Análisis descriptivo del compromiso de órganos en niños con dengue grave en Neiva, Colombia
Descriptive analysis of organ involvement in children with severe dengue in Neiva, Colombia
DOI:
https://doi.org/10.15446/revfacmed.v65n4.59835Palabras clave:
Dengue, Miocarditis, Hepatitis, Encefalitis (es)Dengue, Myocarditis, Hepatitis, Encephalitis (en)
Introducción. La infección por dengue puede comprometer órganos como el miocardio y el hígado. Tal hecho puede agravar la evolución clínica, por ello estos órganos han sido considerados en la clasificación revisada de la Organización Mundial de la Salud (OMS) para esta enfermedad.
Objetivo. Describir la presencia de afectación por dengue en órganos como miocardio, hígado y sistema nervioso central (SNC) en niños de Neiva, Colombia
Materiales y métodos. Este estudio analizó 930 niños con diagnóstico de dengue confirmado que ingresaron al Hospital Universitario Hernando Moncaleano Perdomo de Neiva entre enero de 2009 y diciembre de 2010. Para el diagnóstico y estratificación clínica se usó la clasificación revisada de la OMS. La infección por dengue se confirmó por detección plasmática de NS1 o IgM específica. Se realizó seguimiento clínico y paraclínico diario durante toda la hospitalización.
Resultados. De los 930 niños, 105 fueron clasificados como dengue grave (DG) y, de estos, 19 presentaron órganos afectados. El miocardio fue el más comprometido (14 casos), seguido por el hígado (4 casos) y el SNC (1 caso).
Conclusión. El compromiso clínico del miocardio, el hígado o el SNC se observó en el 18% de los casos de niños con DG. Es necesario un diagnóstico y tratamiento oportuno de esta patología en niños.
Introduction: Dengue can compromise organs such as the myocardium and the liver. Clinical evolution may be aggravated by this fact, and for that reason, these organs have been considered in the revised classification of the World Health Organization (WHO) for this disease.
Objective: To describe the affectation caused by dengue in organs such as the myocardium, the liver and the central nervous system (CNS) in children from Neiva, Colombia.
Materials and methods: This study analyzed 930 children diagnosed with confirmed dengue and admitted to the Hernando Moncaleano Perdomo University Hospital of Neiva between January 2009 and December 2010. Diagnosis and clinical stratification were obtained based on the revised WHO classification. Dengue infection was confirmed by NS1 or specific IgM plasma detection. Daily clinical and paraclinical follow-up was performed during the full length of hospital stay.
Results: Out of 930 children, 105 were classified as severe dengue (SD) and, of these, 19 had affected organs. The myocardium was the most compromised organ (14 cases), followed by the liver (4 cases) and the CNS (1 case).
Conclusion: Clinical involvement of the myocardium, liver or CNS was observed in 18% of the cases of children with SD. A timely diagnosis and treatment of this pathology in children is necessary.
investigación original
DOI: https://doi.org/10.15446/revfacmed.v65n4.59835
Análisis descriptivo del compromiso de órganos en
niños con dengue grave en Neiva, Colombia
Descriptive analysis of organ involvement in children with severe dengue in Neiva, Colombia
Recibido: 31/08/2016. Aceptado: 13/11/2016.
Doris Martha Salgado1,2, Martha Rocío Vega1,2 • César Alberto Panqueba2 • Carlos Fernando Narváez2 • Jairo Antonio Rodríguez1,2
1 Hospital Universitario Hernando Moncaleano Perdomo de Neiva - Departamento de Pediatría - Neiva - Colombia.
2 Universidad Surcolombiana - Sede Neiva - Facultad de Salud - Grupo Parasitología y Medicina Tropical - Neiva - Colombia.
Correspondencia: Jairo Antonio Rodríguez. Grupo Parasitología y Medicina Tropical, Facultad de Salud, Universidad Surcolombiana. Carrera 14 No. 9-19, Teléfono: +57 8 8718077. Neiva. Colombia. Correo electrónico: jrodriguez@usco.edu.co.
| Resumen |
Introducción. La infección por dengue puede comprometer órganos como el miocardio y el hígado. Tal hecho puede agravar la evolución clínica, por ello estos órganos han sido considerados en la clasificación revisada de la Organización Mundial de la Salud (OMS) para esta enfermedad.
Objetivo. Describir la presencia de afectación por dengue en órganos como miocardio, hígado y sistema nervioso central (SNC) en niños de Neiva, Colombia
Materiales y métodos. Este estudio analizó 930 niños con diagnóstico de dengue confirmado que ingresaron al Hospital Universitario Hernando Moncaleano Perdomo de Neiva entre enero de 2009 y diciembre de 2010. Para el diagnóstico y estratificación clínica se usó la clasificación revisada de la OMS. La infección por dengue se confirmó por detección plasmática de NS1 o IgM específica. Se realizó seguimiento clínico y paraclínico diario durante toda la hospitalización.
Resultados. De los 930 niños, 105 fueron clasificados como dengue grave (DG) y, de estos, 19 presentaron órganos afectados. El miocardio fue el más comprometido (14 casos), seguido por el hígado (4 casos) y el SNC (1 caso).
Conclusión. El compromiso clínico del miocardio, el hígado o el SNC se observó en el 18% de los casos de niños con DG. Es necesario un diagnóstico y tratamiento oportuno de esta patología en niños.
Palabras clave: Dengue; Miocarditis; Hepatitis; Encefalitis (DeCS).
Salgado DM, Vega MR, Panqueba CA, Narváez CF, Rodríguez JA. Análisis descriptivo del compromiso de órganos en niños con dengue grave en Neiva, Colombia. Rev. Fac. Med. 2017;65(4):565-570. Spanish. doi:
https://doi.org/10.15446/revfacmed.v65n4.59835.
| Abstract |
Introduction: Dengue can compromise organs such as the myocardium and the liver. Clinical evolution may be aggravated by this fact, and for that reason, these organs have been considered in the revised classification of the World Health Organization (WHO) for this disease.
Objective: To describe the affectation caused by dengue in organs such as the myocardium, the liver and the central nervous system (CNS) in children from Neiva, Colombia.
Materials and methods: This study analyzed 930 children diagnosed with confirmed dengue and admitted to the Hernando Moncaleano Perdomo University Hospital of Neiva between January 2009 and December 2010. Diagnosis and clinical stratification were obtained based on the revised WHO classification. Dengue infection was confirmed by NS1 or specific IgM plasma detection. Daily clinical and paraclinical follow-up was performed during the full length of hospital stay.
Results: Out of 930 children, 105 were classified as severe dengue (SD) and, of these, 19 had affected organs. The myocardium was the most compromised organ (14 cases), followed by the liver (4 cases) and the CNS (1 case).
Conclusion: Clinical involvement of the myocardium, liver or CNS was observed in 18% of the cases of children with SD. A timely diagnosis and treatment of this pathology in children is necessary.
Keywords: Dengue; Myocarditis; Hepatitis; Encephalitis (MeSH).
Salgado DM, Vega MR, Panqueba CA, Narváez CF, Rodríguez JA. [Descriptive analysis of organ affection in severe dengue children in Neiva, Colombia]. Rev. Fac. Med. 2017;65(4):565-570. Spanish. doi:
https://doi.org/10.15446/revfacmed.v65n4.59835.
Introducción
El dengue ocupa el primer lugar a nivel mundial como enfermedad viral transmitida por artrópodos: 2 500 millones de personas están en riesgo y se estima que hay 90 millones de casos nuevos cada año, incluyendo 500 000 de dengue grave (DG). Se reporta mortalidad hasta de 10%, a pesar de que se conoce que una intervención oportuna puede reducirla a menos del 1% (1).
En América, desde el año 2010, se ha dado un incremento de 4.6 veces en el número de casos de dengue (2). Para Colombia, hasta la semana epidemiológica 17 de 2015, se notificaron 35 796 casos de esta enfermedad, de los cuales 35 318 (98.7%) corresponden a dengue y 478 (1.3%) a DG. 2 138 casos se presentaron en menores de 4 años, 28 de estos con DG; 3 180, en niños de 5 a 9 años, 72 de estos con DG, y 3 930, en niños de 10 a 14 años, 72 de estos con DG. El 80% de los casos de dengue proceden de los departamentos del Valle del Cauca, Tolima, Meta, Santander, Antioquía, Cundinamarca y Huila. A nivel nacional, la hospitalización para los casos de esta enfermedad con signos de alarma fue de 50.2% y para los casos de DG de 85.6%, además se han notificado 121 muertes probables por dengue.
El compromiso de órganos por dengue se presenta con poca frecuencia, sin embargo causa mortalidad. Por lo general, el dengue es un síndrome febril que se acompaña de manifestaciones como pérdida de apetito, nauseas, cefalea, dolor abdominal y, en algunas oportunidades, hemorragias menores (3). Los síntomas y signos encontrados en el dengue no son específicos, pues otras infecciones como leptospirosis, fiebre tifoidea, chikungunya o zika, entre otras, tienen manifestaciones clínicas similares (4).
