Antimicrobial resistance trends in methicillin-resistant and methicillin-susceptible Staphylococcus aureus and Staphylococcus epidermidisisolates obtained from patients admitted to intensive care units. 2010-2015
Tendencias de resistencia antimicrobiana en Staphylococcus aureus y Staphylococcus epidermidis resistentes y susceptibles a meticilina aislados, obtenidos en unidades de cuidados intensivos, 2010-2015
DOI:
https://doi.org/10.15446/revfacmed.v67n3.65741Palabras clave:
Staphylococcus aureus, Staphylococcus epidermidis, Infecciones estafilocócicas, Resistencia a la meticilina, Staphylococcus aureus resistente a meticilina, Farmacorresistencia microbiana, Unidades de cuidados intensivos (en)Staphylococcus aureus, Staphylococcus epidermidis, Staphylococcal Infections, Methicillin Resistance, Methicillin-Resistant Staphylococcus aureus, Intensive Care Units (es)
Descargas
Introducción. La aparición y la diseminación de cepas resistentes en hospitales, principalmente en unidades de cuidado intensivo (UCI), se han convertido en un serio problema de salud pública.
Objetivo. Analizar la tendencia de los fenotipos de resistencia de Staphylococcus aureus y Staphylococcus epidermidis resistentes y susceptibles a meticilina aislados en pacientes atendidos en UCI de un hospital de alta complejidad de Cartagena, Colombia, del 2010 al 2015.
Materiales y métodos. Estudio analítico transversal realizado entre enero de 2010 y diciembre de 2015. Se utilizaron aislamientos de S. aureus y S. epidermidis meticilino-susceptibles y meticilino-resistentes (SARM, SASR, SERM y SESM). La técnica de susceptibilidad empleada fue el método microdilución en caldo para la detección de la concentración mínima inhibitoria.
Resultados. Se identificaron 313 aislamientos de Staphylococcus spp., la mayoría resistentes a meticilina (63.6%). Las cepas SARM y SERM correspondieron al 13.7% y al 27.8% del total de aislamientos, respectivamente. Los mayores porcentajes de resistencia en SARM y SERM correspondieron a eritromicina (57.6% y 81.2%, respectivamente), clindamicina (54.6% y 71.0%), ciprofloxacina (48.4% y 36.4%) y trimetoprima-sulfametoxazol (36.4% y 51.4%).
Conclusión. Los resultados encontrados sugieren el replanteamiento de las estrategias de control de la resistencia antimicrobiana en el hospital objeto de estudio.
Introduction: The emergence and spread of antimicrobial-resistant strains in hospitals, mainly in intensive care units (ICU), has become a serious public health problem.
Objective: To analyze the temporal trends of bacterial resistance phenotypes of methicillin-resistant and methicillin-susceptible Staphylococcus aureus and Staphylococcus epidermidis isolates obtained from ICU patients of a tertiary hospital in Cartagena, Colombia, between 2010 and 2015.
Methods: A cross-sectional study was carried out between January 2010 and December 2015. Methicillin-resistant and Methicillin-susceptible S. aureus and S. epidermidis isolates (MRSA, MSSA, MRSE and MSSE) were used. Culture medium microdilution technique was used to detect minimal inhibitory concentration (MIC).
Results: 313 Staphylococcus spp. isolates were identified, and most of there were methicillin-resistant (63.6%). Methicillin-resistant S. aureus (MRSA) and methicillin-resistant S. epidermidis (MRSE) strains represented 13.7% and 27.8%, respectively, of the total sample. The highest antibiotic resistance values in MRSA and MRSE isolates were observed for the following antibiotics: erythromycin (57.6% and 81.2%, respectively), clindamycin (54.6% and 71.0%), ciprofloxacin (48.4% and 36.4%) and trimethoprim-sulfametoxazole (36.4% and 51.4%).
Conclusions: The results reported here suggest the need to rethink the control strategies designed to minimize antibiotic resistance in the hospital in which this study was conducted.
original research
DOI: https://doi.org/10.15446/revfacmed.v67n3.65741
Antimicrobial resistance trends in methicillin-resistant and methicillin-susceptible Staphylococcus aureus and Staphylococcus epidermidis isolates obtained from patients admitted to intensive care units. 2010-2015
Tendencias de resistencia antimicrobiana en Staphylococcus aureus y Staphylococcus epidermidis resistentes y susceptibles a meticilina aislados, obtenidos en unidades de cuidados intensivos, 2010-2015
Received: 18/06/2017. Accepted: 28/11/2017.
Raimundo Castro-Orozco1,2 • Claudia Consuegra-Mayor1 • Gloria Mejía-Chávez1 • Jacqueline Hernández-Escolar1 • Nelson Alvis-Guzmán2,3
1 Universidad de San Buenaventura - Cartagena Campus - Faculty of Health Sciences - Cartagena de Indias D.T. - Colombia.
2 Universidad de Cartagena - Faculty of Economics - Cartagena de Indias D.T. - Colombia.
3 Universidad de la Costa (CUC) - Economics Department - Barranquilla - Colombia.
Corresponding author: Raimundo Castro-Orozco. Facultad de Ciencias de la Salud, Sede Cartagena, Universidad de San Buenaventura. Calle Real de Ternera No. 30-966, bloque A, piso 3. Phone number: +57 5 6539595, ext.: 135. Cartagena de Indias D.T. Colombia. Email: rorozco@usbctg.edu.co.
| Absctract |
Introduction: The emergence and spread of antimicrobial-resistant strains in hospitals, mainly in intensive care units (ICU), has become a serious public health problem.
Objective: To analyze the temporal trends of bacterial resistance phenotypes of methicillin-resistant and methicillin-susceptible Staphylococcus aureus and Staphylococcus epidermidis isolates obtained from ICU patients of a tertiary hospital in Cartagena, Colombia, between 2010 and 2015.
Methods: A cross-sectional study was carried out between January 2010 and December 2015. Methicillin-resistant and Methicillin-susceptible S. aureus and S. epidermidis isolates (MRSA, MSSA, MRSE and MSSE) were used. Culture medium microdilution technique was used to detect minimal inhibitory concentration (MIC).
Results: 313 Staphylococcus spp. isolates were identified, and most of them were methicillin-resistant (63.6%). Methicillin-resistant S. aureus (MRSA) and methicillin-resistant S. epidermidis (MRSE) strains represented 13.7% and 27.8%, respectively, of the total sample. The highest antibiotic resistance values in MRSA and MRSE isolates were observed for the following antibiotics: erythromycin (57.6% and 81.2%, respectively), clindamycin (54.6% and 71.0%), ciprofloxacin (48.4% and 36.4%) and trimethoprim-sulfametoxazole (36.4% and 51.4%).
Conclusions: The results reported here suggest the need to rethink the control strategies designed to minimize antibiotic resistance in the hospital in which the study was conducted.
Keywords: Staphylococcus Aureus; Staphylococcus Epidermidis; Staphylococcal Infections; Methicillin Resistance; Methicillin-Resistant Staphylococcus Aureus; Intensive Care Units (MeSH).
| Resumen |
Introducción. La aparición y la diseminación de cepas resistentes en hospitales, principalmente en unidades de cuidado intensivo (UCI), se han convertido en un serio problema de salud pública.
Objetivo. Analizar la tendencia de los fenotipos de resistencia de Staphylococcus aureus y Staphylococcus epidermidis resistentes y susceptibles a meticilina aislados en pacientes atendidos en UCI de un hospital de alta complejidad de Cartagena, Colombia, del 2010 al 2015.
Materiales y métodos. Estudio analítico transversal realizado entre enero de 2010 y diciembre de 2015. Se utilizaron aislamientos de S. aureus y S. epidermidis meticilino-susceptibles y meticilino-resistentes (SARM, SASR, SERM y SESM). La técnica de susceptibilidad empleada fue el método microdilución en caldo para la detección de la concentración mínima inhibitoria.
Resultados. Se identificaron 313 aislamientos de Staphylococcus spp., la mayoría resistentes a meticilina (63.6%). Las cepas SARM y SERM correspondieron al 13.7% y al 27.8% del total de aislamientos, respectivamente. Los mayores porcentajes de resistencia en SARM y SERM correspondieron a eritromicina (57.6% y 81.2%, respectivamente), clindamicina (54.6% y 71.0%), ciprofloxacina (48.4% y 36.4%) y trimetoprima-sulfametoxazol (36.4% y 51.4%).
Conclusión. Los resultados encontrados sugieren el replanteamiento de las estrategias de control de la resistencia antimicrobiana en el hospital objeto de estudio.
Palabras clave: Staphylococcus aureus; Staphylococcus epidermidis; Infecciones estafilocócicas; Resistencia a la meticilina; Staphylococcus aureus resistente a meticilina; Farmacorresistencia microbiana; Unidades de cuidados intensivos (DeCS).
Castro-Orozco R, Consuegra-Mayor C, Mejía-Chávez G, Hernández-Escolar J, Alvis-Guzmán N. Antimicrobial resistance trends in methicillin-resistant and methicillin-susceptible Staphylococcus aureus and Staphylococcus epidermidis isolates obtained from patients admitted to intensive care units. 2010-2015. Rev. Fac. Med. 2019;67(3):409-16. English. doi: https://doi.org/10.15446/revfacmed.v67n3.65741.
