Impacto de las condiciones sociodemográficas sobre el control prenatal en Latinoamérica
Impact of sociodemographic conditions on prenatal care in Latin America
DOI:
https://doi.org/10.15446/revfacmed.v67n3.69536Palabras clave:
Atención prenatal, Accesibilidad a los servicios de salud, Embarazo (es)Prenatal Care, Health Services Accessibility, Pregnancy (en)
Introducción. El control prenatal corresponde a una estrategia encaminada a prevenir las posibles complicaciones del embarazo, el parto y el puerperio. Diversos estudios aislados se han realizado para identificar factores que pueden afectar de forma negativa el control prenatal.
Objetivo. Realizar una síntesis cualitativa de la literatura respecto al impacto de las condiciones sociodemográficas sobre el control prenatal en Latinoamérica.
Materiales y métodos. Se realizó una búsqueda de la literatura a junio de 2018 en las bases de datos EBSCO, Embase, ScienceDirect, LILACS, SciELO, Cochrane Library, MEDLINE-PubMed y Google Scholar, con los términos “prenatal care” AND “Health services accessibility” AND “Pregnancy, Health services accessibility” AND “Pregnancy, prenatal care” AND “Health services accessibility” y sin límite de tiempo.
Resultados. Se encontraron 13 artículos con información relevante para el desarrollo de la presente revisión.
Conclusiones. La literatura disponible sugiere que condiciones sociodemográficas desfavorables podrían incidir de manera negativa sobre el control prenatal. El cuidado del hogar, la atención de otros hijos, la afiliación al sistema de seguridad social, la obligación laboral y el desempleo parecen ser los principales factores que afectan la calidad del mismo.
Introduction: Prenatal care is a strategy aimed at preventing the possible complications of pregnancy, childbirth and the postpartum period. Several isolated studies have been conducted to identify factors that may negatively affect prenatal care.
Objective: To make a qualitative synthesis of the literature regarding the impact of sociodemographic conditions on prenatal care in Latin America.
Materials and methods: A literature search was conducted in June 2018 on the EBSCO, Embase, ScienceDirect, LILACS, SciELO, Cochrane Library, MEDLINE-PubMed and Google Scholar databases, with the terms “prenatal care” AND “Health services accessibility” AND “Pregnancy, Health services accessibility” AND “Pregnancy, prenatal care” AND “Health services accessibility”, without a time frame.
Results: Thirteen articles were found with information relevant to the development of the present review.
Conclusions: The available literature suggests that unfavourable socio-demographic conditions may have a negative impact on prenatal care. Household care, care of other children, affiliation to the social security system, obligation to work and unemployment seem to be the main factors affecting the quality of the system.
artículo de revisión
DOI: https://doi.org/10.15446/revfacmed.v67n3.69536
Impacto de las condiciones sociodemográficas sobre el control prenatal en Latinoamérica
Impact of sociodemographic conditions on prenatal care in Latin America
Recibido: 20/12/2017. Aceptado: 30/04/2018.
Nasly Violedy Ipia-Ordóñez1 • Darío Fernando Ortega-Vallejo2 • Piedad Andrea Acosta-Mora3 • William Andrés López-Lasso4 Jhon Edward Martínez-Rodríguez4 • Norma Constanza Corrales-Zúñiga5 • Carlos Andrés Rosero-Montero1 • Anuar Alonso Cedeño-Burbano6
1 Clínica la Estancia - Unidad de Cuidados Intensivos - Popayán - Colombia.
2 Clínica DESA - Servicio de Consulta Externa - Santiago de Cali - Colombia.
3 Fundación Hospital San Pedro - Servicio de Urgencias - San Juan de Pasto - Colombia.
4 Hospital Universitario San José - Unidad de Cuidados Intensivos - Popayán - Colombia.
5 Clínica Comfandi - Servicio de Consulta Externa - Santiago de Cali - Colombia.
6 Universidad del Cauca - Facultad de Ciencias de la Salud - Programa de Especialización en Anestesiología - Popayán - Colombia.
Correspondencia: Anuar Alonso Cedeño-Burbano. Departamento de Anestesiología, Universidad del Cauca. Calle 6 No. 10N-143, Hospital Universitario San José de Popayán, piso 3. Teléfono: +57 234508. Popayán. Colombia. Correo electrónico: anuarcedeno@outlook.com.
| Resumen |
Introducción. El control prenatal corresponde a una estrategia encaminada a prevenir las posibles complicaciones del embarazo, el parto y el puerperio. Diversos estudios aislados se han realizado para identificar factores que pueden afectar de forma negativa el control prenatal.
Objetivo. Realizar una síntesis cualitativa de la literatura respecto al impacto de las condiciones sociodemográficas sobre el control prenatal en Latinoamérica.
Materiales y métodos. Se realizó una búsqueda de la literatura a junio de 2018 en las bases de datos EBSCO, Embase, ScienceDirect, LILACS, SciELO, Cochrane Library, MEDLINE-PubMed y Google Scholar, con los términos “prenatal care” AND “Health services accessibility” AND “Pregnancy, Health services accessibility” AND “Pregnancy, prenatal care” AND “Health services accessibility” y sin límite de tiempo.
Resultados. Se encontraron 13 artículos con información relevante para el desarrollo de la presente revisión.
Conclusiones. La literatura disponible sugiere que condiciones sociodemográficas desfavorables podrían incidir de manera negativa sobre el control prenatal. El cuidado del hogar, la atención de otros hijos, la afiliación al sistema de seguridad social, la obligación laboral y el desempleo parecen ser los principales factores que afectan la calidad del mismo.
Palabras clave: Atención prenatal; Accesibilidad a los servicios de salud; Embarazo (DeCS).
