang MC, Wang H, Lai L. Snoring in a sitting position and neck circumference are predictors of sleep apnea in Chinese patients. Sleep Breath. 2014;18(1):133-6. http://doi.org/bnkb.
Chung SA, Yuan H, Chung F. A systemic review of obstructive sleep apnea and its implications for anesthesiologists. Anesth Analg. 2008;107(5):1543-63. http://doi.org/fgwn2k.
Vasu TS, Doghramji K, Cavallazzi R, Grewal R, Hirani A, Leiby B, et al. Obstructive sleep apnea syndrome and postoperative complications: a systematic review of the literature. Arch Otolaryngol Head Neck Surg. 2015;136(10):1020-4. http://doi.org/bn3r.
Degache F, Sforza E, Dauphinot V, Celle S, Garcin A, Collet P, et al. Relation of central fat mass to obstructive sleep apnea in the elderly. Sleep. 2013;36(4):501-7. http://doi.org/bn3s.
Chung F, Subramanyam R, Liao P, Sasaki E, Shapiro C, Sun Y. High STOP-Bang score indicates a high probability of obstructive sleep apnoea. Br J Anaesth. 2012;108(5):768-75. http://doi.org/bnq5.
Arnaud C, Dematteis M, Pepin JL, Baguet JP, Lévy P. Obstructive sleep apnea, immuno-inflammation, and atherosclerosis. Semin Immunopathol. 2009;31(1):113-25. http://doi.org/bzrkpz.
Isono S. Obstructive Sleep Apnea of obese Adults: pathophysiology and perioperative airway management. Anesthesiology. 2009;110(4):908-21. http://doi.org/dttvcb.
Del Olmo-Arroyo F, Hernandez-Castillo R, Soto A, Martínez J, Rodríguez-Cintrón W. Perioperative management of obstructive sleep apnea: a survey of Puerto Rico anesthesia providers. Sleep Breath. 2015;19(4):1141-6. http://doi.org/bn3t.
Raveendran R, Chung F. Perioperative consideration of obstructive sleep apnea in ambulatory surgery. Anesthesiol Clin. 2014;32(2):321-8. http://doi.org/bn3v.
Joshi GP, Ankichetty SP, Gan TJ, Chung F. Society for ambulatory anesthesia consensus statement on preoperative selection of adult patients with obstructive sleep apnea scheduled for ambulatory surgery. Anesth Analg. 2012;115(5):1060-8. http://doi.org/bn3w.
Woolf SH, Aron LY. The US health disadvantage relative to other high-income countries: findings from a National Research Council/Institute of Medicine report. JAMA. 2013;309(8):771-2. http://doi.org/bn3x.
American Society of Anesthesiologists Task Force on Sedation and Analgesia by Non-Anesthesiologists. Practice guidelines for sedation and analgesia by non-anesthesiologists. Anesthesiology. 2002;96(4):1004-17. http://doi.org/dqst27.
Ibarra P, Galindo M, Molano A, Niño C, Rubiano A, Echeverry P, et al. Recomendaciones para la sedación y la analgesia por médicos no anestesiólogos y odontólogos de pacientes mayores de 12 años. Revista Colombiana de Anestesiología. 2012;40(1):67-74. http://doi.org/f2fjnc.
Ankichetty S, Chung F. Considerations for patients with obstructive sleep apnea undergoing ambulatory surgery. Curr Opin Anaesthesiol. 2011;24(6):605-11. http://doi.org/cc67q6.
Chung F, Elsaid H. Screening for obstructive sleep apnea before surgery: why is it important? Curr Opin Anaesthesiol. 2009;22(3):405-11. http://doi.org/drpn5b.
Seet E, Chung F. Obstructive sleep apnea: preoperative assessment. Anesthesiol Clin. 2010;28(2):199-215. http://doi.org/fmpzbq.
Porhomayon J, Nader ND, Leissner KB, El-Solh AA. Respiratory Perioperative Management of Patients With Obstructive Sleep Apnea. J Intensive Care Med. 2012;29(3):145-53. http://doi.org/bn3z.
Liao P, Yegneswaran B, Vairavanathan S, Zilberman P, Chung F. Postoperative complications in patients with obstructive sleep apnea: a retrospective matched cohort study. Can J Anesth. 2009;56(11):819-28. http://doi.org/fgp374.
Apfelbaum JL, Silverstein JH, Chung FF, Connis RT, Fillmore RB, Hunt SE, et al. Practice guidelines for postanesthetic care: an updated report by the American Society of Anesthesiologists Task Force on Postanesthetic Care. Anesthesiology. 2013;118(2):291-307. http://doi.org/bn32.
Seet E, Chung F. Obstructive Sleep Apnea: Preoperative Assessment. Anesthesioliogy Clin. 2010;28(2):199-215. http://doi.org/fmpzbq.
Grupo español de sueño (GES). Documento de consenso Nacional sobre el síndrome de Apneas-hipoapneas del sueño (SAHS). Arch Bronconeumol. 2005;41(Supl 4):7-9.
Hillman DR, Platt PR, Eastwood PR. Anesthesia, Sleep, and Upper Airway Collapsibility. Anesthesiol Clin. 2010;28(3):443-55. http://doi.org/dcbbzh.
Chung F, Liao P, Fazel H, Elsaid H, Amirshahi B, Shapiro C, et al. What Are the Factors Predicting the Postoperative Apnea-Hypopnea Index? Chest. 2010;138(4):703A. http://doi.org/cs69xm.
Phoromayon J, El-Slh A, Chhangani S, Nader ND. The management of surgical patients with obstructive sleep apnea. Lung. 2011;189(5):359-67. http://doi.org/c9bv7w.
Cómo citar
APA
ACM
ACS
ABNT
Chicago
Harvard
IEEE
MLA
Turabian
Vancouver
Descargar cita
CrossRef Cited-by
1. Abigail Almaguer Valadez, Belia Garduño, Lilia Mayorga Padilla, Daniela Alejandra Becerril Gaitan. (2023). Obstructive Sleep Apnea. , p.349. https://doi.org/10.1007/978-3-031-35225-6_20.
Dimensions
PlumX
Visitas a la página del resumen del artículo
Descargas
Licencia
Derechos de autor 2017 Revista de la Facultad de Medicina

Esta obra está bajo una licencia Creative Commons Reconocimiento 3.0 Unported.
-






