Castro-Orozco R, Consuegra-Mayor C, Mejía-Chávez G, Hernández-Escolar J, Alvis-Guzmán N. [Tendencias de resistencia antimicrobiana en Staphylococcus aureus y Staphylococcus epidermidis resistentes y susceptibles a meticilina aislados, obtenidos en unidades de cuidados intensivos, 2010-2015]. Rev. Fac. Med. 2019;67(3):409-16. English. doi:
https://doi.org/10.15446/revfacmed.v67n3.65741.
Introducción
The last 20 years have been characterized by the emergence and spread of antibiotic-resistant bacteria, which in turn have become a determining factor for the failure of antibiotic therapies, mainly in patients admitted to intensive care units (ICU). (1,2) This public health problem has serious implications on morbidity and mortality rates, and on public health systems stability, provided that both direct and indirect economic costs increase heavily due long-term hospitalizations and greater drug consumption. (3)
To date, different strategies have been developed to minimize the impact this public health problem can have on health systems, including appropriate antibiotics prescription, cleaning and disinfection programs, antimicrobial stewardship programs, and epidemiological surveillance of antimicrobial resistance. (2,4)
It has been estimated that in patients admitted to a hospital the risk of contracting a nosocomial infection is ~10%. In addition, said risk almost quadruples when the individual is admitted to the ICU, since antimicrobial therapy is a common practice in ICU patients. (5,6) Moreover, multidrug-resistant bacteria infection susceptibility may be higher in these critically ill patients (7-9), which limits treatment options and makes mandatory to determine antimicrobial resistance profiles among clinical isolates retrieved from said patients.
Given how antimicrobial resistance works, any modification to be made in antimicrobial management schemes should be based on both antimicrobial resistance surveillance data and bacterial etiology. (10)
Changes made to the antimicrobial management schemes are not generally applicable to other hospitals, for they are based on the intrinsic characteristics of each hospital and depend on several aspects such as the type of hospital (facilities), antibiotics availability, and specific local data obtained from monitoring antimicrobial resistance. (11)
Staphylococcus spp. are frequently cultured from hospitalized patients and are characterized by being resistant to multiple antimicrobials. Methicillin-resistant Staphylococcus aureus (MRSA) and methicillin-resistant Staphylococcus epidermidis (MRSE) can be used as markers to evaluate antimicrobial resistance time trends in critically ill patients. (12-19)
Espinosa et al. (20), in a systematic review on antimicrobial resistance in gram-positive cocci in Colombian hospitals, reported a higher isolation frequency of methicillin-resistant staphylococci in ICU isolates in comparison to non-ICU isolates. (20) This finding is consistent with those of Villalobos et al. (16) and Villalobos et al. (21), who reported MRSA antibiotic resistance phenotypes and profiles in tertiary hospitals in Colombia. In this context, the importance of an active in vitro antimicrobial resistance surveillance program should be noted.
Effective surveillance of antimicrobial resistant organisms allows generating reports that provide necessary information for analyzing and monitoring resistance patterns; likewise, these surveillance data can be used for making decisions regarding the treatment. (22)
The objective of the present study was to evaluate the temporal trends of MRSA and MRSE antibiotic resistance phenotypes from isolates obtained between 2010 and 2015 from ICU patients in a tertiary hospital located in Cartagena, Colombia.
Materials and methods
Study population
All S. aureus and S. epidermidis isolates were obtained from patients admitted between January 2010 and December 2015 to three different ICUs (11 adult ICU beds, 11 pediatric ICU beds, and 6 neonatal ICU beds) in a tertiary hospital in Cartagena, Colombia. Samples collection was performed before chemotherapy was carried out.
Study design
A cross-sectional study was carried out to evaluate antimicrobial resistance trends of methicillin-resistant and methicillin-susceptible S. aureus (MRSA and MSSA, respectively) and methicillin-resistant and methicillin-susceptible S. epidermidis (MRSE and MSSE, respectively) by using isolates obtained from ICU patients as resistant markers.
Bacterial identification
A MicroScan® Microbiology System (Siemens Healthcare Diagnostics) was used to perform an automated identification process of the staphylococcal species.
Antimicrobial susceptibility tests
A MicroScan® automated system (Dade Behring, Sacramento, USA) was used to determine antibiotic resistance/susceptibility by using the minimal inhibitory concentration (MIC) technique.
Antibiotics
Antibiotic susceptibility was determined for the following antibiotics: clindamycin (CLI, R≥4 µg/mL), ciprofloxacin (CIP, R≥4 µg/mL), daptomycin (DAP, S ≤1 µg/mL), erythromycin (ERI, R≥8 µg/mL), gentamicin (GEN, R≥16 µg/mL), linezolid (LZD, R≥8 µg/mL), moxifloxacin (MXF, R≥4 µg/mL), nitrofurantoin (NIT, R≥128 µg/mL), oxacillin (OXA, R≥4 µg/mL for S. aureus, R≥0.5 µg/mL for coagulase-negative staphylococci), penicillin (PEN, R≥0.25 µg/mL), rifampin (RIF, R≥4 µg/mL), trimethoprim-sulfamethoxazole (SXT, R≥ 4/76 µg/mL), and vancomycin (VAN, R≥16 µg/mL for S. aureus, R≥32 µg/mL for coagulase-negative staphylococci).
MIC interpretive standards for all antimicrobials tested were defined according to the standard breakpoints established by the Clinical and Laboratory Standards Institute (CLSI). (23) Isolates were classified as sensitive (S) or resistant (R); besides, strains with intermediate sensitivity (I) were included in the latter category.
Statistical Analysis
IBM SPSS Statistics for Windows, version 23.0, was used for statistical analysis. Annual absolute and relative resistance frequencies were analyzed. For dichotomous outcomes effect size in terms of odds ratio (24) and associated 95% confidence intervals, 95%CI were used. Fisher´s exact test was performed in order to compare antibiotic resistance percentages between S. aureus and S. epidermidis isolates, and Chi-square test for linear trends was used to analyze the 6-years resistance trend.
All tests of significance were calculated with a two-tailed alpha of 5%, and multiple antibiotic resistance (MAR) index was determined using the procedure described by Krumperman (25).
Ethical considerations
The study was approved by the Bioethics Committee of Universidad de San Buenaventura (Affidavit 005/August-19-2014), which classified it as a risk-free research according to the provisions of article 11 of Resolution 8430/1993, issued by the Colombian Ministry of Health (26), provided that the data used here were obtained from bacterial strains collected from patients admitted to ICUs. Likewise, the ethical principles for medical research involving human subjects outlined by the Declaration of Helsinki were followed. (27)
Results
A total of 313 staphylococcal strains were isolated and identified, of which 63.6% (199/313; 95%CI 58.1- 68.7) were methicillin-resistant staphylococcal isolates (Table 1: MRSA + MRSE + other MR-CoNS). Said isolates were obtained from patients admitted to the adult ICU (AICU) (57.1%; 93/163; 95%CI: 49.4- 64.4), the neonatal ICU (NICU) (78.8%; 67/85; 95%CI: 69.0-86.2), and the pediatric ICU (PICU) (60.0%; 39/65; 95%CI: 47.9-71.0) (Table 1).
Table 1. Distribution of methicillin-resistant and methicillin-susceptible Staphylococcus species isolates according by type of intensive care unit service. 2010-2015.
|
AICU |
PICU |
NICU |
||||
|
n (%) |
95%CI |
n (%) |
95%CI |
n (%) |
95%CI |
|
|
MSSA |
34 (20.9) |
15.3 to 27.7% |
14 (21.5) |
13.3 to 33.0% |
3 (3.5) |
1.2 to 9.9% |
|
MRSA |
27 (16.6) |
1.6 to 23.0% |
11 (16.9) |
9.7 to 27.8% |
5 (5.9) |
2.5 to 13.0% |
|
MSSE |
17 (10.4) |
6.6 to 16.1% |
7 (10.8) |
5.3 to 20.6% |
5 (5.9) |
2.5 to 13.0% |
|
MRSE |
28 (17.2) |
12.2 to 23.7% |
14 (21.5) |
13.3 to 33.0% |
45 (52.9) |
42.4 to 63.2% |
|
Other MS-CoNS |
19 (11.6) |
7.6 to 17.5% |
5 (7.7) |
3.3 to 16.8% |
10 (11.8) |
6.5 to 20.3% |
|
Other MR-CoNS |
38 (23.3) |
17.5 to 30.4% |
14 (21.5) |
13.3 to 33.0% |
17 (20.0) |
12.9 to 29.7% |
|
Total |
163 |
65 |
85 |
|||
AICU: adult intensive care unit; PICU: pediatric intensive care unit; NICU: neonatal intensive care unit; MSSA: methicillin-susceptible S. aureus; MRSA: methicillin-resistant S. aureus; MSSE: methicillin-susceptible S. epidermidis; MRSE: methicillin-resistant S. epidermidis; MS-CoNS: methicillin-susceptible coagulase-negative staphylococci; MR-CoNS: methicillin-resistant coagulase-negative staphylococci.
Source: Own elaboration.
According to the six years susceptibility test results , methicillin resistance rates of S. aureus and S. epidermidis for the whole period were 45.7% (43/94; 95%CI: 36.0-55.8) and 75.0% (87/116; 95%CI: 66.4-82.0), respectively.