Ipia-Ordóñez NV, Ortega-Vallejo DF, Acosta-Mora PA, López-Lasso WA, Martínez-Rodríguez JE, Corrales-Zúñiga NC, et al. Impacto de las condiciones sociodemográficas sobre el control prenatal en Latinoamérica. Rev. Fac. Med. 2019;67(3):519-23. Spanish. doi: https://doi.org/10.15446/revfacmed.v67n3.69536.
| Abstract |
Introduction: Prenatal care is a strategy aimed at preventing the possible complications of pregnancy, childbirth and the postpartum period. Several isolated studies have been conducted to identify factors that may negatively affect prenatal care.
Objective: To make a qualitative synthesis of the literature regarding the impact of sociodemographic conditions on prenatal care in Latin America.
Materials and methods: A literature search was conducted in June 2018 on the EBSCO, Embase, ScienceDirect, LILACS, SciELO, Cochrane Library, MEDLINE-PubMed and Google Scholar databases using the following terms: “prenatal care” AND “Health services accessibility” AND “Pregnancy, Health services accessibility” AND “Pregnancy, prenatal care” AND “Health services accessibility”. No time limits were considered in the search.
Results: Thirteen articles with information relevant to the development of the present review were found.
Conclusions: The available literature suggests that unfavourable socio-demographic conditions may have a negative impact on prenatal care. Household care, care of other children, affiliation to the social security system, obligation to work and unemployment seem to be the main factors affecting the quality of prenatal care.
Keywords: Prenatal Care; Health Services Accessibility; Pregnancy (MeSH).
Ipia-Ordóñez NV, Ortega-Vallejo DF, Acosta-Mora PA, López-Lasso WA, Martínez-Rodríguez JE, Corrales-Zúñiga NC, et al. [Impact of sociodemographic conditions on prenatal care in Latin America]. Rev. Fac. Med. 2019;67(3):519-23. Spanish. doi: https://doi.org/10.15446/revfacmed.v67n3.69536.
Introducción
El control prenatal tiene como fin determinar las condiciones de salud materna y fetal, identificar factores de riesgo y educar a la gestante para el ejercicio de la maternidad y la crianza (1). Un adecuado control prenatal permite la aplicación de un gran número de medidas encaminadas a determinar y mantener la salud maternofetal en el embarazo (2). Aun así, cada año cerca de 530 000 mujeres mueren por causas maternas, 4 millones de niños nacen muertos y 4 millones mueren en el período neonatal, con tasas más altas de muerte materna y neonatal en poblaciones de extrema pobreza (3-5). La mayoría de las defunciones maternas se originan por complicaciones obstétricas, las cuales son evitables por medio de intervenciones médicas oportunas, es decir, son susceptibles de ser intervenidas durante el control prenatal (6).
El beneficio de la atención prenatal ha sido documentado en muchos estudios (7-13). Un adecuado control de este tipo tiene un impacto benéfico sobre la evolución del embarazo y la preparación de las mujeres para el periodo post natal (14). Muchos investigadores han observado que el uso y las condiciones del cuidado prenatal varían según los grupos de riesgo médico, socioeconómico, demográfico y cultural, sugiriendo que estas características podrían modificar los efectos de la atención prenatal (15-17).
La mayoría de los modelos de control prenatal no han sido evaluados de forma rigurosa (1,18,19). Sin embrago, estudios derivados de países de medianos y bajos ingresos han sugerido que pocas visitas prenatales son un factor de riesgo significativo para el aumento de la mortalidad perinatal y la permanencia más prolongada de los recién nacidos en las unidades de cuidados intensivos neonatales (20,21). Además, se han encontrado diferencias en el uso y la calidad de la atención en salud materna cuando se consideran factores específicos como edad de la madre, etnicidad, nivel educativo, religión, factores culturales, costos, ubicación y calidad de los servicios en salud (22-32).
El objetivo del presente artículo es realizar una síntesis cualitativa de la literatura para responder a la pregunta ¿Cómo impactan las condiciones sociodemográficas el programa de control prenatal en Latinoamérica?
Materiales y métodos
Se diseñó una estrategia de búsqueda de la literatura basada en los componentes de la pregunta PICO sin la utilización de control ni desenlace (outcome) para maximizar la sensibilidad de la misma. La búsqueda se hizo a junio de 2018, sin límite de tiempo, en las bases de datos EBSCO, Embase, ScienceDirect, LILACS, SciELO, Cochrane Library, MEDLINE-PubMed y Google Scholar y con los términos “prenatal care” AND “Health services accessibility” AND “Pregnancy, Health services accessibility” AND “Pregnancy, prenatal care” AND “Health services accessibility”.
La búsqueda se restringió a estudios en inglés, portugués y español y solo se seleccionaron investigaciones en humanos realizadas en países de Latinoamérica correspondientes a revisiones sistemáticas, ensayos clínicos, estudios de cohorte, casos controles, estudios descriptivos y estudios cualitativos. Comentarios, cartas al editor, reportes de caso y artículos editoriales fueron excluidos.
La estrategia de búsqueda y selección de los estudios incluidos en la presente revisión se muestra en la Figura 1.
Dos revisores independientes evaluaron los resultados de la búsqueda. En principio se evaluó el título y resumen y de ser necesario el texto completo de las publicaciones. Las discrepancias sobre la inclusión de los estudios fueron resueltas mediante la participación de un tercer investigador.
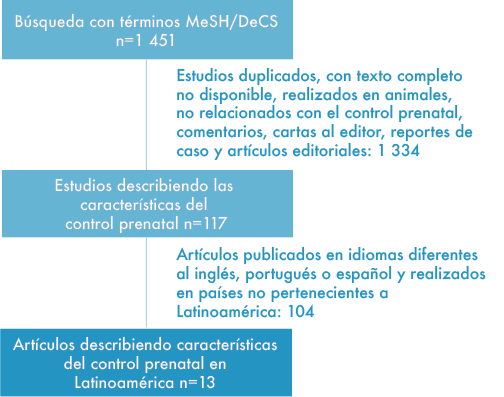
Figura 1. Flujograma de búsqueda y selección de los estudios.
Fuente: Elaboración propia.
Resultados
Se encontraron 13 estudios relevantes para el desarrollo de la presente revisión, incluyendo 2 estudios de casos y controles, 9 estudios descriptivos y 2 estudios cualitativos, los cuales se describen en la Tabla 1.