La Organización Mundial de la Salud (OMS) propuso una nueva clasificación para promover la identificación clínica temprana y el tratamiento oportuno del dengue (5). La clasificación anterior dejaba espacio para casos no clasificables, denominados inusuales, en pacientes con manifestaciones graves que no cumplian los criterios de choque o hemorragia. La última clasificación divide los casos en dos grupos: a) dengue, que a su vez se subdivide en dengue con signos de alarma (DCSA) o sin signos de alarma (DSSA), y b) DG, definido por uno de los siguientes cuadros sindromáticos:
1. Fuga vascular severa, acumulación de líquidos con o sin choque
2. Sangrado severo
3. Daño severo de órgano, incluyendo compromiso hepático, encefalitis/encefalopatía, falla renal y disfunción miocárdica.
Estas manifestaciones contribuyen con la mortalidad y pueden ocurrir aún en ausencia de fuga vascular o choque (5,6), como ha sido mostrado en otro reporte realizado en Neiva, Colombia (7).
El objetivo del presente estudio es determinar la frecuencia y las características clínicas y bioquímicas del compromiso de órgano en niños con DG durante un periodo de dos años en Neiva.
Materiales y métodos
Descripción del estudio
Se realizó un estudio descriptivo de casos pediátricos en niños hospitalizados con diagnóstico confirmado de dengue y clasificados acorde a los criterios revisados por la OMS (5) en el Departamento de Pediatría del Hospital Universitario Hernando Moncaleano Perdomo de Neiva en un periodo comprendido entre enero de 2009 y diciembre de 2010. Este trabajo fue aprobado por el comité de ética del hospital donde se realizó la investigación; como requisito para la participación en el estudio, el consentimiento informado fue diligenciado por los padres o acudientes de los niños participantes.
Criterio de inclusión
Para asignar los criterios de inclusión del estudio se tuvo en cuenta la definición de la OMS que afirma que un paciente padece de dengue si presenta una enfermedad febril aguda de hasta 7 días, de origen no aparente, que se acompaña de dos o más de los siguientes síntomas: cefalea, dolor retro ocular, mialgias, artralgias, postración o exantema, acompañado o no de hemorragias. También son factores determinantes de esta enfermedad un hemograma sugestivo de enfermedad viral, los antecedentes de desplazamiento (hasta 15 días antes del inicio de síntomas) o el haber residido en un área endémica de dengue.
Criterios de inclusión para dengue con signos de alarma
Se incluyen a los pacientes que cumplen con la anterior definición y, además, presentan cualquiera de los siguientes signos de alarma: dolor abdominal intenso y continuo, vómito persistente, diarrea, somnolencia o irritabilidad, hipotensión postural, hepatomegalia dolorosa >2cm, disminución de la diuresis, caída de la temperatura, hemorragias en mucosas o caída abrupta de plaquetas (<100 000) asociada a hemoconcentración.
Criterio de inclusión para dengue grave
Se incluyeron pacientes con criterio de dengue que presentaran cualquiera de las siguientes manifestaciones: extravasación severa del plasma, hemorragias severas según criterio clínico o daño grave de órganos.
Criterios de exclusión
Se excluyeron a los pacientes con imposibilidad de seguimiento, enfermedad del colágeno, neoplasias, cardiopatía congénita o patología crónica o que rehusaran la inclusión en el estudio.
Definición de casos por dengue
Miocarditis: es la inflamación del miocardio identificada mediante criterios clínicos y marcadores bioquímicos, electrocardiográficos y ecocardiográficos. Los criterios clínicos incluyen presencia de alteraciones del ritmo cardiaco, falla cardiaca no explicable o paciente con choque que no responde a una adecuada reanimación hídrica. Dentro de los estudios paraclínicos se encuentran los bioquímicos como el aumento de CPK (creatin fosfoquinasa) y su fracción MB, aumento en el nivel de troponinas I (inhibitoria) o T (transportadora), alteraciones electrocardiográficas como bradicardia o taquiarritmias, trastornos en la repolarización en onda T, segmento ST y ecocardiográficas que revelen disfunción miocárdica (8).
Sospecha de encefalitis: es la presencia de fiebre, cefalea y alteración del estado de conciencia no explicado por otras causas como falla hepática, choque, trastorno hidroelectrolitico, hemorragia intracraneana, presencia de IgM dengue-específica o NS1 en plasma; tampoco se presenta ningún otro patógeno en LCR y las neuroimágenes son sugestivas de encefalitis (9).
Hepatitis: es definida teniendo en cuenta la alteración de las aminotransferasas en suero y se consideraron cifras mayores a 10 veces el valor de referencia y por encima de 1000 U/ml, que corresponden a hepatitis grave según la OMS. Constituye falla hepática si se asocia a hipoglicemia, acidosis y alteración de la coagulación (10).
ELISA para diagnóstico de dengue y diferenciación entre infección primaria o secundaria
La infección por dengue se confirmó mediante la determinación plasmática de IgM específica contra el virus del dengue o la presencia de la proteína viral NS1, ambas detectadas por prueba ELISA (11) o identificación de genoma viral por RT-PCR (12). Para esto, se recolectaron muestras de sangre venosa total periférica en tubos con EDTA durante la fase aguda de la enfermedad, se obtuvo el plasma y se guardó a -70ºC hasta su uso. No se realizó PCR en líquido cefaloraquídeo.
La IgM, la IgG —plasmáticos específicos de dengue— y la proteína NS1 se determinaron usando estuches comerciales Dengue IgM capture Elisa (Ref: E-DEN01M), Dengue IgG capture Elisa (Ref: E-DEN02G) y Dengue Early Elisa (Ref: E-DEN02P), respectivamente (todos de Panbio, Alere, Australia). Se determinó si la infección era primaria o secundaria mediante la positividad IgG o IgM, siendo primarios aquellos IgM positivos e IgG negativos y secundarios si las dos inmunoglobulinas son positivas; si solo la IgG es positiva, se considera positiva si el valor aumenta en dos tomas sucesivas o si la NS1 también es positiva.
Análisis estadístico
Se creó una base de datos que permitió tabular y registrar a diario los datos clínicos y paraclínicos encontrados en los pacientes del estudio durante su hospitalización.
Los datos se mostraron como medianas y rangos.
Se consideró que había diferencias estadísticas significativas con p<0.05 utilizando el paquete Graph Prism versión 5.0; también se usaron las pruebas no paramétricas de Mann Whitney y Kruskal Wallis. Si en Kruskal-Wallis p<0.05, se realizaron pruebas postest para establecer diferencias entre cada uno de los grupos.
Resultados
930 niños con dengue confirmado fueron incluidos en este estudio; de ellos, 825 fueron clasificados como DCSA y 105 como DG. El cuadro predominante en gravedad fue el choque con 83 casos (79%), seguido de organopatía con 19 (18.1%) y sangrado severo con 3 (2.9%). Los 19 casos de organopatía fueron 14 miocarditis, 4 hepatitis y 1 encefalitis. Todos los pacientes clasificados como DG fueron admitidos en la unidad de cuidados intensivos pediátrica. En la Tabla 1 se muestran 102 pacientes con DG y compromiso de órganos; 3 no se incluyeron, pues cursaban con sangrados severos.
Los días de fiebre al ingreso fueron iguales en todos los pacientes y tuvieron una media de 5 días, no hubo diferencia de género en miocarditis, choque o hepatitis; sin embargo, la miocarditis tuvo tendencia a ser más frecuente en varones (9 de 14) y en niños con mayor edad que aquellos con hepatitis: 54 meses en quienes presentaron miocarditis versus 19 meses en quienes presentaron hepatitis (p=0.021, Mann-Whitney test). El vómito fue la mayor manifestación gastrointestinal en todos los grupos, no obstante se encontró hepatomegalia de forma general. Aunque no fue significativo, llamó la atención la presencia de menor derrame pleural en pacientes con diagnóstico de hepatitis (Tabla 1).
De los 19 pacientes, 3 tuvieron infección primaria, un caso asociado a hepatitis, otro a miocarditis y otro a encefalitis, el resto fueron infecciones secundarias. En cuanto a los otros pacientes con cuadro de DG, el 86% fue secundario, guardando una proporción similar a lo descrito con el grupo de afección de órganos.
Se analizaron 149 muestras en el laboratorio mediante RT-PCR; de estas, 63 fueron positivas, 12 correspondieron a serotipo dengue 1 (DEN 1), 34 a DEN 2, 15 a DEN 3 y 2 a DEN 4. De los niños con compromiso de órganos, 2 fueron DEN2 (miocarditis y hepatitis), 1 fue DEN3 (encefalitis) y 1 fue DEN1 (miocarditis).
En cuanto a los hallazgos de laboratorio, se observó recuento leucocitario similar entre choque y miocarditis; el recuento leucocitario en los pacientes con hepatitis fue superior y se evidenció una tendencia no significativa de trombocitopenia (media de 26 000) en niños con choque. Las transaminasas fueron más altas en los niños con hepatitis que en los otros dos grupos (p=0.002) (Tabla 1). No hay diferencias significativas en los otros datos analizados. Los valores de CPK en los niños con miocarditis se determinaron presentando una media de
183 U/L y la fracción MB fue de 15.5 U/L, valor que corresponde al 8.5% de la CPK total. La miocarditis fue el compromiso más frecuente en esta serie de niños con DG. La Figura 1 muestra 4 electrocardiogramas con hallazgos usuales de esta inflamación.