Regarding species identification, by using the automated identification system it was found that 53.0% (116/219; 95%CI: 43.4-59.5) of the coagulase-negative Staphylococcus (CoNS) that were tested belonged to the S. epidermidis species, while 15.5% (34/219; 95%CI: 11.3-20.9), to S. hominis subsp hominis, and 11.4% (25/219; 95%CI: 7.9-16.3) to S. haemolyticus. The remaining 20.1% of isolates belonged to other coagulase-negative staphylococci (CoNS) species, including S. auricularis, S. hominis subsp novobiosepticum, S. warneri, S. lugdunensis, S. simulans, S. xylosus, S. intermedius, S. sciuri, S. capitis subsp capitis, and S. capitis subsp urealyticus.
Resistance to methicillin was detected in 71.2% (156/219; 95%CI: 64.9-76.8) of the CoNS isolates. In addition, 13.7% (43/313; 95%CI: 10.4-18.0) and 27.8% (87/313; 95%CI: 23.1-33.0) isolates were MRSA and MRSE, respectively (Table 1).
Sample-based MRSA, MSSA, MRSE, and MSSE isolates distribution is shown in Table 2. Most of these strains (52.9 to 96.6%) were isolated from blood cultures, while the remaining ones were obtained from orotracheal and ocular secretions (<30%), and other body fluids (<10%).
Table 2. Distribution of methicillin-resistant and methicillin-susceptible Staphylococcus species isolates based on the sample type they were retrieved from. 2010-2015.
|
MSSA |
MRSA |
MSSE |
MRSE |
|||||
|
n (%) |
95%CI |
n (%) |
95%CI |
n (%) |
95%CI |
n (%) |
95%CI |
|
|
Blood |
27 (52.9) |
39.5 to 66.0% |
24 (55.8) |
41.1 to 69.6% |
28 (96.6) |
82.8 to 99.4% |
74 (85.1) |
76.1 to 91.1% |
|
Secretions * |
15 (29.4) |
18.7 to 43.0% |
12 (27.9) |
16.8 to 42.7% |
0 (0) |
0.0 to 11.7% |
6 (6.9) |
3.2 to 14.2% |
|
Fluids † |
4 (7.8) |
3.1 to 18.5% |
4 (9.3) |
3.7 to 21.6% |
1 (1) |
0.6 to 17.2% |
1 (1.1) |
0.2 to 6.2% |
|
Bronquial lavage |
3 (5.9) |
2.0 to 15.9% |
1 (2.3) |
0.4 to 12.2% |
0 (0) |
0.0 to 11.7% |
1 (1.1) |
0.2 to 6.2% |
|
Urine |
2 (3.9) |
1.1 to 13.2% |
0 (0) |
0.0 to 8.2% |
0 (0) |
0.0 to 11.7% |
3 (3.5) |
1.2 to 9.7% |
|
Catheter tips |
0 (0) |
0.0 to 7.0% |
2 (4.7) |
1.3 to 15.5% |
0 (0) |
0.0 to 11.7% |
2 (2.3) |
0.6 to 8.0% |
|
Total |
51 |
43 |
29 |
87 |
||||
MSSA: methicillin-susceptible S. aureus; MRSA: methicillin-resistant S. aureus; MSSE: methicillin-susceptible S. epidermidis; MRSE: methicillin-resistant S. epidermidis.
* Secretions: orotracheal, ocular and other secretions.
† Fluids: pleural, peritoneal and other fluids.
Source: Own elaboration.
Antimicrobial resistance profiles are shown in Table 3. All staphylococcal isolates were identified as sensitive to daptomycin (DAP). Regarding MRSA and MRSE isolates, the highest resistance rates were found for erythromycin (ERI) (57.6% and 81.2%, respectively), clindamycin (CLI) (54.6% and 71.0%, respectively), ciprofloxacin (CIP) (48.4% and 36.4%, respectively) and trimethoprim-sulfamethoxazole (SXT) (36.4% and 51.4%, respectively).
In addition, resistance percentages to ERI, CLI, gentamicin (GEN), CIP, and SXT were far higher in in MRSA than in MSSA isolates. A similar behavior was only observed between MRSE and MSSE isolates (Table 4).
Table 3. Antimicrobial resistance profiles of the methicillin-resistant and methicillin-susceptible Staphylococcus species isolates. 2010-2015.
|
MSSA |
MRSA |
MSSE |
MRSE |
|||||
|
n (%) |
95%CI |
n (%) |
95%CI |
n (%) |
95%CI |
n (%) |
95%CI |
|
|
CLI |
8 (15.7) |
8.2 to 28.0% |
18 (54.6) |
38.9 to 67.5% |
3 (14.3) |
19.9 to 52.7% |
44 (71.0) |
51.6 to 71.6% |
|
CIP |
1 (3.1) |
1.1 to 13.2% |
15 (48.4) |
26.4 to 54.4% |
3 (16.7) |
9.9 to 38.4% |
20 (36.4) |
18.3 to 36.6% |
|
DAP |
0 (0) |
0.0 to 7.0% |
0 (0) |
0.0 to 8.2% |
0 (0) |
0.0 to 11.7% |
0 (0) |
0.0 to 4.2% |
|
ERI |
6 (15.8) |
12.5 to 34.6% |
19 (57.6) |
43.3 to 71.6% |
8 (38.1) |
31.4 to 65.6% |
56 (81.2) |
65.9 to 83.6% |
|
GEN |
1 (2.5) |
0.4 to 10.3% |
12 (36.4) |
18.6 to 45.1% |
4 (19.1) |
7.6 to 34.6% |
51 (70.8) |
58.6 to 77.7% |
|
LZD |
0 (0) |
0.0 to 7.0% |
4 (12.5) |
3.7 to 21.6% |
0 (0) |
0.0 to 11.7% |
0 (0) |
0.0 to 4.2% |
|
MXF |
0 (0) |
0.4 to 10.3% |
11 (33.3) |
14.9 to 40.2% |
1 (4.8) |
5.5 to 30.6% |
7 (11.5) |
5.5 to 18.5% |
|
NIT |
2 (12.5) |
1.1 to 13.2% |
3 (23.1) |
2.4 to 18.6% |
0 (0) |
0.0 to 11.7% |
0 (0) |
0.0 to 4.24% |
|
RIF |
1 (2.5) |
0.4 to 10.3% |
5 (15.2) |
5.1 to 24.5% |
1 (4.8) |
1.9 to 22.0% |
22 (30.6) |
18.3 to 36.6% |
|
SXT |
2 (5) |
1.1 to 13.2% |
12 (36.4) |
16.8 to 42.7% |
5 (25) |
7.6 to 34.6% |
37 (51.4) |
32.7 to 53.0% |
|
VAN |
0 (0) |
0.0 to 7.0% |
2 (6.1) |
1.3 to 15.5% |
1 (4.8) |
0.6 to 17.2% |
1 (1.4) |
0.2 to 6.2% |
MSSA: methicillin-susceptible S. aureus; MRSA: methicillin-resistant S. aureus; MSSE: methicillin-susceptible S. epidermidis; MRSE: methicillin-resistant S. epidermidis; CLI: clindamycin; CIP: ciprofloxacin; DAP: daptomycin; ERI: erythromycin; GEN: gentamicin; LZD: linezolid; MXF: moxifloxacin; NIT: nitrofurantoin; RIF: rifampin; SXT: trimethoprim-sulfamethoxazole; VAN: vancomycin.
Source: Own elaboration.
Table 4. Comparison of antibiotic resistance phenotypes of methicillin-resistant and methicillin-susceptible Staphylococcus species isolates. 2010-2015.
|
MRSA vs. MSSA |
Antibiotic resistance phenotypes |
p-value* |
Effect size (OR) |
95%CI |
|
CLI-R |
0.0001 |
6.2 |
2.4 to 15.9 |
|
|
CIP-R |
≤0.00001 |
16.0 |
3.4 to 74.7 |
|
|
ERI-R |
0.0003 |
5.1 |
2.1 to 12.3 |
|
|
GEN-R |
0.0001 |
21.7 |
2.7 to 174.1 |
|
|
SXT-R |
0.0011 |
9.5 |
2.0 to 45.3 |
|
|
MRSE vs. MSSE |
Antibiotic resistance phenotypes |
p-value* |
Effect size (OR) |
95%CI |
|
CLI-R |
0.0097 |
3.1 |
1.3 to 7.4 |
|
|
CIP-R |
0.536 |
1.4 |
0.5 to 3.7 |
|
|
ERI-R |
0.0054 |
3.4 |
1.4 to 8.0 |
|
|
GEN-R |
≤0.00001 |
10.7 |
3.8 to 29.9 |
|
|
SXT-R |
0.014 |
3.6 |
1.3 to 9.8 |
MSSA: methicillin-susceptible S. aureus; MRSA: methicillin-resistant S. aureus; MSSE: methicillin-susceptible S. epidermidis; MRSE: methicillin-resistant S. epidermidis; CLI-R: clindamycin-resistant; CIP-R: ciprofloxacin-resistant; ERI-R: erythromycin-resistant; GEN-R: gentamicin-resistant; SXT-R: trimethoprim-sulfamethoxazole-resistant.
* p-values were estimated by means of Fisher’s exact test.
Source: Own elaboration.
Concerning MSSA strains, all resistance percentage values were <20%; on the contrary, resistance percentages to ERI and SXT in MSSE isolates were comparable with the high percentage values observed in MRSA isolates (p=0.41; X2=0.68 and p=0.296; X2=1.1, respectively).
Vancomycin MIC values for 2 MRSA isolates (4.7%; 95%CI: 1.3-15.5) were 8 µg/mL, vancomycin-intermediate S. aureus (VISA), and 16 µg/mL, vancomycin-resistant S. aureus (VRSA), while in 2 MRSE isolates (2.3%; 95%CI: 0.6-8.0) vancomycin MIC values were ≥16 µg/mL.