Tabla 1. Principales estudios que describen factores sociodemográficos asociados a la calidad del control prenatal en Latinoamérica.
|
Características del estudio |
Metodología |
Principales hallazgos |
|
|
Estudios realizados en Colombia |
Mendoza-Tascón et al. (33). Estudio de casos y controles. Colombia, 2014 |
Se incluyeron 570 casos (embarazadas menores de 20 años) y 2 093 controles (embarazadas mayores de 20 años) |
Se encontró asociación entre el embarazo adolescente y una mala adherencia al control prenatal (p<0.0001) después de ajustarse por escolaridad <11 años, ausencia de esposo o compañero permanente, no afiliación a seguridad social y gravidez ≥2 gestaciones. |
|
Miranda-Mellano (34). Estudio descriptivo. Colombia, 2014 |
Se incluyeron 730 gestantes que acudieron a la consulta de control prenatal en un centro hospitalario |
Se encontró asociación significativa entre un adecuado de control prenatal y la afiliación al sistema de salud (OR: 2.2, IC95%: 1.3-3.6). |
|
|
Moya-Plata et al. (35). Estudio descriptivo. Colombia, 2009 |
Participaron 160 gestantes que acudieron a realizarse control prenatal a un centro hospitalario |
Se identificó que 30% de las maternas tuvieron de 1 a 3 controles prenatales, 49% entre 4 y 6 y 21% 7 o más. |
|
|
Díaz-Martínez et al. (36). Estudio descriptivo. Colombia, 1999 |
Se analizaron 93 muertes perinatales ocurridas durante un año |
Se encontró que 17.9% de las muertes pudieron haberse evitado con un adecuado control prenatal y 15.4% si las madres hubieran acudido al mismo. |
|
|
Estudios realizados en Latinoamérica |
Huanco et al. (37). Estudio de casos y controles. Perú, 2008 |
Se incluyeron 17 965 casos (embarazadas entre 10 y 19 años) y 49 014 controles (embarazadas entre 20 y 29 años) |
Se encontró asociación significativa entre el embarazo en adolescentes y un inadecuado control prenatal (OR: 1.2 IC95%: 1.14-1.25), debido en su mayoría a un inicio tardío del mismo (OR: 1.52, IC95%: 1.49-1.63). |
|
Faneite et al. (38). Estudio descriptivo. Venezuela, 2008 |
Se incluyeron 1 000 gestantes que acudieron a consulta prenatal en un centro hospitalario |
Los principales factores de inasistencia al control fueron domicilio lejano (52.3%), desempleo (27.3%) y desconocimiento de la importancia del control prenatal (48.8%). |
|
|
Pécora et al. (39). Estudio descriptivo. Argentina, 2007 |
Se reclutaron 401 gestantes en su primera visita al control prenatal |
Se encontró que 76% no concurrió de manera oportuna al control. Este fenómeno se justificó por imposibilidad de acceso a la cita (33%), razones laborales (13%), atención de otros hijos (11%), larga distancia al centro hospitalario (9%), desconocimiento de la importancia del programa (9%) y razones económicas (6%). |
|
|
Ramírez-Zetina et al. (40). Estudio descriptivo multicéntrico. México, 1994 |
Se incluyeron 279 puérperas, reclutadas en las primeras 48 horas postparto |
Se describió la relación entre ausencia de control prenatal y bajos ingresos familiares, dependencia económica materna, convivencia en unión libre, poca comunicación con la pareja, falta de seguro médico y presencia de un embarazo no deseado. |
|
|
Domingues et al. (41). Estudio descriptivo. Brasil, 2007 |
Se incluyeron 2 353 que acudieron al control prenatal |
Se encontró que 25% de las gestantes tuvo inicio tardío del control prenatal. Las principales razones fueron desconocimiento del estado de embarazo (40%), dificultad para el acceso al servicio (27%) y razones personales (18%). |
|
|
Staein A et al. (42). Estudio descriptivo. Uruguay, 2010 |
Se incluyeron 80 gestantes asistentes a control prenatal a un centro hospitalario |
El 42.5% de las gestantes asistieron de manera tardía a su primer control prenatal. Entre estas, 38.24% fueron adolescentes entre 15 y 19 años, 64.7% se encontraban en unión libre, 26.1% tenían a su cargo más de tres hijos y 79.4% presentaron la secundaria incompleta como máximo nivel educativo. |
|
|
Verde et al. (43). Estudio descriptivo. Uruguay, 2009 |
Se analizaron 135 casos de recién nacidos cuyas madres no realizaron control prenatal |
Se encontró que 48.9% de las madres justificaron la ausencia de control debido a carencia de interés en el programa, 17.8% por hijos a su cargo, 10.4% por ausencia de seguro médico, 7.4% por falta de ginecólogo o partera en el centro de referencia, 4.5% por falta de dinero y 3.6% por una larga distancia geográfica al centro de atención. |
|
|
Poffald et al. (44). Estudio cualitativo. Chile, 2012 |
Participaron 160 embarazadas, con el objetivo de explicar el ingreso tardío al control prenatal |
Se encontró que la negación y ocultamiento del embarazo fueron factores de vulnerabilidad familiar y social, que impidieron el acceso oportuno al mismo. |
|
|
Quelopana-del Valle et al. (45). Estudio cualtitativo. México, 2006 |
Se incluyeron 34 gestantes asistentes a centros médicos para inicio del control prenatal |
Se encontró que la percepción de barreras fue el predictor más importante de inicio tardío del control prenatal. Otras limitantes de acceso asociadas fueron actitud negativa hacia el embarazo y problemas económicos |
Fuente: Elaboración propia.
Discusión
La atención prenatal es la actividad médica de rutina más común en todo el mundo (46-49). Sin embargo, no existen estudios con una metodología rigurosa que permitan recomendar las estrategias más adecuadas al respecto. Así las cosas, se han realizado diversas investigaciones observacionales en un intento por evaluar el impacto de las condiciones sociodemográficas sobre el control prenatal en distintos grupos poblacionales.