Figura 1. Electrocardiogramas de pacientes con miocarditis por dengue.
A: Ritmo sinusal, bradicardia, (frecuencia cardiaca de 50 latidos por minuto) y alteraciones de la repolarización con onda T de baja amplitud de predominio en DII y AVF; B: Trastorno de la repolarización apical y lateral con ondas T planas y negativas; C: bradicardia sinusal (frecuencia cardiaca de 48 latidos por minuto) y alteraciones de la repolarización; D: muestra DII con taquicardia y alteraciones en la repolarización dada por T negativa.
Fuente: Documentos obtenidos durante la realización del estudio.
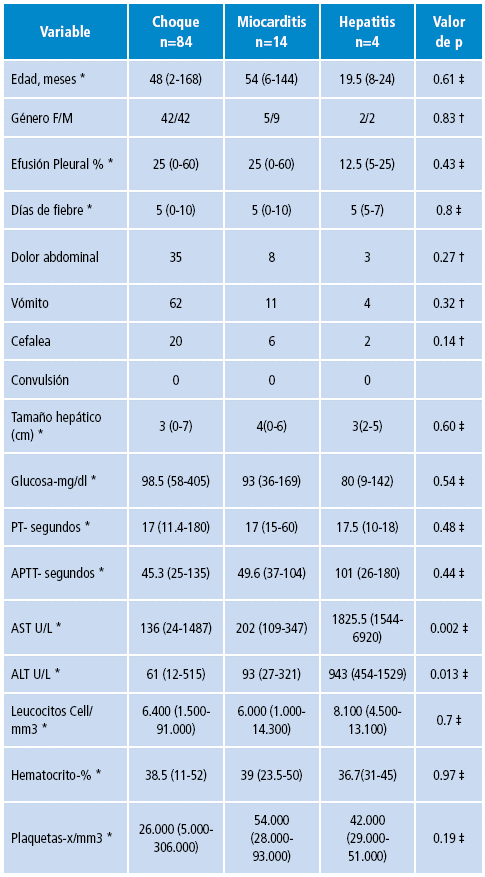
Tabla 1. Hallazgos clínicos y de laboratorio en pacientes con dengue grave.
|
Variable |
Choque n=84 |
Miocarditis n=14 |
Hepatitis n=4 |
Valor de p |
|
Edad, meses * |
48 (2-168) |
54 (6-144) |
19.5 (8-24) |
0.61 ‡ |
|
Género F/M |
42/42 |
5/9 |
2/2 |
0.83 † |
|
Efusión Pleural % * |
25 (0-60) |
25 (0-60) |
12.5 (5-25) |
0.43 ‡ |
|
Días de fiebre * |
5 (0-10) |
5 (0-10) |
5 (5-7) |
0.8 ‡ |
|
Dolor abdominal |
35 |
8 |
3 |
0.27 † |
|
Vómito |
62 |
11 |
4 |
0.32 † |
|
Cefalea |
20 |
6 |
2 |
0.14 † |
|
Convulsión |
0 |
0 |
0 |
|
|
Tamaño hepático (cm) * |
3 (0-7) |
4(0-6) |
3(2-5) |
0.60 ‡ |
|
Glucosa-mg/dl * |
98.5 (58-405) |
93 (36-169) |
80 (9-142) |
0.54 ‡ |
|
PT- segundos * |
17 (11.4-180) |
17 (15-60) |
17.5 (10-18) |
0.48 ‡ |
|
APTT- segundos * |
45.3 (25-135) |
49.6 (37-104) |
101 (26-180) |
0.44 ‡ |
|
AST U/L * |
136 (24-1487) |
202 (109-347) |
1825.5 (1544-6920) |
0.002 ‡ |
|
ALT U/L * |
61 (12-515) |
93 (27-321) |
943 (454-1529) |
0.013 ‡ |
|
Leucocitos Cell/mm3 * |
6.400 (1.500-91.000) |
6.000 (1.000-14.300) |
8.100 (4.500-13.100) |
0.7 ‡ |
|
Hematocrito-% * |
38.5 (11-52) |
39 (23.5-50) |
36.7(31-45) |
0.97 ‡ |
|
Plaquetas-x/mm3 * |
26.000 (5.000-306.000) |
54.000 (28.000-93.000) |
42.000 (29.000-51.000) |
0.19 ‡ |
PT: tiempo de protrombina; APTT: tiempo parcial de tromboplastina activado; AST: aspartato aminotransferasa; ALT: alanino aminotransferasa.
* Mediana.
† Valor p con prueba de Fisher.
‡ Valor p con prueba de Kruskal-Wallis.
Fuente: Elaboración propia.
De 10 ecocardiogramas realizados, 5 evidenciaron disminución en la fracción de eyección, 3 de ellos leves, con valores entre 41% y 55%, y 2 severos, con valores >20%; además, se encontraron alteraciones en la función contráctil localizada en septum (tres casos), en ventrículo izquierdo (dos casos), en ventrículo derecho (dos casos) o, de forma generalizada, biventricular (cuatro casos).
Discusión
En el presente estudio, 825 niños fueron clasificados como DCSA y 105 como DG, lo que se explica por el hecho de que el Hospital Universitario Hernando Moncaleano Perdomo de Neiva es un centro de referencia regional. El choque por dengue fue la manifestación más frecuente de DG, debido a fuga plasmática progresiva, haciendo su detección un desafío para el clínico dado que un retraso en el tratamiento puede resultar en mal pronóstico (5). Además del choque, se incluyen otras consecuencias como hemoconcentración, hipoalbuminemia, edemas, efusión pleural y ascitis, cuya magnitud está relacionada con la severidad de la fuga plasmática y de los volúmenes de líquido fugado (13). Se presentó el caso de un niño que falleció con choque y falla multiorgánica.
Del total de pacientes (n=930), 11.3% cursó con DG. La frecuencia de compromiso de órganos encontrada fue de 18.1%, similar a la descrita en la serie de Salgado et al. (7), constituyéndose en la segunda causa de DG, después del choque. La miocarditis, con 14 casos, ocupó el primer lugar dentro de las causas de organopatía, resaltando la importancia de su diagnóstico en dengue (7,14,15).
La patogénesis de la miocarditis dengue no se encuentra establecida con plenitud, sin embargo se describe como una condición multifactorial en la que el virus juega un papel importante con su capacidad de invadir el miocardiocito, llevándolo a lisis o apoptosis; de igual forma, en la lesión endotelial con fuga plasmática y edema se plantea compromiso intracelular por alteración en la homeostasis del calcio; todo esto, sumado al rol de los mediadores inmunológicos (citoquinas) sobre la célula miocárdica, da como resultado un proceso complejo no solo en su génesis, sino también en el diagnóstico y curso evolutivo (16). Algunos autores atribuyen las alteraciones cardiacas solo a hipoperfusión coronaria secundaria al choque (17).
La miocarditis asociada al dengue se ha descrito desde los años 70 con alteraciones, en su mayoría, en la conducción cardiaca. Estas observaciones soportan la hipótesis de que la disfunción muscular es la responsable de las arritmias, como se ha reportado con casos de bradiarritmias o taquiarritmias que llevan a bajo gasto cardiaco, evidenciadas en los trazados electrocardiográficos y demostradas con ecocardiogramas con bajas fracciones de eyección y acortamiento, franca disminución de los índices cardiaco y de Tei e hipoquinesia septal; los cambios en el segmento ST y de la onda T incluyen hemoconcentración (17,18), como se observó en varios casos de esta serie.
La disfunción ventricular se describió en India con componente tanto sistólico como diastólico y como causa de choque refractario (19). Algunos factores como la concentración intracelular de calcio incrementada, la activación del sistema de caspasas y el aumento en la apoptosis de las células musculares contribuyen aún más con la disfunción contráctil miocárdica (20). En otras publicaciones se ha descrito esta afección con miocarditis fulminante aguda severa en pacientes admitidos con choque por dengue en las unidades de cuidado intensivo (21).
En Colombia, en una cohorte de pacientes infectados por dengue de un estudio hecho también en Neiva, la miocarditis se reportó en el 10.7% de los casos (11 de 102). Tal estudio mostró alteraciones electrocardiográficas en todos los casos, como ha sido consistentemente reportado en la literatura y en el presente estudio, lo que refuerza la utilidad del electrocardiograma en áreas de alta endemicidad como el primer examen de tamizaje cuando se ha sospechado la miocarditis dengue (22).
Las anormalidades electrocardiográficas más comunes incluyen taquicardia sinusal con cambios inespecíficos en la onda T o en el segmento ST. También se han observado arritmias ventriculares o supraventriculares y alteraciones en el sistema de conducción cardiaco, tales como bloqueo atrio-ventricular e intraventricular (bloqueos de rama izquierda o derecha). Con frecuencia se observa elevación en el segmento ST, depresión en el segmento ST, inversión en la onda T y pobre progresión de la onda R y ondas Q (23) (Figura 1).