Resistance phenotypes trends in MRSA and MRSE isolates were higher in the last year of the study (January-December 2015), with the exception of resistance to SXT, since SXT-resistant isolates were not identified during this period. On the other hand, for the whole six years of the study, the lowest resistance percentages in MRSA and MRSE isolates were found for SXT (27.9% and 42.5%, respectively) (Table 5).
Table 5. Trends of antimicrobial resistance phenotypes of methicillin-resistant and methicillin-susceptible Staphylococcus species isolates. 2010-2015.
|
2010 |
2011 |
2012 |
2013 |
2014 |
2015 |
|||||||
|
Resistance phenotypes |
MRSA |
MRSE |
MRSA |
MRSE |
MRSA |
MRSE |
MRSA |
MRSE |
MRSA |
MRSE |
MRSA |
MRSE |
|
n (%) |
n (%) |
n (%) |
n (%) |
n (%) |
n (%) |
n (%) |
n (%) |
n (%) |
n (%) |
n (%) |
n (%) |
|
|
CLI-R |
3 (100) |
6 (66.7) |
0 (0) |
7 (70) |
1 (16.7) |
7 (63.6) |
1 (11.1) |
13 (68.4) |
12 (92.3) |
11 (84.6) |
6 (60) |
10 (66.7) |
|
ERI-R |
3 (100) |
16 (100) |
0 (0) |
8 (80) |
3 (50) |
8 (72.7) |
1 (11.1) |
13 (68.4) |
12 (92.3) |
10 (76.9) |
6 (60) |
10 (66.7) |
|
CIP-R |
1 (100) |
6 (66.7) |
0 (0) |
7 (70) |
3 (50) |
7 (63.6) |
2 (22.2) |
13 (68.4) |
9 (69.2) |
11 (84.6) |
2 (20) |
3 (20) |
|
GEN-R |
3 (100) |
11 (68.8) |
0 (0) |
6 (54.5) |
3 (50) |
11 (84.6) |
0 (0) |
13 (68.4) |
6 (46.2) |
10 (76.9) |
1 (10) |
9 (60) |
|
SXT-R |
2 (66.7) |
11 (68.8) |
0 (0) |
6 (54.5) |
5 (83.3) |
9 (69.2) |
0 (0) |
11 (57.9) |
5 (38.5) |
0 (0) |
0 (0) |
0 (0) |
MSSA: methicillin-susceptible S. aureus; MRSA: methicillin-resistant S. aureus; MSSE: methicillin-susceptible S. epidermidis; MRSE: methicillin-resistant S. epidermidis; CLI-R: clindamycin-resistant; CIP-R: ciprofloxacin-resistant; ERI-R: erythromycin-resistant; GEN-R: gentamicin-resistant; SXT-R: trimethoprim-sulfamethoxazole-resistant. Note: Multiresistant strains were included individually for each antibiotic evaluated.
Source: Own elaboration.
Furthermore, in the case of methicillin-resistant isolates, a high frequency of multi-drug resistant strains was observed (MRSA: 26/43; 60.5%; 95%CI: 45.6-73.6; MRSE: 68/87; 78.2%; 95%CI: 68.4-85.6). In this regard, 28 multiresistant phenotypes (MR-ANT) were identified in 26 MRSA (12 MR-ANT) and 68 MRSE (16 MR-ANT) strains. The MR-Ant frequency order was as follows: CLI-CIP-ERI-GEN-SXT (MRSA: 19.2%; 5/26; 95%CI: 8.5-37.9; MRSE: 23.5%; 16/68; 95%CI: 15.0- 34.9), CLI-CIP-ERI (MRSA: 23.1%; 6/26; 95%CI: 11.0-42.1), CLI-ERI-GEN (MRSE: 14.7%; 10/68; 95%CI: 8.2-25.0), and CLI-ERI-GEN-SXT (MRSE: 11.8%; 8/68; 95%CI: 6.1-21.5).
Multiple antibiotic resistances were also observed: 9 isolates (MRSA: 2/43; 4.7%; 95%CI: 1.3-15.5; MRSE: 7/87; 8.1%; 95%CI: 4.0-15.7) were resistant to a combination of seven antibiotics; 22 (MRSA: 6/43; 14.0%; 95%CI: 6.6-27.3; MRSE: 16/87; 18.4%; 95%CI: 11.7- 27.8), to a six antibiotics combination, and 13 (MRSA: 1/43; 2.3%; 95%CI: 0.4-12.1; MRSE: 12/87; 13.8%; 95%CI: 8.1- 22.6), to a five antibiotics combination.
The highest MAR index values observed in the methicillin-resistant Staphylococcus species isolates ranged from 0.8 to 0.9, while in methicillin-susceptible strains these ranged from 0.2 and 0.4. In addition, in most methicillin-resistant isolates MAR index was higher than 0.2 (MRSE: 79.3%; 69/87; 95CI 69.7 to 86.5%; MRSA: 60.5%; 26/43; 95%CI: 45.6-73.6), in contrast with methicillin-susceptible isolates, where most of them had a MAR index value lower than 0.2 (MSSE: 24.1%; 7/29; 95%CI: 12.2-42.1; MSSA: 3.9%; 2/51; 95%CI: 1.1-13.2).
On the other hand, the analysis of the methicillin-resistance trend of S. aureus isolates allowed finding a significant increase (p=0.031; X2 lineal trend=4.673; 1 df; slope=1.72) during the six years study period, somehow this epidemiological characteristic was not observed in other bacterial strains for the same period (Chi-square for lineal trend, MSSA: p=0.732; MRSE: p=0.082; MSSE: p=0.323) (Figure 1).
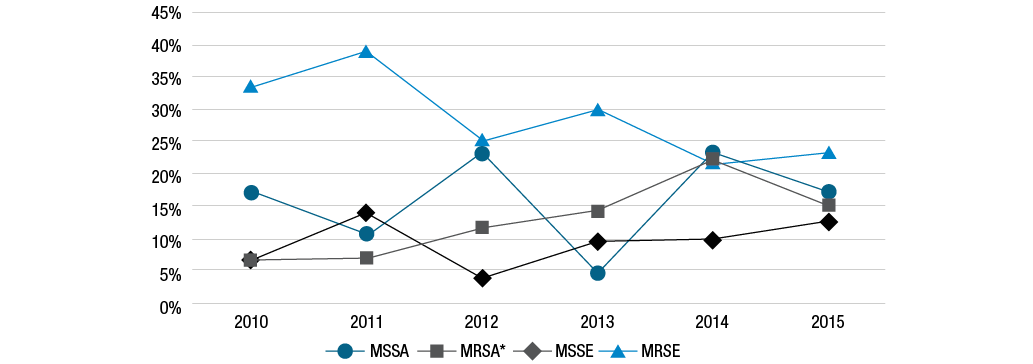
Figure 1. Frequency of methicillin-resistant and methicillin-susceptible Staphylococcus species isolates. 2010-2015.
MSSA: methicillin-susceptible S. aureus; MRSA: methicillin-resistant S. aureus; MSSE: methicillin-susceptible S. epidermidis; MRSE: methicillin-resistant S. epidermidis.
* p=0.031; X2 lineal trend=4.673; 1df; m=1.72.
Source: Own elaboration.
Discussion
Staphylococcus species have emerged as significant pathogens in both hospital-acquired and community-onset infections. (28-31) Hospital isolates of bacterial strains tend to have higher rates of resistance to antimicrobial agents, especially those collected from ICU patients. (20)
In this study, a higher frequency of methicillin-resistant staphylococci clinical isolates was reported in comparison with methicillin-susceptible isolates, which is consistent with the findings of national (16,32-38) and international studies. (12,39-44) In part, this could be explained by the relationship between antibiotic selective pressure and the emergence of antimicrobial-resistant organisms in hospitals. (45,46)
Most methicillin-resistant strains, mainly MRSE, were isolated from patients who were admitted to the NICU. This finding is consistent with several works reporting that S. epidermidis is one of the most common bacterial pathogens in this population. (32,39,41,43,47-51) Major risk factors for presenting these staphylococcal infections include prematurity, invasive procedures, prolonged hospitalization, and immune immaturity. (52,53)
On the other hand, the percentage values of MRSA and MRSE strains isolated from blood cultures are similar to those reported by Cortes et al. (34) in bacteremic patients admitted to the ICUs of 33 Colombian hospitals.
All these similarities suggest three possible scenarios at a national level: (i) failure of empirical antibacterial therapy (34,54), (ii) increased hospital stay lengths for clinically ill patients (55), and increased risk of mortality in ICU patients. (34,56)
Also, it was found that MRSE isolates showed a higher resistance frequency to antistaphylococcal antibiotics such as ERI, CLI and SXT that MRSA strains did. Somehow, in the case of ciprofloxacin, this pattern was not observed. Similar results were described by Álvarez et al. (57) In an attempt to explain these findings, the authors of the present study suggest two key factors: selective pressure caused by antibiotic use and cross-transmission of resistant bacteria.
Significant differences between antimicrobial resistance rates of methicillin-resistant and methicillin-susceptible Staphylococcus isolates have also been reported by other authors, although they have done so when comparing coagulase-negative Staphylococcus strains isolated from septicemic patients. (31)
About a third of the methicillin-resistant isolates were also resistant to other antibiotics including macrolides, lincosamides, quinolones, aminoglycosides, rifamycins, oxazolidinones, nitrofurans and antifolates. In addition, if a MAR index value >0.2 can be considered a multiple antimicrobial resistance characteristic (58), the presence of these multidrug-resistant strains could support the emergence of the three hypothetical scenarios described above.