No todas las embarazadas logran acceder al control prenatal por diferentes razones, algunas de ellas ajenas a la voluntad de las pacientes (1); se han encontrado varios factores relacionados con un control prenatal deficiente, expresados en su mayoría con el inicio tardío del control y un menor número de controles. Entre estos se incluyen la adolescencia, la etnia no blanca, los bajos ingresos, la alta paridad, el bajo nivel educativo, el bajo estatus socioeconómico, la falta de afiliación al sistema de seguridad social y la ausencia de pareja estable (50-58).
La calidad del control prenatal depende de muchos factores, en su mayoría difíciles de evaluar, escapando incluso a los métodos cuantitativos. La atención prenatal debe cumplir idealmente con cinco atributos básicos: precocidad, periodicidad, completitud, cobertura y gratuidad (1), los cuales no siempre se consiguen, en especial en el contexto de los sistemas de salud de los países latinoamericanos.
El estudio de Huanco et al. (37) en Perú reveló la relación entre el embarazo ocurrido en la adolescencia y un control prenatal de mala calidad; estos resultados son consistentes con los encontrados por Mendoza-Tascón et al. (33) en Colombia y Stein & Ferreira (42) en Uruguay. Del mismo modo, el estudio de Faneite et al. (38), llevado a cabo en Venezuela, describió la influencia negativa sobre control prenatal de factores como la obligación laboral-desempleo, el cuidado del hogar y de otros hijos, la ausencia de pareja estable, el domicilio lejano y el desconocimiento de la importancia del programa de control antenatal. Este panorama es similar al encontrado en otros países de Latinoamérica en los trabajos de Pécora et al. (39) en Argentina, Ramírez-Zetina et al. (40) en México, Domingues et al. (41) en Brasil y Stein & Ferreira (42) y Verde et al. (43) en Uruguay.
En Colombia se encontraron 4 estudios que describen indirectamente la situación del programa en el territorio nacional. Moya-Plata et al. (35) encontraron que el 30% de las gestantes de su estudio acudieron a menos de 3 controles prenatales. Mendoza-Tascón et al. (33) destacaron la mala adherencia al control prenatal en mujeres menores de 20 años, hallazgo consistente con lo obtenido por Huanco et al. (37) y Stein & Ferreira (42) en otros países de Latinoamérica. Miranda-Mellano (34) encontró una asociación negativa entre la ausencia de seguridad social y un control prenatal inadecuado, lo que concuerda con los hallazgos de Domingues et al. (41) en Brasil y Verde et al. (43) en Uruguay. Entre tanto, Díaz-Martínez et al. (36), en un análisis de casos de mortalidad perinatal, describieron que aproximadamente 1 de cada 5 muertes podría haberse evitado si las madres hubieran acudido al control prenatal o este hubiera sido adecuado, destacando la relevancia del programa en materia de salud pública.
Conclusión
La literatura disponible sugiere que condiciones sociodemográficas desfavorables podrían incidir de forma negativa sobre el control prenatal. El cuidado del hogar, la atención de otros hijos, la afiliación al sistema de seguridad social, la obligación laboral y el desempleo parecen representar los principales factores que afectan el acceso al mismo. Otros factores involucrados en la calidad del control prenatal son la escolaridad, la edad de la madre al momento de la gestación y las facilidades geográficas para acceder al servicio.
Conflicto de intereses
Ninguno declarado por los autores.
Financiación
Ninguna declarada por los autores.
Agradecimientos
Ninguno declarado por los autores.
Referencias
1.Cáceres-Manrique FM. El control prenatal: una reflexión urgente. Rev Colomb Obstet Ginecol. 2009;60(2):165-70.
2.Minakami H, Maeda T, Fujii T, Hamada H, Iitsuka Y, Itakura A, et al. Guidelines for obstetrical practice in Japan: Japan Society of Obstetrics and Gynecology (JSOG) and Japan Association of Obstetricians and Gynecologists (JAOG) 2014 edition. J Obstet Gynaecol Res. 2014;40(6):1469-99. http://doi.org/c4hh.
3.Costello A, Osrin D, Manandhar D. Reducing maternal and neonatal mortality in the poorest communities. BMJ. 2004;329(7475):1166-8. http://doi.org/c2rgq9.
4.Haines A, Cassels A. Can the millennium development goals be attained? BMJ. 2004;329(7462):394-7. http://doi.org/cm6k8d.
5.Maine D, Rosenfield A. The Safe Motherhood Initiative: why has it stalled? Am J Public Health. 1999;89(4):480-2. http://doi.org/d3xsd7.
6.Delgado-Noguera M, Daza-Córdoba C. Factores que afectan el proceso de vigilancia epidemiológica de la mortalidad materna en el departamento del Cauca. Revista Colombiana de Obstetricia y Ginecología. 2000;51(2):71-6.
7.Gortmaker SL. The effects of prenatal care upon the health of the newborn. Am J Public Health. 1979;69(7):653-60. http://doi.org/fpz2mm.
8.Shiono P, Klebanoff M, Graubard B, Berendes H, Rhoads G. Birth weight among women of different ethnic groups. JAMA. 1986;255(1):48-52. http://doi.org/b68vsr.
9.Murray JL, Bernfield M. The differential effect of prenatal care on the incidence of low birth weight among blacks and whites in a prepaid health care plan. N Engl J Med. 1988;319(21):1385-91. http://doi.org/cx7mrw.
10.Tyson J, Guzick D, Rosenfeld CR, Lasky R, Gant N, Jiminez J, et al. Prenatal care evaluation and cohort analyses. Pediatrics. 1990;85(2):195-204.
11.Malloy MH, Kao TC, Lee YJ. Analyzing the effect of prenatal care on pregnancy outcome: a conditional approach. Am J Public Health. 1992;82(3):448-50.