Uno de los parámetros importantes para evaluación de la afección miocárdica es la medida de las enzimas cardiacas como CPK MB y troponinas T e I. Al grupo de pacientes con miocarditis fue al único al que se le determinó la CPK MB, considerando que son indicadores de daño miocárdico, por lo que no fue realizada su evaluación para todos los pacientes del estudio. Analizando el resultado de la CPK MB, se observa que tiene una relación del 5% al 10% de la CPK total, con una CPK en un rango de 90-135 U/ml, lo que muestra un leve incremento de acuerdo con la hipótesis de que el daño principal del virus del dengue es a nivel funcional más que a lisis de la célula miocárdica (16).
Es importante mencionar el uso de otras pruebas que contribuyen a hacer el diagnóstico de miocarditis, tales como el ecocardiograma, que mostró disfunción miocárdica en 10 pacientes con diferentes componentes (septal, anteroseptal, ventrículo izquierdo y biventricular) y confirmó la severidad del compromiso miocárdico como se reportó con anterioridad (22).
La miocarditis observada en el curso de una enfermedad febril aguda con diagnóstico de dengue confirma el compromiso de este órgano como parte de la afectación del virus del dengue (23).
De los niños incluidos en este estudio, 4 tuvieron hepatitis con recuperación clínica satisfactoria, siendo más frecuente en lactantes. Aunque no hay un claro consenso en el límite de las aminotransferasas, De Souza et al., en el año 2004, sugirieron en Brasil que cuando el valor de las enzimas hepáticas se aumenta 10 veces más respecto al valor de referencia para la edad, hay mayor correlación con hepatitis (10). La OMS, en la clasificación revisada, fijó el valor de las aminotransferasas en >1000 U/mL. En esta serie, el pico de elevación fue encontrado entre el día 5 y 6 de la enfermedad (24).
Trabajos con niños afectados por dengue con edades entre 1 y 15 años en Tailandia describe fatalidad por hepatitis aguda causada por ese virus (25,26). En Brasil se hizo el reporte de nueve casos de hepatitis fatal con choque y se demostró la presencia del virus del dengue en los hepatocitos y en las células de Kupffer, además de cambios histológicos como necrosis hepática masiva y hepatitis aguda paucicelular (27).
Aunque los cuatro serotipos se han asociado a hepatitis fulminante por dengue, los serotipos 1 y 3 parecen tener mayor tropismo hepático (28). En Colombia, todos los serotipos circulan de forma simultánea (1), hecho que incrementa el riesgo de sufrir hepatitis dengue, como se evidenció en este estudio con la detección de los cuatro serotipos. En Santander, Colombia, se presentaron 913 casos de niños con fiebre dengue hemorrágico durante un periodo de 12 años; de estos, 10 fallecieron y a 3 se les demostró infiltración grasa hepática (29). La hepatitis, en general, suele ser benigna, pero en algunos casos puede evolucionar a falla hepática y muerte como desenlace de la infección.
El virus del dengue y la proteína viral NS1 han sido detectados en el líquido cefalorraquídeo, lo que sugiere la posibilidad de que este también puede afectar el SNC (30). Uno de los niños incluidos en este estudio, cuya evolución clínica fue favorable, tuvo convulsión febril asociada a vómito en el segundo día de la enfermedad; también tuvo edema cerebral evidente en la escanografía cerebral. Los pacientes con DG muestran un gran rango de manifestaciones neurológicas, incluyendo encefalopatía y convulsiones, que pueden ocurrir como primera manifestación clínica hasta en el 50% de los afectados por DG y hasta en el 16% en dengue primario (31).
Existen reportes relacionados con síndrome de Guillain Barré, encefalomielitis diseminada aguda, mielitis y neuritis óptica (32), por lo que se recomienda hacer un análisis clínico permanente para determinar afección neurológica por virus del dengue, realizar una escanografía y tener presente que puede haber compromiso oftalmológico, el cual hasta hace algunos años era desconocido.
El presente estudio refuerza la importancia del compromiso de órganos en sus tres formas más comunes en niños con diagnóstico de DG. Sin embargo, tiene la limitación de ser retrospectivo, por lo cual es importante realizar investigaciones prospectivas que consideren compromiso de órganos como causa de DG y establezcan su incidencia y el impacto que pueda tener en su morbimortalidad.
Conclusión
Si bien el choque es la presentación más común del DG, como ha sido reportado en la literatura y se demostró en este estudio, se resalta la importancia de considerar el daño de órganos como consecuencia de la infección por este virus, dado que su detección oportuna contribuirá con el objetivo de disminuir su mortalidad.
Conflicto de intereses
Ninguno declarado por los autores.
Financiación
Este trabajo fue financiado por la Vicerrectoría de Investigación y Proyección Social de la Universidad Surcolombiana.
Agradecimientos
Al Departamento de Pediatría del Hospital Universitario Hernando Moncaleano Perdomo de Neiva.
Referencias
1.San Martin JL, Brathwaite O, Zambrano B, Solorzano JO, Bouckenooghe A, Dayan GH, et al. The epidemiology of dengue in the americas over the last three decades: a worrisome reality. Am J Trop Med Hyg. 2010;82(1):128-35.
2.Brathwaite Dick O, San Martin JL, Montoya RH, del Diego J, Zambrano B, Dayan GH. The history of dengue outbreaks in the Americas. Am J Trop Med Hyg. 2012;87(4):584-93. http://doi.org/bn75.
3.Martinez-Torres E. Dengue y dengue hemorrágico: aspectos clínicos. Salud Publica Mex. 1995;37 Suppl:S29-44.
4.Staples JE, Breiman RF, Powers AM. Chikungunya fever: an epidemiological review of a re-emerging infectious disease. Clin Infect Dis. 2009;49(6):942-8. http://doi.org/cmrrx4.
5.World Health Organization, Special Programme for Research and Training in Tropical Diseases. Dengue: guidelines for diagnosis, treatment, prevention and control: new edition. Geneva; WHO; 2009.
6.Ranjit S, Kissoon N. Dengue hemorrhagic fever and shock syndromes. Pediatr Crit Care Med. 2011;12(1):90-100. http://doi.org/dmxc22.
7.Salgado DM, Rodríguez JA, Garzón M, Cifuentes G, Ibarra M, Vega MR, et al. Caracterización Clínica y Epidemiológica de Dengue Hemorrágico en Neiva, Colombia, 2004. Rev Salud Publica. 2007;9(1):53-63.
8.Kindermann I, Barth C, Mahfoud F, Ukena C, Lenski M, Yilmaz A, et al. Update on myocarditis. J Am Coll Cardiol. 2012;59(9):779-92. http://doi.org/f2nckj.
9.Carod-Artal FJ, Wichmann O, Farrar J, Gascon J. Neurological complications of dengue virus infection. Lancet Neurol. 2013;12(9):906-19. http://doi.org/f2nbg8
10.Souza LJ, Alves JG, Nogueira RM, Gicovate Neto C, Bastos DA, Siqueira EW, et al. Aminotransferase changes and acute hepatitis in patients with dengue fever: analysis of 1,585 cases. Braz J Infect Dis. 2004;8(2):156-63. http://doi.org/fwhs6n.
11.Sang CT, Cuzzubbo AJ, Devine PL. Evaluation of a commercial capture enzyme-linked immunosorbent assay for detection of immunoglobulin M and G antibodies produced during dengue infection. Clin Diagn Lab Immunol. 1998;5(1):7-10.
12.Lanciotti RS, Calisher CH, Gubler DJ, Chang GJ, Vorndam AV. Rapid detection and typing of dengue viruses from clinical samples by using reverse transcriptase-polymerase chain reaction. J Clin Microbiol. 1992;30(3):545-51.
13.Basuki PS, Budiyanto, Puspitasari D, Husada D, Darmowandowo W, Ismoedijanto, et al. Application of revised dengue classification criteria as a severity marker of dengue viral infection in Indonesia. Southeast Asian J Trop Med Public Health. 2010;41(5):1088-94.
14.Khongphatthanayothin A, Suesaowalak M, Muangmingsook S, Bhattarakosol P, Pancharoen C. Hemodynamic profiles of patients with dengue hemorrhagic fever during toxic stage: an echocardiographic study. Intensive Care Med. 2003;29(4):570-4. http://doi.org/fdg85r.
15.Nimmagadda SS, Mahabala C, Boloor A, Raghuram PM, Nayak UA. Atypical Manifestations of Dengue Fever (DF) - Where Do We Stand Today? J Clin Diagn Res. 2014;8(1):71-3. http://doi.org/b932.
16.Salgado DM, Eltit JM, Mansfield K, Panqueba C, Castro D, Vega MR, et al. Heart and skeletal muscle are targets of dengue virus infection. Pediatr Infect Dis J. 2010;29(3):238-42. http://doi.org/bs2t9g.
17.Wali JP, Biswas A, Chandra S, Malhotra A, Aggarwal P, Handa R, et al. Cardiac involvement in Dengue Haemorrhagic Fever. Int J Cardiol. 1998;64(1):31-6. http://doi.org/d76x6z.