Out of 43 MRSA isolates, 2 vancomycin-intermediate and vancomycin-resistant strains were identified in adult bacteremia cases. To date, there are no reports of VISA or VRSA isolates in Colombian hospitals. (21,33,35-37,49,57) However, one study conducted in Caldas, Colombia, in 1996 (38), reported the existence of VRSA strains isolated from patients admitted to the ICU, but these isolates were identified using the disc diffusion method. Despite the fact that VRSA isolates presence has not been confirmed by a reference laboratory, this finding could be interpreted as an early warning of the occurrence of clinically relevant pathogens for which only limited therapeutic options are available.
A final aspect that should be noted in this context is that in a recent study Rossi et al. (59) reported vancomycin resistance transmission between MRSA strains isolated from blood cultures.
Conclusion
The most effective antibiotics in MRSA and MRSE isolates were daptomycin, linezolid and vancomycin. The significant and rising trend in the number of MRSA isolates may be an indication of the need to redefine existing strategies to minimize antimicrobial resistance. It is necessary to periodically conduct surveillance studies in all hospitals in the country to achieve effective control strategies of multi-drug-resistant infections and to reduce antimicrobial resistance rates.
Conflicts of interest
None stated by the authors.
Funding
None stated by the authors.
Acknowledgements
None stated by the authors.
References
1.Morillo-Garcia A, Aldana-Espinal JM, Olry de Labry-Lima A, Valencia-Martín R, López-Márquez R, Loscertales-Abril M, et al. Hospital costs associated with nosocomial infections in a pediatric intensive care unit. Gac Sanit. 2015;29(4):282-7. http://doi.org/f3gxt9.
2.Lee CR, Cho IH, Jeong BC, Lee SH. Strategies to minimize antibiotic resistance. Int J Environ Res Public Health. 2013;10(9):4274-305. http://doi.org/gchm6p.
3.Friedman ND, Temkin E, Carmeli Y. The negative impact of antibiotic resistance. Clinic Microbiol Infect. 2016;22(5):416-422. http://doi.org/f8n8mp.
4.Morales FE, Villa LA, Fernández PB, López MA, Mella S, Muñoz M. Evolución del consumo de antimicrobianos de uso restringido y tendencia de la susceptibilidad in vitro en el Hospital Regional de Concepción, Chile. Rev Chilena Infectol. 2012;29(5):492-8. http://doi.org/c4c8.
5.Brusselaers N, Vogelaers D, Blot S. The rising problem of antimicrobial resistance in the intensive care unit. Ann Intensive Care. 2011;1:47. http://doi.org/dfvghv.
6.Briceño I, Suarez ME. Resistencia Bacteriana en la Unidad de Cuidados Intensivos del Hospital Universitario de Los Andes. MEDICRIT. 2006 [cited 2019 Apr 10];3(2):30-42. Available from: https://bit.ly/2KlBmdA.
7.López-Pueyo MJ, Barcenilla-Gaite F, Amaya-Villar R, Garnacho-Montero J. Multirresistencia antibiótica en unidades de críticos. Med Intensiva. 2011;35(1):41-53. http://doi.org/dx2x87.
8.De Waele JJ, Akova M, Antonelli M, Canton R, Carlet J, De Backer D, et al. Antimicrobial resistance and antibiotic stewardship programs in the ICU: insistence and persistence in the fight against resistance. A position statement from ESICM/ESCMID/WAAAR round table on multi-drug resistance. Intensive Care Med. 2018;44(2):189-96. http://doi.org/gc4xmn.
9.Bassetti M, Poulakou G, Timsit JF. Focus on antimicrobial use in the era of increasing antimicrobial resistance in ICU. Intensive Care Med. 2016;42(6):955-8. http://doi.org/c4c9.
10.Castro-Orozco R, Barreto-Maya AC, Guzmán-Álvarez H, Ortega-Quiroz RJ, Benítez-Peña L. [Antimicrobial resistance pattern for gram-negative uropathogens isolated from hospitalised patients and outpatients in Cartagena, 2005-2008]. Rev Salud Pública. 2010;12(6):1010-9.
11.Cook E, Marchaim D, Kaye KS. Building a successful infection prevention program: key components, processes, and economics. Infect Dis Clin North Am. 2011;25(1):1-19. http://doi.org/b3m92z.
12.De Santis V, Gresoiu M, Corona A, Wilson AP, Singer M. Bacteraemia incidence, causative organisms and resistance patterns, antibiotic strategies and outcomes in a single university hospital ICU: continuing improvement between 2000 and 2013. J Antimicrob Chemother. 2015;70(1):273-8. http://doi.org/f63zzp.
13.Tukenmez Tigen E, Dogru A, Koltka EN, Unlu C, Gura M. Device-associated nosocomial infection rates and distribution of antimicrobial resistance in a medical-surgical intensive care unit in Turkey. Jpn J Infect Dis. 2014;67(1):5-8.
14.Rodrigues-Moreira MR, Guimarães MP, de Araujo-Rodrigues AA, Gontijo-Filho PP. Antimicrobial use, incidence, etiology and resistance patterns in bacteria causing ventilator-associated pneumonia in a clinical-surgical intensive care unit. Rev Soc Bras Med Trop. 2013;46(1):39-44. http://doi.org/f4rfsw.
15.Bataar O, Khuderchuluun C, Lundeg G, Chimeddorj S, Brunauer A, Gradwohl-Matis I, et al. Rate and pattern of antibiotic resistance in microbiological cultures of sepsis patients in a low-middle-income country’s ICU. Middle East J Anaesthesiol. 2013 [CITED 2019 Apr 10];22(3):293-300. Available from: https://bit.ly/2YVighE.
16.Villalobos-Rodríguez AP, Díaz-Ortega MH, Barrero-Garzón LI, Rivera-Vargas SM, Henríquez-Iguarán DE, Villegas-Botero MV, et al. [Trends of bacterial resistance phenotypes in high-complexity public and private hospitals in Colombia]. Rev Panam Salud Pública. 2011;30(6):627-33.
17.Hoerlle JL, Brandelli A. Antimicrobial resistance of Staphylococcus aureus isolated from the intensive care unit of a general hospital in southern Brazil. J Infect Dev Ctries. 2009;3(7):504-10. http://doi.org/bqbqv7.
18.Zhanel GG, DeCorby M, Laing N, Weshnoweski B, Vashisht R, Tailor F, et al. Antimicrobial-resistant pathogens in intensive care units in Canada: results of the Canadian National Intensive Care Unit (CAN-ICU) study, 2005-2006. Antimicrob Agents Chemother. 2008;52(4):1430-7. http://doi.org/cp4jmv.
19.Leal AL, Eslava-Schmalbach J, Alvarez C, Buitrago G, Méndez M, Grupo para el Control de la Resistencia Bacteriana en Bogotá (GREBO). [Endemic tendencies and bacterial resistance markers in third-level hospitals in Bogotá, Colombia]. Rev Salud Pública. 2006;8 Suppl 1:59-70.
20.Espinosa CJ, Cortés JA, Castillo JS, Leal AL. [Systematic review of antimicrobial resistance among Gram positive cocci in hospitals in Colombia]. Biomédica. 2011;31(1):27-34.
21.Villalobos AP, Barrero LI, Rivera SM, Ovalle MV, Valera D. [Surveillance of healthcare associated infections, bacterial resistance and antibiotic consumption in high-complexity hospitals in Colombia, 2011]. Biomédica. 2014;34 Suppl 1:67-80.
22.Cantón R. [Interpretive reading of the antibiogram: a clinical necessity]. Enferm Infecc Microbiol Clin. 2010;28(6):375-85. http://doi.org/dbw48z.
23.Clinical and Laboratory Standards Institute (CLSI). M100-S25. Performance Standards for Antimicrobial Susceptibility Testing; Twenty-Fifth Informational Supplement. Wayne: Clinical and Laboratory Standards Institute; 2015.
24.Gaskin CJ, Happell B. Power, effects, confidence, and significance: an investigation of statistical practices in nursing research. Int J Nurs Stud. 2014;51(5):795-806. http://doi.org/c4dg.
25.Krumperman PH. Multiple antibiotic resistance indexing of Escherichia coli to identify high-risk sources of fecal contamination of foods. Appl Environ Microbiol. 1983;46(1):165-70.
26.Colombia. Ministerio de Salud. Resolución 8430 de 1993 (octubre 4): Por la cual se establecen las normas científicas, técnicas y administrativas para la investigación en salud. Bogotá D.C.; octubre 4 de 1993 [cited 2019 Apr 10]. Available from: https://bit.ly/2nH9STI.
27.Asociación Médica Mundial. Declaración de Helsinki de la Asociación Médica Mundial. Principios éticos para las investigaciones médicas en seres humanos. Fortaleza: 64.a Asamblea General de la AMM; 2013 [cited 2019 Apr 10]. Available from: https://bit.ly/2r2W2cs.
28.Argudín MA, Vanderhaeghen W, Vandendriessche S, Vandecandelaere I, André FX, Denis O, et al. Antimicrobial resistance and population structure of Staphylococcus epidermidis recovered from animals and humans. Vet Microbiol. 2015;178(1-2):105-13. http://doi.org/c4dh.