12.Mustard CA, Roos NP. The relationship of prenatal care and pregnancy complications to birthweight in Winnipeg, Canada. Am J Public Health. 1994;84(9):1450-7. http://doi.org/c8cj9m.
13.Blondel B, Pusch D, Schmidt E. Some characteristics of antenatal care in 13 European countries. Br J Obstet Gynaecol. 1985;92(6):565-8. http://doi.org/dhpqfn.
14.Barros H, Tavares M, Rodrigues T. Role of prenatal care in preterm birth and low birthweight in Portugal. J Public Health Med. 1996;18(3):321-8. http://doi.org/c4hj.
15.Alexander GR, Kotelchuck M. Assessing the role and effectiveness of prenatal care: history, challenges, and directions for future research. Public Health Rep. 2001;116(4):306-16. http://doi.org/dsmvjn.
16.Alexander GR, Cornely DA. Racial disparities in pregnancy outcomes: the role of prenatal care utilization and maternal risk status. Am J Prev Med. 1987;3(5):254-61. http://doi.org/c4jf.
17.Mor JM, Alexander GR, Kogan MD, Kieffer EC, Hulsey TC. Determinants of prenatal care use in Hawaii: implications for health promotion. Am J Prev Med. 1995;11(2):79-85. http://doi.org/c4jg.
18.Vecino-Ortiz A. Determinants of demand for antenatal care in Colombia. Health Policy. 2008;86(2-3):363-72. http://doi.org/dzxs3n.
19.Carroli G, Villar J, Piaggio G, Khan-Neelofur D, Gülmezoglu M, Mugford M, et al. WHO systematic review of randomised controlled trials of routine antenatal care. Lancet. 2001;357(9268):1565-70. http://doi.org/fq4mrh.
20.Santos-Neto ET, Oliveira AE, Zandonade E, Leal Mdo C. Access to prenatal care: assessment of the adequacy of different indices. Cad Saude Publica. 2013;29(8):1664-74. http://doi.org/c4jh.
21.Dowswell T, Carroli G, Duley L, Gates S, Gülmezoglu AM, Khan-Neelfur D, et al. Alternative versus standard packages of antenatal care for low-risk pregnancy. Cochrane Database Syst Rev. 2010;(10):CD000934. http://doi.org/bs5kmc.
22.Say L, Raine R. A systematic review of inequalities in the use of maternal health care in developing countries: examining the scale of the problem and the importance of context. Bull World Health Organ. 2007;85(10):812-9. http://doi.org/c4jj.
23.Al-Nadhedh N. Factors affecting the choice of maternal and child health services in a rural area of Saudi Arabia. East Mediterr Health J. 1995;1(2):261-9.
24.Magadi MA, Agwanda AO, Obare FO. A comparative analysis of the use of maternal health services between teenagers and older mothers in sub-Saharan Africa: evidence from Demographic and Health Surveys (DHS). Soc Sci Med. 2007;64(6):1311-25. http://doi.org/dhhpq5.
25.Glei DA, Goldman N. Understanding ethnic variation in pregnancy-related care in rural Guatemala. Ethn Health. 2000;5(1):5-22. http://doi.org/dq3c9c.
26.Pallikadavath S, Foss M, Stones RW. Antenatal care: provision and inequality in rural north India. Soc Sci Med. 2004;59(6):1147-58. http://doi.org/frnfhw.
27.Gyimah SO, Takyi BK, Addai I. Challenges to the reproductive-health needs of African women: on religion and maternal health utilization in Ghana. Soc Sci Med. 2006;62(12):2930-44. http://doi.org/dn7jhf.
28.Glei DA, Goldman N, Rodríguez G. Utilization of care during pregnancy in rural Guatemala: does obstetrical need matter? Soc Sci Med. 2003;57(12):2447-63. http://doi.org/dm4b3j.
29.Li J. Gender inequality, family planning, and maternal and child care in a rural Chinese county. Soc Sci Med. 2004;59(4):695-708. http://doi.org/cdjct2.
30.Nwakoby BN. Use of obstetric services in rural Nigeria. J R Soc Health. 1994;114(3):132-6. http://doi.org/bb9kwk.
31.McCray TM. An issue of culture: the effects of daily activities on prenatal care utilization patterns in rural South Africa. Soc Sci Med. 2004;59(9):1843-55. http://doi.org/dbvn3n.
32.Duong DV, Binns CW, Lee AH. Utilization of delivery services at the primary health care level in rural Vietnam. Soc Sci Med. 2004;59(12):2585-95. http://doi.org/bqtx6g.
33.Mendoza-Tascón LA, Arias-Guatiboza MD, Peñaranda-Ospina CB, Mendoza-Tascón LI, Manzano-Penagos S, Varela-Bahena AM. Influencia de la adolescencia y su entorno en la adherencia al control prenatal e impacto sobre la prematuridad, bajo peso al nacer y mortalidad neonatal. Rev. Chil. Obstet. ginecol. 2015;80(4):306-15. http://doi.org/c4jm.
34.Miranda-Mellano C. Factores de capacidad en el uso de control prenatal adecuado en gestantes de Sincelejo (Colombia). Salud Uninorte. 2016;32(3):436-51.
35.Moya-Plata D, Guiza-Salazar IJ, Mora-Merchan MA. Ingreso Temprano al Control Prenatal en una Unidad Materno Infantil. Rev Cuid. 2010;1(1):44-52. http://doi.org/c4jp.
36.Díaz-Martínez LA, Cáceres-Manrique FM, Becerra-Mojica CH, Pérez-Vera L, Uscátegui-Dacarett AM. Causas y Determinantes de la Mortalidad Perinatal, Bucaramanga, 1999. MedUNAB. 2000;3(7):5-16.
37.Huanco D, Ticona M, Ticona M, Huanco F. Frecuencia y repercusiones maternas y perinatales del embarazo en adolescentes atendidas en hospitales del Ministerio de Salud del Perú, año 2008. Rev. chil. obstet. ginecol. 2012;77(2):122-8. http://doi.org/c4jq.