18.Kabra SK, Juneja R, Madhulika, Jain Y, Singhal T, Dar L, et al. Myocardial dysfunction in children with dengue haemorrhagic fever. Natl Med J India. 1998;11(2):59-61.
19.Khongphatthanayothin A, Lertsapcharoen P, Supachokchaiwattana P, La-Orkhun V, Khumtonvong A, Boonlarptaveechoke C, et al. Myocardial depression in dengue hemorrhagic fever: prevalence and clinical description. Pediatr Crit Care Med. 2007;8(6):524-9. http://doi.org/cb7b7s.
20.Lee IK, Lee WH, Liu JW, Yang KD. Acute myocarditis in dengue hemorrhagic fever: a case report and review of cardiac complications in dengue-affected patients. Int J Infect Dis. 2010;14(10):e919-22. http://doi.org/fg63j6.
21.Shann F. Severe dengue: coming soon to a pediatric intensive care unit near you? Pediatr Crit Care Med. 2005;6(4):490-2.
22.Salgado DM, Panqueba CA, Castro D, Vega MR, Rodríguez JA. Miocarditis en Niños con Fiebre por Dengue Hemorrágico en un Hospital Universitario de Colombia. Rev Salud Publica. 2009;11(4):591-600. http://doi.org/dzgfh2.
23.Punja M, Mark DG, McCoy JV, Javan R, Pines JM, Brady W. Electrocardiographic manifestations of cardiac infectious-inflammatory disorders. Am J Emerg Med. 2010;28(3):364-77. http://doi.org/bkn5kb.
24.de Souza LJ, Gonçalves Carneiro H, Souto Filho JT, Ferreira de Souza T, Azevedo-Cortes V, Neto CG, et al. Hepatitis in dengue shock syndrome. Braz J Infect Dis. 2002;6(6):322-7.
25.Huerre MR, Lan NT, Marianneau P, Hue NB, Khun H, Hung NT, et al. Liver histopathology and biological correlates in five cases of fatal dengue fever in Vietnamese children. Virchows Arch. 2001;438(2):107-15.
26.Bhamarapravati N, Tuchinda P, Boonyapaknavik V. Pathology of Thailand haemorrhagic fever: a study of 100 autopsy cases. Ann Trop Med Parasitol. 1967;61(4):500-10. http://doi.org/b737.
27.de Macedo FC, Nicol AF, Cooper LD, Yearsley M, Pires AR, Nuovo GJ. Histologic, viral, and molecular correlates of dengue fever infection of the liver using highly sensitive immunohistochemistry. Diagn Mol Pathol. 2006;15(4):223-8. http://doi.org/dhb2c3.
28.Thein S, Aung MM, Shwe TN, Aye M, Zaw A, Aye K, et al. Risk factors in dengue shock syndrome. Am J Trop Med Hyg. 1997;56(5):566-72.
29.Méndez A, González G. Manifestaciones clínicas inusuales del dengue hemorrágico en niños. Biomedica. 2006;26(1):61-70.
30.Solomon T, Dung NM, Vaughn DW, Kneen R, Thao LT, Raengsakulrach B, et al. Neurological manifestations of dengue infection. Lancet. 2000;355(9209):1053-9. http://doi.org/bwcwdg.
31.Misra UK, Kalita J, Syam UK, Dhole TN. Neurological manifestations of dengue virus infection. J Neurol Sci. 2006;244(1-2):117-22. http://doi.org/cc3fsc.
32.Murthy JM. Neurological complication of dengue infection. Neurol India. 2010;58(4):581-4. http://doi.org/djsfgx.
Recibido: 31 de agosto de 2016; Aceptado: 13 de noviembre de 2016
Resumen
Introducción.
La infección por dengue puede comprometer órganos como el miocardio y el hígado. Tal hecho puede agravar la evolución clínica, por ello estos órganos han sido considerados en la clasificación revisada de la Organización Mundial de la Salud (OMS) para esta enfermedad.
Objetivo.
Describir la presencia de afectación por dengue en órganos como miocardio, hígado y sistema nervioso central (SNC) en niños de Neiva, Colombia
Materiales y métodos.
Este estudio analizó 930 niños con diagnóstico de dengue confirmado que ingresaron al Hospital Universitario Hernando Moncaleano Perdomo de Neiva entre enero de 2009 y diciembre de 2010. Para el diagnóstico y estratificación clínica se usó la clasificación revisada de la OMS. La infección por dengue se confirmó por detección plasmática de NS1 o IgM específica. Se realizó seguimiento clínico y paraclínico diario durante toda la hospitalización.
Resultados.
De los 930 niños, 105 fueron clasificados como dengue grave (DG) y, de estos, 19 presentaron órganos afectados. El miocardio fue el más comprometido (14 casos), seguido por el hígado (4 casos) y el SNC (1 caso).
Conclusión.
El compromiso clínico del miocardio, el hígado o el SNC se observó en el 18% de los casos de niños con DG. Es necesario un diagnóstico y tratamiento oportuno de esta patología en niños.
Palabras clave:
Dengue, Miocarditis, Hepatitis, Encefalitis (DeCS).Abstract
Introduction:
Dengue can compromise organs such as the myocardium and the liver. Clinical evolution may be aggravated by this fact, and for that reason, these organs have been considered in the revised classification of the World Health Organization (WHO) for this disease.
Objective:
To describe the affectation caused by dengue in organs such as the myocardium, the liver and the central nervous system (CNS) in children from Neiva, Colombia.
Materials and methods:
This study analyzed 930 children diagnosed with confirmed dengue and admitted to the Hernando Moncaleano Perdomo University Hospital of Neiva between January 2009 and December 2010. Diagnosis and clinical stratification were obtained based on the revised WHO classification. Dengue infection was confirmed by NS1 or specific IgM plasma detection. Daily clinical and paraclinical follow-up was performed during the full length of hospital stay.
Results:
Out of 930 children, 105 were classified as severe dengue (SD) and, of these, 19 had affected organs. The myocardium was the most compromised organ (14 cases), followed by the liver (4 cases) and the CNS (1 case).
Conclusion:
Clinical involvement of the myocardium, liver or CNS was observed in 18% of the cases of children with SD. A timely diagnosis and treatment of this pathology in children is necessary.
Keywords:
Dengue, Myocarditis, Hepatitis, Encephalitis (MeSH).Introducción
El dengue ocupa el primer lugar a nivel mundial como enfermedad viral transmitida por artrópodos: 2 500 millones de personas están en riesgo y se estima que hay 90 millones de casos nuevos cada año, incluyendo 500 000 de dengue grave (DG). Se reporta mortalidad hasta de 10%, a pesar de que se conoce que una intervención oportuna puede reducirla a menos del 1% 1.
En América, desde el año 2010, se ha dado un incremento de 4.6 veces en el número de casos de dengue 2. Para Colombia, hasta la semana epidemiológica 17 de 2015, se notificaron 35 796 casos de esta enfermedad, de los cuales 35 318 (98.7%) corresponden a dengue y 478 (1.3%) a DG. 2 138 casos se presentaron en menores de 4 años, 28 de estos con DG; 3 180, en niños de 5 a 9 años, 72 de estos con DG, y 3 930, en niños de 10 a 14 años, 72 de estos con DG. El 80% de los casos de dengue proceden de los departamentos del Valle del Cauca, Tolima, Meta, Santander, Antioquía, Cundinamarca y Huila. A nivel nacional, la hospitalización para los casos de esta enfermedad con signos de alarma fue de 50.2% y para los casos de DG de 85.6%, además se han notificado 121 muertes probables por dengue.
El compromiso de órganos por dengue se presenta con poca frecuencia, sin embargo causa mortalidad. Por lo general, el dengue es un síndrome febril que se acompaña de manifestaciones como pérdida de apetito, nauseas, cefalea, dolor abdominal y, en algunas oportunidades, hemorragias menores 3. Los síntomas y signos encontrados en el dengue no son específicos, pues otras infecciones como leptospirosis, fiebre tifoidea, chikungunya o zika, entre otras, tienen manifestaciones clínicas similares 4.
La Organización Mundial de la Salud (OMS) propuso una nueva clasificación para promover la identificación clínica temprana y el tratamiento oportuno del dengue 5. La clasificación anterior dejaba espacio para casos no clasificables, denominados inusuales, en pacientes con manifestaciones graves que no cumplian los criterios de choque o hemorragia. La última clasificación divide los casos en dos grupos: a) dengue, que a su vez se subdivide en dengue con signos de alarma (DCSA) o sin signos de alarma (DSSA), y b) DG, definido por uno de los siguientes cuadros sindromáticos:
-
Fuga vascular severa, acumulación de líquidos con o sin choque
-
Sangrado severo
-
Daño severo de órgano, incluyendo compromiso hepático, encefalitis/encefalopatía, falla renal y disfunción miocárdica.
Estas manifestaciones contribuyen con la mortalidad y pueden ocurrir aún en ausencia de fuga vascular o choque 5,6, como ha sido mostrado en otro reporte realizado en Neiva, Colombia 7.
El objetivo del presente estudio es determinar la frecuencia y las características clínicas y bioquímicas del compromiso de órgano en niños con DG durante un periodo de dos años en Neiva.