29.Rincón S, Panesso D, Díaz L, Carvajal LP, Reyes J, Munita JM, et al. Resistencia a antibióticos de última línea en cocos Gram positivos: la era posterior a la vancomicina. Biomédica. 2014;34 Suppl 1:191-208. http://doi.org/c4dj.
30.Cabrera CE, Gómez RF, Zuñiga AE, Corral RH, López B, Chávez M. Epidemiology of nosocomial bacteria resistant to antimicrobials. Colomb Med. 2011 [cited 2019 Apr 10];42(1):117-25. Available from: https://bit.ly/2VCScG3.
31.Koksal F, Yasar H, Samasti M. Antibiotic resistance patterns of coagulase-negative staphylococcus strains isolated from blood cultures of septicemic patients in Turkey. Microbiol Res. 2009;164(4):404-10. http://doi.org/c55qcr.
32.Hernández-Carrillo M, Revelo-Motta JP, Posada-España PA, Benavidez-Solarte PA, Ramírez-Serrato SV, Benítez-Soto CA, et al. Prevalencia de resistencia bacteriana a los antibióticos en una UCI neonatal de Nariño, Colombia. Rev Colomb Salud Libre. 2015;10(1):16-25.
33.Mateus JE, León FJ, González GM, Narváez E. Resistencia a los antibióticos en dos unidades de cuidados intensivos de Bucaramanga (Colombia). Salud Soc Uptc. 2014;1(1):12-8.
34.Cortes JA, Leal AL, Montañez AM, Buitrago G, Castillo JS, Guzman L, Grupo para el Control de la Resistencia Bacteriana en Bogotá (GREBO). Frequency of microorganisms isolated in patients with bacteremia in intensive care units in Colombia and their resistance profiles. Braz J Infect Dis. 2013;17(3):346-52. http://doi.org/f2j339.
35.Morales GI, Yaneth MC, Chávez KM. Caracterización de la resistencia in vitro a diferentes antimicrobianos en cepas de Staphylococcus spp. en una institución hospitalaria de la ciudad de Valledupar entre enero y julio de 2009. Rev Cienc Salud. 2012 [cited 2019 Apr 10];10(2):169-77. Available from: https://bit.ly/2UGDv7K.
36.Sosa-Ávila LM, Machuca-Pérez MA, Sosa-Ávila CA, González-Rugeles CI. Infecciones por Staphylococcus aureus meticilino resistente en niños en Bucaramanga Colombia. Salud UIS. 2010;42(3):248-55.
37.Arias CA, Reyes J, Zúniga M, Cortés L, Cruz C, Rico CL, et al., Colombian Antimicrobial Resistance Group (RESCOL). Multicentre surveillance of antimicrobial resistance in enterococci and staphylococci from Colombian hospitals, 2001-2002. J Antimicrob Chemother. 2003;51(1):59-68. http://doi.org/dnhjmr.
38.Jaramillo E. Resistencia bacteriana a los antibióticos en la Unidad de Cuidados Intensivos, Hospital de Caldas, 1992-1994. Colombia Med. 1996 [cited 2019 Apr 10];27(2):69-76. Available from: https://bit.ly/2GfeDfj.
39.Lona-Reyes JC, Verdugo-Robles MA, Pérez-Ramírez RO, Pérez-Molina JJ, Ascencio-Esparza EP, Benítez-Vázquez EA. Etiology and antimicrobial resistance patterns in early and late neonatal sepsis in a Neonatal Intensive Care Unit. Arch Argente Pediatr. 2015;113(4):317-23. http://doi.org/c4dk.
40.Custovic A, Smajlovic J, Hadzic S, Ahmetagic S, Tihic N, Hadzagic H. Epidemiological surveillance of bacterial nosocomial infections in the surgical intensive care unit. Mater Sociomed. 2014;26(1):7-11. http://doi.org/c4dm.
41.Urzedo JE, Levenhagen MM, Pedroso RS, Abdallah VO, Sabino SS, Brito DV. Nosocomial infections in a neonatal intensive care unit during 16 years: 1997-2012. Rev Soc Bras Med Trop. 2014;47(3):321-6. http://doi.org/f6cj9s.
42.Fajardo-Olivares M, Hidalgo-Orozco R, Rodríguez-Garrido S, Gaona-Álvarez C, Sánchez-Silos RM, Hernández-Rastrollo R, et al. [Activity of vancomycin, teicoplanin and linezolid in methicillin resistant coagulase-negative Staphylococci isolates from paediatric blood cultures]. Rev Esp Quimioter. 2012;25(1):25-30.
43.Brito DV, Brito CS, Resende DS, Moreira do OJ, Abdallah VO, Gontijo-Filho PP. Nosocomial infections in a Brazilian neonatal intensive care unit: a 4-year surveillance study. Rev Soc Bras Med Trop. 2010;43(6):633-7. http://doi.org/dtgx24.
44.Erdem I, Ozgultekin A, Sengoz-Inan A, Ozturk-Engin D, Senbayrak-Akcay S, Turan G, et al. Bloodstream infections in a medical-surgical intensive care unit: incidence, aetiology, antimicrobial resistance patterns of Gram-positive and Gram-negative bacteria. Clin Microbiol Infect. 2009;15(10):943-6. http://doi.org/cnfg7q.
45.Fraimow HS, Tsigrelis C. Antimicrobial resistance in the intensive care unit: mechanisms, epidemiology, and management of specific resistant pathogens. Crit Care Clin. 2011;27(1):163-205. http://doi.org/cpcw5d.
46.Kolár M, Urbánek K, Látal T. Antibiotic selective pressure and development of bacterial resistance. Int J Antimicrob Agents. 2001;17(5):357-63. http://doi.org/ckkvqz.
47.Dal-Bó K, da Silva RM, Sakae TM. Nosocomial infections in a neonatal intensive care unit in South Brazil. Rev Bras Ter Intensiva. 2012;24(4):381-5. http://doi.org/c4dq.
48.Coronell W, Rojas J, Escamilla-Gil MA, Manotas MC, Sánchez MA. Infección nosocomial en unidades de cuidados intensivos neonatales. CCAP. 2009;9(3):30-9.
49.Mendoza-Tascón LA, Arias-Guatibonza MD. Susceptibilidad antimicrobiana en una Unidad de Cuidados Intensivos Neonatales: experiencia de 43 meses. Rev Enfer Infec Pediatr. 2010 [cited 2019 Apr 10];23(93):13-24. Available from: https://bit.ly/2Ggw2Ej.
50.Shimabuku R, Velásquez P, Yábar J, Zerpa R, Arribasplata G, Fernández S, et al. Etiología y susceptibilidad antimicrobiana de las infecciones neonatales. An Fac Med. 2004 [cited 2019 Apr 10];65(1):19-24. Available from: https://bit.ly/2UamD4K.
51.Álvarez M, Velazco E, Nieves B, Alviarez E, Araque M, Salazar E, et al. Caracterización fenotípica de cepas de Staphylococcus coagulasa negativa aisladas de una unidad de alto riesgo neonatal. Kasmera. 2008;36(1):7-16.
52.Marchant EA, Boyce GK. MG, Sadarangani M, Lavoie PM. Neonatal sepsis due to coagulase-negative staphylococci. Clin Dev Immunol. 2013:1-10. http://doi.org/gb7dkm.
53.Saiman L. Risk factors for hospital-acquired infections in the neonatal intensive care unit. Semin Perinatol. 2002;26(5):315-21. http://doi.org/bzvk3x.
54.Allegranzi B, Luzzati R, Luzzani A, Girardini F, Antozzi L, Raiteri R, et al. Impact of antibiotic changes in empirical therapy on antimicrobial resistance in intensive care unit-acquired infections. J Hosp Infect. 2002;52(2):136-40. http://doi.org/b86ssw.
55.Castillo JS, Leal AL, Cortes JA, Alvarez CA, Sanchez R, Buitrago G, et al., Grupo para el Control de la Resistencia Bacteriana en Bogotá (GREBO). Mortality among critically ill patients with methicillin-resistant Staphylococcus aureus bacteremia: a multicenter cohort study in Colombia. Rev Panam Salud Pública. 2012;32(5):343-50. http://doi.org/f4m36z.
56.Cosgrove SE. The relationship between antimicrobial resistance and patient outcomes: mortality, length of hospital stay, and health care costs. Clin Infect Dis. 2006;42(Suppl 2):S82-9. http://doi.org/cm7xw3.
57.Álvarez C, Cortes J, Arango A, Correa C, Leal A, Grupo para el Control de la Resistencia Bacteriana en Bogotá (GREBO). [Anti-microbial resistance in intensive care units in Bogotá, Colombia, 2001-2003]. Rev Salud Pública. 2006;8(Suppl 1):86-101. http://doi.org/d975n4.
58.Vanegas M, Correa N, Morales A, Martínez A, Rúgeles L, Jiménez F. Resistencia a antibioticos de bacterias aisladas de biopelículas en una planta de alimentos. Rev MVZ Córdoba. 2009;14(2):1677-83.
59.Rossi F, Diaz L, Wollam A, Panesso D, Zhou Y, Rincon S, et al. Transferable vancomycin resistance in a community-associated MRSA lineage. N Engl J Med. 2014;370(16):1524-31. http://doi.org/c4dr.
Referencias
Morillo-Garcia A, Aldana-Espinal JM, Olry de Labry-Lima A, Valencia-Martín R, López-Márquez R, Loscertales-Abril M, et al. Hospital costs associated with nosocomial infections in a pediatric intensive care unit. Gac Sanit. 2015;29(4):282-7. http://doi.org/f3gxt9.