38.Faneite P, Rivera C, Rodríguez F, Amato R, Moreno S, Cangemi L. Consulta prenatal: motivos de inasistencia, ¿se justifica? Rev Obstet Ginecol Venez. 2009;69(3):147-51.
39.Pécora A, San Martín ME, Cantero A, Furfaro K, Jankovic MP, Llompart V. Control prenatal tardío: ¿barreras en el sistema de salud? Revista del Hospital Materno Infantil Ramón Sardá. 2008;27(3):114-9.
40.Ramírez-Zetina M, Richardson V, Ávila H, Caraveo VE, Salomón RE, Bacardí M, et al. La atención prenatal en la ciudad fronteriza de Tijuana, México. Rev Panam Salud Publica. 2000;7(2):97-101.
41.Domingues RM, Leal Mdo C, Hartz ZM, Dias MA, Vettore MV. Access to and utilization of prenatal care services in the Unified Health System of the city of Rio de Janeiro, Brazil. Rev Bras Epidemiol. 2013;16(4):953-65. http://doi.org/f6bhkd.
42.Stein A, Ferreira A. Accesibilidad al primer control de embarazo en un centro de salud de la ciudad de Montevideo. Enfermería: cuidados humanizados. 2012;1(1):11-9.
43.Verde ME, Varela L, Episcopo C, García R, Briozzo L, Impallomeni I, et al. Embarazo sin control: Análisis epidemiológico. Rev. Méd. Urug. 2012;28(2):100-7.
44.Poffald L, Hirmas M, Aguilera X, Vega J, González MJ, Sanhueza G. Barreras y facilitadores para el control prenatal en adolescentes: resultados de un estudio cualitativo en Chile. Salud pública Méx. 2013;55(6):572-9.
45.Quelopana-del Valle AM, Champion JD, Salazar-González BC. Factores Psicosociales que Influyen el Inicio del Control Prenatal. Desarrollo Cientif Enferm. 2007;15(3):102-6.
46.Villar J, Ba’aqeel H, Piaggio G, Lumbiganon P, Miguel Belizán J, Farnot U, et al. WHO antenatal care randomised trial for the evaluation of a new model of routine antenatal care. Lancet. 2001;357(9268):1551-64. http://doi.org/dsvtdk.
47.Villar J, Bergsjø P. Scientific basis for the content of routine antenatal care. I. Philosophy, recent studies, and power to eliminate or alleviate adverse maternal outcomes. Acta Obstet Gynecol Scand. 1997;76(1):1-14. http://doi.org/bxm97h.
48.Bergsjø P, Villar J. Scientific basis for the content of routine antenatal care. II. Power to eliminate or alleviate adverse newborn outcomes; some special conditions and examinations. Acta Obstet Gynecol Scand. 1997;76(1):15-25. http://doi.org/cfhzz4.
49.Villar J, Carroli G, Khan-Neelfur D, Piaggio G, Gülmezoglu M. Patterns of routine antenatal care for low-risk pregnancy. Cochrane Database Syst Rev. 2001;(4):CD000934. http://doi.org/cv3h6q.
50.Essex C, Counsell AM, Geddis DC. The demographic characteristics of early and late attenders for antenatal care. Aust N Z J Obstet Gynaecol. 1992;32(4):306-8. http://doi.org/dm2p8b.
51.Petitti D, Coleman C, Binsacca D, Allen B. Early prenatal care in urban black and white women. Birth. 1990;17(1):1-5. http://doi.org/d9f7cm.
52.Melnikow J, Alemagno S. Adequacy of prenatal care among inner-city women. J Fam Pract. 1993;37(6):575-82.
53.LaVeist TA, Keith VM, Gutierrez ML. Black/white differences in prenatal care utilization: an assessment of predisposing and enabling factors. Health Serv Res. 1995;30(1):43-58.
54.Roberts RO, Yawn BP, Wickes SL, Field CS, Garretson M, Jacobsen SJ. Barriers to prenatal care: factors associated with late initiation of care in a middle-class midwestern community. J Fam Pract. 1998;47(1):53-61.
55.Blondel B, Kaminski M, Breart G. Antenatal care and maternal demographic and social characteristics. Evolution in France between 1972 and 1976. J Epidemiol Community Health. 1980;34(3):157-63. http://doi.org/c7m6r6.
56.Buekens P. Variations in provision and uptake of antenatal care. Baillieres Clin Obstet Gynaecol. 1990;4(1):187-205. http://doi.org/dnvh68.
57.Brown S. Drawing women into prenatal care. Family Planning Perspectives. 1989;21(2):73-88. http://doi.org/dnz53v.
58.Joseph CL. Identification of factors associated with delayed antenatal care. J Natl Med Assoc. 1989;81(1):57-63.
Jean-Baptiste Marc Bourgery. (1797- 1849)
“Traité complet de l’anatomie de l’homme: comprenant la médecine operatoire”
Referencias
Cáceres-Manrique FM. El control prenatal: una reflexión urgente. Rev Colomb Obstet Ginecol. 2009;60(2):165-70.
Minakami H, Maeda T, Fujii T, Hamada H, Iitsuka Y, Itakura A, et al. Guidelines for obstetrical practice in Japan: Japan Society of Obstetrics and Gynecology (JSOG) and Japan Association of Obstetricians and Gynecologists (JAOG) 2014 edition. J Obstet Gynaecol Res. 2014;40(6):1469-99. http://doi.org/c4hh.
Costello A, Osrin D, Manandhar D. Reducing maternal and neonatal mortality in the poorest communities. BMJ. 2004;329(7475):1166-8. http://doi.org/c2rgq9.
Haines A, Cassels A. Can the millennium development goals be attained? BMJ. 2004;329(7462):394-7. http://doi.org/cm6k8d.
Maine D, Rosenfield A. The Safe Motherhood Initiative: why has it stalled? Am J Public Health. 1999;89(4):480-2. http://doi.org/d3xsd7.