Materiales y métodos
Descripción del estudio
Se realizó un estudio descriptivo de casos pediátricos en niños hospitalizados con diagnóstico confirmado de dengue y clasificados acorde a los criterios revisados por la OMS 5 en el Departamento de Pediatría del Hospital Universitario Hernando Moncaleano Perdomo de Neiva en un periodo comprendido entre enero de 2009 y diciembre de 2010. Este trabajo fue aprobado por el comité de ética del hospital donde se realizó la investigación; como requisito para la participación en el estudio, el consentimiento informado fue diligenciado por los padres o acudientes de los niños participantes.
Criterio de inclusión
Para asignar los criterios de inclusión del estudio se tuvo en cuenta la definición de la OMS que afirma que un paciente padece de dengue si presenta una enfermedad febril aguda de hasta 7 días, de origen no aparente, que se acompaña de dos o más de los siguientes síntomas: cefalea, dolor retro ocular, mialgias, artralgias, postración o exantema, acompañado o no de hemorragias. También son factores determinantes de esta enfermedad un hemograma sugestivo de enfermedad viral, los antecedentes de desplazamiento (hasta 15 días antes del inicio de síntomas) o el haber residido en un área endémica de dengue.
Criterios de inclusión para dengue con signos de alarma
Se incluyen a los pacientes que cumplen con la anterior definición y, además, presentan cualquiera de los siguientes signos de alarma: dolor abdominal intenso y continuo, vómito persistente, diarrea, somnolencia o irritabilidad, hipotensión postural, hepatomegalia dolorosa >2cm, disminución de la diuresis, caída de la temperatura, hemorragias en mucosas o caída abrupta de plaquetas (<100 000) asociada a hemoconcentración.
Criterio de inclusión para dengue grave
Se incluyeron pacientes con criterio de dengue que presentaran cualquiera de las siguientes manifestaciones: extravasación severa del plasma, hemorragias severas según criterio clínico o daño grave de órganos.
Criterios de exclusión
Se excluyeron a los pacientes con imposibilidad de seguimiento, enfermedad del colágeno, neoplasias, cardiopatía congénita o patología crónica o que rehusaran la inclusión en el estudio.
Definición de casos por dengue
Miocarditis: es la inflamación del miocardio identificada mediante criterios clínicos y marcadores bioquímicos, electrocardiográficos y ecocardiográficos. Los criterios clínicos incluyen presencia de alteraciones del ritmo cardiaco, falla cardiaca no explicable o paciente con choque que no responde a una adecuada reanimación hídrica. Dentro de los estudios paraclínicos se encuentran los bioquímicos como el aumento de CPK (creatin fosfoquinasa) y su fracción MB, aumento en el nivel de troponinas I (inhibitoria) o T (transportadora), alteraciones electrocardiográficas como bradicardia o taquiarritmias, trastornos en la repolarización en onda T, segmento ST y ecocardiográficas que revelen disfunción miocárdica 8.
Sospecha de encefalitis: es la presencia de fiebre, cefalea y alteración del estado de conciencia no explicado por otras causas como falla hepática, choque, trastorno hidroelectrolitico, hemorragia intracraneana, presencia de IgM dengue-específica o NS1 en plasma; tampoco se presenta ningún otro patógeno en LCR y las neuroimágenes son sugestivas de encefalitis 9.
Hepatitis: es definida teniendo en cuenta la alteración de las aminotransferasas en suero y se consideraron cifras mayores a 10 veces el valor de referencia y por encima de 1000 U/ml, que corresponden a hepatitis grave según la OMS. Constituye falla hepática si se asocia a hipoglicemia, acidosis y alteración de la coagulación 10.
ELISA para diagnóstico de dengue y diferenciación entre infección primaria o secundaria
La infección por dengue se confirmó mediante la determinación plasmática de IgM específica contra el virus del dengue o la presencia de la proteína viral NS1, ambas detectadas por prueba ELISA 11 o identificación de genoma viral por RT-PCR 12. Para esto, se recolectaron muestras de sangre venosa total periférica en tubos con EDTA durante la fase aguda de la enfermedad, se obtuvo el plasma y se guardó a -70°C hasta su uso. No se realizó PCR en líquido cefaloraquídeo.
La IgM, la IgG -plasmáticos específicos de dengue- y la proteína NS1 se determinaron usando estuches comerciales Dengue IgM capture Elisa (Ref: E-DEN01M), Dengue IgG capture Elisa (Ref: E-DEN02G) y Dengue Early Elisa (Ref: E-DEN02P), respectivamente (todos de Panbio, Alere, Australia). Se determinó si la infección era primaria o secundaria mediante la positividad IgG o IgM, siendo primarios aquellos IgM positivos e IgG negativos y secundarios si las dos inmunoglobulinas son positivas; si solo la IgG es positiva, se considera positiva si el valor aumenta en dos tomas sucesivas o si la NS1 también es positiva.
Análisis estadístico
Se creó una base de datos que permitió tabular y registrar a diario los datos clínicos y paraclínicos encontrados en los pacientes del estudio durante su hospitalización.
Los datos se mostraron como medianas y rangos.
Se consideró que había diferencias estadísticas significativas con p<0.05 utilizando el paquete Graph Prism versión 5.0; también se usaron las pruebas no paramétricas de Mann Whitney y Kruskal Wallis. Si en Kruskal-Wallis p<0.05, se realizaron pruebas postest para establecer diferencias entre cada uno de los grupos.
Resultados
930 niños con dengue confirmado fueron incluidos en este estudio; de ellos, 825 fueron clasificados como DCSA y 105 como DG. El cuadro predominante en gravedad fue el choque con 83 casos (79%), seguido de organopatía con 19 (18.1%) y sangrado severo con 3 (2.9%). Los 19 casos de organopatía fueron 14 miocarditis, 4 hepatitis y 1 encefalitis. Todos los pacientes clasificados como DG fueron admitidos en la unidad de cuidados intensivos pediátrica. En la Tabla 1 se muestran 102 pacientes con DG y compromiso de órganos; 3 no se incluyeron, pues cursaban con sangrados severos.
PT: tiempo de protrombina; APTT: tiempo parcial de tromboplastina activado; AST: aspartato aminotransferasa; ALT: alanino aminotransferasa. * Mediana. † Valor p con prueba de Fisher. ‡ Valor p con prueba de Kruskal-Wallis. Fuente: Elaboración propia.Tabla 1: Hallazgos clínicos y de laboratorio en pacientes con dengue grave.
Los días de fiebre al ingreso fueron iguales en todos los pacientes y tuvieron una media de 5 días, no hubo diferencia de género en miocarditis, choque o hepatitis; sin embargo, la miocarditis tuvo tendencia a ser más frecuente en varones (9 de 14) y en niños con mayor edad que aquellos con hepatitis: 54 meses en quienes presentaron miocarditis versus 19 meses en quienes presentaron hepatitis (p=0.021, Mann-Whitney test). El vómito fue la mayor manifestación gastrointestinal en todos los grupos, no obstante se encontró hepatomegalia de forma general. Aunque no fue significativo, llamó la atención la presencia de menor derrame pleural en pacientes con diagnóstico de hepatitis (Tabla 1).
De los 19 pacientes, 3 tuvieron infección primaria, un caso asociado a hepatitis, otro a miocarditis y otro a encefalitis, el resto fueron infecciones secundarias. En cuanto a los otros pacientes con cuadro de DG, el 86% fue secundario, guardando una proporción similar a lo descrito con el grupo de afección de órganos.
Se analizaron 149 muestras en el laboratorio mediante RT-PCR; de estas, 63 fueron positivas, 12 correspondieron a serotipo dengue 1 (DEN 1), 34 a DEN 2, 15 a DEN 3 y 2 a DEN 4. De los niños con compromiso de órganos, 2 fueron DEN2 (miocarditis y hepatitis), 1 fue DEN3 (encefalitis) y 1 fue DEN1 (miocarditis).
En cuanto a los hallazgos de laboratorio, se observó recuento leucocitario similar entre choque y miocarditis; el recuento leucocitario en los pacientes con hepatitis fue superior y se evidenció una tendencia no significativa de trombocitopenia (media de 26 000) en niños con choque. Las transaminasas fueron más altas en los niños con hepatitis que en los otros dos grupos (p=0.002) (Tabla 1). No hay diferencias significativas en los otros datos analizados. Los valores de CPK en los niños con miocarditis se determinaron presentando una media de 183 U/L y la fracción MB fue de 15.5 U/L, valor que corresponde al 8.5% de la CPK total. La miocarditis fue el compromiso más frecuente en esta serie de niños con DG. La Figura 1 muestra 4 electrocardiogramas con hallazgos usuales de esta inflamación.
Figura 1: Electrocardiogramas de pacientes con miocarditis por dengue.
De 10 ecocardiogramas realizados, 5 evidenciaron disminución en la fracción de eyección, 3 de ellos leves, con valores entre 41% y 55%, y 2 severos, con valores >20%; además, se encontraron alteraciones en la función contráctil localizada en septum (tres casos), en ventrículo izquierdo (dos casos), en ventrículo derecho (dos casos) o, de forma generalizada, biventricular (cuatro casos).