Lee CR, Cho IH, Jeong BC, Lee SH. Strategies to minimize antibiotic resistance. Int J Environ Res Public Health. 2013;10(9):4274-305. http://doi.org/gchm6p.
Friedman ND, Temkin E, Carmeli Y. The negative impact of antibiotic resistance. Clinic Microbiol Infect. 2016;22(5):416-422. http://doi.org/f8n8mp.
Morales FE, Villa LA, Fernández PB, López MA, Mella S, Muñoz M. Evolución del consumo de antimicrobianos de uso restringido y tendencia de la susceptibilidad in vitro en el Hospital Regional de Concepción, Chile. Rev Chilena Infectol. 2012;29(5):492-8. http://doi.org/c4c8.
Brusselaers N, Vogelaers D, Blot S. The rising problem of antimicrobial resistance in the intensive care unit. Ann Intensive Care. 2011;1:47. http://doi.org/dfvghv.
Briceño I, Suarez ME. Resistencia Bacteriana en la Unidad de Cuidados Intensivos del Hospital Universitario de Los Andes. MEDICRIT. 2006 [cited 2019 Apr 10];3(2):30-42. Available from: https://bit.ly/2KlBmdA.
López-Pueyo MJ, Barcenilla-Gaite F, Amaya-Villar R, Garnacho-Montero J. Multirresistencia antibiótica en unidades de críticos. Med Intensiva. 2011;35(1):41-53. http://doi.org/dx2x87.
De Waele JJ, Akova M, Antonelli M, Canton R, Carlet J, De Backer D, et al. Antimicrobial resistance and antibiotic stewardship programs in the ICU: insistence and persistence in the fight against resistance. A position statement from ESICM/ESCMID/WAAAR round table on multi-drug resistance. Intensive Care Med. 2018;44(2):189-96. http://doi.org/gc4xmn.
Bassetti M, Poulakou G, Timsit JF. Focus on antimicrobial use in the era of increasing antimicrobial resistance in ICU. Intensive Care Med. 2016;42(6):955-8. http://doi.org/c4c9.
Castro-Orozco R, Barreto-Maya AC, Guzmán-Álvarez H, Ortega-Quiroz RJ, Benítez-Peña L. [Antimicrobial resistance pattern for gram-negative uropathogens isolated from hospitalised patients and outpatients in Cartagena, 2005-2008]. Rev Salud Pública. 2010;12(6):1010-9.
Cook E, Marchaim D, Kaye KS. Building a successful infection prevention program: key components, processes, and economics. Infect Dis Clin North Am. 2011;25(1):1-19. http://doi.org/b3m92z.
De Santis V, Gresoiu M, Corona A, Wilson AP, Singer M. Bacteraemia incidence, causative organisms and resistance patterns, antibiotic strategies and outcomes in a single university hospital ICU: continuing improvement between 2000 and 2013. J Antimicrob Chemother. 2015;70(1):273-8. http://doi.org/f63zzp.
Tukenmez Tigen E, Dogru A, Koltka EN, Unlu C, Gura M. Device-associated nosocomial infection rates and distribution of antimicrobial resistance in a medical-surgical intensive care unit in Turkey. Jpn J Infect Dis. 2014;67(1):5-8.
Rodrigues-Moreira MR, Guimarães MP, de Araujo-Rodrigues AA, Gontijo-Filho PP. Antimicrobial use, incidence, etiology and resistance patterns in bacteria causing ventilator-associated pneumonia in a clinical-surgical intensive care unit. Rev Soc Bras Med Trop. 2013;46(1):39-44. http://doi.org/f4rfsw.
Bataar O, Khuderchuluun C, Lundeg G, Chimeddorj S, Brunauer A, Gradwohl-Matis I, et al. Rate and pattern of antibiotic resistance in microbiological cultures of sepsis patients in a low-middle-income country’s ICU. Middle East J Anaesthesiol. 2013 [CITED 2019 Apr 10];22(3):293-300. Available from: https://bit.ly/2YVighE.
Villalobos-Rodríguez AP, Díaz-Ortega MH, Barrero-Garzón LI, Rivera-Vargas SM, Henríquez-Iguarán DE, Villegas-Botero MV, et al. [Trends of bacterial resistance phenotypes in high-complexity public and private hospitals in Colombia]. Rev Panam Salud Pública. 2011;30(6):627-33.
Hoerlle JL, Brandelli A. Antimicrobial resistance of Staphylococcus aureus isolated from the intensive care unit of a general hospital in southern Brazil. J Infect Dev Ctries. 2009;3(7):504-10. http://doi.org/bqbqv7.
Zhanel GG, DeCorby M, Laing N, Weshnoweski B, Vashisht R, Tailor F, et al. Antimicrobial-resistant pathogens in intensive care units in Canada: results of the Canadian National Intensive Care Unit (CAN-ICU) study, 2005-2006. Antimicrob Agents Chemother. 2008;52(4):1430-7. http://doi.org/cp4jmv.
Leal AL, Eslava-Schmalbach J, Alvarez C, Buitrago G, Méndez M, Grupo para el Control de la Resistencia Bacteriana en Bogotá (GREBO). [Endemic tendencies and bacterial resistance markers in third-level hospitals in Bogotá, Colombia]. Rev Salud Pública. 2006;8 Suppl 1:59-70.
Espinosa CJ, Cortés JA, Castillo JS, Leal AL. [Systematic review of antimicrobial resistance among Gram positive cocci in hospitals in Colombia]. Biomédica. 2011;31(1):27-34.
Villalobos AP, Barrero LI, Rivera SM, Ovalle MV, Valera D. [Surveillance of healthcare associated infections, bacterial resistance and antibiotic consumption in high-complexity hospitals in Colombia, 2011]. Biomédica. 2014;34 Suppl 1:67-80.
Cantón R. [Interpretive reading of the antibiogram: a clinical necessity]. Enferm Infecc Microbiol Clin. 2010;28(6):375-85. http://doi.org/dbw48z.
Clinical and Laboratory Standards Institute (CLSI). M100-S25. Performance Standards for Antimicrobial Susceptibility Testing; Twenty-Fifth Informational Supplement. Wayne: Clinical and Laboratory Standards Institute; 2015.
Gaskin CJ, Happell B. Power, effects, confidence, and significance: an investigation of statistical practices in nursing research. Int J Nurs Stud. 2014;51(5):795-806. http://doi.org/c4dg.
Krumperman PH. Multiple antibiotic resistance indexing of Escherichia coli to identify high-risk sources of fecal contamination of foods. Appl Environ Microbiol. 1983;46(1):165-70.
Colombia. Ministerio de Salud. Resolución 8430 de 1993 (octubre 4): Por la cual se establecen las normas científicas, técnicas y administrativas para la investigación en salud. Bogotá D.C.; octubre 4 de 1993 [cited 2019 Apr 10]. Available from: https://bit.ly/2nH9STI.
Asociación Médica Mundial. Declaración de Helsinki de la Asociación Médica Mundial. Principios éticos para las investigaciones médicas en seres humanos. Fortaleza: 64.a Asamblea General de la AMM; 2013 [cited 2019 Apr 10]. Available from: https://bit.ly/2r2W2cs.
Argudín MA, Vanderhaeghen W, Vandendriessche S, Vandecandelaere I, André FX, Denis O, et al. Antimicrobial resistance and population structure of Staphylococcus epidermidis recovered from animals and humans. Vet Microbiol. 2015;178(1-2):105-13. http://doi.org/c4dh.
Rincón S, Panesso D, Díaz L, Carvajal LP, Reyes J, Munita JM, et al. Resistencia a antibióticos de última línea en cocos Gram positivos: la era posterior a la vancomicina. Biomédica. 2014;34 Suppl 1:191-208. http://doi.org/c4dj.
Cabrera CE, Gómez RF, Zuñiga AE, Corral RH, López B, Chávez M. Epidemiology of nosocomial bacteria resistant to antimicrobials. Colomb Med. 2011 [cited 2019 Apr 10];42(1):117-25. Available from: https://bit.ly/2VCScG3.
Koksal F, Yasar H, Samasti M. Antibiotic resistance patterns of coagulase-negative staphylococcus strains isolated from blood cultures of septicemic patients in Turkey. Microbiol Res. 2009;164(4):404-10. http://doi.org/c55qcr.
Hernández-Carrillo M, Revelo-Motta JP, Posada-España PA, Benavidez-Solarte PA, Ramírez-Serrato SV, Benítez-Soto CA, et al. Prevalencia de resistencia bacteriana a los antibióticos en una UCI neonatal de Nariño, Colombia. Rev Colomb Salud Libre. 2015;10(1):16-25.
Mateus JE, León FJ, González GM, Narváez E. Resistencia a los antibióticos en dos unidades de cuidados intensivos de Bucaramanga (Colombia). Salud Soc Uptc. 2014;1(1):12-8.
Cortes JA, Leal AL, Montañez AM, Buitrago G, Castillo JS, Guzman L, Grupo para el Control de la Resistencia Bacteriana en Bogotá (GREBO). Frequency of microorganisms isolated in patients with bacteremia in intensive care units in Colombia and their resistance profiles. Braz J Infect Dis. 2013;17(3):346-52. http://doi.org/f2j339.