Delgado-Noguera M, Daza-Córdoba C. Factores que afectan el proceso de vigilancia epidemiológica de la mortalidad materna en el departamento del Cauca. Revista Colombiana de Obstetricia y Ginecología. 2000;51(2):71-6.
Gortmaker SL. The effects of prenatal care upon the health of the newborn. Am J Public Health. 1979;69(7):653-60. http://doi.org/fpz2mm.
Shiono P, Klebanoff M, Graubard B, Berendes H, Rhoads G. Birth weight among women of different ethnic groups. JAMA. 1986;255(1):48-52. http://doi.org/b68vsr.
Murray JL, Bernfield M. The differential effect of prenatal care on the incidence of low birth weight among blacks and whites in a prepaid health care plan. N Engl J Med. 1988;319(21):1385-91. http://doi.org/cx7mrw.
Tyson J, Guzick D, Rosenfeld CR, Lasky R, Gant N, Jiminez J, et al. Prenatal care evaluation and cohort analyses. Pediatrics. 1990;85(2):195-204.
Malloy MH, Kao TC, Lee YJ. Analyzing the effect of prenatal care on pregnancy outcome: a conditional approach. Am J Public Health. 1992;82(3):448-50.
Mustard CA, Roos NP. The relationship of prenatal care and pregnancy complications to birthweight in Winnipeg, Canada. Am J Public Health. 1994;84(9):1450-7. http://doi.org/c8cj9m.
Blondel B, Pusch D, Schmidt E. Some characteristics of antenatal care in 13 European countries. Br J Obstet Gynaecol. 1985;92(6):565-8. http://doi.org/dhpqfn.
Barros H, Tavares M, Rodrigues T. Role of prenatal care in preterm birth and low birthweight in Portugal. J Public Health Med. 1996;18(3):321-8. http://doi.org/c4hj.
Alexander GR, Kotelchuck M. Assessing the role and effectiveness of prenatal care: history, challenges, and directions for future research. Public Health Rep. 2001;116(4):306-16. http://doi.org/dsmvjn.
Alexander GR, Cornely DA. Racial disparities in pregnancy outcomes: the role of prenatal care utilization and maternal risk status. Am J Prev Med. 1987;3(5):254-61. http://doi.org/c4jf.
Mor JM, Alexander GR, Kogan MD, Kieffer EC, Hulsey TC. Determinants of prenatal care use in Hawaii: implications for health promotion. Am J Prev Med. 1995;11(2):79-85. http://doi.org/c4jg.
Vecino-Ortiz A. Determinants of demand for antenatal care in Colombia. Health Policy. 2008;86(2-3):363-72. http://doi.org/dzxs3n.
Carroli G, Villar J, Piaggio G, Khan-Neelofur D, Gülmezoglu M, Mugford M, et al. WHO systematic review of randomised controlled trials of routine antenatal care. Lancet. 2001;357(9268):1565-70. http://doi.org/fq4mrh.
Santos-Neto ET, Oliveira AE, Zandonade E, Leal Mdo C. Access to prenatal care: assessment of the adequacy of different indices. Cad Saude Publica. 2013;29(8):1664-74. http://doi.org/c4jh.
Dowswell T, Carroli G, Duley L, Gates S, Gülmezoglu AM, Khan-Neelfur D, et al. Alternative versus standard packages of antenatal care for low-risk pregnancy. Cochrane Database Syst Rev. 2010;(10):CD000934. http://doi.org/bs5kmc.
Say L, Raine R. A systematic review of inequalities in the use of maternal health care in developing countries: examining the scale of the problem and the importance of context. Bull World Health Organ. 2007;85(10):812-9. http://doi.org/c4jj.
Al-Nadhedh N. Factors affecting the choice of maternal and child health services in a rural area of Saudi Arabia. East Mediterr Health J. 1995;1(2):261-9.
Magadi MA, Agwanda AO, Obare FO. A comparative analysis of the use of maternal health services between teenagers and older mothers in sub-Saharan Africa: evidence from Demographic and Health Surveys (DHS). Soc Sci Med. 2007;64(6):1311-25. http://doi.org/dhhpq5.
Glei DA, Goldman N. Understanding ethnic variation in pregnancy-related care in rural Guatemala. Ethn Health. 2000;5(1):5-22. http://doi.org/dq3c9c.
Pallikadavath S, Foss M, Stones RW. Antenatal care: provision and inequality in rural north India. Soc Sci Med. 2004;59(6):1147-58. http://doi.org/frnfhw.
Gyimah SO, Takyi BK, Addai I. Challenges to the reproductive-health needs of African women: on religion and maternal health utilization in Ghana. Soc Sci Med. 2006;62(12):2930-44. http://doi.org/dn7jhf.
Glei DA, Goldman N, Rodríguez G. Utilization of care during pregnancy in rural Guatemala: does obstetrical need matter? Soc Sci Med. 2003;57(12):2447-63. http://doi.org/dm4b3j.
Li J. Gender inequality, family planning, and maternal and child care in a rural Chinese county. Soc Sci Med. 2004;59(4):695-708. http://doi.org/cdjct2.
Nwakoby BN. Use of obstetric services in rural Nigeria. J R Soc Health. 1994;114(3):132-6. http://doi.org/bb9kwk.
McCray TM. An issue of culture: the effects of daily activities on prenatal care utilization patterns in rural South Africa. Soc Sci Med. 2004;59(9):1843-55. http://doi.org/dbvn3n.
Duong DV, Binns CW, Lee AH. Utilization of delivery services at the primary health care level in rural Vietnam. Soc Sci Med. 2004;59(12):2585-95. http://doi.org/bqtx6g.
Mendoza-Tascón LA, Arias-Guatiboza MD, Peñaranda-Ospina CB, Mendoza-Tascón LI, Manzano-Penagos S, Varela-Bahena AM. Influencia de la adolescencia y su entorno en la adherencia al control prenatal e impacto sobre la prematuridad, bajo peso al nacer y mortalidad neonatal. Rev. Chil. Obstet. ginecol. 2015;80(4):306-15. http://doi.org/c4jm.