Discusión
En el presente estudio, 825 niños fueron clasificados como DCSA y 105 como DG, lo que se explica por el hecho de que el Hospital Universitario Hernando Moncaleano Perdomo de Neiva es un centro de referencia regional. El choque por dengue fue la manifestación más frecuente de DG, debido a fuga plasmática progresiva, haciendo su detección un desafío para el clínico dado que un retraso en el tratamiento puede resultar en mal pronóstico 5. Además del choque, se incluyen otras consecuencias como hemoconcentración, hipoalbuminemia, edemas, efusión pleural y ascitis, cuya magnitud está relacionada con la severidad de la fuga plasmática y de los volúmenes de líquido fugado 13. Se presentó el caso de un niño que falleció con choque y falla multiorgánica.
Del total de pacientes (n=930), 11.3% cursó con DG. La frecuencia de compromiso de órganos encontrada fue de 18.1%, similar a la descrita en la serie de Salgado et al. 7, constituyéndose en la segunda causa de DG, después del choque. La miocarditis, con 14 casos, ocupó el primer lugar dentro de las causas de organopatía, resaltando la importancia de su diagnóstico en dengue 7,14,15.
La patogénesis de la miocarditis dengue no se encuentra establecida con plenitud, sin embargo se describe como una condición multifactorial en la que el virus juega un papel importante con su capacidad de invadir el miocardiocito, llevándolo a lisis o apoptosis; de igual forma, en la lesión endotelial con fuga plasmática y edema se plantea compromiso intracelular por alteración en la homeostasis del calcio; todo esto, sumado al rol de los mediadores inmunológicos (citoquinas) sobre la célula miocárdica, da como resultado un proceso complejo no solo en su génesis, sino también en el diagnóstico y curso evolutivo 16. Algunos autores atribuyen las alteraciones cardiacas solo a hipoperfusión coronaria secundaria al choque 17.
La miocarditis asociada al dengue se ha descrito desde los años 70 con alteraciones, en su mayoría, en la conducción cardiaca. Estas observaciones soportan la hipótesis de que la disfunción muscular es la responsable de las arritmias, como se ha reportado con casos de bradiarritmias o taquiarritmias que llevan a bajo gasto cardiaco, evidenciadas en los trazados electrocardiográficos y demostradas con ecocardiogramas con bajas fracciones de eyección y acortamiento, franca disminución de los índices cardiaco y de Tei e hipoquinesia septal; los cambios en el segmento ST y de la onda T incluyen hemoconcentración 17,18, como se observó en varios casos de esta serie.
La disfunción ventricular se describió en India con componente tanto sistólico como diastólico y como causa de choque refractario 19. Algunos factores como la concentración intracelular de calcio incrementada, la activación del sistema de caspasas y el aumento en la apoptosis de las células musculares contribuyen aún más con la disfunción contráctil miocárdica 20. En otras publicaciones se ha descrito esta afección con miocarditis fulminante aguda severa en pacientes admitidos con choque por dengue en las unidades de cuidado intensivo 21.
En Colombia, en una cohorte de pacientes infectados por dengue de un estudio hecho también en Neiva, la miocarditis se reportó en el 10.7% de los casos (11 de 102). Tal estudio mostró alteraciones electrocardiográficas en todos los casos, como ha sido consistentemente reportado en la literatura y en el presente estudio, lo que refuerza la utilidad del electrocardiograma en áreas de alta endemicidad como el primer examen de tamizaje cuando se ha sospechado la miocarditis dengue 22.
Las anormalidades electrocardiográficas más comunes incluyen taquicardia sinusal con cambios inespecíficos en la onda T o en el segmento ST. También se han observado arritmias ventriculares o supraventriculares y alteraciones en el sistema de conducción cardiaco, tales como bloqueo atrio-ventricular e intraventricular (bloqueos de rama izquierda o derecha). Con frecuencia se observa elevación en el segmento ST, depresión en el segmento ST, inversión en la onda T y pobre progresión de la onda R y ondas Q 23 (Figura 1).
Uno de los parámetros importantes para evaluación de la afección miocárdica es la medida de las enzimas cardiacas como CPK MB y troponinas T e I. Al grupo de pacientes con miocarditis fue al único al que se le determinó la CPK MB, considerando que son indicadores de daño miocárdico, por lo que no fue realizada su evaluación para todos los pacientes del estudio. Analizando el resultado de la CPK MB, se observa que tiene una relación del 5% al 10% de la CPK total, con una CPK en un rango de 90-135 U/ml, lo que muestra un leve incremento de acuerdo con la hipótesis de que el daño principal del virus del dengue es a nivel funcional más que a lisis de la célula miocárdica 16.
Es importante mencionar el uso de otras pruebas que contribuyen a hacer el diagnóstico de miocarditis, tales como el ecocardiograma, que mostró disfunción miocárdica en 10 pacientes con diferentes componentes (septal, anteroseptal, ventrículo izquierdo y biventricular) y confirmó la severidad del compromiso miocárdico como se reportó con anterioridad 22.
La miocarditis observada en el curso de una enfermedad febril aguda con diagnóstico de dengue confirma el compromiso de este órgano como parte de la afectación del virus del dengue 23.
De los niños incluidos en este estudio, 4 tuvieron hepatitis con recuperación clínica satisfactoria, siendo más frecuente en lactantes. Aunque no hay un claro consenso en el límite de las aminotransferasas, De Souza et al., en el año 2004, sugirieron en Brasil que cuando el valor de las enzimas hepáticas se aumenta 10 veces más respecto al valor de referencia para la edad, hay mayor correlación con hepatitis 10. La OMS, en la clasificación revisada, fijó el valor de las aminotransferasas en >1000 U/mL. En esta serie, el pico de elevación fue encontrado entre el día 5 y 6 de la enfermedad 24.
Trabajos con niños afectados por dengue con edades entre 1 y 15 años en Tailandia describe fatalidad por hepatitis aguda causada por ese virus 25,26. En Brasil se hizo el reporte de nueve casos de hepatitis fatal con choque y se demostró la presencia del virus del dengue en los hepatocitos y en las células de Kupffer, además de cambios histológicos como necrosis hepática masiva y hepatitis aguda paucicelular 27.
Aunque los cuatro serotipos se han asociado a hepatitis fulminante por dengue, los serotipos 1 y 3 parecen tener mayor tropismo hepático 28. En Colombia, todos los serotipos circulan de forma simultánea 1, hecho que incrementa el riesgo de sufrir hepatitis dengue, como se evidenció en este estudio con la detección de los cuatro serotipos. En Santander, Colombia, se presentaron 913 casos de niños con fiebre dengue hemorrágico durante un periodo de 12 años; de estos, 10 fallecieron y a 3 se les demostró infiltración grasa hepática 29. La hepatitis, en general, suele ser benigna, pero en algunos casos puede evolucionar a falla hepática y muerte como desenlace de la infección.
El virus del dengue y la proteína viral NS1 han sido detectados en el líquido cefalorraquídeo, lo que sugiere la posibilidad de que este también puede afectar el SNC 30. Uno de los niños incluidos en este estudio, cuya evolución clínica fue favorable, tuvo convulsión febril asociada a vómito en el segundo día de la enfermedad; también tuvo edema cerebral evidente en la escanografía cerebral. Los pacientes con DG muestran un gran rango de manifestaciones neurológicas, incluyendo encefalopatía y convulsiones, que pueden ocurrir como primera manifestación clínica hasta en el 50% de los afectados por DG y hasta en el 16% en dengue primario 31.
Existen reportes relacionados con síndrome de Guillain Barré, encefalomielitis diseminada aguda, mielitis y neuritis óptica 32, por lo que se recomienda hacer un análisis clínico permanente para determinar afección neurológica por virus del dengue, realizar una escanografía y tener presente que puede haber compromiso oftalmológico, el cual hasta hace algunos años era desconocido.
El presente estudio refuerza la importancia del compromiso de órganos en sus tres formas más comunes en niños con diagnóstico de DG. Sin embargo, tiene la limitación de ser retrospectivo, por lo cual es importante realizar investigaciones prospectivas que consideren compromiso de órganos como causa de DG y establezcan su incidencia y el impacto que pueda tener en su morbimortalidad.
Conclusión
Si bien el choque es la presentación más común del DG, como ha sido reportado en la literatura y se demostró en este estudio, se resalta la importancia de considerar el daño de órganos como consecuencia de la infección por este virus, dado que su detección oportuna contribuirá con el objetivo de disminuir su mortalidad.
Agradecimientos
Al Departamento de Pediatría del Hospital Universitario Hernando Moncaleano Perdomo de Neiva.
Referencias
Referencias
San Martin JL, Brathwaite O, Zambrano B, Solorzano JO, Bouckenooghe A, Dayan GH, et al. The epidemiology of dengue in the americas over the last three decades: a worrisome reality. Am J Trop Med Hyg. 2010;82(1):128-35.
Brathwaite Dick O, San Martin JL, Montoya RH, del Diego J, Zambrano B, Dayan GH. The history of dengue outbreaks in the Americas. Am J Trop Med Hyg. 2012;87(4):584-93. http://doi.org/bn75.