Morales GI, Yaneth MC, Chávez KM. Caracterización de la resistencia in vitro a diferentes antimicrobianos en cepas de Staphylococcus spp. en una institución hospitalaria de la ciudad de Valledupar entre enero y julio de 2009. Rev Cienc Salud. 2012 [cited 2019 Apr 10];10(2):169-77. Available from: https://bit.ly/2UGDv7K.
Sosa-Ávila LM, Machuca-Pérez MA, Sosa-Ávila CA, González-Rugeles CI. Infecciones por Staphylococcus aureus meticilino resistente en niños en Bucaramanga Colombia. Salud UIS. 2010;42(3):248-55.
Arias CA, Reyes J, Zúniga M, Cortés L, Cruz C, Rico CL, et al., Colombian Antimicrobial Resistance Group (RESCOL). Multicentre surveillance of antimicrobial resistance in enterococci and staphylococci from Colombian hospitals, 2001-2002. J Antimicrob Chemother. 2003;51(1):59-68. http://doi.org/dnhjmr.
Jaramillo E. Resistencia bacteriana a los antibióticos en la Unidad de Cuidados Intensivos, Hospital de Caldas, 1992-1994. Colombia Med. 1996 [cited 2019 Apr 10];27(2):69-76. Available from: https://bit.ly/2GfeDfj.
Lona-Reyes JC, Verdugo-Robles MA, Pérez-Ramírez RO, Pérez-Molina JJ, Ascencio-Esparza EP, Benítez-Vázquez EA. Etiology and antimicrobial resistance patterns in early and late neonatal sepsis in a Neonatal Intensive Care Unit. Arch Argente Pediatr. 2015;113(4):317-23. http://doi.org/c4dk.
Custovic A, Smajlovic J, Hadzic S, Ahmetagic S, Tihic N, Hadzagic H. Epidemiological surveillance of bacterial nosocomial infections in the surgical intensive care unit. Mater Sociomed. 2014;26(1):7-11. http://doi.org/c4dm.
Urzedo JE, Levenhagen MM, Pedroso RS, Abdallah VO, Sabino SS, Brito DV. Nosocomial infections in a neonatal intensive care unit during 16 years: 1997-2012. Rev Soc Bras Med Trop. 2014;47(3):321-6. http://doi.org/f6cj9s.
Fajardo-Olivares M, Hidalgo-Orozco R, Rodríguez-Garrido S, Gaona-Álvarez C, Sánchez-Silos RM, Hernández-Rastrollo R, et al. [Activity of vancomycin, teicoplanin and linezolid in methicillin resistant coagulase-negative Staphylococci isolates from paediatric blood cultures]. Rev Esp Quimioter. 2012;25(1):25-30.
Brito DV, Brito CS, Resende DS, Moreira do OJ, Abdallah VO, Gontijo-Filho PP. Nosocomial infections in a Brazilian neonatal intensive care unit: a 4-year surveillance study. Rev Soc Bras Med Trop. 2010;43(6):633-7. http://doi.org/dtgx24.
Erdem I, Ozgultekin A, Sengoz-Inan A, Ozturk-Engin D, Senbayrak-Akcay S, Turan G, et al. Bloodstream infections in a medical-surgical intensive care unit: incidence, aetiology, antimicrobial resistance patterns of Gram-positive and Gram-negative bacteria. Clin Microbiol Infect. 2009;15(10):943-6. http://doi.org/cnfg7q.
Fraimow HS, Tsigrelis C. Antimicrobial resistance in the intensive care unit: mechanisms, epidemiology, and management of specific resistant pathogens. Crit Care Clin. 2011;27(1):163-205. http://doi.org/cpcw5d.
Kolár M, Urbánek K, Látal T. Antibiotic selective pressure and development of bacterial resistance. Int J Antimicrob Agents. 2001;17(5):357-63. http://doi.org/ckkvqz.
Dal-Bó K, da Silva RM, Sakae TM. Nosocomial infections in a neonatal intensive care unit in South Brazil. Rev Bras Ter Intensiva. 2012;24(4):381-5. http://doi.org/c4dq.
Coronell W, Rojas J, Escamilla-Gil MA, Manotas MC, Sánchez MA. Infección nosocomial en unidades de cuidados intensivos neonatales. CCAP. 2009;9(3):30-9.
Mendoza-Tascón LA, Arias-Guatibonza MD. Susceptibilidad antimicrobiana en una Unidad de Cuidados Intensivos Neonatales: experiencia de 43 meses. Rev Enfer Infec Pediatr. 2010 [cited 2019 Apr 10];23(93):13-24. Available from: https://bit.ly/2Ggw2Ej.
Shimabuku R, Velásquez P, Yábar J, Zerpa R, Arribasplata G, Fernández S, et al. Etiología y susceptibilidad antimicrobiana de las infecciones neonatales. An Fac Med. 2004 [cited 2019 Apr 10];65(1):19-24. Available from: https://bit.ly/2UamD4K.
Álvarez M, Velazco E, Nieves B, Alviarez E, Araque M, Salazar E, et al. Caracterización fenotípica de cepas de Staphylococcus coagulasa negativa aisladas de una unidad de alto riesgo neonatal. Kasmera. 2008;36(1):7-16.
Marchant EA, Boyce GK. MG, Sadarangani M, Lavoie PM. Neonatal sepsis due to coagulase-negative staphylococci. Clin Dev Immunol. 2013:1-10. http://doi.org/gb7dkm.
Saiman L. Risk factors for hospital-acquired infections in the neonatal intensive care unit. Semin Perinatol. 2002;26(5):315-21. http://doi.org/bzvk3x.
Allegranzi B, Luzzati R, Luzzani A, Girardini F, Antozzi L, Raiteri R, et al. Impact of antibiotic changes in empirical therapy on antimicrobial resistance in intensive care unit-acquired infections. J Hosp Infect. 2002;52(2):136-40. http://doi.org/b86ssw.
Castillo JS, Leal AL, Cortes JA, Alvarez CA, Sanchez R, Buitrago G, et al., Grupo para el Control de la Resistencia Bacteriana en Bogotá (GREBO). Mortality among critically ill patients with methicillin-resistant Staphylococcus aureus bacteremia: a multicenter cohort study in Colombia. Rev Panam Salud Pública. 2012;32(5):343-50. http://doi.org/f4m36z.
Cosgrove SE. The relationship between antimicrobial resistance and patient outcomes: mortality, length of hospital stay, and health care costs. Clin Infect Dis. 2006;42 Suppl 2:S82-9. http://doi.org/cm7xw3.
Álvarez C, Cortes J, Arango A, Correa C, Leal A, Grupo para el Control de la Resistencia Bacteriana en Bogotá (GREBO). [Anti-microbial resistance in intensive care units in Bogotá, Colombia, 2001-2003]. Rev Salud Pública. 2006;8 Suppl 1:86-101. http://doi.org/d975n4.
Vanegas M, Correa N, Morales A, Martínez A, Rúgeles L, Jiménez F. Resistencia a antibioticos de bacterias aisladas de biopelículas en una planta de alimentos. Rev MVZ Córdoba. 2009;14(2):1677-83.
Rossi F, Diaz L, Wollam A, Panesso D, Zhou Y, Rincon S, et al. Transferable vancomycin resistance in a community-associated MRSA lineage. N Engl J Med. 2014;370(16):1524-31. http://doi.org/c4dr.
Cómo citar
APA
ACM
ACS
ABNT
Chicago
Harvard
IEEE
MLA
Turabian
Vancouver
Descargar cita
CrossRef Cited-by
1. Ivan Gutierrez-Tobar, Cristobal Carvajal, Pablo Vasquez-Hoyos, Alejandro Díaz-Díaz, Juan Pablo Londono Ruiz, Joam Andrade, Jhon Camacho-Cruz, Andrea Restrepo-Gouzy, Monica Trujillo-Honeysberg, Juan Gonzalo Mesa-Monsalve, Ignacio Perez, Richard Von Moltke, Maria Beltran-Echeverry, Jessica F. Toro, Angela P. Niño, Germán Camacho-Moreno, Juan Pablo Calle-Giraldo, Nancy Yhomara Cabeza, Lina Marcela Sandoval-Calle, Paola Perez Camacho, Jaime Patiño Niño, Paula Araque-Muñoz, Yazmin Rodríguez-Peña, Claudia Beltran-Arroyave, Yamile Chaucanez-Bastidas, Juan Lopez, Diego Galvis-Trujillo, Sandra Beltrán-Higuera, Ana-Cristina Marino, Natalia González Leal, Miguel Ángel Luengas Monroy, Derly Carolina Hernandez-Moreno, Rosalba Vivas Trochez, Carlos Garces, Eduardo López-Medina. (2024). Epidemiological and microbiological characteristics of S. aureus pediatric infections in Colombia 2018–2021, a national multicenter study (Staphylored Colombia). Frontiers in Pediatrics, 12 https://doi.org/10.3389/fped.2024.1386310.
2. Bingqing Chen, Lingyun Yao, Rongjuan Cai, Wei Chen, Yue Wang. (2024). Antimicrobial Resistance Profiles and mupA Gene Characterization of Staphylococcus epidermidis Recovered from Facial Skin of Healthy Females in Shanghai, China. Clinical, Cosmetic and Investigational Dermatology, Volume 17, p.2813. https://doi.org/10.2147/CCID.S481517.
Dimensions
PlumX
Visitas a la página del resumen del artículo
Descargas
Licencia
Derechos de autor 2019 Revista de la Facultad de Medicina

Esta obra está bajo una licencia Creative Commons Reconocimiento 3.0 Unported.
-





