Miranda-Mellano C. Factores de capacidad en el uso de control prenatal adecuado en gestantes de Sincelejo (Colombia). Salud Uninorte. 2016;32(3):436-51.
Moya-Plata D, Guiza-Salazar IJ, Mora-Merchan MA. Ingreso Temprano al Control Prenatal en una Unidad Materno Infantil. Rev Cuid. 2010;1(1):44-52. http://doi.org/c4jp.
Díaz-Martínez LA, Cáceres-Manrique FM, Becerra-Mojica CH, Pérez-Vera L, Uscátegui-Dacarett AM. Causas y Determinantes de la Mortalidad Perinatal, Bucaramanga, 1999. MedUNAB. 2000;3(7):5-16.
Huanco D, Ticona M, Ticona M, Huanco F. Frecuencia y repercusiones maternas y perinatales del embarazo en adolescentes atendidas en hospitales del Ministerio de Salud del Perú, año 2008. Rev. chil. obstet. ginecol. 2012;77(2):122-8. http://doi.org/c4jq.
Faneite P, Rivera C, Rodríguez F, Amato R, Moreno S, Cangemi L. Consulta prenatal: motivos de inasistencia, ¿se justifica? Rev Obstet Ginecol Venez. 2009;69(3):147-51.
Pécora A, San Martín ME, Cantero A, Furfaro K, Jankovic MP, Llompart V. Control prenatal tardío: ¿barreras en el sistema de salud? Revista del Hospital Materno Infantil Ramón Sardá. 2008;27(3):114-9.
Ramírez-Zetina M, Richardson V, Ávila H, Caraveo VE, Salomón RE, Bacardí M, et al. La atención prenatal en la ciudad fronteriza de Tijuana, México. Rev Panam Salud Publica. 2000;7(2):97-101.
Domingues RM, Leal Mdo C, Hartz ZM, Dias MA, Vettore MV. Access to and utilization of prenatal care services in the Unified Health System of the city of Rio de Janeiro, Brazil. Rev Bras Epidemiol. 2013;16(4):953-65. http://doi.org/f6bhkd.
Stein A, Ferreira A. Accesibilidad al primer control de embarazo en un centro de salud de la ciudad de Montevideo. Enfermería: cuidados humanizados. 2012;1(1):11-9.
Verde ME, Varela L, Episcopo C, García R, Briozzo L, Impallomeni I, et al. Embarazo sin control: Análisis epidemiológico. Rev. Méd. Urug. 2012;28(2):100-7.
Poffald L, Hirmas M, Aguilera X, Vega J, González MJ, Sanhueza G. Barreras y facilitadores para el control prenatal en adolescentes: resultados de un estudio cualitativo en Chile. Salud pública Méx. 2013;55(6):572-9.
Quelopana-del Valle AM, Champion JD, Salazar-González BC. Factores Psicosociales que Influyen el Inicio del Control Prenatal. Desarrollo Cientif Enferm. 2007;15(3):102-6.
Villar J, Ba’aqeel H, Piaggio G, Lumbiganon P, Miguel Belizán J, Farnot U, et al. WHO antenatal care randomised trial for the evaluation of a new model of routine antenatal care. Lancet. 2001;357(9268):1551-64. http://doi.org/dsvtdk.
Villar J, Bergsjø P. Scientific basis for the content of routine antenatal care. I. Philosophy, recent studies, and power to eliminate or alleviate adverse maternal outcomes. Acta Obstet Gynecol Scand. 1997;76(1):1-14. http://doi.org/bxm97h.
Bergsjø P, Villar J. Scientific basis for the content of routine antenatal care. II. Power to eliminate or alleviate adverse newborn outcomes; some special conditions and examinations. Acta Obstet Gynecol Scand. 1997;76(1):15-25. http://doi.org/cfhzz4.
Villar J, Carroli G, Khan-Neelfur D, Piaggio G, Gülmezoglu M. Patterns of routine antenatal care for low-risk pregnancy. Cochrane Database Syst Rev. 2001;(4):CD000934. http://doi.org/cv3h6q.
Essex C, Counsell AM, Geddis DC. The demographic characteristics of early and late attenders for antenatal care. Aust N Z J Obstet Gynaecol. 1992;32(4):306-8. http://doi.org/dm2p8b.
Petitti D, Coleman C, Binsacca D, Allen B. Early prenatal care in urban black and white women. Birth. 1990;17(1):1-5. http://doi.org/d9f7cm.
Melnikow J, Alemagno S. Adequacy of prenatal care among inner-city women. J Fam Pract. 1993;37(6):575-82.
LaVeist TA, Keith VM, Gutierrez ML. Black/white differences in prenatal care utilization: an assessment of predisposing and enabling factors. Health Serv Res. 1995;30(1):43-58.
Roberts RO, Yawn BP, Wickes SL, Field CS, Garretson M, Jacobsen SJ. Barriers to prenatal care: factors associated with late initiation of care in a middle-class midwestern community. J Fam Pract. 1998;47(1):53-61.
Blondel B, Kaminski M, Breart G. Antenatal care and maternal demographic and social characteristics. Evolution in France between 1972 and 1976. J Epidemiol Community Health. 1980;34(3):157-63. http://doi.org/c7m6r6.
Buekens P. Variations in provision and uptake of antenatal care. Baillieres Clin Obstet Gynaecol. 1990;4(1):187-205. http://doi.org/dnvh68.
Brown S. Drawing women into prenatal care. Family Planning Perspectives. 1989;21(2):73-88. http://doi.org/dnz53v.
Joseph CL. Identification of factors associated with delayed antenatal care. J Natl Med Assoc. 1989;81(1):57-63.
Cómo citar
APA
ACM
ACS
ABNT
Chicago
Harvard
IEEE
MLA
Turabian
Vancouver
Descargar cita
Licencia
Derechos de autor 2019 Revista de la Facultad de Medicina

Esta obra está bajo una licencia Creative Commons Reconocimiento 3.0 Unported.
-





