Martinez-Torres E. Dengue y dengue hemorrágico: aspectos clínicos. Salud Publica Mex. 1995;37 Suppl:S29-44.
Staples JE, Breiman RF, Powers AM. Chikungunya fever: an epidemiological review of a re-emerging infectious disease. Clin Infect Dis. 2009;49(6):942-8. http://doi.org/cmrrx4.
World Health Organization, Special Programme for Research and Training in Tropical Diseases. Dengue: guidelines for diagnosis, treatment, prevention and control: new edition. Geneva; WHO; 2009.
Ranjit S, Kissoon N. Dengue hemorrhagic fever and shock syndromes. Pediatr Crit Care Med. 2011;12(1):90-100. http://doi.org/dmxc22.
Salgado DM, Rodríguez JA, Garzón M, Cifuentes G, Ibarra M, Vega MR, et al. Caracterización Clínica y Epidemiológica de Dengue Hemorrágico en Neiva, Colombia, 2004. Rev Salud Publica. 2007;9(1):53-63.
Kindermann I, Barth C, Mahfoud F, Ukena C, Lenski M, Yilmaz A, et al. Update on myocarditis. J Am Coll Cardiol. 2012;59(9):779-92. http://doi.org/f2nckj.
Carod-Artal FJ, Wichmann O, Farrar J, Gascon J. Neurological complications of dengue virus infection. Lancet Neurol. 2013;12(9):906-19. http://doi.org/f2nbg8
Souza LJ, Alves JG, Nogueira RM, Gicovate Neto C, Bastos DA, Siqueira EW, et al. Aminotransferase changes and acute hepatitis in patients with dengue fever: analysis of 1,585 cases. Braz J Infect Dis. 2004;8(2):156-63. http://doi.org/fwhs6n.
Sang CT, Cuzzubbo AJ, Devine PL. Evaluation of a commercial capture enzyme-linked immunosorbent assay for detection of immunoglobulin M and G antibodies produced during dengue infection. Clin Diagn Lab Immunol. 1998;5(1):7-10.
Lanciotti RS, Calisher CH, Gubler DJ, Chang GJ, Vorndam AV. Rapid detection and typing of dengue viruses from clinical samples by using reverse transcriptase-polymerase chain reaction. J Clin Microbiol. 1992;30(3):545-51.
Basuki PS, Budiyanto, Puspitasari D, Husada D, Darmowandowo W, Ismoedijanto, et al. Application of revised dengue classification criteria as a severity marker of dengue viral infection in Indonesia. Southeast Asian J Trop Med Public Health. 2010;41(5):1088-94.
Khongphatthanayothin A, Suesaowalak M, Muangmingsook S, Bhattarakosol P, Pancharoen C. Hemodynamic profiles of patients with dengue hemorrhagic fever during toxic stage: an echocardiographic study. Intensive Care Med. 2003;29(4):570-4. http://doi.org/fdg85r.
Nimmagadda SS, Mahabala C, Boloor A, Raghuram PM, Nayak UA. Atypical Manifestations of Dengue Fever (DF) - Where Do We Stand Today? J Clin Diagn Res. 2014;8(1):71-3. http://doi.org/b932.
Salgado DM, Eltit JM, Mansfield K, Panqueba C, Castro D, Vega MR, et al. Heart and skeletal muscle are targets of dengue virus infection. Pediatr Infect Dis J. 2010;29(3):238-42. http://doi.org/bs2t9g.
Wali JP, Biswas A, Chandra S, Malhotra A, Aggarwal P, Handa R, et al. Cardiac involvement in Dengue Haemorrhagic Fever. Int J Cardiol. 1998;64(1):31-6. http://doi.org/d76x6z.
Kabra SK, Juneja R, Madhulika, Jain Y, Singhal T, Dar L, et al. Myocardial dysfunction in children with dengue haemorrhagic fever. Natl Med J India. 1998;11(2):59-61.
Khongphatthanayothin A, Lertsapcharoen P, Supachokchaiwattana P, La-Orkhun V, Khumtonvong A, Boonlarptaveechoke C, et al. Myocardial depression in dengue hemorrhagic fever: prevalence and clinical description. Pediatr Crit Care Med. 2007;8(6):524-9. http://doi.org/cb7b7s.
Lee IK, Lee WH, Liu JW, Yang KD. Acute myocarditis in dengue hemorrhagic fever: a case report and review of cardiac complications in dengue-affected patients. Int J Infect Dis. 2010;14(10):e919-22. http://doi.org/fg63j6.
Shann F. Severe dengue: coming soon to a pediatric intensive care unit near you? Pediatr Crit Care Med. 2005;6(4):490-2.
Salgado DM, Panqueba CA, Castro D, Vega MR, Rodríguez JA. Miocarditis en Niños con Fiebre por Dengue Hemorrágico en un Hospital Universitario de Colombia. Rev Salud Publica. 2009;11(4):591-600. http://doi.org/dzgfh2.
Punja M, Mark DG, McCoy JV, Javan R, Pines JM, Brady W. Electrocardiographic manifestations of cardiac infectious-inflammatory disorders. Am J Emerg Med. 2010;28(3):364-77. http://doi.org/bkn5kb.
de Souza LJ, Gonçalves Carneiro H, Souto Filho JT, Ferreira de Souza T, Azevedo-Cortes V, Neto CG, et al. Hepatitis in dengue shock syndrome. Braz J Infect Dis. 2002;6(6):322-7.
Huerre MR, Lan NT, Marianneau P, Hue NB, Khun H, Hung NT, et al. Liver histopathology and biological correlates in five cases of fatal dengue fever in Vietnamese children. Virchows Arch. 2001;438(2):107-15.
Bhamarapravati N, Tuchinda P, Boonyapaknavik V. Pathology of Thailand haemorrhagic fever: a study of 100 autopsy cases. Ann Trop Med Parasitol. 1967;61(4):500-10. http://doi.org/b737.
de Macedo FC, Nicol AF, Cooper LD, Yearsley M, Pires AR, Nuovo GJ. Histologic, viral, and molecular correlates of dengue fever infection of the liver using highly sensitive immunohistochemistry. Diagn Mol Pathol. 2006;15(4):223-8. http://doi.org/dhb2c3.
Thein S, Aung MM, Shwe TN, Aye M, Zaw A, Aye K, et al. Risk factors in dengue shock syndrome. Am J Trop Med Hyg. 1997;56(5):566-72.
Méndez A, González G. Manifestaciones clínicas inusuales del dengue hemorrágico en niños. Biomedica. 2006;26(1):61-70.
Solomon T, Dung NM, Vaughn DW, Kneen R, Thao LT, Raengsakulrach B, et al. Neurological manifestations of dengue infection. Lancet. 2000;355(9209):1053-9. http://doi.org/bwcwdg.
Misra UK, Kalita J, Syam UK, Dhole TN. Neurological manifestations of dengue virus infection. J Neurol Sci. 2006;244(1-2):117-22. http://doi.org/cc3fsc.
Murthy JM. Neurological complication of dengue infection. Neurol India. 2010;58(4):581-4. http://doi.org/djsfgx.
Cómo citar
APA
ACM
ACS
ABNT
Chicago
Harvard
IEEE
MLA
Turabian
Vancouver
Descargar cita
CrossRef Cited-by
1. Manuel Vides-Rosales, Diego Vides-Tesorero, Jaime Twanow. (2025). Neurological disorders related to pediatric dengue infection. Seminars in Pediatric Neurology, 54, p.101210. https://doi.org/10.1016/j.spen.2025.101210.
2. Teresa Isabel Veliz-Castro, Nereida Josefina Valero-Cedeño, Alexandra Pionce-Parrales, Mariana Torres-Portillo. (2022). Aminotransferasas y perfil lipídico en pacientes ecuatorianos con infección activa por virus dengue. Kasmera, 50 https://doi.org/10.56903/kasmera.5036015.
3. Jaime E. Castellanos, Paula Esteban, Juanita Panqueba-Salgado, Daniela Benavides-del-Castillo, Valentina Pastrana, Gladys Acosta, Doris Salgado, Carlos F. Narvaez, Sigrid Camacho-Ortega, Eliana Calvo, Myriam L. Velandia-Romero, Thomas R. Chauncey. (2021). A Case Series of Severe Dengue with Neurological Presentation in Children from a Colombian Hyperendemic Area. Case Reports in Medicine, 2021, p.1. https://doi.org/10.1155/2021/6643738.
4. Norton Pérez-Gutiérrez, Paula Andrea Amador-León. (2021). Dengue: actualidades y estándares en el manejo clínico. Revisión de tema. Acta Colombiana de Cuidado Intensivo, 21(1), p.66. https://doi.org/10.1016/j.acci.2020.04.007.
Dimensions
PlumX
Visitas a la página del resumen del artículo
Descargas
Licencia
Derechos de autor 2017 Revista de la Facultad de Medicina

Esta obra está bajo una licencia Creative Commons Reconocimiento 3.0 Unported.
-






















